![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
56 Cards in this Set
- Front
- Back
|
What is the tylenol dose for peds
|
40mg/kg every 4 hours, not more than 5 doses/day
|
|
|
What does TORCH stand for?
|
Toxoplasmosis
Other (such as syphilis, varicella, mumps, parvovirus, and HIV) Rubella CMV Herpes simplex |
|
|
first line treatment for AOM
|
amoxicillin 80-90mg/kg/day dosed BID
|
|
|
what is the cause of most cases of AOM?
|
respiratory viruses - they are self limiting
|
|
|
what is the most common bacteria associated with AOM?
|
strep pneumoniae ~40%
H. influenzae ~25-30% Moraxella catarrhalis 10-15% |
|
|
what are the most common pathogens for EOM?
|
pseudomonas aeruginosa
Staph aureus fungal = aspergillus |
|
|
how does EOM present?
|
rapid onset of ear pain, tenderness, itching, aural fullness and hearing loss
|
|
|
what is the treatment for uncomplicated EOM?
|
cleaning of the ear canal and application of topical anti-infective agents.
|
|
|
what are currant jelly stools associated with?
|
Intussusception
|
|
|
How is Intussusception diagnosed?
|
barium or air-contrast enemas. They are both diagnostic and therapeutic
|
|
|
What is the common presentation of a child with AOM?
|
Fever, Irritability, Poor sleep, Appetite decrease
Ear pain, feeling of fullness Upper resp. symptoms |
|
|
Findings on PE of AOM?
|
bulging TM
decreased landmark visibility light reflex dull or missing mobility decreased Neurologically - may see decreased balance |
|
|
Treatment of pain of AOM
|
topical benzocaine (auralgan) DO NOT USE if TM perforated
|
|
|
If you suspect AOM in kids ______ age, treat with antibiotics, do not wait for observation first
|
<6months
|
|
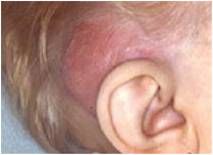
What is this a picture of?
|
mastoiditis
|
|
|
Cystic mass of epithelial cells and cholesterol
|
Cholesteatoma
|
|
|
Presentation of sinusitis with gradual onset
|
Post nasal drainage, rhinorrhea, daytime cough (may be worse at night) longer than 10-14 days
Pain: forehead, retro-orbital, tooth or maxillary pain |
|
|
Sudden presentation with sinusitis
|
High fever
Nasal discharge Headache in older children Periorbital inflammation |
|
|
Physical Examination findings with sinusitis
|
Nasal mucosa inflamed
Nasal or postnasal discharge Sinus percussion Periorbital swelling or cellulitis, pressure to palpation over medial canthus of eye (ethmoiditis) |
|
|
DDx with sinusitis
|
Sequential viral upper respiratory
tract infections |
|
|
Important to know if the symptoms of sinusitis have improved and then gotten worse, if so it is probably?
|
viral that turns into bacterial
|
|
|
treatment of sinusitis
|
Oral antibiotics: 10-21 days
Symptomatic care OTC decongestants (NOT for kids <2) Inhaled corticosteroids Pain relief Hospitalization / Referral for signs of complications |
|
|
sinusitis - refer to ENT if
|
Not improving after two courses of appropriate antibiotics
Signs of complications |
|
|
Periorbital (preseptal) cellulitis treatment
|
Mild - oral antibiotics w/close F/U
Severe: hospitalization for iv antibiotics |
|
|
Orbital (postseptal) cellulitis s/s
|
Proptosis
Pain with eye movement Limited extraocular movements Impaired vision |
|
|
how is Orbital (postseptal) cellulitis diagnosed?
|
CT scan
|
|
|
Treatment of Orbital (postseptal) cellulitis
|
IV antibiotics
Ophthalmology referral Some need surgical intervention, debridement and drainage |
|
|
Complications of Orbital (postseptal) cellulitis
|
Central nervous system
Meningitis Subdural abscess Epidural abscess Brain abscess Vascular Cavernous sinus thrombosis Bone Osteomyelitis frontal bone (Pott’s puffy tumor) |
|
|
Second line treatment for AOM?
|
Amoxicillin-clavulanate: 80-90 mg/kg/day amoxicillin 6.4mg/kg/day clavulanate in 2 doses (Augmentin ES)
Cefdinir 14mg/kg/day daily or divided BID Cefpodoxime 10mg/kg/day daily Cefuroxime 30mg/kg/day divided BID |
|
|
treatment for AOM if PCN allergy with type 1 rxn?
|
Azithromycin 10mg/kg/day day 1, 5mg/kg/day days 2-5 (Not a first line drug for otitis media)
Clindamycin 30-40mg/kg/day divided TID (horrible tasting, lots of GI upset |
|
|
What makes resistance a higher risk for kids with AOM?
|
Daycare attendance
Recent antibiotics (<30days) Age less than 2 years |
|
|
AOM with ipsilateral conjunctivitis more likely caused by?
|
H. influenzae
|
|
|
treatment of Otitis media with PE tubes in place?
|
Ciprofloxacin otic drops: 5 drops BID – don’t need oral antibiotics. Can still get otitis media w/tubes
|
|
|
Hand/foot/mouth disease is caused by?
|
coxsackie virus
|
|
|
Physical Examination findings with tonsillitis
|
Oropharynx
Tonsil size and presence or absence of exudate Palatal petechiae Peritonsillar swelling Uvula deviation Cervical adenopathy Sandpaper rash Tympanic membrane evaluation Hepatosplenomegaly |
|
|
How long is strep pyogenes Contagious?
|
24 hours after treatment started
|
|
|
treatment of strep pyogenes
|
Penicillin VK
<13 years 250mg bid 10 days >13 years 500mg bid 10days amoxicillin 40mg/kg daily divided bid 10 days Benzathine penicillin G <27kg 600,000 units IM > 27 kg 1.2 million units IM Penicillin allergic: Azithromycin 12mg/kg daily for 5 days Cephalosporins |
|
|
complications of strep pyogenes
|
Peritonsillar abscess, otitis media, cervical adenitis
Rheumatic fever post-strep glomerulonephritis -Hematuria with RBCs and RBC casts Decreased complement levels (C3 and sometimes C4) |
|
|
Glomerulonephritis s/s and characteristics
|
Recent strep infection (throat or skin, present w/tea or coke colored urine – take their BP)
3-7 years of age Hematuria, hypertension, edema Self-limiting |
|
|
Infectious Mononucleosis is caused by?
|
Epstein-Barr virus
|
|
|
S/S of Mononucleosis
|
Exudative tonsillitis
Fever Cervical adenopathy Hepatosplenomegaly and generalized adenopathy may be present |
|
|
Lab test for Mononucleosis
|
Monospot
Positive heterophile antibody test and serologic test for antibodies against EBV are usually diagnostic. |
|
|
Pathogen associated with Epiglottitis
|
Haemophilus influenzae type b
|
|
|
Epiglottitis S/S
|
drooling, stridor,
|
|
|
Age group most likely to see epiglottitis?
|
Toddlers
|
|
|
What does the classic thumbprint sign indicate?
|
epiglottitis
|
|
|
Common name for laryngotracheobronchitis?
|
croup
|
|
|
Most common age group to see croup?
|
< 2 years old – older than 2 yrs, think about asthma
|
|
|
etiology of croup
|
usually viral, most often parainfluenza, also RSV, flu, adenovirus, mycoplasma
|
|
|
Presentation of croup
|
Prodrome: Upper respiratory symptoms
Respiratory Barky cough – worsens at night Inspiratory stridor – is at rest? Fever |
|
|
How long does croup usually last?
|
Resolves in 1-2 days.
|
|
|
Physical findings with croup
|
Barky cough
Inspiratory stridor Signs of respiratory distress – nasal flaring, retractions |
|
|
treatment of croup
|
Mild
Symptomatic – Cold air, humidity Moderate to severe Symptomatic – even in the office Dexamethasone 0.6 mg/kg po/im Nebulization |
|
|
3 stages of pertussis
|
1. Catarrhal stage – treat at this stage! URI symptoms 1-2 weeks
2.Paroxysmal stage -Paroxysmal cough 1-2 weeks 3. Convalescent stage -Milder cough |
|
|
Diagnosis of pertussis
|
Nasal swab for culture, DFA or DNA amplification
CBC: leukocytosis with lymphocytosis |
|
|
Treatment of pertussis
|
Supportive
Antibiotics Azithromycin 10mg/kg daily 5-7 days, adult 500mg daily 5-7 days Erythromycin 40-50mg/kg/day divided QID 14 days Trimethoprim-sulfamethoxazole one DS tab BID 14 days Hospitalization Droplet precautions for five days |

