![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
190 Cards in this Set
- Front
- Back
|
What situation could result in maternal antibodies attacking fetal blood cells during a second pregnancy?
|
Mom is Rh negative and fetus is Rh positive
(Hemolytic Disease of the Newborn - HDN) |
|
|
Stercobilin and urobilin are both breakdown products of what component of blood?
|
Heme
|
|
|
The intrinsic and extrinsic pathways of blood clotting are identical after formation of ...
|
Prothrombinase
|
|
|
What are components of blood?
|
Blood plasma 55%
Formed elements Platelets White blood cells Red Blood cells |
|
|
Types of Bones
|
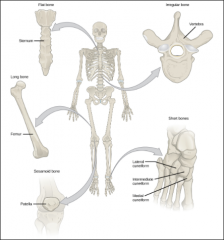
Long
Flat Irregular Short Sesamoid |
|
|
Long Bones
|
Long
Consist of a shaft and epiphysis Slightly curved to absorb weight Compact bone tissue & Spongy bone tissue [e.g. femur, tibia, fibula, humerus, ulna, radius, phalanges] |
|
|
Short Bones
|
Cube shaped
Spongy bone with a thin layer of compact bone tissue [e.g. carpal and tarsal bones] |
|
|
Flat Bones
|
Thin and composed of two nearly parallel plates of compact bone tissue enclosing a layer of spongy bone tissue
Afford protection and provide areas of attachment for muscles [e.g. cranial bones, sternum, ribs, and scapulae] |
|
|
Irregular Bones
|
Complex shapes
Vary in amount of spongy and compact bone [e.g. vertebrae, hip bones, facial bones, and calcaneus] |
|
|
Sesamoid Bones
|
Develop in certain tendons where there is considerable friction, tension and physical stress
Vary in number from person to person Usually small Protect tendons from excessive wear and tear Often change the direction of pull of a tendon [e.g. patellae, bones in palms and soles] |
|
|
Axial Skeleton
|
![The bones along a longitudinal axis of the body
[skull (cranium and face), hyoid, auditory ossicles, vertebral column, and thorax (sternum and ribs)]
80 Bones](https://images.cram.com/images/upload-flashcards/00/33/09/3003309_m.png)
The bones along a longitudinal axis of the body
[skull (cranium and face), hyoid, auditory ossicles, vertebral column, and thorax (sternum and ribs)] 80 Bones |
|
|
Appendicular Skeleton
|
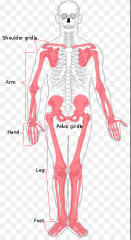
Whatever bones are added to the axial skeleton (appendages)
[pectoral girdles (clavicle and scapula), upper limbs (humerus, ulna, radius, carpals, metacarpals, and phalanges), pelvic girdle, lower limbs (femur, patella, fibula, tibia, tarsals, metatarsals, and phalanges)] 126 Bones |
|
|
Fetal Vertebral Column
|
Single concave curve
|
|
|
Adult Vertebral Column
|
Four curves, two concave and two convex
Primary: Thoracic and Sacral curves that retain the concave shape Secondary: Cervical and Lumbar curves that grow to be convex |
|
|
Cranial Bones
|
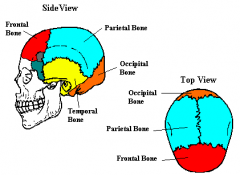
Frontal
Parietal Sphenoid Ethmoid Lacrimal Zygomatic Vomer Temporal Nasal Maxilla Mandible Occipital |
|
|
Scoliosis
|
Lateral bending of the vertebral column in the thoracic region
|
|
|
Kyphosis
|
Hunchback
Increase in the thoracic curve |
|
|
Lordosis
|
Increase in the lumbar curve
"hollow back" |
|
|
Atlas Vertebra
|
Large arch
No spinous process Largest superior articulating process First cervical vertebra |
|
|
Axis Vertebra
|
Has an 8th process: Dens process (pivot)
Second cervical vertebra |
|
|
Cervical Vertebrae
|
Have bifurcated spinous processes
Small bodies Large vertebral arch 3 foramina: 1 vertebral foramen (largest in all the spinal column), 2 transverse foramina |
|
|
Thoracic Vertebrae
|
Large and strong
Slanted spinous processes Costal facets for articulation with the tubercles of the ribs Superior articular facets for articulation with the heads of ribs Demifacets on the sides |
|
|
Lumbar Vertebrae
|
Largest and strongest
Largest bodies Hatchet-shaped spinous processess Quadrilateral in shape, thick and broad |
|
|
Sacrum
|
Triangular bone formed by the union of 5 sacral vertebrae
8 sacral foramina Top: Base; Bottom: Apex |
|
|
Coccyx
|
Tailbone
Triangular in shape Formed by the fusion on 4 coccygeal vertebrae Points anteriorly |
|
|
Sutures
|
Fxn: Immovable joints between bones of the skull that absorb shock and keep pressure from building up in the cranium
Coronal Saggital Lambdoid Squamous |
|
|
Fontanels
|
Fxn: "soft spots", membranous sections of the skull that allow the head to be flexible for birth and enable the brain the grow
Anterior Posterior Anterolateral (2) Posterolateral (2) |
|
|
Canal/Meatus
|
Tube-like passageway
|
|
|
Condyle
|
Rounded articular process
|
|
|
Foramen
|
Opening or hole through a bone
|
|
|
Fossa
|
Shallow depression
|
|
|
Ramus
|
Branch-like process
|
|
|
Fissure
|
Narrow slit or cleft in the bone
|
|
|
Spinal Process
|
Pointed posterior projection
|
|
|
Transverse Process
|
Extends laterally from each pedicle to the side
|
|
|
Sternoclavicular Joint
|
Where the clavicle articulates with the manubrium of the sternum
|
|
|
Acromioclavicular Joint
|
Where the scapula articulates with the clavical
|
|
|
Glenohumeral Joint
|
Where the scapula articulates with the humerus
|
|
|
The 3 hip bones
|
Ilium
Ischium Pubis |
|
|
Male Pelvis
|
Heavy
Rough Large Vertical Narrow true pelvis Tilted forward Pelvic inlet is heart shaped <90 degree pubic arch angle |
|
|
Female Pelvis
|
Small
Light Large true pelvis Tilted forward Flared Pelvic inlet is round or oval >90 degree pubic arch angle Wide sciatic notch |
|
|
True Pelvis
|
Portion of pelvis inferior to pelvic brim
Surrounds the pelvic cavity |
|
|
False Pelvis
|
Portion of pelvis superior to pelvic brim
Wide area extending to top of the iliac crest |
|
|
Directional Terms
|
Posterior
Anterior Lateral Medial Superior Inferior Distal Proximal Contralateral Ipsilateral |
|
|
Number of Bones in the Upper Extremity
(And know where they are) |
64
Clavicle - 2 Scapula - 2 Humerus - 2 Ulna - 2 Radius - 2 Carpals - 16 Metacarpals - 10 Phalanges - 28 |
|
|
Structural Joint Classification
|
Based on the presence or absence of a space between the articulating bones
Also based on the type of connective tissue that binds the bones together Synovial Cartilaginous Fibrous |
|
|
Synovial Joints
|
The bones forming the joint have a synovial cavity and are united by the dense irregular connective tissue of an articular capsule, and often by accessory ligaments
|
|
|
Cartilaginous Joints
|
No synovial cavity, and the bones are held together by cartilage
|
|
|
Fibrous Joints
|
No synovial cavity, and the bones are held together by dense irregular connective tissue that is rich in collagen fibres
|
|
|
Functional Joint Classification
|
Relates to the degree of movement the joint permits
Synarthrosis Amphiarthrosis Diarthrosis |
|
|
Synarthrosis Joints
|
Immovable joint
|
|
|
Amphiarthrosis Joints
|
Slightly movable joint
|
|
|
Diarthrosis Joint
|
Freely movable joint
All are synovial joints |
|
|
Hyaline Cartilage
|
The type of cartilage that covers the articular ends of bones
|
|
|
Synovial Fluid
|
The fluid that lubricates, reduces friction, and gives nutrition to a joint
|
|
|
Articular Cartilage
|
The tissue at the end of a bone that reduces friction in a joint
|
|
|
Bursae
|
The sac-like structure that is sometimes present to reduce friction
|
|
|
Synovial Membrane
|
Structure that secretes synovial fluid
|
|
|
Articular Capsule
|
Surrounds a synovial joint, encloses the synovial cavity, and unites the articulating bones
|
|
|
Fibrous Membrane
|
Consists of dense irregular connective tissue that attaches to the periosteum of the articulating bones
|
|
|
Synovial Cavity
|
A space between articulating bones
|
|
|
Factors affecting ROM in synovial joints
|
Articulating bones - shape or structure
Ligaments - tightness and strength Muscles - Arrangement and tension Body part contact Hormones Disuse |
|
|
Aging in Joints
|
Decreased production of synovial fluid in joints
Articular cartilage thins Ligaments shorten and lose flexibility Rheumatism and Arthritis |
|
|
Diseases of Joints
|
Rheumatoid Arthritis
Osteoarthritis Gouty Arthritis |
|
|
Rheumatoid Arthritis
|
Joints are swollen, stiff and painful
Body attacks its own tissues Inflammation of the joints Loss of function Occurs bilaterally |
|
|
Osteoarthritis
|
Due to wear and tear of the body
degenerative joint disorder joint cartilage is gradually lost ends of the bones are exposed bones grow more and create spurs, which add to the discomfort first the hips and the knees effected mainly the articular cartilage |
|
|
Gouty Arthritis
|
build up of uric acid in the blood
reacts with sodium and creates crystals that accumulate in the tissues of joints kidneys and feet effected associated with a lot of alcohol and red meat intake |
|
|
Functions of Muscle Tissue
|
Movement
Stabilizing Body Positions Storing and Moving Substances within the body Heat production |
|
|
Properties of Muscle Tissue
|
Electric Excitability
Contractibility Extensibility Elasticity |
|
|
Electric Excitability
|
Ability to respond to a stimulus
|
|
|
Contractility
|
Develops tension and can shorten length (or vice versa)
|
|
|
Extensibility
|
Extend or stretch
|
|
|
Elasticity
|
Can return to original shape after contraction or extension
|
|
|
Skeletal muscle contraction will continue to occur as long as what chemicals are available in the cytosol of the muscle fibre?
|
Calcium Ions and ATP
|
|
|
Aerobic cellular respiration in skeletal muscles
|
Pyruvic acid generated by glycolysis enters the mitochondria
O2 is essential CO2 is produced as a waste product Can be used to generate ATP from fats, proteins or carbohydrates |
|
|
After prolonged strenuous exercise has stopped, heavy breathing will often continue for several minutes in order to provide the oxygen needed to...
|
Convert the lactic acid produced during exercise back into glycogen
Resynthesize creatine phosphate Replace oxygen displaced from muscle myoglobin |
|
|
Myasthenia Gravis is an autoimmune disorder that targets the ACh receptors at the NMJ and ultimately reduces the number of available receptors. Predict what happens if you treat the patient with a drug that inhibits the activity of acetylcholinesterase?
|
Normal contraction
|
|
|
What region of a sarcomere contain thin filaments?
|
I band
|
|
|
The type of tendon formed when the connective tissue elements of a skeletal muscle extend as a broad flat layer
|
Aponeurosis
|
|
|
The sequence of structures that action potentials must move through to excite skeletal muscle contraction
|
Axon of neuron - Sarcolemma - T tubules
|
|
|
Myofibrils contain ...
|
Contractile proteins
Regulatory proteins Structural proteins |
|
|
Calcium ions are released from the sarcoplasmic reticulum into the cytosol ...
|
at the beginning of contraction
|
|
|
What energizes the myosin head?
|
ATP hydrolysis reaction
|
|
|
Epimysium
|
The outermost layer of dense, irregular connective tissue, encircling the entire muscle
|
|
|
Perimysium
|
A layer of dense, irregular connective tissue
Surrounds groups of 10-100 or more muscle fibres, separating them into bundles called fascicles |
|
|
Endomysium
|
Penetrates the interior of each fascicle and separates individual muscle fibre from one another
Reticular fibres |
|
|
Somatic Motor Neurons
|
Stimulate skeletal muscle fibres to contract
Joined with the muscle at the neuromuscular junction |
|
|
Hypertrophy
|
The increase of the size of existing muscle fibres
|
|
|
Hyperplasia
|
The increase in the number of muscle cells
|
|
|
Sarcolemma
|
The plasma membrane of a muscle cell
|
|
|
Sarcoplasm
|
The cytoplasm of a muscle fibre
|
|
|
T Tubules
|
Tiny invaginations of the sarcolemma that tunnel in from the surface toward the centre of each muscle fibre
|
|
|
Myofilaments
|
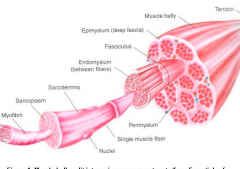
Protein structures within myofibrils
Thin filaments: composed mostly of protein actin Thick filaments: composed mostly of the protein myosin Both are directly involved in the contractile process 2 thin filaments for ever thick filament |
|
|
Sarcomere
|
The basic functional units of a myofibril
The filaments inside a myofibril are arranged in these compartments |
|
|
Sarcomere Regions
|
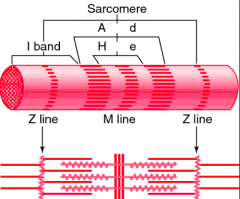
Z disc
M line I band A band H zone |
|
|
Z disc
|
Narrow, plate-shaped region of dense protein material
Separate one sarcomere from the next |
|
|
M line
|
The middle of the sarcomere
Formed by supporting proteins that hold the thick filaments together at the center |
|
|
I band
|
A lighter, less dense area that contains the rest of the thin filaments but no thick filaments
A Z disc passes through the centre of each |
|
|
A band
|
The darker middle part of the sarcomere
Extends the entire length of the thick filaments |
|
|
H zone
|
Narrow
In the centre of each A band Contains thick but no thin filaments |
|
|
Location of the Heart
|
Mediastinum: from the sternum anteriorly to the vertebral column posteriorly, medially between the two lungs and the pleural membranes that cover them, sits on the diaphragm
|
|
|
Heart Layers
|
Pericardium - triple-layered sac that surrounds & protects the heart
Myocardium - middle layer; large thick muscle portion Epicardium - thin, transparent outer layer of the heart wall Endocardium - Inner layer |
|
|
Contractile Proteins
|
Proteins that generate force during muscle contraction
-Myosin -Actin |
|
|
Regulatory Proteins
|
Proteins that help switch muscle contraction process on and off
-Tropomyosin -Troponin |
|
|
Structural Proteins
|
Proteins that keep thick and thin filaments of myofibrils in proper alignment, give myofibrils elasticity and extensibility, and link myofibrils to sarcolemma and extracellular matrix
-Titin -Actinin -Myomesin -Nebulin -Dystrophin |
|
|
Myosin
|
Makes up thick filaments
A tail and two heads Bind to myosin binding sites on actin molecules of thin filaments during muscle contraction |
|
|
Actin
|
The main component of thin filaments
|
|
|
Tropomyosin
|
A component of thin filament
When the skeletal muscle is relaxed it covers myosin-binding sites on actin molecules to prevent myosin from binding to actin |
|
|
Troponin
|
Component of thin filament
When Ca ions bind to it, it changes shape, which moves tropomyosin away from myosin-binding sites on actin molecules |
|
|
Titin
|
Connects Z disc to M line of sarcomere
Stabilizes thick filament position Can stretch and then spring back unharmed |
|
|
Actinin
|
Protein of Z disc that attaches to actin molecules of thin filaments and to titin molecules
|
|
|
Myomesin
|
Forms M line of sarcomere
Binds to titin molecules and connects adjacent thick filaments to one another |
|
|
Nebulin
|
Wraps around the entire length of each thin filament
Helps anchor thin filaments to Z discs Regulates length of thin filaments during development |
|
|
Dystrophin
|
Links thin filaments of sarcomere to integral membrane proteins in sarcolemma
Helps reinforce sarcolemma and help transmit tension generated by sarcomeres to tendons |
|
|
4-Step Contraction
|
1.) Release of acetylcholine from synaptic vesicle
2.) Activation of ACh receptors 3.) Production of muscle action potential 4.) Termination of ACh activity (ACh is broken down) |
|
|
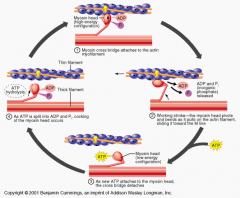
Sliding Filament Theory
|
1.) ATP hydrolysis: myosin heads hydrolyze ATP and become reoriented and energized
2.) Attachment of myosin to actin to form cross-bridges 3.) Power stroke: Myosin cross-bridges rotate towards the centre of sarcomere 4.) Detachment of myosin from actin: as myosin heads bind to ATP, the cross-bridges detach from actin |
|
|
Cross-bridges
|
When the myosin heads attach to actin during contraction
|
|
|
Role of Calcium in Contraction
|
An increase in Ca ion concentration in the sarcoplasm starts muscle contraction, and a decrease stops it
Stored inside the sarcoplasmic reticulum Binds with troponin |
|
|
Acetylcholine (ACh)
|
Neurotransmitter that's released because of the activation of a motor nueron
|
|
|
Acetylcholinesterase
|
Breaks down ACh after a short period of time (enzyme)
|
|
|
3 Sources of ATP
|
1.) Phosphagen System (stored ATP) 3 sec.
2.) Glycolysis (anaerobic respiration, no O2 available) 30-40 sec. 3.) Aerobic Respiration (krebs cycle, cellular respiration in the mitochondria, 36 mol. of ATP) min.-hours |
|
|
Motor Unit
|
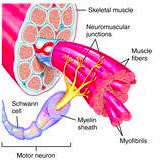
Consists of a somatic motor neuron plus all the skeletal muscle fibres it stimulates
A single one makes contact with an average of 150 skeletal muscle fibres All of the muscle fibres in one unit contract in unison |
|
|
Twitch Contraction Periods
|
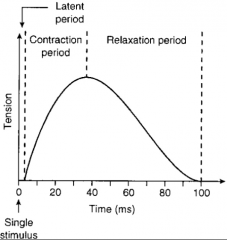
1.) Latent period: the delay (2 milliseconds)
2.) Contraction period: 10-100 milliseconds, Ca binds to troponin, myosin binding sites on actin are exposed, and cross-bridges form 3.) Relaxation period: 10-100 milliseconds, Ca is actively transported back into the sarcoplasmic reticulum, myosin-binding sites are covered by tropomyosin, myosin heads detach from actin, and tension in the muscle fibre decreases |
|
|
Unfused (incomplete) tetanus
|
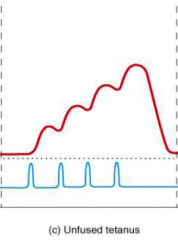
A skeletal muscle fibre is stimulated at a rate of 20-30 times per second
Can only partially relax between stimuli |
|
|
Fused (complete) tetanus
|
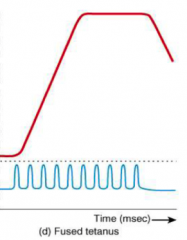
Skeletal muscle fibre is stimulated at a higher rate of 80-100 times per second
Does not relax at all Sustained contraction in which individual twitches cannot be detected |
|
|
Spasm
|
Sudden involuntary contraction of a single muscle within a large group of muscles
|
|
|
Cramps
|
Involuntary and often painful muscle contractions
Caused by inadequate blood flow to muscles, overuse and injury,or abnormal blood electrolyte levels |
|
|
Tremor
|
Rhythmic
|
|
|
Oxygen Debt
|
The added oxygen over and above the resting oxygen consumption that is taken into the body after exercise
Used to "pay back" or restore metabolic conditions to the resting level |
|
|
Functions of Blood
|
Transportation
Regulation Protection |
|
|
Plasma
|
91.5% water with dissolved solutes
Proteins: Albumins, globulins, fibrinogen |
|
|
Albumins
|
Major clotting proteins
Antibodies and Enzymes Synthesize in the liver Give rise to blood's viscosity Help maintain BP |
|
|
Globulins
|
Make up antibodies (gamma)
Carry bilirubin and steroids (alpha) Carry copper and iron (beta) Control blood osmotic pressure Act as carrier molecules |
|
|
Fibrinogen
|
Involved in blood clot formation
|
|
|
Hematocrit
|
The percentage of the total blood volume occupied by RBCs
|
|
|
Erythropoiesis
|
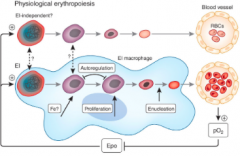
Production of RBCs
Increased in low levels of O2 |
|
|
Erythropoietin
|
Found in the kidneys and liver
Increases the number of RBC precursor cells to give rise to more RBCs |
|
|
Fibrinolysis
|
Dissolves small inappropriate clots
Once the clot isn’t needed it dissolves those clots too |
|
|
Development of Blood cells
|
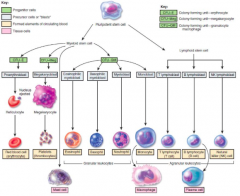
|
|
|
Blood Types
|
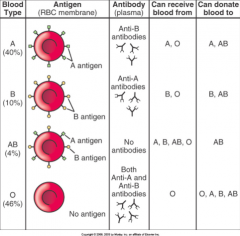
A, B, AB, O
|
|
|
Agglutination
|
The clumping of blood cells
|
|
|
Hemolysis
|
Getting the wrong type of blood
The rapid destruction of the donor red blood cells |
|
|
Anemia
|
Low percentage of RBCs or hemoglobin
Most often the result of low iron intake, hemolysis, autoimmune disease, blood loss, or lack of production in the bone marrow |
|
|
Polycythemia
|
The percentage of RBCs is abnormally high
The hematocrit may be 65% or higher |
|
|
Sickle Cell Disease
|
The RBCs contain HB-S, an abnormal kind of hemoglobin
The RBCs are sickle-shaped and rupture easily Leads to anemia |
|
|
Contraction and Relaxation in a skeletal muscle fibre
|
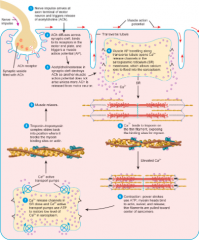
|
|
|
How long are RBCs in circulation for?
|
120 days
|
|
|
Formation and Destruction of RBCs
|
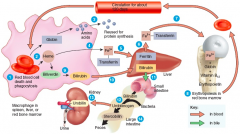
1.) Macrophages in spleen, liver or red bone marrow phagocytize old RBCs
2.) Globin and Heme are split apart 3.) Globin broken down into amino acids 4.) Iron removed from the heme and associates with transferrin 5.) Fe3+ detaches from transferrin and attaches to ferritin (iron-storage protein) 6.) Fe3+ reattaches to transferrin on release or absorption 7.) Fe3+ - transferrin complex is carried to red bone marrow where it is used for hemoglobin synthesis 8.) Erythropoiesis in red bone marrow results in the production of RBCs 9.) Non-iron portion of heme is converted to biliverdin and then into bilirubin 10.) Bilirubin enters the blood and is transported to the liver 11.) Bilirubin is released into bile and passes into the small and then large intestines 12.) In the large intestine bacteria convert bilirubin into urobilinogen 13.) Some urobilinogen is absorbed back into the blood and converted into a yellow pigment called urobilin and excreted in urine 14.) Most urobilinogen is eliminated in feces as a brown pigment called stercobilin |
|
|
Granular vs. Agranular WBCs
|
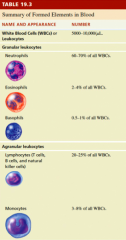
If the cells appear granulated when stained
|
|
|
Granular WBCs
|
Neutrophils (60-70%)
Eosinophils (2-4%) Basophils (0.5-1%) |
|
|
Agranular WBCs
|
Lymphocytes (20-25%)
Monocytes (3-8%) |
|
|
Neutrophils
|
Phagocytosis
Most abundant Nucleus has 2-5 lobes |
|
|
Eosinophils
|
Combats effectiveness of histamines
Allergic reactions Fights parasites Nucleus has 2 lobes |
|
|
Basophils
|
Inflammation response
Allergic reaction Least numerous Dark blue granules |
|
|
Lymphocytes
|
"Immune Response"
Specific to different antigens int he body Found in lymphoid tissues and lymph T-cells: immune response, destroys bacteria B-cells: develop into plasma cells to produce antibodies NK Cells: defenders, attack microbes |
|
|
Monocytes
|
Macrophages: wandering/fixed
Major histocompatibility antigens (MHC): proteins that protrude from the plasma membrane so the body can recognize them as foreign or not Cell communication |
|
|
Emigration
|
WBCs leaving the blood stream to collect where they’re needed
|
|
|
Chemotaxis
|
Signaling to bring phagocytes to the site where they’re needed
|
|
|
Platelet Formation
|
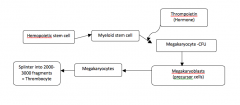
|
|
|
Thrombopoietin
|
Megakaryocyte growth and development hormone
Produced by the liver and kidneys |
|
|
Megakaryocytes
|
Huge cells that splinter into 2000-3000 fragments, each fragment being a platelet
|
|
|
Megakaryoblasts
|
The precursor cells to megakaryocytic
|
|
|
Chambers of the Heart
|
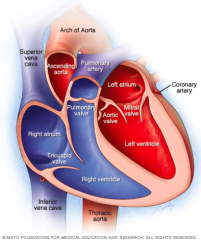
Right atrium: received deoxygenated blood from the vena cava
Right ventricle: pumps blood out of the heart to the lungs through the pulmonary arteries Left atrium: receives newly oxygenated blood from the lungs through the pulmonary veins Left ventricle: pumps blood to the body through the aorta |
|
|
Chordae Tendineae
|
Tendon-like cords connected to the valves
|
|
|
Papillary Muscles
|
Cone-shaped trabeculae carneae
Anchor the Chordae Tendineae |
|
|
Septum
|
Either interventricular or interartriular
Separates the chambers (ventricles or atria) |
|
|
The path of blood through the pulmonary and systemic circulations
|
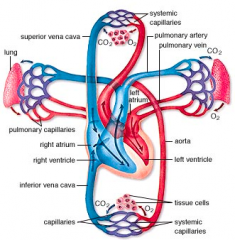
Right atrium
Tricuspid valve Right Ventricle Pulmonary Valve Pulmonary Trunk Pulmonary Arteries Pulmonary Capillaries Pulmonary Veins Left Atrium Bicuspid Valve Left Ventricle Aortic Valve Aorta Systematic Arteries Systematic Capillaries Systematic Veins Superior and Inferior Vena Cava Coronary Sinus Right atrium |
|
|
Heart Valves and how they work
|
Atrioventricular and Semilunar
Blood always flows from an area of high pressure to an area of low pressure The flow of blood operates the valves of the heart |
|
|
Atrioventricular Valves
|
Bicuspid and Tricuspid
|
|
|
Semilunar Valves
|
Aortic and Pulmonary
|
|
|
Stenosis
|
The narrowing of a heart valve
|
|
|
Murmur
|
Abnormal sounds in the heartbeat cycle
|
|
|
Myocardium
|
Separates the different chambers of the heart
|
|
|
Coronary Arteries
|
Supply blood to the heart tissue
|
|
|
Coronary Circulation
|
Only the innermost tissues lining the chambers of the heart can derive oxygen from the blood flowing through those chambers
Only during the relaxation phase |
|
|
Intercalated Discs
|
Connect the individual heart muscle cells
Thickening of the sarcomatic lining |
|
|
Gap Junctions
|
Allow direct transmission of the depolarizing current from cell to cell, across the chambers of the heart, so that the cells contract in unison
|
|
|
Desmosomes
|
Hold the cardiac muscle cells together
|
|
|
Order of impulse conduction in the heart
|
SA (sinoatrial) Node
AV (atrioventricular) Node AV Bundle Bundle Branches Purkinje fibres |
|
|
Sinoatrial Node
|
The 'Natural Pacemaker'
Sets the pace for the rest of the conduction |
|
|
Atrioventricular Node
|
Slows the signal down, allowing the atrium to mechanically move blood into the ventricles
|
|
|
Action Potential through the heart
|
step 1: Depolarization - threshold is reached and AP starts, opens Na+ gated channels (fast) and inflow into muscle fibre produced rapid depolarization
step 2: Plateau - maintains depolarization, Ca+2 gated channels (slow) open and inflow into cytosol through the sarcolemma into the cardiac fibre step 3: Repolarization: Recovery of Resting Membrane Potential, K+ gated channels are opened and outflow closes Ca+2 and Na+ channels |
|
|
Electrocardiogram (ECG)
|
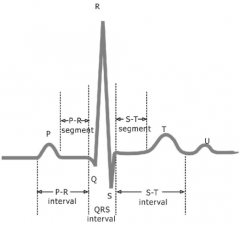
Recording of the electrical current as APs pass through the heart
P wave QRS Complex T wave |
|
|
P Wave
|
Atrial Depolarization
Small upwards deflection Contraction |
|
|
QRS Complex
|
Ventricular depolarization and atrial repolarization
Begins as a downward deflection, continues as a large upright triangular wave, and ends as a downward wave |
|
|
T Wave
|
Ventricular repolarization
Dome-shaped upward deflection Relaxation |
|
|
Diastole
|
Relaxing
|
|
|
Systol
|
Contraction
|
|
|
Heart Sounds
|
'lub' - louder and longer
'dup' - shorter and quieter |
|
|
Factors of Heart Rate
|
Hormones
Age Gender Fitness Temperature |

