![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
123 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
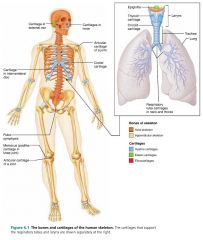
skeletal cartilage |
cartilage molded to fit its body location and function; no nerves or blood vessels, fibers form a structural mesh
|
|
|
|
perichondrium
|
a layer of dense irregular connective tissue surrounding skeletal cartilage, resists outward expansion and contains blood vessels
|
|
|
|
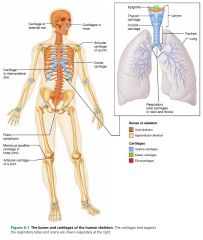
1. hyaline
2. elastic 3. fibrocartilage |
3 types of skeletal cartilages |
|
|
|
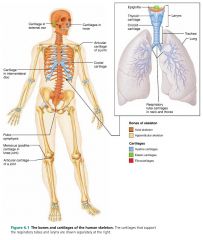
hyaline cartilage |
cartilage with a glasslike extracellular matrix, provides support with flexibility and resilience; visible collagen fibers |
|
|
|
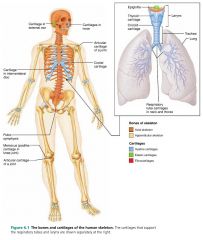
– the ends of movable joints |
locations of hyaline cartilage |
|
|
|
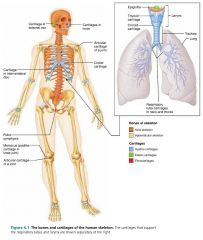
elastic cartilage
|
cartilage with stretchy elastic fibers that allows for bending; contains collagen fibers and visible elastic fibers |
|
|
|
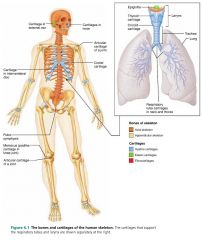
– outer ear
– epiglottis |
locations of elastic cartilage |
|
|
|
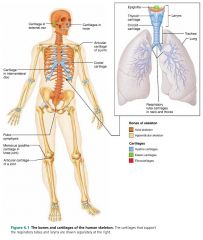
fibrocartilage
|
highly compressible cartilage with great tensile strength; contains thick and visible collagen fibers
|
|
|
|
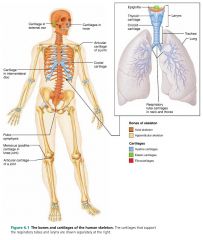
– intervertebral discs
– menisci (knees, jaw) |
locations of fibrocartilage
|
|
|
|
1. appositional growth
2. interstitial growth |
2 forms of cartilage growth |
|
|
|
appositional growth
|
form of cartilage growth in which chondrocytes of the perichondrium secrete new matrix against the external face of the existing cartilage tissue
|
|
|
|
interstitial growth
|
form of cartilage growth in which the chondrocytes divide and secrete new matrix, expanding the cartilage from within
|
|
|
|
206
|
# of bones in the human body
|
|
|
|
1. axial
2. appendicular |
2 main groups of the skeleton
|
|
|
|
1. support
2. protection 3. movement 4. hematopoiesis 5. hormone production 6. mineral and growth factor storage 7. fat storage |
7 important functions of bone
|
|
|
|
hematopoiesis
|
blood cell formation
|
|
|
|
1. calcium
2. phosphate |
2 important minerals stored in bone matrix
|
|
|
|
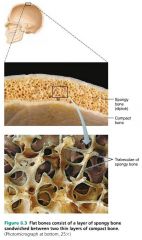
compact bone
|
smooth and dense external layer of a bone
|
|
|
|
spongy bone
|
trabeculae–lined internal layer of a bone
|
|
|
|
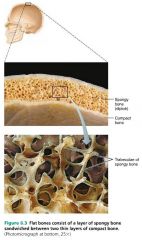
trabeculae
|
small needle–like or flat pieces that form the honeycomb shape in spongy bone; open spaces filled with bone marrow
|
|
|
|
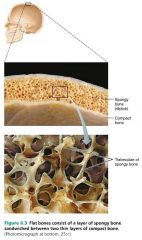
diploë |
the sandwich–like spongy bone of short, flat, and irregular bones
|
|
|
|
diaphysis
|
the long, tube–shaped shaft of a long bone; compact bone surrounding a central medullary cavity |
|
|
|
medullary cavity
|
central cavity of the diaphysis containing fat (yellow marrow); called the yellow marrow cavity in adults
|
|
|
|
epiphyses
|
the broad ends of long bones
|
|
|
|
articular cartilage
|
covers the ends of the epiphyses, cushions the opposing ends of bones during movement and absorbs stress
|
|
|
|
epiphyseal line
|
remnant of the epiphyseal plate
|
|
|
|
epiphyseal plate
|
a hyaline cartilage disc separating the diaphysis and each epiphysis that grows during childhood and lengthens the bone
|
|
|
|
1. periosteum
2. endosteum |
2 membranes covering a bone
|
|
|
|
periosteum
|
a glistening white, double–layered membrane covering the external surface of a bone; provides nutrition to the bone
|
|
|
|
1. fibrous layer
2. osteogenic layer |
2 layers of the periosteum
|
|
|
|
fibrous layer
|
outer layer of the periosteum; dense irregular connective tissue
|
|
|
|
osteogenic layer
|
inner layer of the periosteum; contains osteogenic cells
|
|
|
|
nutrient foramina
|
openings in the periosteum that allow nerve fibers and blood vessels to pass through the bone shaft to the marrow cavity
|
|
|
|
Sharpey's fibers (perforating fibers)
|
collagen fibers that secure the periosteum to the underlying bone matrix
|
|
|
|
endosteum
|
a delicate connective tissue membrane covering the internal surface of bones
|
|
|
|
red marrow
|
hematopoietic tissue found within the trabecular cavities of spongy bone (long bones) and in the diploe (flat bones)
|
|
|
|
red marrow cavities
|
cavities that house hematopoietic tissue
|
|
|
|
1. trabecular cavities (long bones)
2. diploë |
2 types of red marrow cavities
|
|
|
|
bone markings
|
projections, depressions, and openings on bone surfaces that serve as sites of muscle, ligament, and tendon attachment, as joint surfaces, or as conduits for blood vessels and nerves
|
|
|
|
1. attachment (muscles, ligaments, tendons) |
3 functions of bone markings |
|
|
|
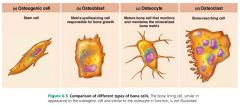
1. osteogenic cells
2. osteoblasts 3. osteocytes 4. bone lining cells 5. osteoclasts |
5 major cell types in bone |
|
|
|
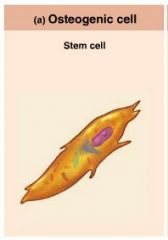
osteogenic cells (osteoprogenitor cells) |
active stem cells found in the periosteum and endosteum; become osteoblasts or bone lining cells |
|
|
|
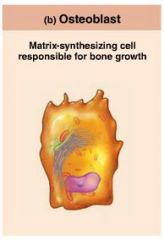
osteoblasts
|
bone–forming cells that secrete the bone matrix
|
|
|
|
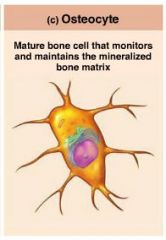
osteocytes
|
mature bone cells that monitor and maintain the bone matrix; spidery cells that occupy spaces (lacunae) that conform to their shape
|
|
|
|
bone lining cells
|
flat cells that help maintain the bone matrix in areas where no remodeling occurs |
|
|
|
1. periosteal cells
2. endosteal cells |
2 types of bone lining cells
|
|
|
|
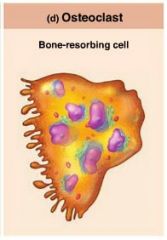
osteoclasts
|
giant multinucleate cells with ruffled borders that break down bone with lysosomal enzymes |
|
|
|
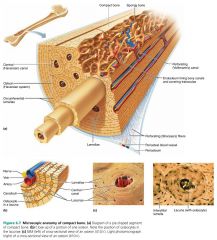
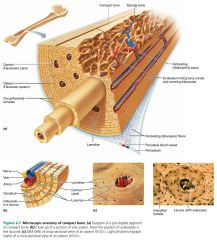
osteon (Haversian system)
|
the cylinder–shaped structural unit of compact bone; tiny weight–bearing pillars
|
|
|
|
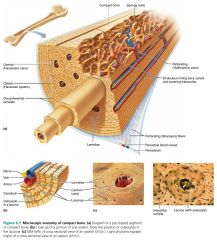
lamella
|
concentric rings of bone matrix making up an osteon (Haversian system) |
|
|
|
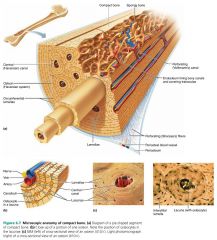
central canal (Haversian canal)
|
canal containing blood vessels and nerve fibers running through the core of each osteon
|
|
|
|
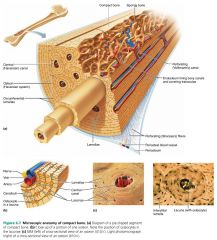
perforating canal (Volkmann's canals)
|
canals connecting the blood and nerve supply of the periosteum to the central canals and medullary cavity
|
|
|
|
lacunae |
hollow spaces housing the spider–shaped osteocytes at the junctions of the lamellae |
|
|
|
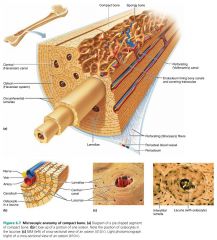
canaliculi
|
hairlike canals connecting the lacunae to each other and to the central canal
|
|
|
|
interstitial lamellae
|
incomplete lamellae lying between intact osteons; fill gaps or are remnants of old osteons
|
|
|
|
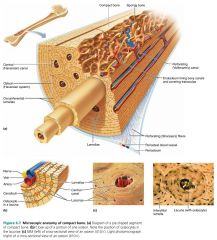
circumferential lamellae
|
lamellae covering the entire circumference of the diaphysis; resist twisting of the long bone
|
|
|
|
1. bone cells
2. osteoid |
2 organic components of bone (33%)
|
|
|
|
osteoid
|
organic part of bone matrix including ground substance and collagen fibers
|
|
|
|
sacrificial bonds
|
stretchy and breakable bonds between collagen molecules that can be reformed
|
|
|
|
mineral salts (hydroxyapatites)
|
inorganic component of bone (65%); tiny, tightly packed crystals surrounding collagen fibers in the bone matrix; account for a bone's hardness; ex. calcium phosphate
|
|
|
|
ossification (osteogenesis)
|
the process of bone formation
|
|
|
|
1. endochondral ossification |
2 types of bone formation in a human embryo
|
|
|
|
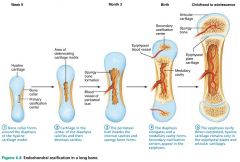
endochondral ossification
|
bone developed by replacing hyaline cartilage; "cartilage bones", includes all bones below the base of the skull (except the clavicles) |
|
|
|
Stage 1 of 5
|
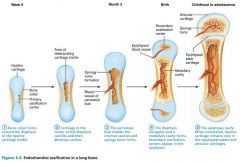
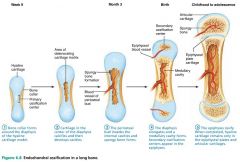
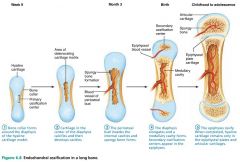
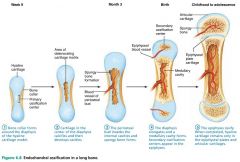
Endochondral Ossification: a bone collar forms around the diaphysis of the hyaline cartilage model
|
|
|
|
Stage 2 of 5
|
Endochondral Ossification: cartilage in the center of the diaphysis calcifies and cavities develop; chondrocytes die
|
|
|
|
Stage 3 of 5
|
Endochondral Ossification: the periosteal bud invades the internal cavities and spongy bone forms
|
|
|
|
Stage 4 of 5
|
Endochondral Ossification: the diaphysis elongates and a medullary cavity forms, osteoclasts break down spongy bone
|

|
|
|
Stage 5 of 5
|
Endochondral Ossification: the epiphyses ossify |
|
|
|
primary ossification center |
the center of a hyaline cartilage shaft where long bone formation typically begins
|
|
|
|
periosteal bud
|
collection of elements that invade a newly forming bone (nutrient artery and vein, nerve fibers, red marrow elements, osteogenic cells, and osteoclasts)
|
|
|
|
secondary ossification center
|
the centers where bone is created from cartilage in one or both epiphyses |
|
|
|
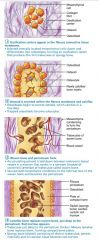
intramembranous ossification
|
a bone develops from a fibrous membrane; membrane bone, includes the cranial bones and the clavicles |
|
|
|
mesenchymal cells
|
cells responsible for bone development in intramembranous ossification
|
|
|
|
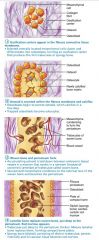
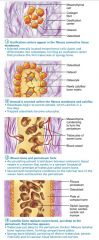
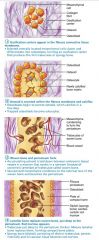
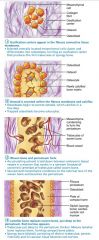
Stage 1 of 4
|
Intramembranous Ossification: ossification centers appear in the fibrous connective tissue membrane; mesenchymal cells become osteoblasts
|
|
|
|
Stage 2 of 4
|
Intramembranous Ossification: osteoblasts secrete osteoid within the fibrous membrane that calcifies
|
|
|
|
Stage 3 of 4
|
Intramembranous Ossification: woven bone and periosteum forms
|
|
|
|
Stage 4 of 4
|
Intramembranous Ossification: lamellar bone replaces woven bone, red marrow appears
|
|
|
|
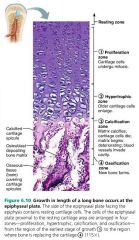
1. proliferation zone |
4 zones of bone growth
|
|
|
|
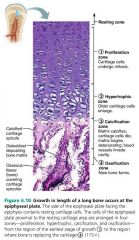
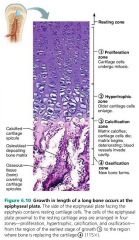
proliferation zone |
Bone growth: area where cartilage cells undergo mitosis |
|
|
|
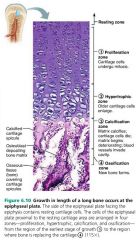
hypertrophic zone |
Bone growth: area where older cartilage cells enlarge
|
|
|
|
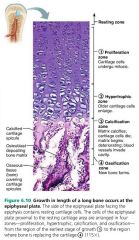
calcification zone
|
Bone growth: area where matrix calcifies, cartilage cells die, blood vessels invade cavity |
|
|
|
ossification zone |
Bone growth: area where new bone forms |
|
|
|
epiphyseal plate closure
|
the process of longitudinal bone growth ending when the epiphysis and diaphysis bones fuse |
|
|
|
growth hormone
|
hormone that stimulates epiphyseal plate activity; released by the anterior pituitary gland
|
|
|
|
thyroid hormone
|
hormone that regulates growth hormone so that the skeleton grows proportionally
|
|
|
|
sex hormones
|
hormones promoting growth spurts in adolescensce; masculinization or feminization; induce epiphyseal closure
|
|
|
|
bone remodeling
|
process of deposit and resorption of bone in the periosteum and endosteum
|
|
|
|
1. bone deposit
2. bone resorption |
2 stages of bone remodeling
|
|
|
|
1. osteoblasts (deposition)
2. osteoclasts (resorption) |
"remodeling units" that coordinate bone deposition and resorption
|
|
|
|
1. hormonal controls
2. response to mechanical stress |
2 factors influencing bone remodeling
|
|
|
|
1. nerve impulses
2. muscle contraction 3. blood coagulation 4. secretion |
4 reasons calcium is necessary
|
|
|
|
parathyroid hormone (PTH)
|
hormone that stimulates osteoclasts to resorb bone, releasing calcium into the blood
|
|
|
|
calcitonin
|
hormone that temporarily lowers calcium levels
|
|
|
|
hypercalcemia
|
condition resulting in undesirable calcium salt deposits in the blood vessels and kidneys
|
|
|
|
leptin
|
hormone released by adipose tissue that inhibits osteoblasts
|
|
|
|
Wolff's Law
|
law stating that a bone grows or remodels in response to the demands placed on it
|
|
|
|
hormonal controls
|
determine whether and when bone remodeling occurs, in response to changing blood calcium levels
|
|
|
|
mechanical stress
|
determines where remodeling occurs
|
|
|
|
fracture
|
term for broken bones
|
|
|
|
nondisplaced fractures
|
broken bone ends retain their normal position
|
|
|
|
displaced fractures
|
broken bone ends are out of normal alignment
|
|
|
|
complete fracture
|
bone is broken all the way through
|
|
|
|
incomplete fracture
|
bone is not broken all the way through
|
|
|
|
open (compound) fracture
|
broken bone penetrates the skin
|
|
|
|
closed (simple) fracture |
broken bone does not penetrate the skin
|
|
|
|
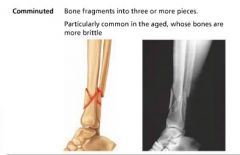
comminuted fracture
|
bone fragments into three or more pieces; common in the elderly |
|
|
|
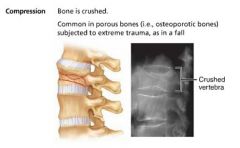
compression fracture
|
bone is crushed; common in porous bones |
|
|
|
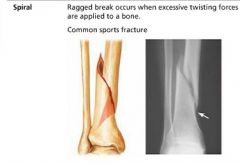
spiral fracture
|
ragged break occuring when excessive twisting forces are applied to a bone; common in sports
|
|
|
|
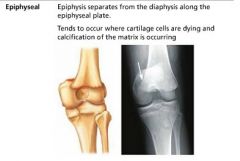
epiphyseal fracture
|
epiphysis separates from the diaphysis along the epiphyseal plate; common when chondrocytes are dying and calcification of the matrix is occurring
|
|
|
|
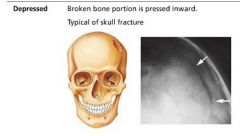
depressed fracture
|
broken bone portion is pressed inward; common in skull fracture
|
|
|
|
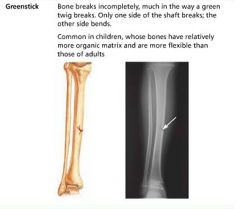
greenstick fracture
|
bone breaks incompletely (only one side breaks); common in children
|
|
|
|
closed (external) reduction
|
the physician's hands coax the broken bone ends into position
|
|
|
|
open (internal) reduction
|
the broken bone ends are secured together surgically with pins or wires |
|
|
|
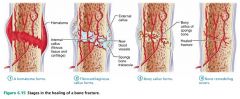
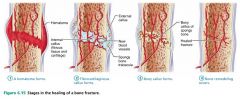
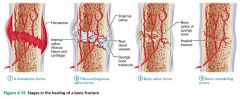
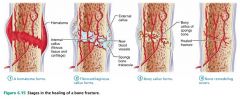
Stage 1 of 4
|
Bone repair: a hematoma forms
|
|
|
|
Stage 2 of 4
|
Bone repair: fibrocartilaginous callus forms
|
|
|
|
Stage 3 of 4 |
Bone repair: bony callus forms
|
|
|
|
Stage 4 of 4
|
Bone repair: bone remodeling occurs
|
|
|
|
hematoma
|
mass of clotted blood
|
|
|
|
fibrocartilaginous callus
|
mass of repair tissue in a broken bone
|
|
|
|
bony (hard) callus
|
spongy bone that replaces the fibrocartilaginous callus in a broken bone
|
|
|
|
osteomalacia
|
includes a number of disorders in which bones are poorly mineralized, becoming soft and weak; caused by insufficient calcium or vitamin D
|
|
|
|
rickets
|
osteomalacia in children; much more severe
|
|
|
|
osteoporosis
|
a group of diseases in which bone resorption outpaces bone deposit; bones become fragile and porous
|
|
|
|
Paget's disease
|
disease characterized by haphazard bone deposit and resorption; too much spongy bone, not enough compact bone |
|

