![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
181 Cards in this Set
- Front
- Back
|
What are the structural components of a lymph node? |
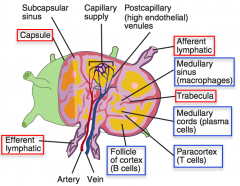
- Many afferents
- 1 or more efferents - Capsule - Trabeculae - Follicle - Medulla - Paracortex |
|
|
What is the function of lymph nodes?
|
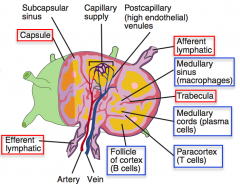
- Non-specific filtration by macrophages (medullary sinus)
- Storage of B cells (follicle) and T cells (paracortex) - Immune response activation |
|
|
Where in the lymph node are B cells localized and proliferating?
|
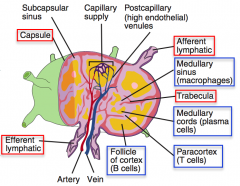
Follicle (outer cortex)
|
|
|
What are the types of follicles in a lymph node? Difference?
|
1° Follicle:
- Dense - Dormant 2° Follicle: - Pale central germinal centers - Active |
|
|
What are the components of the medulla of a lymph node?
|
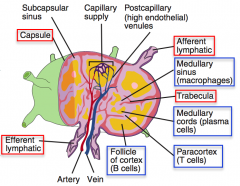
- Medullary cords (closely packed lymphocytes and plasma cells)
- Medullary sinuses (communicate with efferent lymphatics and contain reticular cells and macrophages) |
|
|
Where in the lymph node are plasma cells localized?
|
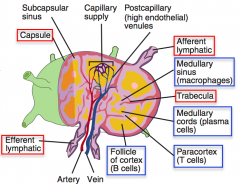
Medullary cords
|
|
|
Where in the lymph node are macrophages localized?
|
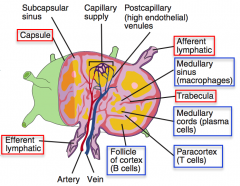
Medullary sinuses
|
|
|
Where in the lymph node are T cells localized?
|
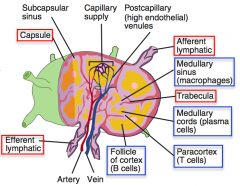
Paracortex (region of cortex between follicles and medulla)
|
|
|
What is in the Paracortex of lymph nodes?
|
- T cells (between follicles and medulla)
- Contains high endothelial venules (through which T and B cells enter from blood) |
|
|
How do T and B cells enter the lymph node from the blood?
|
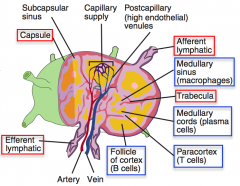
Via the high endothelial venules (in the paracortex)
|
|
|
Which part of lymph nodes is not well developed in patients with DiGeorge syndrome?
|
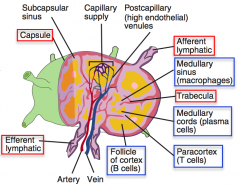
Paracortex (where T cells are housed)
|
|
|
Which part of the lymph node enlarges in an extreme cellular immune response (eg, viral infection)?
|
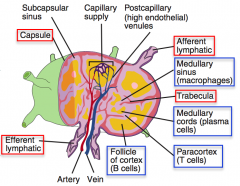
Paracortex
|
|
|
What are the lymph node clusters?
|
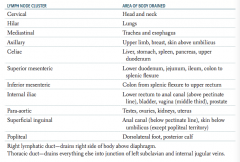
- Cervical
- Hilar - Mediastinal - Axillary - Celiac - Superior mesenteric - Inferior mesenteric - Internal iliac - Para-aortic - Superficial inguinal - Popliteal |
|
|
What part of the body is drained through the cervical lymph nodes?
|
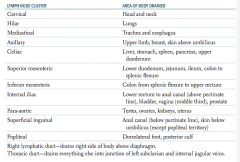
Head and neck
|
|
|
What part of the body is drained through the hilar lymph nodes?
|
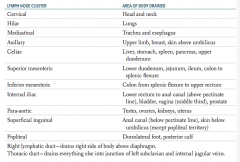
Lungs
|
|
|
What part of the body is drained through the mediastinal lymph nodes?
|
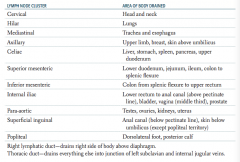
Trachea and esophagus
|
|
|
What part of the body is drained through the axillary lymph nodes?
|
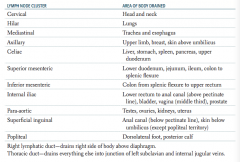
Upper limb, breast, skin above umbilicus
|
|
|
What part of the body is drained through the celiac lymph nodes?
|
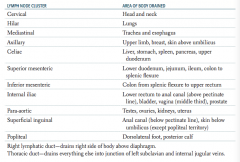
Liver, stomach, spleen, pancreas, upper duodenum
|
|
|
What part of the body is drained through the superior mesenteric lymph nodes?
|
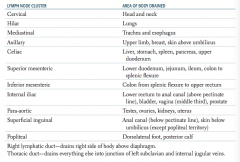
Lower duodenum, jejunum, ileum, colon to splenic flexure
|
|
|
What part of the body is drained through the inferior mesenteric lymph nodes?
|
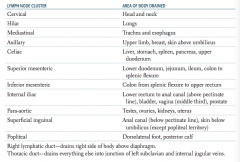
Colon from splenic flexure to upper rectum
|
|
|
What part of the body is drained through the internal iliac lymph nodes?
|
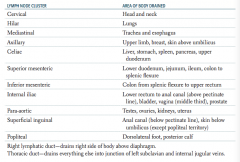
Lower rectum to anal canal (above pectinate line), bladder, vagina (middle third), prostate
|
|
|
What part of the body is drained through the para-aortic lymph nodes?
|
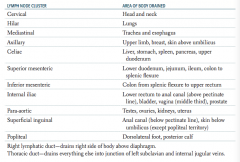
Testes, ovaries, kidneys, uterus
|
|
|
What part of the body is drained through the superficial inguinal lymph nodes?
|
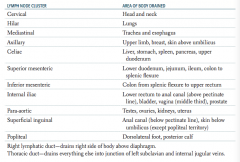
Anal canal (below pectinate line), skin below umbilicus (except popliteal territory)
|
|
|
What part of the body is drained through the popliteal lymph nodes?
|
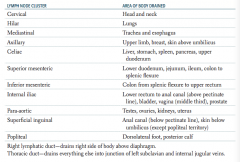
Dorsolateral foot, posterior calf
|
|
|
Which lymphatic duct drains the right side of the body above the diaphragm?
|
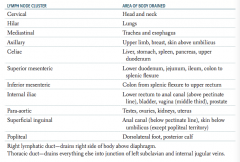
Right lymphatic duct
|
|
|
Which lymphatic duct drains the everything but the right side of the body above the diaphragm?
|
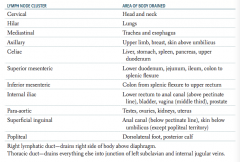
Thoracic duct - drains into the junction of the left subclavian and internal jugular veins
|
|
|
What is the appearance of sinusoids of the spleen? Location?
|
- Long, vascular channels in red pulp
- Fenestrated "barrel hoop" basement membrane |
|
|
What kind of cells are found near the sinusoids of the spleen?
|
Macrophages
|
|
|
What is the appearance of the basement membrane of sinusoids of the spleen?
|
Fenestrated "barrel hoop" basement membrane
|
|
|
Where are T cells found in the spleen?
|
Periarterial lymphatic sheath within the white pulp of the spleen
|
|
|
Where are B cells found in the spleen?
|
Follicles within the white pulp of the spleen
|
|
|
Where are Antigen Presenting Cells (APCs) found in the spleen?
|
Marginal zone - in between the red pulp and the white pulp - this is where APCs present blood-borne antigens
|
|
|
What is the function of macrophages in the spleen?
|
Remove encapsulated bacteria
|
|
|
What are the implications of splenic dysfunction (eg, post-splenectomy or in sickle cell disease)?
|
↓ IgM → ↓ complement activation → ↓ C3b opsonization → ↑ susceptibility to encapsulated organisms
|
|
|
What are the encapsulated organisms?
|
SHiNE SKiS:
- Streptococcus penumoniae - Haemophilus Influenzae type B - Neisseria meningitidis - Escherichia coli - Salmonella species - Klebsiella pneumoniae - Streptococci Group B |
|
|
What are the signs on peripheral blood smear of a patient with a splenectomy?
|
- Howell-Jolly Bodies (nuclear remnants)
- Target Cells - Thrombocytosis |
|
|
What happens in the thymus?
|
Site of T-cell differentiation and maturation
|
|
|
What is the origin of the thymus?
|
From epithelium of 3rd pharyngeal pouch
|
|
|
What is the origin of the lymphocytes in the thymus?
|
Mesenchymal origin
|
|
|
What are the contents of the thymus?
|
- Cortex: immature T cells
- Medulla: mature T cells and Hassall corpuscles containing epithelial reticular cells |
|
|
Which part of the thymus contains immature T cells?
|
Cortex of thymus (densely packed)
|
|
|
Which part of the thymus contains mature T cells?
|
Medulla of thymus (pale)
|
|
|
What is the location of Hassall corpuscles? What do they contain?
|
Medulla of thymus
- Contain epithelial reticular cells |
|
|
What cells/structures contribute to the innate immunity?
|
- Neutrophils
- Macrophages - Monocytes - Dendritic cells - Natural killer cells (lymphoid origin) - Complement |
|
|
What cells/structures contribute to the adaptive immunity?
|
- T cells
- B cells - Circulating antibodies |
|
|
How is the innate immunity encoded?
|
Germline encoded
|
|
|
How does microbial resistance differ between the innate and adaptive immunities over generations?
|
- Innate: resistance persists through generations, does not change within an organism's lifetime
- Adaptive: microbial resistance is not heritable |
|
|
How do you get variation of lymphocyte development?
|
V(D)J recombination
|
|
|
What is the general response of the innate immunity to pathogens? Timeline?
|
- Non-specific
- Occurs rapidly (minutes to hours) |
|
|
What is the general response of the adaptive immunity to pathogens? Timeline?
|
- Highly specific and refined over time
- Develops over long periods, memory response is faster and more robust |
|
|
Which type of immunity includes physical barriers? Examples?
|
Innate Immunity, physical barriers:
- Epithelial tight junctions - Mucus |
|
|
Which type of immunity includes secreted proteins? Examples?
|
Innate Immunity:
- Lysozyme - Complement - CRP - Defensins Adaptive: - Immunoglobulins |
|
|
What are the key features in pathogen recognition by the innate immunity?
|
Toll-Like Receptors (TLRs):
- Pattern recognition receptors that recognize Pathogen-Associated Molecular Patterns (PAMPs) - Eg: LPS (G-), Flagellin (bacteria), ssRNA (viruses) |
|
|
What are the key features in pathogen recognition by the adaptive immunity?
|
Memory Cells:
- Activated B and T cells - Subsequent exposure to a previously encountered antigen → stronger, quicker immune response |
|
|
What encodes MHC molecules?
|
HLA genes
|
|
|
What is the function of MHC I and II?
|
Present antigen fragments to T cells and bind TCRs
|
|
|
What HLA loci are associated with MHC class I?
|
- HLA-A
- HLA-B - HLA-C |
|
|
What HLA loci are associated with MHC class II?
|
- HLA-DR
- HLA-DP - HLA-DQ |
|
|
What do MHC class I bind?
|
T cell receptor and CD8
|
|
|
What do MHC class II bind?
|
T cell receptor and CD4
|
|
|
What cells express MHC class I?
|
All nucleated cells EXCEPT RBCs
|
|
|
What cells express MHC class II?
|
Only on Antigen Presenting Cells
|
|
|
What is the function of MHC class I?
|
Present ENDOGENOUSLY synthesized antigens (eg, VIRAL) to CD8+ CYTOTOXIC T cells
|
|
|
What is the function of MHC class II?
|
Present EXOGENOUSLY synthesized antigens (eg, BACTERIAL proteins, VIRAL capsid proteins) to CD4+ HELPER T cells
|
|
|
How does antigen get loaded on a MHC class I?
|
Antigen peptides loaded onto MHC I in RER after delivery via TAP peptide transporter
|
|
|
How does antigen get loaded on a MHC class II?
|
Antigen loaded following release of invariant chain in an acidified endosome
|
|
|
How do MHC molecules get transported to the cell surface?
|
- MHC I: β2-microglobulin
- MHC II: unknown |
|
|
What are the structural components of MHC class I?
|
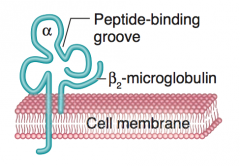
- Larger α chain that contains the peptide-binding groove
- β2-microglobulin |
|
|
What are the structural components of MHC class II?
|
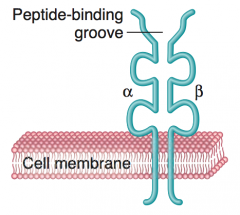
- Equivalent sided α and β chains
- Peptide-binding groove is between these chains |
|
|
Which disease(s) is/are associated with HLA-A3?
|
Hemochromatosis
|
|
|
Which disease(s) is/are associated with HLA-B27?
|
PAIR (aka seronegative arthropathies)
- Psoriatic arthritis - Ankylosing spondylitis - arthritis of Inflammatory bowel disease - Reactive arthritis (ie, Reiter syndrome) |
|
|
Which disease(s) is/are associated with HLA-DQ2/DQ8?
|
Celiac Disease
|
|
|
Which disease(s) is/are associated with HLA-DR2?
|
- Multiple Sclerosis
- Hay fever - SLE - Goodpasture syndrome |
|
|
Which disease(s) is/are associated with HLA-DR3?
|
- Diabetes Mellitus type 1
- SLE - Graves disease |
|
|
Which disease(s) is/are associated with HLA-DR4?
|
- Rheumatoid arthritis (4 walls in a room)
- Diabetes Mellitus type 1 |
|
|
Which disease(s) is/are associated with HLA-DR5?
|
- Pernicious anemia → Vitamin B12 deficiency
- Hashimoto thyroiditis |
|
|
What HLA subtype is associated with Hemochromatosis? What other diseases are associated with this HLA subtype, if any?
|
HLA-A3
|
|
|
What HLA subtype is associated with Psoriatic Arthritis? What other diseases are associated with this HLA subtype, if any?
|
HLA-B27
- Psoriatic Arthritis - Ankylosing Spondylitis - Arthritis of Inflammatory Bowel Disease - Reactive Arthritis (formerly Reiter Syndrome) |
|
|
What HLA subtype is associated with Ankylosing Spondylitis? What other diseases are associated with this HLA subtype, if any?
|
HLA-B27
- Psoriatic Arthritis - Ankylosing Spondylitis - Arthritis of Inflammatory Bowel Disease - Reactive Arthritis (formerly Reiter Syndrome) |
|
|
What HLA subtype is associated with Arthritis of Inflammatory Bowel Disease? What other diseases are associated with this HLA subtype, if any?
|
HLA-B27
- Psoriatic Arthritis - Ankylosing Spondylitis - Arthritis of Inflammatory Bowel Disease - Reactive Arthritis (formerly Reiter Syndrome) |
|
|
What HLA subtype is associated with Reactive Arthritis (ie, Reiter Syndrome)? What other diseases are associated with this HLA subtype, if any?
|
HLA-B27
- Psoriatic Arthritis - Ankylosing Spondylitis - Arthritis of Inflammatory Bowel Disease - Reactive Arthritis (formerly Reiter Syndrome) |
|
|
What HLA subtype is associated with Celiac Disease? What other diseases are associated with this HLA subtype, if any?
|
HLA-DQ2/DQ8
|
|
|
What HLA subtype is associated with Multiple Sclerosis? What other diseases are associated with this HLA subtype, if any?
|
HLA-DR2
- Multiple Sclerosis - Hay Fever - SLE - Goodpasture Syndrome |
|
|
What HLA subtype is associated with Hay Fever? What other diseases are associated with this HLA subtype, if any?
|
HLA-DR2
- Multiple Sclerosis - Hay Fever - SLE - Goodpasture Syndrome |
|
|
What HLA subtype is associated with SLE? What other diseases are associated with this HLA subtype, if any?
|
HLA-DR2
- Multiple Sclerosis - Hay Fever - SLE - Goodpasture Syndrome HLA-DR3 - Diabetes Mellitus type 1 - SLE - Graves Disease |
|
|
What HLA subtype is associated with Goodpasture Syndrome? What other diseases are associated with this HLA subtype, if any?
|
HLA-DR2
- Multiple Sclerosis - Hay Fever - SLE - Goodpasture Syndrome |
|
|
What HLA subtype is associated with Diabetes Mellitus Type 1? What other diseases are associated with this HLA subtype, if any?
|
HLA-DR3
- Diabetes Mellitus type 1 - SLE - Graves Disease HLA-DR4 - Rheumatoid Arthritis - Diabetes Mellitus type 1 |
|
|
What HLA subtype is associated with Graves Disease? What other diseases are associated with this HLA subtype, if any?
|
HLA-DR3
- Diabetes Mellitus type 1 - SLE - Graves Disease |
|
|
What HLA subtype is associated with Rheumatoid Arthritis? What other diseases are associated with this HLA subtype, if any?
|
HLA-DR4
- Rheumatoid Arthritis - Diabetes Mellitus type 1 |
|
|
What HLA subtype is associated with SLE? What other diseases are associated with this HLA subtype, if any?
|
HLA-DR4
- Rheumatoid Arthritis - Diabetes Mellitus type 1 |
|
|
What HLA subtype is associated with Pernicious Anemia (vitamin B12 deficiency)? What other diseases are associated with this HLA subtype, if any?
|
HLA-DR5
- Pernicious anemia → vitamin B12 deficiency - Hashimoto thyroiditis |
|
|
What HLA subtype is associated with Hashimoto thyroiditis? What other diseases are associated with this HLA subtype, if any?
|
HLA-DR5
- Pernicious anemia → vitamin B12 deficiency - Hashimoto thyroiditis |
|
|
What is the only lymphocyte member of the innate immune system?
|
Natural Killer Cells
|
|
|
What "weapons" do Natural Killer Cells use? Mechanism?
|
- Use perforin and granzymes to induce apoptosis of virally infected cells and tumor cells
- Also kills via antibody-dependent cell-mediated cytotoxicity (CD16 binds Fc region of bound Ig, activating NK cell) |
|
|
What enhances the activity of Natural Killer Cells?
|
- IL-2
- IL-12 - IFN-β - IFN-α |
|
|
What activates Natural Killer Cells?
|
Induced to kill when exposed to a non-specific activation signal on target cell and/or to an absence of class I MHC on target cell surface
|
|
|
How can antibodies mediate activation of Natural Killer Cells?
|
Antibody-Dependent Cell-Mediated Cytotoxicity:
- CD16 binds Fc region of bound Ig, activating the NK cells |
|
|
What are the major functions of B cells?
|
- Recognize antigen
- Produce antibody - Maintain immunologic memory |
|
|
What happens when a B cell recognizes an antigen?
|
Undergoes somatic hypermutation to optimize antigen specificity
|
|
|
How do B cells produce antibodies?
|
Differentiate into plasma cells to secrete specific immunoglobulins
|
|
|
What is the function of CD4+ T cells?
|
- Help B cells make antibody
- Produce cytokines to activate other cells of immune system |
|
|
What is the function of CD8+ T cells?
|
Kill virus-infected cells directly
|
|
|
What type of hypersensitivity reaction is mediated by T cells?
|
Delayed cell-mediated hypersensitivity (type IV)
|
|
|
What type of organ rejection are T cells involved in?
|
Both acute and chronic cellular organ rejection
|
|
|
What is the original form of the T cell? Location?
|
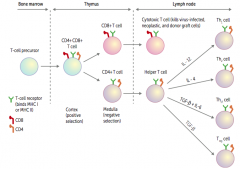
T-cell precursor located in bone marrow
|
|
|
What happens to the T-cell precursor in the bone marrow? Location?
|
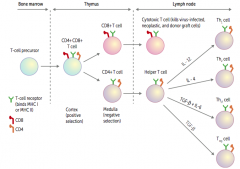
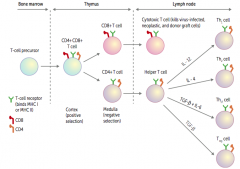
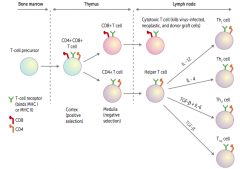
- Moves to cortex of thymus: contains both CD4 and CD8 markers (positive selection)
- Moves to medulla of thymus where it chooses to either be a CD4+ T cell or a CD8+ T cell (negative selection) |
|
|
Where does positive selection of T cells occur? What happens?
|
- Occurs in thymic cortex
- T cells expressing TCRs capable of binding surface self MHC molecules survive |
|
|
Where does negative selection of T cells occur? What happens?
|
- Occurs in thymic medulla
- T cells expressing TCRs with HIGH affinity for self antigens undergo apoptosis |
|
|
What happens to the CD8+ T cell in the thymus? Location?
|
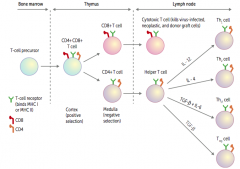
Travels to lymph node
- Becomes a cytotoxic T cell - Kills virus-infected, neoplastic, and donor graft cells |
|
|
What happens to the CD4+ T cell in the thymus? Location?
|
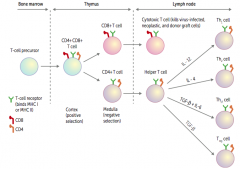
Travels to lymph node
- Becomes a helper T cell - Can either differentiate into Th1, Th2, Th17, Treg cells |
|
|
What causes a helper T cell to differentiate into a Th1 cell?
|
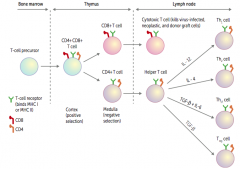
IL-12
|
|
|
What causes a helper T cell to differentiate into a Th2 cell?
|
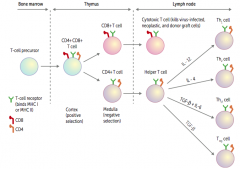
IL-4
|
|
|
What causes a helper T cell to differentiate into a Th17 cell?
|
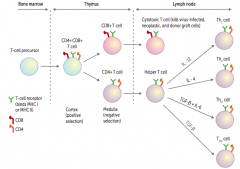
TGF-β and IL-6
|
|
|
What causes a helper T cell to differentiate into a Treg cell?
|
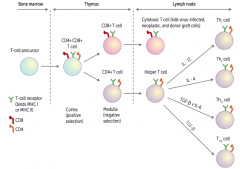
TGF-β
|
|
|
What is the effect of IL-12 on an undifferentiated Helper T cell?
|
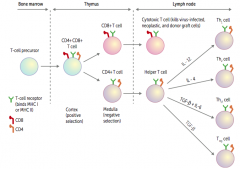
Differentiates into Th1 cell
|
|
|
What is the effect of IL-4 on an undifferentiated Helper T cell?
|
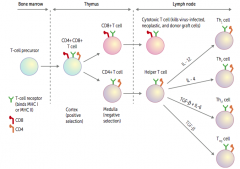
Differentiates into Th2 cell
|
|
|
What is the effect of TGF-β + IL-6 on an undifferentiated Helper T cell?
|
Differentiates into Th17 cell
|
|
|
What is the effect of TGF-β on an undifferentiated Helper T cell?
|
Differentiates into Treg cell
|
|
|
what are the types of antigen presenting cells?
|
- B cells
- Macrophages - Dendritic cells |
|
|
How many signals are required for T cell activation, B cell activation, and class switching?
|
Two signals
|
|
|
How is a naive helper T cell activated?
|
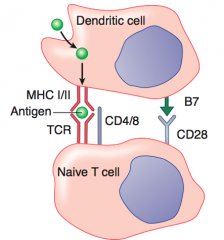
1. Foreign body phagocytosed by DC
2. Foreign Ag presented on MHC II → recognized by TCR on Th (helper) cell 3. "Costimulatory signal" given by interaction of B7 and CD28 4. Th cell activates and produces cytokines |
|
|
How is a naive cytotoxic T cell activated?
|
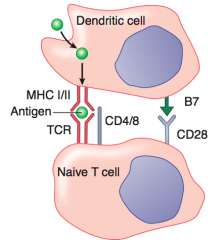
1. Foreign body phagocytosed by DC
2. Foreign Ag presented on MHC I → recognized by TCR on Tc (cytotoxic) cells 3. "Costimulatory signal" given by interaction of B7 and CD28 4. Tc cell activates and is able to recognize and kill virus-infected cell |
|
|
What are the first and second signals required for activation of Th cells?
|
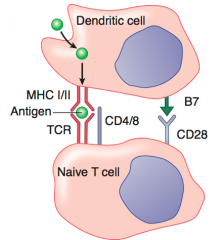
1. Foreign antigen on MHC II recognized by TCR
2. Costimulatory signal by interaction of B7 and CD28 |
|
|
What are the first and second signals required for activation of Tc cells?
|
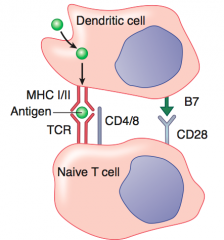
1. Foreign antigen on MHC I recognized by TCR
2. Costimulatory signal by interaction of B7 and CD28 |
|
|
How is a B cell activated? How does it undergo class switching?
|
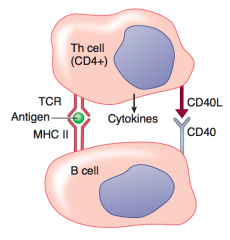
1. Helper T cell activated
2. B cell receptor mediated endocytosis; foreign antigen is presented on MHC II and recognized by TCR on Th cell 3. CD40 receptor on B cell binds CD40 ligand on Th cell 4. Th cell secretes cytokines that determine Ig class switching of B cell. |
|
|
What are the implications of an activated B cell?
|
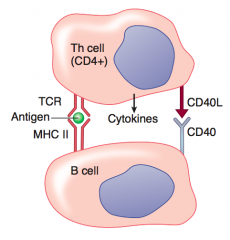
B cell activates and undergoes:
- Class switching - Affinity maturation - Antibody production |
|
|
What are the first and second signals required for activation of B cells?
|
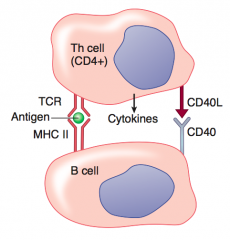
1. Recognition of Ag on MHC II by TCR on Th cell
2. CD40 receptor on B cell binds CD40 ligand on Th cell |
|
|
What do Th1 helper T cells secrete?
|
IFN-γ
|
|
|
What do Th2 helper T cells secrete?
|
- IL-4
- IL-5 - IL-6 - IL-13 |
|
|
What is the action of Th1 cells?
|
Activates macrophages and cytotoxic T lymphocytes (CTLs)
|
|
|
What is the action of Th2 cells?
|
- Recruits eosinophils for parasite defense
- Promotes IgE production by B cells |
|
|
What inhibits Th1 cells? Source?
|
IL-4 and IL-10 (from Th2 cells)
|
|
|
What inhibits Th2 cells? Source?
|
IFN-γ (from Th1 cells)
|
|
|
What mediator do macrophages secrete? Action?
|
- Release IL-12, which stimulates T cells to differentiate into Th1 cells
- Th1 cells secrete IFN-γ to stimulate macrophages |
|
|
What is the function of cytotoxic T cells?
|
Kill virus infected, neoplastic, and donor graft cells by inducing apoptosis
|
|
|
What do cytotoxic T cells release?
|
Preformed proteins:
- Perforin - helps to deliver the content of granules into target cell - Granzyme B - serine protease, activates apoptosis inside target cell - Granulysin - antimicrobial, induces apoptosis |
|
|
What is the function of Perforin? Source?
|
- Helps to deliver the content of granules into target cells
- From cytotoxic T cells |
|
|
What is the function of Granzyme B? Source?
|
- Serine protease, activates apoptosis inside target cells
- From cytotoxic T cells |
|
|
What is the function of Granulysin? Source?
|
- Animicrobial, induces apoptosis
- From cytotoxic T cells |
|
|
What is the function of regulatory T cells?
|
Help maintain specific immune tolerance by suppressing CD4 and CD8 T-cell effector functions
|
|
|
How do you identify Regulatory T cells?
|
Expression of cell surface markers:
- CD3 - CD4 - CD25 (α chains of IL-2 receptor) - Transcription factor FOXP3 |
|
|
What do activated regulatory T cells release? Action?
|
Produce anti-inflammatory cytokines: IL-10 and TGF-β
|
|
|
What part of the antibody recognizes antigens?
|
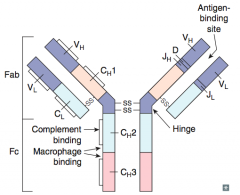
Variable part of L and H chains
|
|
|
Which antibodies fix complement? How?
|
IgM and IgG antibodies use their Fc portion to fix complement
|
|
|
What are the two parts of the antibody?
|
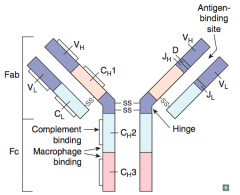
- Fc (contant) region
- Fab (antigen binding) region |
|
|
What contributes to the Fc fraction of the antibody?
|
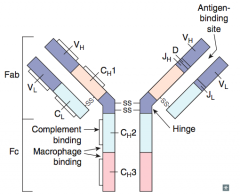
Only the heavy chains
|
|
|
What contributes to the Fab fraction of the antibody?
|
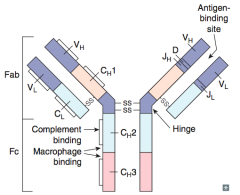
Both the heavy and light chains
|
|
|
What does the Fab fraction of the antibody determine?
|
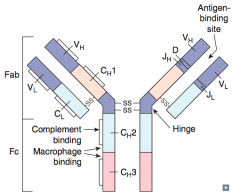
Antigen Binding Fragment:
- Determines idiotype: unique antigen-binding pocket - Only 1 antigenic specificity expressed per B cell |
|
|
What are the characteristics of the Fc portion of the antibody?
|
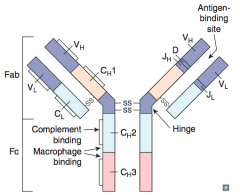
- Constant
- Carboxy terminal - Complement binding close to hinge (IgM and IgG) - Carbohydrate side chains - Determines isotype (IgM, IgD, etc) |
|
|
What part of the antibody determines the isotype (IgM, IgD, etc)?
|
Fc portion
|
|
|
How is antibody diversity generated?
|
- Random "recombination" of VJ (light-chain) or V(D)J (heavy-chain) genes
- Random combination of heavy chains with light chains - Somatic hypermutation (following Ag stimulation) - Addition of nucleotides to DNA during recombination by terminal deoxynucleotidyl transferase |
|
|
What recombination occurs in the light chains of antibodies to generate diversity?
|
VJ recombination
|
|
|
What recombination occurs in the heavy chains of antibodies to generate diversity?
|
V(D)J recombination
|
|
|
What occurs to an antibody following antigen stimulation to increase Ab diversity?
|
Somatic hypermutation
|
|
|
What additional change can occur during recombination to generate antibody diversity?
|
Addition of nucleotides to DNA during recombination by terminal deoxynucleotidyl transferase
|
|
|
What are the functions of antibodies?
|
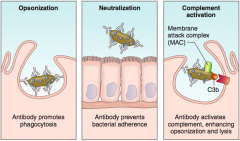
- Opsonization: antibody binding promotes phagocytosis
- Neutralization: antibody binding prevents bacterial adherence - Complement activation: antibody activates complement, enhancing opsonization and lysis |
|
|
What happens in "opsonization"?
|
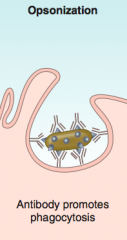
Antibody binding promotes phagocytosis
|
|
|
What happens in "neutralization"?
|
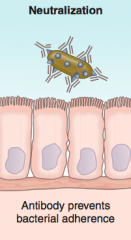
Antibody binding prevents bacterial adherence
|
|
|
What happens in "complement activation"?
|
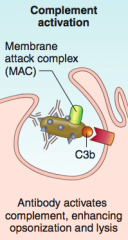
Antibody activates complement, enhancing opsonization and lysis (via membrane attack complex)
|
|
|
What immunoglobulins do mature B lymphocytes express on their surface?
|
IgM and IgD
|
|
|
What can happen to the IgM and IgD on the surfaces of mature B lymphocytes?
|
They may differentiate in germinal centers of lymph nodes by isotype swtiching (gene rearrangement) into plasma cells that secrete IgA, IgE, or IgG
|
|
|
What mediates isotype switching of mature B lymphocytes?
|
Mediated by cytokines and CD40 ligand
|
|
|
What is the main antibody in primary (immediate) response to an antigen? Secondary (delayed) response to an antigen?
|
- Primary / immediate: IgM
- Secondary / delayed: IgG |
|
|
What is the most abundant immunoglobulin isotype in the serum?
|
IgG
|
|
|
What are the actions of IgG?
|
- Secondary (delayed) response to antigen
- Fix complement - Cross placenta (provides infant w/ passive immunity) - Opsonize bacteria - Neutralize bacterial toxins and viruses |
|
|
What are the actions of IgA?
|
- Prevents attachment of bacteria and viruses to mucus membranes
- Does not fix complement - Picks up secretory component from epithelial cells before secretion |
|
|
What is the structure of IgA depending on location?
|
- Monomer in circulation
- Dimer when secreted |
|
|
What is the most produced antibody? Why is it not the most abundant isotype in the serum?
|
IgA - released in secretions (tears, saliva, mucus) and early breast milk (colostrum)
|
|
|
How does IgA cross epithelial cells?
|
Transcytosis
|
|
|
What are the actions of IgM?
|
- Fixes complement
- Primary / immediate response to antigen - Antigen receptor on surface of B cells |
|
|
What is the organization of IgM depending on location?
|
- Monomer on B cell
- Pentamer when secreted (allows for efficient trapping of free antigen out of tissue while humoral response evolves) |
|
|
What are the actions of IgD?
|
Unclear function
|
|
|
What is the location of IgD?
|
Found on the surface of many B cells and in the serum
|
|
|
What are the actions of IgE?
|
- Binds mast cells and basophils
- Cross-links when exposed to allergen, mediating immediate (type I) hypersensitivity through release of inflammatory mediators such as histamine - Mediates immunity to worms by activating eosinophils |
|
|
What immunoglobulin has the lowest concentration in the serum?
|
IgE
|
|
|
What are the types of antigens?
|
- Thymus independent antigens
- Thymus dependent antigens |
|
|
What is a thymus independent antigen?
|
- Antigens lacking a peptide component (eg, lipopolysaccharides from G- bacteria)
- Antigens cannot be presented by MHC to T cells |
|
|
What is a thymus dependent antigen?
|
- Antigen that contains a protein component (eg, diphtheria vaccine)
- Can be presented to MHC to T cells |
|
|
Relatively how immunogenic are thymus-independent antigens (lacking a peptide component)?
|
Weakly or non-immunogenic
|
|
|
What are the characteristics of boosters for thymus-independent antigens?
|
Vaccines often require boosters (eg, pneumococcal polysaccharide vaccine)
|
|
|
What causes class switching and immunologic memory?
|
Direct contact of B cells with Th cells (CD40 - CD40 ligand interaction)
|

