![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
44 Cards in this Set
- Front
- Back
|
where does fertilization occur
|
uterin tube
|
|
|
what is capacitation
|
-period of sperm conditioning in female reproductive tract
-prepares the acrosome for fertilization |
|
|
what are the __ three stages of fertilization
|
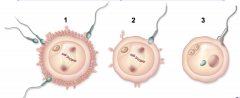
3
1Corona radiata penetration 2 Acrosome reaction and zona pellucida penetration 3 Fusion of sperm and oocyte plasma membranes and pronuclei |
|
|
what weeks are considered the pre-embryonic period
|
weeks 1-2
|
|
|
what is the process of the pre-embryonic period
|
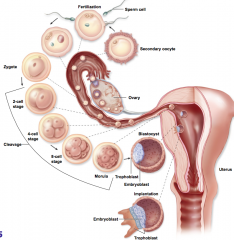
|
|
|
when does implantation usually occure
|
about 7 days after fertilization
|
|
|
the trophoblasts divides into the.....
|
cytotrophoblast a
syncytiotrphoblast |
|
|
what does the syncytiotrophoblast do
|
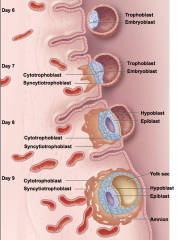
burrows into the stratum functional is of the endometrium
produces human chorionic gonadotropin |
|
|
what is the function of the placenta
|
-exchange of nutrients reparatory gases, wast products and antibodies
-production of estrogen and progesterone |
|
|
what structures form the placenta
|
stratum functionlais -from mother
chorion - fetus |
|
|
do the mothers blood and baby's blood mix
|
no
|
|
|
what weeks of pregnancy are considered the embryonic period
|
3-8
|
|
|
what is the process of the embryonic period
|
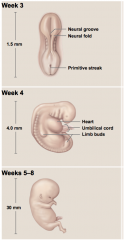
primitive streak forms
gastrulation body folding neuralation limb buds form organogenesis |
|
|
what are the differences between males and females at week 5
|
none
|
|
|
what on the Y chromosome causes testes to develop
|
TDF region (SRY gene)
|
|
|
if there is no TDF region present what develops
|
ovaries
|
|
|
t/f embryos initially only contain male or female duct systems
|
f
they have both |
|
|
what determines which duct system generates and which degenerates
|
genes and hormones
|
|
|
what are the ducts that end up being in the female called
|
paramesonephric ducts
|
|
|
what are the ducts that end up being in the male called
|
mesonephric ducts
|
|
|
internal female development
|
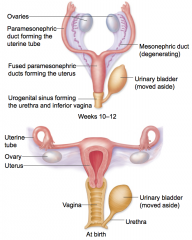
|
|
|
internal male development
|
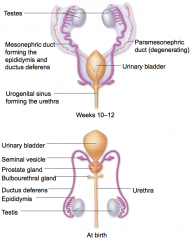
|
|
|
what are the structures at the sexually indifferent state of development
|
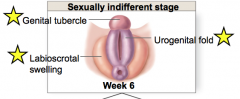
-genital tubercle
labioscrotal swelling urogenital fold |
|
|
external development
|
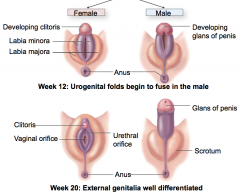
|
|
|
what is the female homologue to the testes
|
ovaries
|
|
|
what is the common function of the ovaries and testes
|
produce gametes and sex hormones
|
|
|
what is the common function of the clitoris and glans of the penis
|
contain autonomic nervous system axons that stimulate feelings of arousal and sexual climax
|
|
|
what is the male homologue to the clitoris
|
glans of the penis
|
|
|
what is the female homologue to the scrotum
|
labia majora
|
|
|
what is the male homologue to the vestibular glands
|
bulbourethral glands
|
|
|
what is the common function of the labia majora and the scrotum
|
protect and cover some reproductive structures
|
|
|
what is the common function of the vestibular glands and the bulbourethral glands
|
secrete mucin for lubricatiion
|
|
|
what are the weeks of the fetal period
|
9-38
|
|
|
what happens during the fetal period of pregnancy
|
Growth and maturation of existing organs
Bones ossify Reproductive organs develop Brain enlarges Body elongates Limbs grow Organ systems become functional Baby movement begins Baby gains weight |
|
|
what are some of the characteristics near the end of pregnancy
|
Gestation lasts 38 weeks from conception (40 weeks from last menstrual period)
Uterus expands ~20 times larger than normal Breasts enlarge and develop ability to produce milk Uterus myometrium becomes more active during last trimester. Mild contractions may occur. Hormones soften the cervix and loosen the pubic symphysis Baby “drops” and is normally oriented head down with face posterior |
|
|
what are the __ stages of labor
|
3
cervical dilation expulsion placental |
|
|
what is cervical dilation
|
-begins with first regal contraction and ends why the cervix is fully dilated
-longest stage |
|
|
how long does expulsion last
|
from full dilation to delivery of baby
|
|
|
what is the placental stage
|
expulsion of the placenta
|
|
|
how long after delivery does is the placenta expulsed
|
15-30 minutes
|
|
|
what are the reason to have a c-section
|
Previous C-section
Narrow pelvis and large fetus Placental abruption (placenta detaches) Placenta previa (placenta covers the cervix) Atypical presentation of baby (breach, etc.) Cord prolapse (umbilical cord exits uterus before baby) Fetal distress |
|
|
what is placental abruption
|
placenta detaches
|
|
|
what is placenta previa
|
placenta cover the cervix
|
|
|
what is a cord prolapse
|
umbilical cord exits the uterus before the baby
|

