![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
51 Cards in this Set
- Front
- Back
|
3 major functions of the cardiovascular system:
|
*Deliver oxygen-carrying blood to the tissues
*Provide nutrients to the cells *Remove waste products from cells |
|
|
Function of:
arteries-- veins-- capillaries-- |
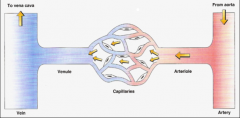
*Arteries carry blood from the heart to the tissues.
*Veins carry blood from tissues back to the heart. *Thin-walled capillaries, interposed between arteries & veins allow exchange of nutrients, wastes and fluid. |
|
|
Discuss 2 "other" functions of the CV system:
|
1) “Homeostatic” functions
-Regulation of blood pressure (baroreceptors) -Regulation of body temperature -Facilitates adjustments to altered physiologic states -Exercise -Change in posture -Hemorrhage 2) Delivery of endocrine hormones to sites of action in tissues |
|
|
Cardiovascular anatomy:
|
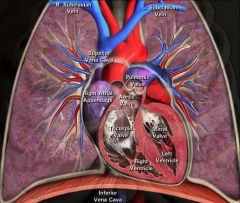
LA is posterior!
|
|
|
Path of blood flow through Heart and Lungs with pressures listed at each step:
|
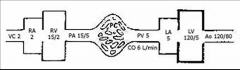
|
|
|
The big picture of blood flow. What % of the blood is present in the:
brain-- coronaries-- renal-- GI-- skeletal muscle-- skin-- |
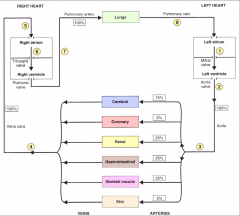
*GI varies by time of day and activity (less in running)
*Renal large % for use and filtering. |
|
|
Diagrams of blood/gas exchange:
|
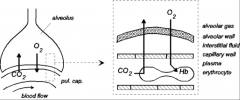
*Very extensive capillary bed in the lungs, obviously.
*O2 and CO2 diffuse directly across endothelial wall. |
|
|
Anatomical location of the pulmonary veins:
|
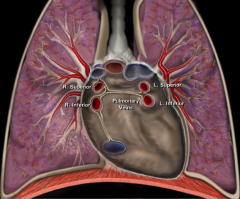
|
|
|
Coronal view of left atrial anatomy:
|
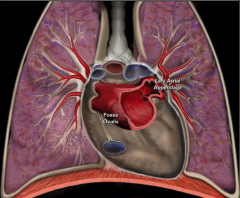
|
|
|
Coronal view of left ventricular anatomy:
|
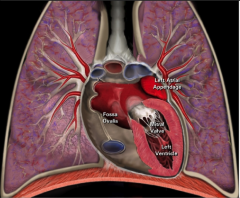
|
|
|
Coronal view of aortic valve anatomy:
|
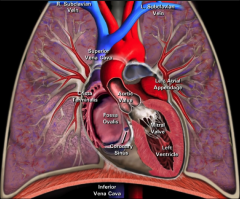
|
|
|
Coronal view of right ventricle and pulmonic valve anatomy:
|
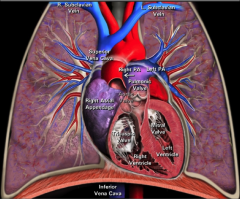
|
|
|
Right heart cardiac blood flow:
|
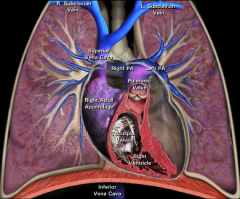
|
|
|
Left heart cardiac blood flow:
|
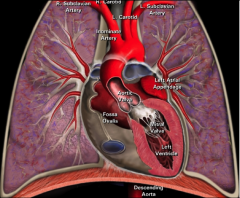
|
|
|
Entire heart cardiac blood flow:
|
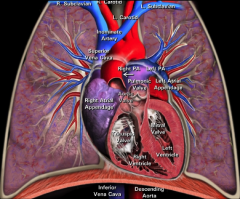
|
|
|
How is CO distributed to organs?
How is is regulated? Give approximate distributions by organ system: |
*Cardiac output distributed to organs in parallel.
*Distribution is variable, regulated by arterioles (by arteriolar constriction and by pre-capillary sphincters). *Approximate distribution: 15% brain 5% heart 25% kidneys 25% GI 25% muscle 5% skin |
|
|
Describe traits of arteries:
|
Arteries:
*Thick-walled *High-pressure system *Become progressively smaller, branching into arterioles *Site of arteriolar resistance *Alpha-1 and Beta-2 receptors Veins: *Thin-walled *Low-pressure system *Large capacitance *Small branches are called “venules” *Also innervated by sympathetic nervous system |
|
|
Describe traits of capillaries:
what 4 things get exchanged here? |
*Lined with a single layer of endothelial cells.
*Surrounded by basal lamina. *Are the site of exchange of: -Nutrients -Gases -Water -Solutes |
|
|
Diagram of the microcirculation:
What adjusts the flow? 2 things. |
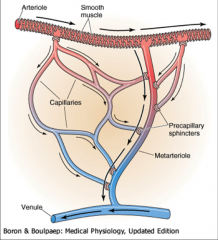
-Flow adjusted by smooth muscle constriction and precapillary sphincters.
|
|
|
Generic diagram of a capillary:
|
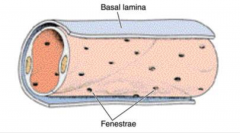
|
|
|
Continuous vs. fenestrated capillaries:
which is most common? where are they located? |
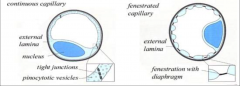
*Continuous are most common (found lots of places). Pinocytotic vesicles are necessary to bring water actively into continuous capillaries. Water can also come in across junctions b/t capillaries.
*Fenestrated ones are located in intestines and glomeruli. Adapted to bring water-soluble substances in more easily. |
|
|
Capillaries: what's the difference in how lipid and water soluble substances cross?
|
*Lipid-soluble substances (e.g. oxygen and CO2) cross the endothelial cell membranes.
*Water-soluble substances (e.g. ions) cross either through: -Water-filled clefts between cells -Large pores in walls of “fenestrated” capillaries -Pinocytotic vesicles via “transcytosis” |
|
|
Discuss selective perfusion of capillaries:
|
*Not all capillaries are perfused at all times (e.g. during exercise).
*Perfusion is governed by dilation or constriction of arterioles and pre-capillary sphincters. *Regulated by sympathetic innervation of blood vessels and vasoactive metabolites which act locally (at tissue level). |
|
|
Area vs. volume of the different types of vessels:
|
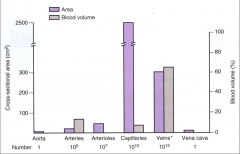
*Note number of the vessel types (x axis).
*10^10 capillaries accounts for huge total cross-sectional area. |
|
|
Equation for velocity of blood flow:
|
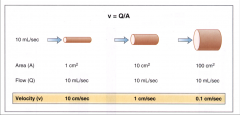
Velocity = rate of a displacement of blood per unit time
Defined as: v = Q/A v = velocity in cm/sec Q = flow in mL/sec A = cross sectional area (cm2) *Velocity increases if area decreases. |
|
|
Where is the v of blood highest? Why?
|
Highest in the Aorta (lowest area...there's only one aorta!)
|
|
|
Where is v of blood lowest? Why?
How much slower is this than flow in the aorta? |
*Capillaries (greatest area; 10^10 capillaries!)
*Allows for more time for exchange of nutrients, etc. *Velocity in aorta ~ 800 x velocity in capillaries |
|
|
Blood flow through a vessel is determined by:
|
*Pressure difference at each end of the vessel
*Resistance of the vessel to blood flow ∆V = IR or ∆P=QR Where: Q = flow (mL/min) ΔP = Pressure difference (mm Hg) R = Resistance (mm Hg/mL/min) |
|
|
Resistance of the entire systemic vasculature is called:
|
“Total Peripheral Resistance” (TPR) or
“Systemic Vascular Resistance” (SVR) |
|
|
The blood flow to the left kidney is measured at 500 mL/min. The pressure in the renal artery is 100 mm Hg. The pressure in the renal vein is 10 mm Hg.
Question: What is the vascular resistance of the left kidney? |
R = ΔP / Q
R = (100 – 10) / 500 = 0.18 mm Hg/mL/min |
|
|
What pressure drop would one measure to calculate the systemic vascular resistance (SVR)?
|
Mean arterial pressure minus mean right atrial pressure.
~90 minus ~5 = ~85 mm Hg |
|
|
What pressure drop would one measure to calculate the pulmonary vascular resistance (PVR)?
|
Mean pulmonary arterial pressure minus mean left atrial pressure (PCWP).
|
|
|
Determinants of vascular resistance include what 3 things?
What equation describes this? |
Blood vessel diameter, blood vessel length, and viscosity of the blood.
*Poiseuille equation |
|
|
What's the Poiseuille equation?
|
R = 8ηl / πr^4
Where η = blood viscosity l = length of blood vessel r = vessel radius (most important determinant of resistance) |
|
|
Relationship of resistance to:
viscosity-- length-- radius-- |
*Resistance increases as viscosity increases.
*Resistance increases as length increases. *Resistance increases as radius decreases to the fourth power. |
|
|
Calculating resistance in series and parallel:
|
Exact same as an electrical circuit.
Rseries = R1 + R2 + R3... 1/Rparallel = 1/R1 + 1/R2 + 1/R3... |
|
|
Examples of series and parallel resistances in the vasculature:
|
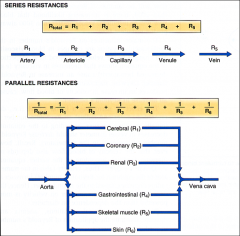
Series: arrangement of blood vessels within an organ.
|
|
|
In series, where is resistance the highest?
|
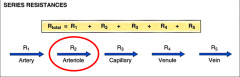
*As blood flows through the series, pressure decreases. Most dramatic drop is at the level of the arterioles.
|
|
|
Laminar vs. turbulent flow:
What's the word for turbulent flow in the heart? What's the word for turbulent flow in the vessels? |
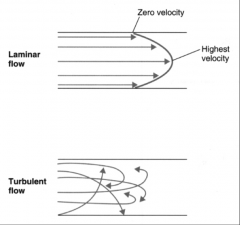
*Ideally, blood flow in the cardiovascular system is laminar.
*Laminar flow implies a parabolic profile of velocity. *Irregularities in the vessel cause turbulent flow. *In turbulent flow, streams are propelled radially and axially *More energy is required *Turbulent flow in the heart can cause a “murmur” *Turbulent flow in blood vessels can cause a “bruit” (blocked carotid bruit is easy to hear) |
|
|
What is Reynold's number?
What does it predict? |

*Reynold’s number is a dimensionless number used to predict whether blood flow is laminar or turbulent.
*NR < 2000 predicts laminar flow. *NR > 2000 predicts turbulent flow. |
|
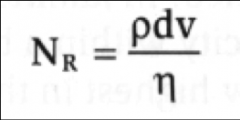
Major influences on Reynold’s number:
|
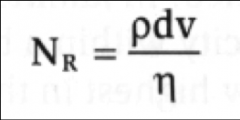
*Blood viscosity (decreased viscosity increases turbulence – e.g. anemia)
*Velocity of flow (increased velocity increases turbulence) |
|
|
How does blood vessel narrowing affect turbulence?
|
*Decreased radius occurs, but velocity increases by SQUARE of radius.
*Therefore, narrower vessels (or stenotic vessels) have higher turbulence. |
|
|
Discuss compliance of blood vessels:
|
Compliance in a blood vessel is similar to compliance of the heart:
*Compliance is proportional to ΔV / ΔP. *Compliance of veins is high – (veins can hold large volume of blood at low pressure). *Compliance of arteries is lower – (they hold a lower volume at a higher pressure). *Older arteries are least compliant. |
|
|
Compare compliance of veins, arteries, and aging arteries:
What was an early treatment for HTN and why is it related to compliance? |
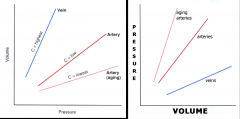
Plot on the left shows compliance (∆V/∆P).
Early treatment for HTN was a diuretic--decreasing volume decreases BP. |
|
|
Describe the overall pressure drop in the CV system:
|
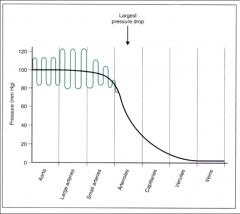
*There is a progressive drop in mean pressure as blood flows from:
-The aorta: to the arteries, to the arterioles, to the capillaries, to the venules and to the great veins. -The largest pressure drop occurs at the arteriolar level. |
|
|
Discuss the pulsatility of the cardiac cycle:
|
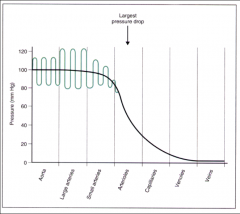
*Arterial pressure is pulsatile, due to the cardiac cycle:
-Systolic pressure represents the highest pressure in the pressure tracing. -Diastolic pressure represents the lowest pressure in the pressure tracing. -MEAN pressure is the driving pressure, and is calculated as: Diastolic pressure + 1/3 of the pulse pressure. |
|
|
Mean pressures of the:
Aorta-- Arterioles-- Capillaries-- VC-- |
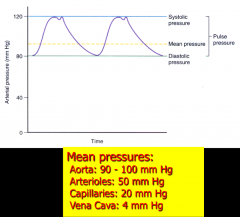
|
|
|
What happens to blood pressure with:
The aging process? Stenosis of the subclavian artery? |
Aging: BP increases (decreased compliance, narrower vessels?).
Stenosis of subclavian: BP in unblocked arm would be normal. BP in blocked arm would be lower (increased resistance causes pressure drop). |
|
|
Major histologic differences b/t arteries and veins:
|
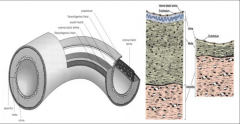
-Media (smooth muscle) much thicker in artery.
-Internal elastic lamina thick in artery; almost non-existent in veins. -Adventitia is much the same. |
|
|
Overall diagram of circulatory system from Costanzo--xs areas, velocity, blood volume, and pressure:
|

*Note higher xs area of capillary bed in the lungs compared to systemic!
*Note velocity of capillary flow. *Note capacitance of veins compared to arteries. *Note loss of "Phases" at the level of the arterioles. Pressure drops b/c of resistance--it's just a blunted pressure at that point. |
|
|
How do you know the severity of a bruit?
|
Pitch.
High pitch is bad! |

