![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
1399 Cards in this Set
- Front
- Back
|
pituitary adenomas
|
<1cm --> microadenoma
>1cm macroadenoma and associated with panhypopituitarism and visual symptoms prolactin 50-60%; GH 15-20%; ACTH 10-15%; LH/FSH 10-15% |
|
|
hyperprolactinemia definition
|
excess prolactin release results in galactorrhea-amenorrhea syndrome
prolactin inhibits the LH surge that causes ovulation by inhibition of hypothalamus (LHRH) which results in the amenorrhea possible but rare in males |
|
|
hyperprolactinemia etiology
|
physiologic causes: pregnancy, early nursing, hypoglycemia, seizure, exercise, stress, sleep, nipple stimulation; prolactinoma; block of pituitary stalk and dopamine by tumors, cranippharyngioma, meningioma, dysgerminoma, empty sella, trauma; pharmacologic causes: dopamine synthesis blockers (phenothiazines, metoclopramide), dopamine-depleting agents (methyldopa, reserpine), tricyclics, narcotics, cocaine, SSRIs, risperidone; also high TRH due to primary hypothyroidism stimulates prolactin (always check TSH)
|
|
|
hyperprolactinemia clinical presentation
|
women: galactorrhea, menstrual abnormalities, osteoposoris, osteopenia, infertility, gynecomastia
men: hypogonadism, erectile dysfunction, decreased libido, gynecomastia, infertility |
|
|
hyperprolactinemia diagnosis
|
exclude pregnancy, lactation, hypothyroidism and medications
prolactinomas may co-secrete GH normal basal fasting PRL level is <20mg/L >100ng/mL in nonpregnant --> probable pituitary adenoma --> MRI of pituitary |
|
|
hyperprolactinemia management
|
1st line: cabergolide or bromocriptine (reduces prolactin to <10% of pre-treatment levels)
if no response or compressive neurologic symptoms --> surgery only 30% of macroadenomas can be resected and >50% recurr |
|
|
acromegaly etiology
|
GH-secreting pituitary adenomas (75% are macroadenomas); rarely ectopic GH or GHRH-secreting tumors
|
|
|
acromegaly clinical presentation
|
enlargement of hands and feet, coarse facial features, thick skin folds; shoe, hat, glove, ring size increase; prognathism and separation of teeth; deeper voice; increased sweating; obstructive sleep apnea; visceromegaly, osteoarthritis, entrapment neuropathy; menstrual problems (prolactin is co-secreted); 30% get cardiac pathologies (cardiomyopathy, hypertension, arrythmia, hypertrophy, diastolic dysfunction, premature atherosclerosis); impaired glucose tolerance (80%), diabetes (13-20%), hypertension (33%), joint disease (articular cartilage proliferation)
|
|
|
acromegaly diagnosis
|
Initial test: IGF-1 levels
confirmation: GH level >5ng/mL after glucose load (should supress GH) if GH excess is confirmed --> MRI (detects tumor in 90%) or CT to localize tumor |
|
|
acromegaly management
|
1st line --> surgery
2nd line --> octeotride (↓GH in 66%) bromocriptine/carbegolide (↓GH in 25%) pegvisomant (GH analog receptor antagonist) 3rd line --> radiotherapy surgery and radiotherapy can result in hypopituitarism (10-20%) |
|
|
acromegaly complications
|
tumor pressure or rupture into brain or sinuses
cardiac failure (MCCOD) diabetes mellitus cord compression visual defects |
|
|
hypopituitarism etiology
|
Tumors:
pituitary adenomas, cysts, hypothalamic tumors (craniopharyngioma, meningioma, glioma); Inflammatory: sarcoidosis, TB, syphilis, eosinophilic granuloma, autoimmune lymphocytic hypophysitis Vascular: Sheehan postpartum necrosis, pituitary apoplexy, hemochromatosis, amyloidosis, CVA/stroke Other: trauma, radiation, surgery, infections, hypoxia |
|
|
hypopituitarism presentation
|
defficiencies in order
gonadotropin deficiency (amenorrhea, genital atrophy/impotence, infertility, decreased libido, loss of axillary and pubic hair) GH deficiency (maybe assymptomatic, hypersensitivity to insulin, hyperlipidemia, short stature in children) TSH deficiency ( hypothyroidism, fatigue, weakness, hyperlipidemia, cold intolerance, dry skin, no goiter) ACTH deficiency (secondary adrenal insuficiency, hypocortisolism, fever, hypotension, hyponatremia [minimal], decreased response to stress, weightloss) |
|
|
hypopituitarism diagnosis
|
measure hormones:
GH --> insulin-induced hypoglycemia ↓ glucose to <40mg/dL which ↑ GH > 10mg/L - if <10mg/L there is deficiency; or arginine infusion; ACTH --> insulin tolerance test should increase plasma cortisol to > 19mg/dL or metyrapone test should suppress cortisol and increase serum ACTH, failure indicates deficiency; measure LH, FSH, estrogen/testosterone TSH --> low T4/T3 levels with normal to low TSH |
|
|
hypopituitarism management
|
treat underlying cause; hormone replacement therapy specially cortisol
|
|
|
Empty sella syndrome (ESS)
|
herniation of suprasellar subarachnoid space through diaphragm; no pituitary seen on MRI or CT; can be idiopathic or secondary to trauma or radiotherapy; presentation: obesity, multiparoous women, headeache and 30% will have hypertension; therapy is reassurance.
|
|
|
diabetes insipidus definition
|
disorder of the neurohypophyseal system (hypothalamus or neurohypophisis) results in ADH deficiency (central DI); or renal resistance to the action of ADH (nephrogenic DI)
|
|
|
central diabetes insipidus etiology
|
neoplastic/infiltrative lessions in hypothalamus or pituitary (60% have adenohypophisis deficiency):
Craniopharyngiomas Encephalitis Meningitis Trauma Tuberculosis Radiotherapy Adenomas Anoxia Leukemia Histocytosis Hypertension Idiopathic syphillis surgery "CEMTTRAAL HHIgh" |
|
|
nephrogenic diabetes insipidus etiology
|
Demeclocycline
Idiopathic Sickle cell Sarcoidosis Sjogren Colchicine Lithium Amyloidosis Myeloma Pyelonephritis or secondary to hypercalcemia, hypokalemia "DIureSSSis CLAMP" |
|
|
diabetes insipidus presentation
|
polyuria, polydipsia, hypernatremia, urine specific gravity <1,010, severe dehydration, weakness, fever, altered mental state, prostration, nocturia
|
|
|
diabetes insipidus diagnosis
|
plasma/urine osmolarity ratio falls to the right of shaded area
then if vasopressin response is normal --> central diabetes insipidus, else nephrogenic |
|
|
diabetes insipidus differential
|
primary polydipsia
drug-induced polydipsia from chlorpromazine, anticholinergics, thioridazine hypothalamic disease |
|
|
diabetes insipidus management
|
CDI: ADH hormone replacement or ADH secretion stimulators (chlorpropamide, clofibrate, carbamazepine)
NDI: HCTZ or amiloride or chlortalidone as well as correction of calcium balance |
|
|
SIADH etiology
|
cancer: small cell lung CA, pancreas CA, ectopic ADH secretion
infections: TB, lung abscess CNS: head injury, CVA, encephalitis drugs: chlorpropamide, clofibrate, vincristine, vinblastine, cyclophosphamide, carbamazepine "inappropriate CCCCCancer VVIBE" Cancer, 4 C drugs, 2 V drugs, Infections, Brain, Ectopic |
|
|
SIADH presentation
|
water retention
ECF expansion without edema or hypertension (natriuresis) hyponatremia concentrated urine signs of cerebral edema when hyponatremia is severe (irritability, confusion, seizures, coma) |
|
|
SIADH diagnosis
|
high ADH is most accurate test
hyponatremia <130mEq/L urine sodium > 20mEq/L; maintained hypervolemia ↓RAA low electrolytes in blood (BUN, creatinine, uric acid) low albumin |
|
|
SIADH management
|
treat underlying cause
fluid restriction to 800-1000mL/d demeclocycline (AVP inhibitor) in case of cerebral edema: hypertonic 3% saline 200-300mL IV in 3-4h |
|
|
hyperthyroidism etiology
|
Graves (toxic diffuse goiter)(most common)
hyperfunctioning adenoma, Plummer disease (toxic multinodular goiter) amiodarone excess TSH (rare) transient hyperthyroidism due to subacute thyroiditis (painful) lymphocytic thyroiditis (painless) thyrotoxicosis factitia ectopic thyroid tissue (struma ovarii, functioning follicular CA) |
|
|
hyperthyroidism presentation
|
Cardiac:
atrial fibrillation, dyspnea, palpitations, angina, heart failure Adrenergic: nervousness, insomnia, irritability, tremors, frequent bowel movements, excessive sweating, heat intolerance, warm moist skin Metabolic: weight loss, weakness, palmar erythema, oligomenorrhea, osteoporosis/hypercalcemia Eye: Staring, infrequent blinking, lid lag Graves has diffuse goiter + exopthalmus + dermopathy-pretibial myxedema and may be associated with PA, MG or DM "CAME" |
|
|
hyperthyroidism diagnosis
|
history and PE plus lab confirmation:
TSH (↓ in primary, ↑ in secondary) ↑ free T4/T3 ↑RAIU TSI in Graves ↑ anti-thyroglobulin and antimicrosomal Ab in Graves and Hashimoto's |
|
|
hyperthyroidism differential
|
Pheochromocytoma
Acromegaly Cardiac (A fib) Mania Myasthenia Anxiety Neurosis MG and orbital tumors can cause opthalmoplegia and exopthalmus if primary, need to specify Graves or thyroiditis "hyperthyroid PACMMAN" |
|
|
hyperthyroidism management
|
immediate: propranolol, PTU, methimazole (can cause agranulocytosis)
later: radioactive iodine ablative therapy or thyroidectomy if 2nd trimester pregnancy, children or compressive symptoms levothyroxine hormone replacement may be needed to avoid hypothyroidism |
|
|
thyroid storm presentation
|
endocrine emergency precipitated by stress, infection, surgery, trauma; presents with:
Tachychardia Hypotension Hot (fever) Vomiting Restlessness Irritability Icteric Coma Diarrhea Dehydration Delirium "Thyroid HHVRIICaneD" |
|
|
thyroid storm management
|
saline/glucose hydration, oxygen, cooling blanket;
1. PTU, 100mg every 2h 2. iodine (inhibits hormone release) 3. propranolol 4. dexamethasone (inhibits hormone release, impairs peripheral generation of T3 and adrenal support) PTU blocks uptake of RAI and should be stopped 1-2 weeks before and after RAIU treatment |
|
|
hypothyroidism etiology
|
95% primary:
Congenital defects Lithium Aspirin Amiodarone Surgery (postablative) Sulfonamides Iodine (radioactive and deficiency) Interferon Hashimoto (MCC) also secondary (pituitary) and tertiary (hypothalamus) "hypothyroidism due to CLAASSIIc Hashimoto" |
|
|
hypothyroidism presentation in newborn
|
Cretinism
Cry hoarsely Coarse features Constipation Retardation (mental and skeletal) Eating problems Eyes widely set Tongue protruding Teeth problems Nose broad and flat Sommnolence Sparse hair Skin is dry Jaundice Abdomen protrudes with umbilical hernia Milestones delayed Migit (dwarfism) "CCCCREETTiNSS JAM" |
|
|
hypothyroidism presentation in adult
|
lethargy, constipation, cold intolerance, mental dullness, anorexia with weight increase, dry skin and hair, deep hoarse voice, myxedema, slow tendon reflexes with prolonged relaxation, pale cool dry skin
hypercholesterolemia, expressionless face, sparse hair, periorbital puffiness, macroglosia, hypokinesis, deafness, hyponatremia, anemia, stiffness, muscle cramps, carpal tunnel syndrome, menorrhagia, |
|
|
hypothyroidism diagnosis
|
history and PE plus lab confirmation:
↑ TSH (primary) or normal/↓ TSH (secondary) ↓T4 and FT4 ↓ T3 also may have hypercholesterolemia ↑ CPK ↑ AST hyponatremia ↑ LDH and 12% have PA |
|
|
hypothyroidism management
|
gradual metabolic restoration with levothyroxine (monitor TSH/T3); if suspicion of 2dary or 3ary give hydrocortisone first then hormone replacement; if myxedema coma signs (respiratory depression and ↑CO2 retention) use very high doses of T4 and T3
|
|
|
subacute thyroiditis
|
also called granulomatous or De Quervain; viral etiology
presents with upper respiratory symptoms plus painful enlarged and firm thyroid lab confirmation is made by ↑ ESR, ↓ RAIU and initial ↑ of T3/T4 then ↓ symptomatic management: aspirin, prednisone, propanolol differential: Graves (there's ↑ RAIU); subsides to normal function |
|
|
Hashimoto etiology
|
chronic autoimmune lymphocytic infiltration of the thyroid with antimicrosomal and antithyroglobulin antibodies
|
|
|
Hashimoto presentation
|
painless asymmetrical nontoxic goiter of firm/rubbery consistency with signs and symptoms of hypothyroidism
|
|
|
Hashimoto diagnosis
|
history and PE
confirmation with needle biopsy labs: normal or ↑ TSH normal or ↓ T4/T3 antimicrosomal antithyroglobulin antiperoxidase antibodies |
|
|
Hashimoto management
|
levothyroxin hormone replacement
|
|
|
Lymphocytic thyroiditis
|
self-limiting episode of thyrotoxicosis associated with chronic lymphocytic thyroiditis
thyroid is nontender, firm, symemetrical and slightly enlarged normal ESR, ↑T4/T3, ↓RAIU antithyroid antibodies may be present but in low titer; its recurrent symptomatic treatment with propranolol |
|
|
Reidel thyroiditis
|
intense fibrosis and enlargement of the thyroid
surgery is needed associated with mediastinal and retroperitoneal fibrosis |
|
|
thyroid adenomas
|
may be nonfunctioning or hyperfunctioning
slow growth types are follicular (most common), papillary and Hurthle treat with ablation surgery or RAI |
|
|
papillary thyroid carcinoma
|
most common and differentiated
more common in women, bimodal frequency slow growing; lymphatic spread psamomma bodies seen in X-rays treat with surgery alone (small) or surgery + radiotherapy and also TSH suppression with levothyroxine |
|
|
follicular thyroid carcinoma
|
2nd most common
more frequent in elderly women hematogenous spread with metastasis to lung and bone total thyroidectomy with postoperative ablative radiation |
|
|
anaplastic thyroid carcinoma
|
3rd most common; more frequent in elderly women; highly malignant with rapid and painful enlargement; 80% die in 1 year of diagnosis; direct spread
|
|
|
medullary thyroid carcinoma
|
least common
arises from parafollicular cells and produces calcitonin associated with MEN IIa and MEN IIb thyroidectomy is indicated differentiate paraneoplastic calcitonin production in lung, breast, pancreas and colon cancer |
|
|
thyroid cancer diagnosis
|
recent growth of thyroid mass with nontenderness or hoarseness
solitary nodule, ↑ calcitonin, x-ray calcifications or increased density suggest malignancy first test is TSH if normal TSH --> FNA procedure (preferred) or scintillation scanning functioning nodules are most likely adenomas while nonfunctioning nodules are malignant in 20% of cases; ultrasound is usefull to distinguish cyst from solid nodule |
|
|
metabolism of calcium
|
regulated by PTH via osteoclast activation, vitamin D activation and distal tubule reabsorption; 80% of ingested calcium is excreted, 20% absorbed; 2% of total calcium is in blood 50% free, 40% protein-bound and 10% bound to citrate or phosphate buffers
|
|
|
hyperparathyroidism etiology
|
most common is primary hyperPTH
malignancies (lung) produce PTH-like peptide granulomatous diseases (sarcoidosis, TB, berylliosis, histoplasmosis) vitamin D intoxication thiazides lithium Paget disease acidosis |
|
|
hyperparathyroidism presentation
|
CONfusion
CONstipation Nephrolithiasis Anorexia Nausea Pancreatitis Polyuria Polydipsia Hypertension (30-50%) short QT wave, ulcers, lethargy "CONstANt PPPtH" |
|
|
hyperparathyroidism management
|
Fluid replacement, furosemide (loop diuretics), biphosphonates (alendronate)
calcitonin if can't wait 2 days for biphosphonates to make effect |
|
|
primary hyperparathyroidism etiology
|
one gland adenoma (80%), gland hyperplasia (20%), MEN I or II
|
|
|
primary hyperparathyroidism presentation
|
Pancreatitis
Peptic ulcer Polyuria Polydipsia Psychiatric disorders Nephrocalcinosis Stones Osteitis fibrosa cystica Fatigability Constipation hypertension short QT arrhythmia "PaNS OF Calcium" osteitis fibrosa cystica: bone pain, fractures, deformities, localized demineralization, bone cysts, brown tumors |
|
|
primary hyperparathyroidism management
|
parathyroidectomy if symptoms of hypercalcemia, bone disease, renal disease, pregnancy
medical RX if calcium <11.5mg/dL: biphosphonates, restriction of dietary calcium, oral hydration, phosphate supplements emergency RX: IV normal saline, furosemide, IV biphosphonates and calcitonin if rapid effect is necessary |
|
|
secondary hyperparathyroidism management
|
cinacalcet: calcimimetic agent shuts off parathyroids; used in secondary hyperPTH caused by hemodialisis and parathyroid OA
|
|
|
hypocalcemia etiology
|
hypoparathyroidism
renal failure hyperphosphatemia hypomagnasemia alkalosis low albumin levels (pseudo hypocalcemia) massive blood transfusion |
|
|
hypocalcemia presentation and RX
|
neural hyperexcitability (seizures, tetany, numbness, tingling), prolonged QT arrhythmia; treat with calcium and vitamin D supplementation
|
|
|
hypoparathyroidism etiology
|
most common is surgical removal of parathyroids
hypomagnesemia, hereditary note: chronic renal failure and low vitamin D produce high levels of PTH but signs and symptoms of hypocalcemia. |
|
|
hypoparathyroidism presentation
|
neuromuscular irritability
tetany laryngospasm cramps seizures Chevostek Trousseau QT prolongation arrhythmia refractory CHF hyperventilation worsens hypoPTH due to alkalosis |
|
|
hypoparathyroidism diagnosis
|
signs and symptoms
low serum calcium or albumin suggests hypoPTH preferable to measure ionized calcium PTH may be high or low |
|
|
hypoparathyroidism management
|
acute: calcium gluconate IV
maintenance: oral calcium, vitamin D and phosphate binders if hyperphosphatemia |
|
|
diabetes etiology
|
type I: genetically susceptible autoimmune destruction of beta cells following viral infection
type II: unknown but theres abnormal insulin secretion and resistance to insulin |
|
|
diabetes presentation
|
polyuria
polydipsia polyphagia hyperglycemia ketoacidosis or hyperosmolar coma signs and symptoms of complications may exist |
|
|
diabetes diagnosis
|
random plasma glucose >200mg/dL plus symptoms or 2 fasting plasma glucose >126mg/dL; glucose tolerance test may be required to show >200mg/dL at 2h and at least one earlier sample; HgA1c >7% suggests diabetic patient has been noncompliant with treatment for the previous 8-12 weeks
|
|
|
type II diabetes management
|
patient education, weight reduction, low fat diet and physical activity
if this fails to keep HgA1c below 7% then drugs; 1st line: sulfonylurea (thin patients) or metformin (obeese patients); 2nd line: add sulfonylurea or metformin; 3rd line: add glitazone or switch to insulin 0.5U/kg; |
|
|
diabetes complications
|
acute: DKA or HONK
chronic: myocardial infarction (#1 cause of death in diabetics) hyperlipidemia diabetic nephropathy (#1 cause of chronic renal failure) diabetic retinopathy gastroparesis erectile dysfunction diabetic foot neuropathy |
|
|
diabetic ketoacidosis presentation
|
Kussmaul respiration
Acidosis Anorexia Abdominal pain Consciousness altered Dehydration Vinegar breath Vomiting and hyperkalemia "Keto AAACiD & Vinegar" |
|
|
diabetic ketoacidosis diagnosis
|
signs and symptoms plus elevated plasma glucose, elevated levels of acetoacetate and hydroxybutirate, metabolic acidosis and increased anion gap
|
|
|
diabetic ketoacidosis management
|
insulin bolus with 5-10 units; potassium if plasma levels <4 mEq/L; fluid and electrolyte replacement
|
|
|
hyperosmolar nonketotic coma presentation
|
Water (profound dehydration)
Weakness Polyuria Polydipsia Confusion Coma SEizures lethargy "WWeePPing CCOMAtoSE" |
|
|
hyperosmolar nonketotic coma diagnosis
|
elevated plasma glucose (1000 mg/dL)
extremely high serum osmolality high BUN mild metabolic acidosis (bicarbonate around 20 mEq/L) without ketosis |
|
|
hyperosmolar nonketotic coma management
|
high-volume fluid and electrolyte replacement + insulin
|
|
|
myocardial infarction risk in diabetes
|
#1 cause of death in diabetics (75%); for every 1% reduction in HgA1c there's 14% risk reduction; for every 10 point decrease in blood pressure there's additional 12% risk reduction
|
|
|
lipid management in diabetics
|
target LDL is <100mg/dL
if 100-130mg/dL: recommend diet, exercise and consider statin if >130mg/dL statin is recommended |
|
|
diabetic nephropathy
|
affects 30-40% of type I and 20-30% of type II diabetics
diffuse membrane and mesangial thickening is most common nodular glomerulosclerosis is also common (Kimmelstiel-Wilson syndrome) screen for proteinuria annually proteinuria is >300mg of albumin in 24 hour urine microalbuminuria is first stage and between 30-300mg all diabetics with proteinuria should be given ACE inhibitor or ARB |
|
|
diabetic retinopathy
|
screen type II diabetics at diagnosis and annually thereafter
screen type I diabetics 5 years after diagnosis and annually thereafter proliferative retinopathy shows vitreous hemorrhages and/or neovascularization and is treated with laser photocoagulation |
|
|
diabetic gastroparesis and erectile dysfunction
|
treat gastroparesis with metoclopramide or erythromycin
50% of diabetics have erectile dysfunction after 10 years, treat with sildenafil |
|
|
diabetic foot
|
due to trauma and infection in presence of diabetic neuropathy
podiatric examination annually responsible for 50% of nontraumatic amputations |
|
|
diabetic neuropathy
|
peripheral neuropathy: most common, symmetrical, numbness, paresthesia, pain, absent reflexes, loss of vibratory sense (treat with gabapentin (best), pregabalin (best), analgesics, amitriptyline, carbamazepine)
mononeuropathy: sudden foot drop, wrist drop or paralysis of III, IV or VI nerves autonomic neuropathy: orthostatic hypotension, syncope, gastroparesis and constipation or diarrhea, bladder dysfunction and urinary retention, impotence and retrograde ejaculation |
|
|
hypoglycemia presentation
|
excessive secretion of epinephrine (sweating, tremor, tachychardia, anxiety, hunger); dysfunction of CNS (dizziness, headache, clouded vision, loss of fine motor skills, confusion, seizures, coma)
|
|
|
posprandial hypoglycemia
|
due to alimentary hyperinsulinism after gastrectomy, vagotomy, etc…; idiopathic or galactosemia
|
|
|
fasting hypoglycemia
|
underproduction of glucose due to hormone deficiencies (panhypopituitarism, adrenal insufficiency), enzyme defects, malnutrition, late pregnancy, acquired liver disease, alcohol, propanolol, salicylates, hyperinsulinism (insulinoma, exogenous insulin, sulfonylureas, quinine, endoteoxic shock, autoimmune insulin receptor antibodies)
|
|
|
insulinoma
|
subacute or chronic hypoglycemia causes blurred vision, headache, slurred speech, weakness
diagnosis: serum insulin level > 8mg/mL with blood glucose <40mg.dL CT, ultrasound or arteriography to localize tumor surgical, diet and medical treatment |
|
|
factitious hyperinsulinism
|
due to self-administration of insulin, Equal or sulfonylureas
hypoglycemia, high immunoreactivity, high insulin and low C peptide |
|
|
ethanol-induced hypoglycemia
|
glycogen is depleted in 18-24 hours and gluconeogenesis is blocked by ethanol concentration of 45mg/dL in blood
|
|
|
classification of hypoglycemia
|
posprandial, fasting, insulinoma, factitious, ethanol-induced
|
|
|
Cushing syndrome etiology
|
MCC is prolonged use of glucocorticoids; adrenal hyperplasia secondary to pituitary adenomas (40%), nonendocrine ACTH-producing tumors; adrenal neoplasia (30%)
|
|
|
Cushing syndrome presentation
|
Buffalo hump
Weakness Wound healing Fat deposition Amenorrhea Leukocytosis Osteoporosis Hypertension Hirsutism Potassium Psychiatric disorders Striae Stones Glucose intolerance Immune depression "BWWFALO HHumPPSS & DIabetes" |
|
|
Cushing syndrome diagnosis
|
Initial test: 1mg overnight dexamethasone suppression test;
if abnormal or false+ --> 24-hour urine free cortisol; if normal, exclude Cushing, if abnormal Cushing syndrome diagnosis; determine etiology: high dose dexamethasone suppression if supression to <50% of control --> pituitary adenoma; if no response then ACTH-producing tumor or adrenal hyperplasia measure ACTH level if high, then it's ACTH-producing tumor (do chest CT) if low it's adrenal hyperplasia --> urinary 17KS, DHEA-S, abdominal CT: if high and >4cm mass then its adrenal CA if normal or <4cm mass then adrenal adenoma |
|
|
hyperaldosteronism etiology
|
primary hyperaldosteronism (low renin) due to unilateral adrenal adenoma (70%)
or bilateral hyperplasia (25-30%) secondary hyperaldosteronism (high renin) due to |
|
|
primary hyperaldosteronism presentation
|
diastolic hypertension
muscle weakness polyuria polydipsia hypokalemia hypernatremia metabolic alkalosis no edema |
|
|
secondary hyperaldosteronism presentation
|
hypokalemia
metabolic alkalosis may or may not have muscle weakness polyuria polydipsia edema no diastolic hypertension no hypernatremia |
|
|
primary hyperaldosteronism diagnosis
|
high urine aldosterone levels and low plasma renin levels (give high-salt diet before lab tests); confirm with CT scan of adrenals
|
|
|
primary hyperaldosteronism management
|
adrenal adenomas are removed surgically
bilateral hyperplasia --> spironolactone |
|
|
Bartter syndrome
|
defect in Na-K-2CL transporter of loops of Henle, acts as furosemide-secreting tumor loosing NaCl which stimulates renin and aldosterone secretion
presentation: secondary hyperaldosteronism with no hypertension, no edema and severe hypokalemic alkalosis |
|
|
syndrome of adrenal androgen excess
|
excess DHEA and androstenidione which are then converted to testosterone due to congenital adrenal hyperplasia or adrenal neoplasia
presentation: hirsutism, oligomenorrhea, acne, virilization; |
|
|
congenital adrenal hyperplasia etiology
|
enzyme deficiencies: 21-beta hydroxylase, 17-hydroxylase, 11-hydroxylase
|
|
|
congenital adrenal hyperplasia presentation
|
21-beta hydroxylase deficiency (95%): low aldosterone in 1/3 (salt-loss, hyponatremia, hyperkalemia, dehydration, hypotension), female pseudohermaphroditism or precocious puberty in males
11-hydroxylase deficiency: virilization and hypertension/hyperkalemia due to 11-deoxycorticosterone; 17-hydroxylase deficiency: hypogonadism (17KS are blocked), hypokalemia, hypertension (11-deoxycorticosterone) |
|
|
congenital adrenal hyperplasia diagnosis
|
suspect infants with failure to thrive, adrenal insufficiency, salt-wasting and/or hypertension
lab studies: serum testosterone, androstenidione, dehydroepiandrostenidione, 17-hydroxyprogesterone, urinary 17KS and pregnanetriol |
|
|
congenital adrenal hyperplasia management
|
hydrocortisone
|
|
|
Adisson disease etiology
|
autoimmune destruction of the adrenals (80%), idiopathic destruction of the adrenals; surgical removal of the glands, destruction due to infection (TB, fungal, CMV, mycobacterium avium); hemorrhage, trauma, metastatic invasion
|
|
|
Adisson disease presentation
|
Acidosis
Weakness Weight loss Pressure is low (in primary) Pigmentation (in primary) Paresthesia Potassium is high Intolerance to stress Cramping Sparse axillary hair Sodium is low "Addison WWith PPPPICmentSS" |
|
|
Addison disease diagnosis
|
initial test: plasma cortisol after 250um of consyntropin -->
subnormal increase in cortisol --> measure ACTH --> if high it's primary adrenal insufficiency; if low its secondary adrenal insufficiency also hemogram (neutropenia, lymphocytosis, eosinophiliaa); elevated potassium and BUN; low sodium; low glucose; low plasma cortisol and low urinary 17-hydroxycorticosteroid |
|
|
Addison disease management
|
glucocorticoid, mineralocorticoid (fludrocortisone) and NaCl replacement; patient education
|
|
|
Adrenal crisis
|
due to major stress in previously undiagnosed patient, bilateral adrenal infarction or hemorrhage, abrupt glucocorticoid withdrawal
presentation: FEver, Vomit, Abdominal pain, Altered mental status, Hypotension "glucocorticoid withdrawal causes FeVAAH" Rx: fluid replacement + hydrocortisone |
|
|
pheochromocytoma epidemiology
|
10% Malignant
10% Children 10% no Hypertension 10% Bilateral 10% Extraadrenal "10% MuCH BEtter adrenaline" 5% autosomal dominnant alone MEN II MEN III von Recklinghousen neurofibromatosis von Hippel-Lindau retinal cerebellar hemangioblastomatosis affects 0.1% of hypertensives |
|
|
pheochromocytoma presentation
|
paroxystic crisis of sudden onset
headache profuse sweating palpitations chest or abdomen pain nausea/vomit hypertensive crisis and tachychardia anxiety tremor weight loss |
|
|
pheochromocytoma diagnosis
|
screening:
plasma metanephrine (no smoking 4 hours before test) urinary free catecholamines urinary metanephrines urinary vanillylmandelic acid plasma catecholamines if screening equivocal --> clonidine suppression test if screening is positive --> CT or MRI if not shown --> MIBG scan serum chromogranin levels correlate with tumor size |
|
|
pheochromocytoma differential
|
essential hypertension
anxiety attacks factitious crisis intracranial lesions autonomic epilepsy |
|
|
pheochromocytoma management
|
if crisis: phentolamine or phenoxybenzamine
after stabilization may use other antihypertensives and surgery |
|
|
primary (hypergonadotropic) hypogonadism etiology
|
Klinefelter
anorchia surgical or accidental castration radio therapy chemotherapy mumps TB leprosy |
|
|
secondary (hypogonadotropic) hypogonadism etiology
|
hypopituitarism
Kallman syndrome (hypogonadism and decreased sense of smell) |
|
|
hypogonadism presentation
|
undeveloped external genitalia, no seondary sexual characteristics, low libido and potency, retarded bone age;
|
|
|
hypogonadism diagnosis and Rx
|
low-normal urinary 17KS
low serum testosterone low LH/FSH in pituitary origin high LH/FSH in primary testicular failure Rx: testosterone |
|
|
Klinefelter syndrome
|
47XXY
hypogonadism gynecomastia sterility small testes high LH/FSH low-normal serum testosterone low urinary 17KS high serum estradiol |
|
|
diseases that present with prominent dysphagia/odynophagia
|
achalasia
esophageal cancer (SCC, adenocarcinoma) scleroderma diffuse esophageal spasm Plummer-Vinson Schatzcki's rings esophagitis Zenker diverticulum Mallory-Weiss syndrome |
|
|
achalasia presentation
|
progressive dysphagia to solids and liquids
regurgitation weight loss due to loss of inhibitory neurons of LES |
|
|
achalasia diagnosis
|
most accurate test is manometry
also barium esophagography (bird beak sign) if alarm symptoms (>60, heme-positive stools, >6 months, weight loss) esophagogastroduodenoscopy |
|
|
achalasia management
|
pneumatic dilation or botulinum toxin injections; if fails then surgical myotomy
|
|
|
esophageal cancer etiology
|
SCC is in upper two thirds and due to alcohol and tobacco
adenocarcinoma in lower third and is associated with reflux disease or Barret's |
|
|
esophageal cancer presentation
|
progressive dysphagia to solids then to liquids
weight loss can have halitosis regurgitation hoarseness hypercalcemia |
|
|
esophageal cancer diagnosis
|
barium swallow
endoscopy with biopsy is mandatory CT to detect local spread bronchoscopy to detect spread to bronchi endoscopic ultrasound for staging |
|
|
esophageal cancer management
|
surgery
if metastasis --> 5-fluoracil and radiotherapy |
|
|
esophageal scleroderma
|
dysphagia or reflux in scleroderma patient
diagnose with manometry treat with omeprazole and metoclopramide (promotility) |
|
|
diffuse esophageal spasm/ nutcracker esophagus
|
intermittent chest pain simulates myocardial infarction with dysphagia
no relation with exertion or swallowing precipitated by cold liquids screen with barium swallow (corkscrew pattern) most accurate test is manometry (disorganized contractions) treat with nifedipine and nitrates |
|
|
Schatzcki's ring
|
painless intermittent dysphagia located distally at squamous-columnar junction of LES
barium esophagram and pneumatic dilation |
|
|
Plummer-Vinson syndrome
|
intermittent dysphagia without pain located in hydropharynx (proximal)
associated with iron defficiency anemia and predisposes to SCC diagnose wih barium esophagram treat iron defficiency and pneumatic dilation |
|
|
esophagitis
|
due mostly to candida in HIV patients; also CMV, HSV or diabetes
also drugs such as alendronate, quinine, risedronate, vitamin C, pottasium, doxycycline, NSAIDs presents with progressive odynophagia only when swallowing (not intermittent) fluconazole or endoscopy |
|
|
Zenker diverticulum
|
outpouching of posterior pharyngeal muscles; halitosis, difficulty initiating swallow, undigested regurgitated food; barium studies; surgery (endoscopy or tube is contraindicated)
|
|
|
Mallory-Weiss syndrome
|
painless upper GI bleeding without dysphagia or odynopahgia
melena or hematemesis diagnose with upper endoscopy resolves spontaneously or epinephrine injections or cauterization |
|
|
etilogy of epigastric pain
|
ulcer disease
pancreatitis GERD gastritis gastric cancer (rare) most common etiology is nonulcer dyspepsia (all tests are normal) |
|
|
diagnosis of diseases causing epigastric pain
|
if >45
and/or alarm symptoms (weight loss, dysphagia, odynophagia, bleeding) and/or nonrespondant to PPIs or H2 blockers --> endoscopy for cancer, lower esophagus dysplasia biopsy ulcer, serology, breath tests and stool antigen detection can be used for H. pylori diagnosis |
|
|
diseases that manifest with epigastric pain
|
GERD
Barret peptic ulcer disease gastritis Zollinger-Ellison gastroparesis dumping syndrome pancreatitis gastric cancer nonulcer dyspepsia |
|
|
GERD etiology
|
idiopathic
nicotine alcohol caffeine peppermint chocolate anticholinergics CCBs nitrates |
|
|
GERD presentation
|
epigastric pain, sore-throat, metal taste, hoarseness, cough, wheezing
|
|
|
GERD diagnosis
|
if symptoms are clear, clinical diagnosis
if equivocal, 24h pH monitoring |
|
|
GERD management
|
PPIs (omeprazole); if nonrespondant then surgery
|
|
|
Barret esophagus
|
complication of GERD
if patient has GERD > 5 year --> endoscopy if Barret --> endoscopy every 2-3 years to check for dysplasia or cancer if low-grade dysplasia --> endoscopy in 3-6 months to check progression if high-grade dysplasia --> distal esophagectomy all should be given PPIs |
|
|
peptic ulcer disease etiology
|
90% of duodenal ulcers and 70-80% of gastric ulcers are due to H. pylori
NSAIDs is second cause also Zollinger Ellison gastric cancer Crohn disease burns head trauma prolonged intubation mechanical ventilation |
|
|
peptic ulcer disease presentation
|
midepigastric pain after eating (gastric) or relieved by eating (duodenal)
could have nausea or vomit there's rarely abdominal tenderness |
|
|
peptic ulcer disease diagnosis
|
most sensitive and specific is upper endoscopy with biopsy and it's performed routinely on those over 45 or with alarm symptoms (weight loss anemia, heme+ stools, dysphagia)
it's the only test to exclude gastric cancer serum antibody against H. pylori is sensitive and cheap; stool antigen and breath tests are also sensitive and can diffferentiate between new and old disease as well as determine if it's cured after treatment |
|
|
peptic ulcer disease management
|
if H. pylori --> PPI+clarithromycin+amoxicillin or tetracycline+metronidazole+-bismuth
ordinary ulcers w/o H. pylori --> PPI alone, misoprostol (rarely), celecoxib indications for surgery --> UGI bleeding or perforation, refractory ulcers, gastric outlet obstruction |
|
|
type A gastritis etiology
|
alcohol, NSAIDs, H. pylori, head trauma, burns, mechanical ventilation
|
|
|
type B gastritis etiology
|
gastric atrophy due to autoimmune destruction of parietal cells with pernicious anemia
|
|
|
gastritis presentation
|
epigastric pain, nausea/vomitting, hematemesis, melena
it can also manifest as asymptomatic bleeding |
|
|
gastritis diagnosis and treatment
|
if H. pylori, dignose and treat as peptic ulcer disease
type B gastritis diagnose with low B12 levels and high methylmalonic acid levels and also antiparietal cell antibodies, anti-intrinsic factor antibodies treat with B12 replacement |
|
|
Zollinger-Ellison presentation
|
95% present with ulcer disease that is recurrent after therapy
multiple ulcers at distal duodenum or resistant to therapy watery diarrhea or steatorrhea due to inhibition of lipase by acid can also present metastatic disease or hypercalcemia in MEN I |
|
|
Zollinger-Ellison diagnosis
|
after clinical suspicion --> elevated gastrin levels while off antisecretory medication
can also measure elevated gastric acid output positive secretin stimulation test (rise in gastrin after secretin injection, abnormal) CT/MRI/ultrasound to localize is 60-80% sensitive for metastasis and can include but not exclude somatostatin receptor scintigraphy is 90% sensitive for metastatic disease endoscopic ultrasound is most sensitive for metastatic disease |
|
|
gastroparesis
|
early satiety, posprandial nausea, sense of abdominal fullness
clinical diagnosis --> abdominal pain and bloating in patient with long history of diabetes treat ith promotility agents such as metoclopramide or erythromycin |
|
|
dumping syndrome
|
rapid release of hypertonic chyme into duodenum with osmotic effects and sudden glucose/insulin peak with hypoglycemia; presents with sweating, shaking, palpitations, lightheadedness shortly after a meal; treat by eating multiple small meals
|
|
|
nonulcer dyspepsia
|
of unknown etiology and diagnosed when all causes of epigastric pain have been excluded and there is still pain
|
|
|
Crohn disease presentation
|
discontinuous transmural granulomas in small or large intestines result in
fever, diarrhea, weight loss abdominal pain and bleeding episcleritis, scleritis, iritis cholangitis arthritis pyoderma gangrenosum erythema nodosum calcium/cholesterol stones painful abdominal masses can be palpated can cause fistulas and predisposes to colon cancer if lessions are located in colon |
|
|
ulcerative colitis presentation
|
continuous ulcerations limited to the mucosa and submucosa of large intestines result in
fever, bloody diarrhea, abdominal pain, weight loss episcleritis, scleritis, iritis cholangitis arthritis pyoderma gangrenosum erythema nodosum no fistulas, no masses predisposes to colon cancer |
|
|
inflammatory bowel disease diagnosis
|
gold standard is endoscopy
CD has vitamin and iron deficiencies; anti-Saccharomyces cerevisiae antibodies (ASCA); increased PT due to vit K deficiency; calcium kidney stones in CD ANCA antibodies in UC |
|
|
inflammatory bowel disease management
|
mesalamine derivatives: pentasa for CD, asacol for UC, rowasa for rectal disease
acute episodes treated with budesonide azathiorprine and 6MP used for long term infliximab for CD in case of fistulas surgery will be required in 60% UC cases and is effective |
|
|
general considerations about diarrhea
|
can be infectious, antibiotic-associated, lactose-intolerance, irritable bowel or carcinoid syndrome
if patient is hypotensive, has orthostasis, fever, abdominal pain or bloody stools is more important to hospitalize and treat than to determine etiology |
|
|
bacillus cereus diarrhea
|
ingestion of spores in refried chinese food
1-6 hour onset vomitting is prominent and no fecal blood |
|
|
campylobacter diarrhea
|
most common cause of infectious diarrhea
can be bloody or not associated with reactive arthritis and Guillain-Barre |
|
|
cryptosporidia, isospora diarrhea
|
found in AIDS < 100 CD4
|
|
|
E. coli O157:H7 diarrhea
|
bloody stools
associated with contaminated hamburger meat and shiga-like toxin antibiotics are contraindicated because dead organism causes HUS platelet transfusions are contraindicated in HUS |
|
|
giardia diarrhea
|
ingestion of unfiltered river or lake water
no bloody stools fullness, bloating and gas can simulate celiac disease |
|
|
salmonella diarrhea
|
most commonly due to ingestion of chicken and eggs or dairy products
|
|
|
shigella diarrhea
|
no clues in diarrhea are strong enough to point to this etiology; only stool culture
|
|
|
yersinia diarrhea
|
no clues in diarrhea are strong enough to point to this etiology, only stool culture
can mimic appendicitis common in people with iron overload/hemochromatosis |
|
|
vibrio diarrhea
|
ingestion of raw shellfish
|
|
|
viral diarrhea
|
associated with children in day-cares; there's absence of red or white cells in stools
|
|
|
staph diarrhea
|
ingestion of dairies, eggs, salads, custards
1-6 hour onset nausea and vomitting predominate |
|
|
ciguatera toxin diarrhea
|
2-6 hours after ingestion of large reef fish (grouper, red snapper, barracuda)
paresthesias, weakness, reversal of heat and cold |
|
|
diagnosis of diarrhea
|
invasive organisms produce fecal leukocytes within 24-36 hours
salmonella, shigella, e. coli, campylobacter, yersinia, vibrio definitive diagnosis of diarrhea is stool culture and fecal analysis for ova for giardia can use ELISA stool antigen detection for cryptosporidia need modified acid-fast test |
|
|
diarrhea management
|
empiric antibiotics until stool culture and if there's abdominal pain, bloody stools and fever;
high-volume stools and dehydration don't justify antibiotics; empirical treatment is ciprofloxacin or fluoroquinolone+metronidazole scombroid is treated with antihistamines giardia with metronidazole isospora with TMP/SMX doxycycline for vibrio |
|
|
antibiotic-associated diarrhea
|
caused mostly by C. difficile and by any antibiotic but mostly associated with clindamycin; history of antibiotics + diarrhea makes diagnosis and patient should have stool C. difficile toxin test; treat with metronidazole or oral vancomycin if resistance
|
|
|
lactose intolerance
|
high prevalence; diarrhea associated with bloating and gas but no blood or leukocytes in stools; empirical diagnosis and treatment is to remove milk, cheese and dairies (except yogurt) with resolution of symptoms in 24-36 hours; precise diagnosis is increased stool osmolality and increased stool osmolar gap
|
|
|
irritable bowel syndrome presentation and diagnosis
|
abdominal pain plus constipation alone (20%) or diarrhea alone or both
diagnosis of exclusion: lactose intolerance, IBD, celiac, carcinoid, giardia, anatomic defects diagnostic criteria: pain relieved by bowel movement, fewer symptoms at night, diarrhea alternating with constipation |
|
|
irritable bowel syndrome management
|
high-fiber diet
antidiarrheals (loperamide, diphenoxylate) antispasmodics (hyoscyamine, dicyclomine, alkaloids) tricyclics for resistant cases intestinal serotonin agents: tegaserod (constipation-predominant) or alosetron (diarrhea-predominant) |
|
|
carcinoid syndrome
|
most located in appendix or ileum but could be bronchial
implies metastatic disease presents with diarrhea, flushing, tachychardia, hypotension, niacin deficiency rash (depletion of tryptophan), endocardial fibrosis (right heart) diagnose with high urinary 5-HIAA treat with octeotride or surgery if tumor is localized |
|
|
malabsorption/steatorrhea syndromes
|
celiac disease, chronic pancreatitis, tropical sprue, Whipple's
|
|
|
malabsorption syndromes general presentation
|
steatorrhea, weight loss, ADEK deficiency, hypocalcemia, easy-bruising/increased PT, iron deficiency (duodenum), folate deficiency megaloblastic anemia), B12 deficiency (megaloblastic anemia, terminal ileum)
|
|
|
malabsorption syndromes specific presentation
|
celiac --> iron deficiency anemia and dermatitis herpetiformis
chronic pancreatitis --> recurrent episodes from alcohol or gallstones tropical sprue --> history of tropical country travel Whipple --> dementia, arthralgias, opthalmoplegia |
|
|
celiac disease diagnosis
|
screen with antigliadin, antiendomysial and antiglutaminase antibodies
endoscopic biopsy is required to exclude small bowel lymphoma and confirm diagnosis |
|
|
chronic pancreatitis diagnosis
|
history of repeated pancreatitis episodes with pancreatic calcifications on x-rays or CT
secretin stimulation test (gold standard but rarely performed) or low trypsin levels |
|
|
tropical sprue and Whipple diagnosis
|
biopsy showing organisms
for Whipple, most sensitive test is PCR of biopsy showing PAS+ macrophages |
|
|
how to differentiate between malabsorption diseases
|
d-xylose, iron, folate and carotene malabsorption point to mucosal problems (celiac, sprue, Whipple)
vitamin B12 malabsortion can also indicate pancreatic enzyme deficiency vitamin K and calcium deficiencies are due to fat malabsorption |
|
|
malabsorption syndromes treatment
|
celiac --> gluten-free diet
chronic pancreatitis --> pancreatic enzyme pills tropical sprue --> TMP-SMX or doxycycline for 6 months Whipple --> TMP-SMX or doxycycline or ceftriaxone for 1 year |
|
|
diverticulosis
|
50% prevalent over 50
asymptomatic or left lower quadrant colicky pain +- painless bleeding diagnose with colonoscopy treat with increased dietary fiber and bulking agents |
|
|
diverticulitis
|
infected diverticula
fever, tenderness, pain, leukocytosis diagnose with CT barium and endoscopy are contraindicated treat with ciprofloxacin/metronidazole, ampicillin/sulbactam, piperazillin/tazobactam, cefotetan/gentamycin |
|
|
constipation
|
can be due to lack of dietary fiber, insuficient fluid intake, CCBs, oral ferrous sulfate, hypothyroidism, opiates, anticholinergics; painful defecation can be dark due to bismuth or iron; treat by stopping medications, hydration, bulking agents, milk of magenesia, docusate
|
|
|
colon cancer
|
heme-positive brown stool and chronic anemia for right side
obstruction and decreased stool caliber for left side can present with strep bovis or C. septicum endocarditis diagnose with colonoscopy or sigmoidoscopy if located 60cm of distal colon if localized to mucosa or submucosa then surgery, else 5FU chemotherapy |
|
|
hereditary nonpolyposis syndrome
|
no polyps
three family members in at least two generations with colon cancer increased incidence of ovarian and endometrial cancer start screening at age 25 and then every 1-2 years |
|
|
hereditary polyposis syndromes
|
FAP has APC gene which confers 100% penetrance for adenomas by 35 and colon cancer by 50
screen with flexible sigmoidoscopy at age 12 and 1-2 years thereafter perform colectomy when first polyp is found juvenile polyposis syndromes has 10% risk of colon cancer and produces hamartomas, not adenomas Cowden syndrome is colon hamartomas with slight risk of colon cancer all can present with rectal bleeding as a child |
|
|
Gardner syndrome
|
colon cancer with multiple, soft tissue tumors such as osteoma, lipoma, cysts, fibrosarcomas
if casual osteoma found in x-ray --> colonoscopy |
|
|
Peutz-Jeghers syndrome
|
hamartomatous polyps in colon with hyperpigmented melanotic spots on lips and skin
abdominal pain due to intussusception/bowel obstruction |
|
|
Turcot syndrome
|
colon cancer with CNS malignancies
|
|
|
GI bleeding etiology
|
upper GI bleed: ulcer, gastritis, Mallory-Weis, esophagitis, gastric cancer, esophageal varices from portal hypertension
lower GI bleed: diverticulosis, angiodysplasia, hemorrhoids, cancer, inflammatory bowel disease; |
|
|
GI bleeding management
|
first fluid resucitation with saline or Ringer
hemogram, PT, type and crossmatch if elevated PT --> fresh frozen plasma if platelets <50,000 transfuse platelets if concomitant cirrhosis --> octeotride to decrease portal hypertension if severe bleed or coagulopathy --> fluids, blood, platelets and plasma if esophageal varices --> octeotride or place bands by endoscopy or perform TIPS elderly --> maintain hematocrit >30% with fluids and/or transfusion younger --> transfuse if hematocrit <20% after these measures --> endoscopy to determine etiology |
|
|
GI bleeding presentation
|
red blood in stools if lower GI bleed
ocult blood with >5-10ml or melena with >100ml of upper GI blood orthostasis: >10 point rise in pulse or >20 point drop in systolic pressure from supine to sitting or standing after 1 minute between measurements indicates 15-20% blood loss pulse above 100 or systolic pressure below 100 indicates 30% blood loss |
|
|
GI bleeding diagnosis
|
endoscopy
nuclear bleeding scan (technetium tagged red blood cells from the patient) angiography usefull in high-volume bleeding also capsule endoscopy |
|
|
acute pancreatitis etiology
|
alcoholism, gallstones, hypercalcemia, hypertriglyceridemia, medications (pentamidine, didanosine, azathiorpine, sulfas), ERCP, trauma, mumps virus
|
|
|
acute pancreatitis presentation
|
midepigastric pain radiates to the back, nausea, vomitting
severe disease can have fever, hypotension, ARDS, leukocytosis Cullen sign (blue umbilical discoloration) Turner's sign (bluish discoloration of flanks) |
|
|
acute pancreatitis diagnosis
|
screening with amylase and lipase levels
Ranson criteria for severity (leukocytosis, hypoxia, hyperglycemia, high LDH and AST) hypocalcemia, high BUN CT scan is more accurate than Ranson criteria for severity gold standard is ERCP |
|
|
acute pancreatitis management
|
supportive with fluids, bowel rest and analgesics
necrosis on CT is indicative of imipenem or cefuroxime to diminish infection risk severe necrosis is indication for percutaneous needle biopsy of pancreas if there's necrosis and infection surgical debridement is indicated drain pseudocyst if >5cm, pain, fistula or rupture |
|
|
acute pancreatitis complications
|
ascites high in amylase
pleural effusion is transudate high in amylase splenic vein thrombosis |
|
|
cirrhosis etiology
|
alcohol (#1 cause)
primary billiary cirrhosis sclerosing cholangitis alpha-1 antitrypsin deficiency hemochromatosis Wilson disease |
|
|
general presentation of cirrhosis
|
low albumin level
portal hypertension esophageal varices ascites (do paracenthesis to exclude infection) peripheral edema increased PT spider angiomata palmar erythema asterixis encephalopathy jaundice low clotting factors except factor VIII and vonWillebrand spontaneou bacterial peritonitis (WBC count >500/mm3 or >250/mm3 neutrophils, treat with ceftriaxone) |
|
|
serum-ascites albumin gradient
|
serum albumin is always higher than ascitic fluid
when SAAG >1.1 then portal hypertension when SAAG <1.1 (high ascitic albumin) then cancer and infections |
|
|
cirrhosis management
|
edema --> diuretics (spironolactone because of high aldosterone levels)
portal hypertension and varices --> propanolol (prevents bleeding) encephalopathy --> neomycin or lactulose (metabolized by bacteria in colon which increases acidity and converts NH3 into amonium which is not absorbed well and eliminated vitamin K is not effective because there are no clotting factors |
|
|
primary billiary cirrhosis
|
fatigue and pruritus
osteoporosis in 20-30% and cirrhosis signs associated with Sjogren, RA, scleroderma diagnose with normal transaminases, high alkaline phosphatase and GGTP, high IgM and antimitochondrial antibodies (specific) biopsy is gold standard treat with orsodeoxycholic acid and cholestyramine UV light for pruritus and liver transplant in late stages |
|
|
primary sclerosing cholangitis
|
fatigue and pruritus, elevated alkaline phosphatase, osteoporosis in 20-30% and cirrhosis signs
associated with inflammatory bowel disease (specially UC) can predispose to cancer of billiary system (15%) diagnose with normal transaminases, high alkaline phosphatase and GGTP, high IgM no antimitochondrial antibodies biopsy is not gold standard, it's ERCP or cholangiogram treat with orsodeoxycholic acid and cholestyramine UV light for pruritus and liver transplant in late stages |
|
|
hemochromatosis
|
genetically predisposed overabsorption of iron in duodenum with accumulation
cirrhosis is most common finding hepatocellular CA (15-20%) restrictive cardiomyopathy (15%) arthralgias, skin hyperpigmentation, diabetes, hypogonadism, vibrio vulfinicus and yersinia infections screen with elevated iron levels, low iron binding capacity and high ferritin biopsy is gold standard treat with phlebotomy or deferoxamine |
|
|
Wilson disease
|
underexcretion and overabsorption of copper with deposition in brain, liver and cornea
coreathetoid movements with psychosis --> slit lamp exam --> Kayser-Fleischer corneal rings also cirrhosis lab tests: low ceruloplasmin and high urinary copper gold standard is biopsy treat with copper chelator penicillamine or liver transplant; |
|
|
alpha-1 antitrypsin deficiency
|
antiprotease is not produced enough by liver
leads to cirrhosis and emphysema at young age in nonsmoker confirm diagnosis with enzyme levels enzyme replacement therapy and smoke cessation |
|
|
chronic hepatitis B/C
|
virus transmitted by blood transfusions, needle sticks and sex
mostly asymptomatic until advanced disease then cirrhosis HbSAg >6 months makes chronic hep B diagnosis hep C antibody and high viral load on PCR is diagnosis for chronic hep C treat hep B with interferon, lamiduvine or adefovir monotherapy treat hep C with pegylated interferon and ribavirin multitherapy |
|
|
characteristics of pain
|
duration, quality, location, radiation, frequency, alleviating or precipitating factors, associated symptoms
|
|
|
chest pain in acute coronary syndrome
|
substernal opressive quality described as tightness, heaviness or pressure; in MI pain lasts >20-30min; constant in frequency, precipitated by exercise, radiates to left shoulder
inferoposterior MI can present with upper abdominal pain, nausea, hypotension and dizziness or fainting (due vagal reflexes) transient ischemia is releived with nitroglycerin associated symptoms are diaphoresis, tachypnea and anxiety |
|
|
musculoskeletal or pulmonary chest pain
|
described as sharp or knife-like and reproduced by changes in position or palpation
|
|
|
tachycardia/tachypnea
|
nonspecific but seen in MI or pulmonary embolism
|
|
|
blood pressure in evaluation of chest pain
|
difference of >20mmHg between two arms suggests aortic dissection (70%); hypotension is seen in massive pulmonary embolism or cardiac shock and it could also be seen in inferoposterior MI
|
|
|
fever in evaluation of chest pain
|
suggests pneumonia or mediastinitis
|
|
|
signs of atherosclerosis
|
corneal lipid rings
narrowed retinal arteries pigment and hair changes in legs may be seen in acute coronary syndrome |
|
|
chest wall exam in chest pain evaluation
|
check for tender areas, respiratory motion, respiratory retractions or accessory muscle use; if palpation reproduces the pain consider musculoskeletal etiology
|
|
|
heart sounds in chest pain evaluation
|
wide physiologic splitting of S2 (inspiration) --> right bundle branch block or right ventricular infarction
paradoxical splitting (expiration) --> LBBB or anterior/lateral infarction S3 --> heart failure S4 --> angina or infarction; aortic regurgitation --> aortic dissection mitral regurgitation --> angina or infarction due to papillary muscle dysfunction |
|
|
lung auscultation in chest pain evaluation
|
assymetry of breath sounds in spontaneous pneumothorax; absent lung sounds in spontaneous pneumothorax or pleural effussion
|
|
|
work-up of chest pain
|
all patients should have 12-lead ECG (MI diagnostic findings are ST elevation or Q waves in 50%, ischemia findings are ST depression or T wave inversion in 35%)
CK-MB, troponins T I C chest x-ray |
|
|
differential diagnosis of chest pain
|
noncardiovascular: costochondritis, hiatal hernia, GERD, peptic ulcer, gallbladder disease
cardiovascular: MI, aortic stenosis, myocarditis, pericarditis, dissecting aortic aneurysm, mitral valve prolapse pulmonary: embolism, pulmonary hypertension, pneumothorax |
|
|
costochondritis differentiating features
|
pain exacerbated with inspiration; reproduced with chest wall palpation
|
|
|
hiatal hernia differentiating features
|
reflux of food, relief with antacids
|
|
|
GERD differentiating features
|
acid reflux, relief with antacids
|
|
|
peptic ulcer differentiating features
|
epigastric pain worse 3h after eating
|
|
|
gallbladder disease differentiating features
|
right upper quadrant pain and tenderness
|
|
|
myocardial infarction differentiating features
|
severe pain > 20 minutes
|
|
|
aortic stenosis differentiating features
|
systolic ejection murmur
|
|
|
myocarditis differentiating features
|
vague mild pain
|
|
|
pericarditis differentiating features
|
sharp pain, worse with lying down, relieved by sitting up
diffuse ST elevation responds to analgesics |
|
|
dissecting aortic aneurysm differentiating features
|
sharp, tearing pain also felt in the back
loss of pulses, wide mediastinum on x-ray diagnosis confirmed by CT, MRI, transesophageal ultrasound or aortography |
|
|
mitral valve prolapse differentiating features
|
transient pain, midsystolic click, young females
|
|
|
pulmonary embolism differentiating features
|
tachypnea, dyspnea, cough, pleuritic pain, hemoptysis
diagnosis confirmed by CT, lung scan or pulmonary angiogram |
|
|
pulmonary hypertension differentiating features
|
signs of right ventricle failure
|
|
|
pneumothorax differentiating features
|
sudden onset of pain and dyspnea
|
|
|
major modifiable IHD risk factors
|
high cholesterol, tobacco, hypertension, physical inactivity, obesity, diabetes
|
|
|
uncontrollable IHD risk factors
|
age, sex, heredity
|
|
|
minor IHD risk factos
|
sex hormones and stress
|
|
|
cholesterol levels in ischemic heart disease
|
the higher the level, the more risk for IHD; LDL is most important to consider (>100mg/dL)
low HDL (<40mg/dL) hypertriglyceridemia (>150mg/dL) high HDL/cholesterol ratio high lipoprotein A |
|
|
stable angina presentation
|
cardiac chest pain episodes on exertion relieved by rest that last 5-15min; ST depression in seen during attack
|
|
|
stable angina diagnosis
|
perform baseline ECG then exercise stress test which is positive when there is >2mm ST depression and/or drop of >10mmHg in systolic pressure
this test is diagnostic (67% sens, 70% spec), determines severity, effectiveness of treatment and functional capacity; contraindicated in most other cardiac diseases can also use thallium nuclear stress test (82% sens, 95% spec), dobutamine or adenosine stress test, stress echocardiogram patients with stable angina need evaluation of severity |
|
|
stable angina management
|
acute episodes --> sublingual nitroglycerin
long-term --> long-acting nitrates (isosorbide), beta-blockers, aspirin, statins, modification of risk factors after evaluating severity decide on revascularization (stent or bypass) |
|
|
differentiate NSTEMI and unstable angina diagnosis
|
if there are ECG signs + elevated cardiac markers --> NSTEMI
if normal cardiac markers 6-24 hours after presentation --> unstable angina |
|
|
unstable angina presentation
|
cardiac chest pain episodes occuring at rest or of increasing severity, frequency and duration resistant to nitrates
|
|
|
thrombolytic therapy
|
beneficial in STEMI but not NSTEMI; in NSTEMI ischemia is mostly due to thrombus-related embolization and platelet-rich instead of fibrin-rich thus thrombolytics are not effective
|
|
|
ECG diagnosis in NSTEMI
|
ST segment deviation (>0.5mm) or new T-wave inversion (>2mm)
but normal ECG or minor changes in up to 50% |
|
|
high-risk features of UA/NSTEMI
|
repetitive or prolonged chest pain (>10min)
elevated biomarkers persistent ECG changes hemodynamic instability (SBP<90) sustained ventricular tachycardia syncope LV EF <40% diabetes chronic kidney disease prior PTCA or CABG |
|
|
UA/NSTEMI management
|
antiplatelet: aspirin and clopidogrel (300mg loading, 75mg/day)
anticoagulant; unfractionated heparin or enoxaparin for 48-72 hours or until angiography glycoprotein IIb/IIIa inhibitors: abciximab, tirofiban (diabetics), eptifibatide beta-blocker invasive: early coronary angiography (48 hours) and revascularization recommended in NSTEMI or high-risk patients |
|
|
STEMI diagnosis
|
clinical symptoms plus ECG:
persistent ST elevation of >1mm in two contiguous limb leads ST elevation of >2mm in two contiguous chest leads new LBBB pattern cardiac biomarkers are not needed for initial diagnosis |
|
|
STEMI atypical presentation
|
elderly or diabetics can present with nausea or dyspnea as sole symptom
as many as 20% are silent (symptoms not severe enough for patient) |
|
|
STEMI general management
|
cardiac monitor
oxygen therapy IV line aspirin nitroglycerin morphine |
|
|
localizations of STEMI
|
inferior, anteroseptal, anterior, lateral, posterior
|
|
|
inferior STEMI ECG localization
|
leads II, III and aVF; artery is right coronary
|
|
|
anteroseptal STEMI ECG localization
|
leads V1-V3; LAD artery
|
|
|
anterior STEMI ECG localization
|
leads V2-V4; LAD artery
|
|
|
lateral STEMI ECG localization
|
leads I, aVL, V4-V6; artery is LAD or circumflex
|
|
|
posterior STEMI ECG localization
|
leads V1-V2 --> tall broad initial R wave, ST depression, tall upright T wave
usually in association of inferior or lateral STEMI artery is posterior descending |
|
|
abnormal Q wave
|
>25% the height of partner R wave
greater than 0.04sec and 2mm deep Q waves are normal in lead III |
|
|
ECG evolution of STEMI
|
hyperacute T waves (immediately to 6-24 hours)
ST elevation (immediately to 1-6 weeks) Q waves (1/several days to years/never) T wave inversion (6-24 hours to months-years) |
|
|
reperfusion therapy
|
PCI (angioplasty/stents) are preferred if <12 hours and <90 minutes from first medical encounter; if PCI is unavailable or too late then thrombolytic therapy
|
|
|
thrombolytic therapy
|
appropiate in place of PCI if >12 hours of onset of STEMI
streptokinase and alteplase by IV infusion reteplase and tecneplase by rapid bolus tPA is most common in US due to antibody formation streptokinase is contraindicated if had been given within 1 year to same patient |
|
|
absolute contraindications to thrombolytic therapy
|
active bleeding
significant closed head or facial trauma within 3 months suspected aortic dissection prior intracranial hemorrhage ischemic stroke within 3 months |
|
|
relative contraindications to thrombolytic therapy
|
recent major surgery (<3 weeks)
traumatic/prolonged cardiopulmonary rescucitation recent internal bleeding active peptic ulcer severe poorly controlled hypertension ischemic stroke <3 months |
|
|
antiplatelet therapy in STEMI
|
aspirin (to all patients) and clopidogrel (300mg) to patients undergoing PCI or fibrinolysis; with long-term maintanance of 75mg (up to 1 month after fibrinolysis or 1 year after stent)
|
|
|
anticoagulant therapy in STEMI
|
unfractionated heparin (or perhaps enoxaparin) an GP IIb/IIIa inhibitors should be used in conjunction with PCI; only heparin in case of fibrinolytic therapy
|
|
|
heparin dosages in STEMI
|
in PCI it depends on concomitant use of GP Iib/IIIa inhibitors; in fibrinolysis: unfractionated heparin in initial bolus of 60 units/kg, followed by initial infusion of 12 units/kg (max 1,000/h); adjusted to attain activated PTT to 1.5-2 times control; enoxaparin may be used in patients <75 but dose adjustment in renal patients
|
|
|
CABG indications
|
should be considered in patients who failed PCI or persistent ischemia resistant to drugs; patient should have suitable anatomy
|
|
|
discharge medications after acute coronary syndrome
|
aspirin (75mg indefinitely)
clopidogrel (75mg upto 1 year after PCI or 1 month or if aspirin contraindicated) beta-blocker (if heart failure carvedilol or metoprolol) ACE inhibitors (if heart failure) statins to all patients should be initiated in hospital short-acting nitrates or isosorbide if continuous frequent pain warfarin in those at risk for systemic thromboembolism ABCDE |
|
|
drug treatments shown to reduce mortality in IHD
|
statins
aspirin beta-blockers CABG in triple vessel or left main disease |
|
|
dysrhythmias as ACS complication
|
bradycardia (treat with atropine)
premature beats supraventricular tachycardias (atrial tachycardia, fibrillation, flutter) ventricular tachyarrhythmias (ventricular tachycardia, accelerated idioventricular rhythm, fibrillation) |
|
|
conduction abnormalities as ACS complication
|
1st, 2nd and 3rd degree heart blocks, hemiblocks, branch blocks
|
|
|
mechanical dysfunction as ACS complication
|
heart failure (left/right or biventricular)
true or pseudoventricular aneurysm acute mitral regurgitation ventricular septal rupture free wall rupture mechanical problems are treated with emergency surgery |
|
|
ischemia as ACS complication
|
recurrent infarction or extension
post-infarction angina after thrombolytics or PCI requires bypass surgery |
|
|
sudden cardiac death
|
is a complication of ACS; most commonly ventricular fibrillation or tachycardia
|
|
|
thromboembolic complications of ACS
|
mural thrombus
deep vein thrombosis due to prolonged immobilization ischemic stroke |
|
|
right ventricular infarction
|
often a complication of inferior MI (30%); diagnosed with ECG and treated with fluids (if its complication)
|
|
|
hypercoagulable states as nonatherosclerotic cause of MI
|
polycythemia vera
thrombocytosis factor V Leyden protein C deficiency antiphospholipid antibodies |
|
|
vasculitis as nonatherosclerotic cause of MI
|
SLE, PAN, takayasu, Kawasaki
|
|
|
coronary spasm
|
due to prinzmetal or cocaine abuse which are nonatherosclerotic causes of MI
|
|
|
Prinzmetal angina
|
episodes of severe angina due to coronary vasospasm
occurs at rest (night or morning hours) ST elevation and can be associated with MI, ventricular arrhythmias or sudden death, migraines exercise stress tests and angiography are normal diagnose with ergonovine |
|
|
coronary embolus as nonatherosclerotic cause of MI
|
atrial myxoma, atrial or ventricular thrombus
|
|
|
compensatory mechanisms in heart failure
|
cardiac: Frank-Starling, tachycardia, ventricular dilation;
neuronal: increased sympathetic adrenergic, reduced vagal activity; hormonal: vasopressin, catecholamines and BNP, renin-angiotensin-aldosterone system |
|
|
systolic heart failure
|
decreased ventricle contraction, dilation and EF<45% due to ischemic cardiomyopathy, dilated cardiomyopathy
|
|
|
dyastolic heart failure
|
filling of one or both ventrciles is impaired with normal EF; can be due to amyloidosis
|
|
|
congestive heart failure
|
syndrome of dyspnea, fatigue, peripheral edema, high JVP and pulmonary edema with crackles
|
|
|
causes of heart failure
|
70% are due to ischemic heart disease
hypertensive, alcoholic and other cardiomyopathies valvular disease congenital heart disease |
|
|
precipitating factors in heart failure
|
important to exclude in diagnosis
excessive dietary Salt uncontrolled Hypertension cardiac Ischemia myocardial Infarction Infections Thyrotoxicosis Arrhythmias Anemia "SHIIIT precipitates A failure" |
|
|
heart failure presentation
|
dyspnea
orthopnea paroxysmal nocturnal dyspnea fatigue pulmonary rales peripheral edema ascites hepatomegaly jugular venous distention displaced apical impulse |
|
|
cardiac Vs. pulmonary dyspnea
|
cardiac is more sudden, not associated with sputum production, without history of pulmonary disease, no lung disease evidence on x-ray, cardiomegaly seen on x-ray
pulmonary dyspnea is the contrary |
|
|
classification of heart failure severity
|
Class I: no limitation of daily activities
Class II: mild limitation, can perform mild exertion Class III: marked limitation, only comfortable at rest Class IV: confined to bed or chair; physical activity or rest brings discomfort |
|
|
heart failure diagnosis
|
check cardiac enzymes to exclude ischemia or MI
x-ray to exclude infection test of choice is echocardiography for diagnosis and classification (ejection fraction) chest x-ray to exclude infection shows cardiomegaly, vascular redistribution, Kerley B-lines, interstitial edema ECG indentifies hypertrophy, ischemia or precipitating arrhythmias BNP is 97% sensitive for decompensated HF |
|
|
heart failure management
|
first line: ACEi + loop diuretic then add carvedilol/metoprolol +- digitalis
ACE inhibitors improve survival and reduce hypertrophy and symptoms; loop diuretics decrease congestive symptoms; betablocker decrease mortality, reduce hospitalizations and improve ejection fraction; other vasodilators: nitrates/hydralazine used if ACEi or ARB are contraindicated; digitalis does not improve survival but reduces severe symptoms; if dyastolic HF use less diuretics and vasodilators and give CCBs (verapamil) to slow heart rate and allow filling |
|
|
pulmonary edema
|
medical emergency
tachypnea, expectoration, cyanosis, nocturnal dyspnea, rales, ronchi, wheezing; x-rays: prominent pulmonary vessels, enlarged cardiac silhouette, Kerley B lines, pleural effusions ECG: to determine if arrhythmia treatment: morphine, furosemide, sitting patient upright, oxygen, nitroglycerin (reduce preload), digoxin (if atrial fibrillation), IV ACEi |
|
|
mitral stenosis etiology
|
abnormal mitral leaflets are affected due to rheumatic fever autoimmune deposits
reduced left ventricular filling, increased left atrial and pulmonary pressure, forward and right heart failure ensues |
|
|
mitral stenosis presentation
|
dyspnea
orthopnea hemoptysis hoarseness paroxysmal nocturnal dyspnea fatigue systemic embolism right heart failure atrial fibrillation pulmonary rales decreased pulse pressure loud S1 with opening snap following S2 diastolic rumble sternal lift |
|
|
mitral stenosis auscultation
|
pulmonary rales, loud S1 with opening snap following S2, diastolic rumble, sternal lift
|
|
|
mitral stenosis diagnosis
|
chest x-ray: large left atrium (double-density right heart border, posterior displacement of esophagus and elevated left mainstem bronchus), Kerley B lines, large pulmonary arteries
ECG: signs of ventricular hypertrophy, left/right atrial abnormalities, atrial fibrillation echocardiography: thickening of mitral valve leaflets, left atrial enlargement |
|
|
mitral stenosis management
|
diuretics, salt restriction, digitalis and anticoagulants if atrial fibrillation
if drugs fail --> surgical valve replacement or commissurotomy |
|
|
acute etiology of mitral regurgitation
|
rupture of chordae tendinae
papillary muscle rupture endocarditis (valvular destruction) trauma |
|
|
chronic etiology of mitral regurgitation
|
Calcifications
Hypertrohpic cardiomyopathy Endocardial cushion defect Endocarditis Fibroelastosis Papillary muscle dysfunction Rheumatic fever mitral Prolapse severe left ventricular dilation "regurgitation by CHEF PReP" |
|
|
mitral regurgitation pathogenesis
|
retrograde left ventricle flow into left atrium increases atrial pressure and decreases forward output which results in volume overload, decreased afterload (flow is eased into left atrium) which allow compensated increased ejection fraction which eventually leads to left ventricular dysfunction
|
|
|
mitral regurgitation presentation
|
dyspnea, orthopnea, paroxysmal nocturnal dyspnea; if severe, right sided failure;
|
|
|
mitral regurgitation auscultation
|
hyperdynamic and displaced (downward left) left ventricular impulse
carotid upstroke diminished holosystolic apical murmur S3 with widely split S2 distended neck veins |
|
|
mitral regurgitation diagnosis
|
x-ray: cardiac enlargement and possble pulmonary congestion
ECG: left ventricular hypertrophy and left atrial enlargement echocardiography: mitral valve can prolapse; distended neck veins |
|
|
mitral regurgitation management
|
therapy: digitalis, diuretics, ACEIs, warfarin; if symptoms persist or are severe: surgery
|
|
|
mitral prolapse presentation
|
most are asymptomatic; can have lightheadedness, palpitations, syncope, chest pain
|
|
|
mitral prolapse auscultation
|
mid-systolic click and late systolic murmur at apex, worsens with Valsalva, improves with squatting
|
|
|
mitral prolapse complications
|
arrhythmias
sudden death CHF bacterial endocarditis valve calcifications transient cerebral ischemic attacks |
|
|
mitral prolapse diagnosis
|
clinical + doppler echocardiography which shows systolic displacement of mitral leaflets into left atrium
|
|
|
mitral prolapse management
|
endocarditis prophylaxis (in severe cases)
betablocker for chest pain or arrhythmias antiarrhythmics surgery rarely necessary |
|
|
aortic stenosis etiology
|
due to age-related calcification of the valve or calcification and fibrosis of congenitally bicuspid valve; also rheumatic fever
|
|
|
aortic stenosis pathogenesis
|
stiff aortic valve increases afterload and left ventricular pressure which results in concentric hypertrophy
noncompliant ventricle and S4 gallop with increased LVEP the heart has increased oxygen demands with decreased coronary flow due to thickness |
|
|
aortic stenosis presentation and auscultation
|
angina
syncope dyspnea pulsus pardus et tardus carotid thrill systolic ejection murmur in aortic area S4 gallop |
|
|
mitral stenosis diagnosis
|
ECG: right ventricular hypertrophy, atrial fib
chest x-ray: large left atrium and pulmonary artery with increased lung vascularity echocardiography: thickening of mitral valve leaflets, left atrial enlargement |
|
|
mitral stenosis management
|
endocarditis prophylaxis no longer recommended
if symptomatic: surgical valve replacement or balloon valvuloplasty |
|
|
aortic stenosis Vs. aortic valve sclerosis
|
both have systolic murmur but in aortic valve sclerosis carotids don’t have delayed upstroke
no hypertrohpy in ECG no excursion of valve leaflets in ecochardiography no hemodynamically significant aortic valve gradient |
|
|
aortic stenosis Vs. hypertrophic obstructive cardiomyopathy
|
both have systolic murmur but in HOC there's characteristic change in murmur with maneuvers; large septal Q waves; characteristic echocardiographic features (asymmetrical hypertrohpy)
|
|
|
aortic stenosis Vs mitral regurgitation
|
both have systolic murmurs but in MR is holosystolic and radiates to axilla, not carotids
carotid upstroke normal dilated ventricle aortic valve normal in eco |
|
|
aortic stenosis Vs. pulmonic stenosis
|
both have systolic murmurs but in pulmonic stenosis it does not radiate to neck; it's loudest on left sternal border and increases with inspiration; chest x-ray and EKG reveal enlarged right heart and valve stenosis
|
|
|
aortic regurgitation etiology
|
hypertension (most common)
infectious endocarditis syphillis ankylosing spondylitis Marfan rheumatic fever aortic dissection aortic trauma |
|
|
aortic regurgitation pathogenesis
|
valve insufficiency leads to volume overload of left ventricle with compensating Frank-Starling; dilation, overstretching and decreased contraction force; if acute, can have large LEVEDP because ventricle is not adapted; acute pulmonary edema can occur; lower systolic blood pressure is due to regurgitation of blood out of aorta and decreased SVR; there's increased systolic pressure and widened pulse
|
|
|
aortic regurgitation presentation
|
dyspnea
diastolic decrescendo, systolic flow and Austin-Flint (presystolic low-pitched apical) murmurs Duroziez sign (murmur over femoral) S3 when decompensated |
|
|
aortic regurgitation diagnosis
|
chest x-ray: LV and aortic dilation
EKG: LV hypertrophy with volume overload (narrow deep Q waves in left precordial leads) echocardiogram: dilated LV and aorta, LV volume overload, fluttering of anterior mitral valve leaflet |
|
|
aortic regurgitation management
|
endocarditis prophylaxis not recommended; salt restriction, ACEIs, aortic valve replacement
|
|
|
dilated cardiomyopathy etiology
|
most common is idiopathic
drugs --> Doxorubicin, Cyclophosphamide, Vincristine, Alcohol infections --> Tuberculosis, Coxsackie metabolic --> Uremia, chronic Hypophosphatemia, Hypokalemia, Hypocalcemia peripartum toxins --> arsenic, cobalt, lead |
|
|
dilated cardiomyopathy presentation
|
signs of left and right systolic heart failure
|
|
|
dilated cardiomyopathy diagnosis
|
x-ray: cardiomegaly/pulmonary congestion
EKG: sinus tachycardia, arrhythmias, conduction abnormalities echo: gold standard, dilated left ventricle, decreased wall motion, mitral regurgitation |
|
|
dilated cardiomyopathy differential
|
valvular heart disease
coronary artery disease hypertensive heart disease |
|
|
dilated cardiomyopathy management
|
treated as those with systolic heart failure
|
|
|
hypertrophic cardiomyopathy etiology
|
autsomal dominant in 60% or sporadically
aortic stenosis hypertension |
|
|
hypertrophic cardiomyopathy pathogenesis
|
unexplained myocardial asymmetrical hypertrophy results in reduced compliance of left ventricle and hypercontractility; increased ejection fraction to 80-90%; obstruction of blood flow
|
|
|
contractility in obstruction of hypertrophic cardiomyopathy
|
increased contractility increases obstruction: digitalis, beta stimulats (isoproterenol, epinephrine), tachycardia, premature beats
decreased contractility decreases obstruction: betablockers, heavy sedation/anesthesia, CCBs |
|
|
preload in obstruction of hypertrophic cardiomyopathy
|
reduced preload increases obstruction: valsalva, low volemia, standing, nitroglycerin, vasodilators, tachycardia
increased preload decreases obstruction: increased volemia, squatting, bradycardia, betablockers |
|
|
afterload in obstruction of hypertrophic cardiomyopathy
|
reduced afterload increases obstruction: hypovolemia, nitroglycerin, vasodilators
increased afterload decreases obstruction: hypervolemia, squatting, alfa stimulation, handgrip exercise |
|
|
hypertrophic cardiomyopathy presentation
|
dyspnea
angina presyncope syncope palpitations large jugular A wave S4 systolic murmur mitral regurgitation murmur |
|
|
hypertrophic cardiomyopathy diagnosis
|
EKG: LV hypertrophy, pseudo Q waves, ventricular arrhythmias
echo: gold standard, asymmetrical hypertrophy, systolic anterior motion of mitral valve, midsystolic closure of aortic valve |
|
|
hypertrophic cardiomyopathy treatment
|
betablockers, CCBs, surgery in severe cases
|
|
|
restrictive cardiomyopathy etiology
|
Neoplasia
Hemochromatosis Amyloidosis Radiation Sarcoidosis Scleroderma "restrictive Neo-HeARtSS" |
|
|
restrictive cardiomyopathy pathogenesis
|
myocardium is rigid and noncompliant, impeding ventricular filling and altering diastolic function similar to constrictive pericarditis
|
|
|
restrictive cardiomyopathy manifestations
|
dyspnea
exercise intolerance weakness elevated jugular venous pressure edema hepatomegaly ascites S3, S4 Kussmaul sign |
|
|
restrictive cardiomyopathy diagnosis
|
x-ray: mild cardiomegaly, pulmonary congestion
EKG: low voltage, conduction disturbances, Q waves echo: characteristic texture with thickening of all cardiac structures |
|
|
restrictive cardiomyopahty treatment
|
no good therapy; eventually die from CHF; consider heart transplant
|
|
|
acute pericarditis etiology
|
idiopathic
viral infections vasculitis metabolism disorders neoplasms trauma drug reactions |
|
|
acute pericarditis presentation
|
substernal or left-sided chest pain worsened by lying down, coughing and deep inspiration, relieved by sitting up and leaning forward
pericardial friction rub best heard with stethoscope diaphragm as patient sits forward and forced expiration |
|
|
acute pericarditis diagnosis and treatment
|
EKG may be diagnostic with diffuse ST elevation and upright T waves at onset of pain
treat etiology and anti-inflammatories "acute pericarditiST" |
|
|
pericardial effusion etiology
|
can be transudate (CHF, overhydration, hypoproteinemia) or exudate (TB, neoplasia) or hemopericardium (aortic aneurysm, aortic dissection, penetrating trauma, free wall rupture, bleeding due to coagulation defects)
|
|
|
pericardial effusion diagnosis and treatment
|
echo is gold standard showing echo-free space between posterior pericardium and posterior left ventricular epicardium; or heart swinging freely in pericardial sac; x-ray shows water-bottle configuration of cardiac silhouette; treat with pericardiocentesis and etiology cure
|
|
|
cardiac tamponade etiology
|
neoplasia
viral TB or suppurative pericarditis intrapericardial hemorrhage wounds postpericardiotomy uremia mediastinal radiotherapy vasculitis |
|
|
cardiac tamponade manifestations
|
dyspnea
fatigue orthopnea neck vein distention hypotension decreased heart sounds pulsus paradoxus (dissapearance during inspiration) |
|
|
cardiac tamponade diagnosis and treatment
|
clinical + echo + catheterization to confirm left and right atrial pressures
pericardiocentesis, subxiphoid surgical drainage |
|
|
Kussmaul sign
|
jugular venous distention that increases with inspiration
|
|
|
constrictive pericarditis etiology
|
thickening of pericardium due to idiopathic
open-heart surgery thoracic radiation postviral infection |
|
|
constrictive pericarditis manifestations
|
dyspnea on exertion
orthopnea (50%) right congestion signs Kussmaul sign distant heart sounds early diastolic apical pericardial knock confused with S3 |
|
|
constrictive pericarditis diagnosis
|
CT is gold standard and shows pericardial thickening and calcifications
x-ray: normal heart EKG: low-voltage T waves |
|
|
first-degree heart block
|
progressive prolongation of PR interval until P wave is blocked and ventricular beat is dropped
block is usually at AV node normal QRS PR interval shortens after dropped beat; RR interval narrows progressively; RR interval is narrower after dropped beat |
|
|
second-degree heart block
|
blocked ventricular beat not preceded by PR changes
site of block is usually infranodal wide or narrow QRS if PR is prolonged, the duration is constant |
|
|
third-degree heart block
|
all atrial beats are blocked; complete dissaciation between PR and QRS
due to fibrous degenerative changes in elderly, inferior or posterior infarction, infiltrative or granulomatous diseases, digitalis, ankylosing spondylitis Adam-Stoke (sudden asystole or ventricular tachyarrhythmias) are common associated with bradycardia and congestion treat with pacemaker |
|
|
paroxysmal supraventricular tachycardia presentation
|
ectopic tachyarrhythmias with sudden onset and termination
regular rhythm between 130-220 beats initiated by supraventricular premature beat 80% are by re-entry; |
|
|
paroxysmal supraventricular tachycardia treatment
|
right carotid massage is first line
IV verapamil or adenosine is preferred second line or IV propanolol, esmolol or digitalis cardioversion if unstable |
|
|
multifocal atrial tachycardia
|
irregular supraventricular rhythm between 100-200 beats
QRS preceded by P but P waves vary in morphology |
|
|
atrial flutter
|
regular rhythm with ventricular rate of 125-150 and atrial rate of 250-300; treat with cardioversion if unstable OR digitalis, verapamil, betablockers
|
|
|
atrial fibrillation etiology
|
associated with heart disease (rheumatic fever, coronary artery disease, CHF, hypertension)
noncardiac (hyperthyroidism, hypoxemia, alcohol intoxication) lone AF (~30%, no structural disease) idiopathic |
|
|
atrial fibrillation presentation
|
supraventricular tachyarrhythmia with disorganized fribrillatory waves that replace P waves that vary in morphology and are irregular along with rapid ventricular response (iregularly irregular); shortness of breath, dizziness, palpitations
|
|
|
EKG in flutter Vs. atrial fibrillation
|
flutter waves that replace P waves (atrial contractions) are more regular than fibrillatory waves which are irregularly irregular
|
|
|
atrial fibrillation diagnosis
|
exam: severity, clinical type (paroxysmal, persistent, first episode), frequency, duration, precipitating factors and associated disease
x-ray: lung disease EKG: verifies rhythm, LVH, pre-excitation, prior MI echo: LVH, valve disease, atrial size thyroid function: exclude hyperthyroidism |
|
|
atrial fibrillation management
|
if hemodynamically unstable --> sedation and cardioversion
else --> control rate with diltiazem, verapamil, B-blocker or digoxin if no spontaneous conversion to sinus rhythm and AF > 48 hours --> immediate cardioversion else --> anticoagulation and elective cardioversion in 3 weeks if AF persists --> long-term anticoagulation (warfarin) and rate control; catheter ablation is also common |
|
|
cardioversion drugs
|
amiodarone, defetilide, felicanide, ibutilide, propafenone, quinidine
"PROPer cardioversion DEFEcates amiodarone" drugs to maintain sinus rhythm: amiodarone, disopyramide, defetilide, flecainide, propafenone, sotalol "PROPer rhythm DEFEcates Amiodarone and DISses Sotalol" |
|
|
complications of cardioversion
|
thromboembolism --> both electrical and pharmacologic; use anticoagulants if elective cardioversion
torsade de pointes --> drug cardioversion |
|
|
Wolf-Parkinson-White syndrome diagnosis
|
ventricle is pre-excited by accesory pathway (Kent bundle); associated with paroxysmal supraventricular arrhythmia, atrial fibrillation and flutter
EKG shows short PR interval, wide QRS wave and delta waves "delta PRwIDE" |
|
|
Wolf-Parkinson-White syndrome management
|
if hemodynamically unstable --> immediate electrical cardioversion
else --> procainamide (digoxin, CCBs and BBs can inhibit normal pathway and are not indicated) definitive treatment is ablation |
|
|
ventricular tachycardia etiology
|
3 or more consecutive ventricular beats at rate >120b/min with wide and bizarre QRS
due to IHD MI cardiomyopathies mitral prolapse metabolic imbalances digoxin toxicity thioridazines |
|
|
ventricular tachycardia presentation
|
hypotension, CHF, syncope, cardiac arrest
variation in systolic pressure and intesity of heart sounds, intermittent canon waves in jugular venous pulse, extra heart sounds wide split between S1 and S2 due to asynchronous ventricular beats |
|
|
ventricular tachycardia management
|
if pulse is not present --> treat as ventricular fibrillation
else if stable pulse --> O2, IV access, lidocaine/amiodarone or procainamide or if hemodynamically unstable, cardioversion if unstable pulse --> O2, IV access, sedation, electrical cardioversion (100, 200, 300, 360J) |
|
|
differential diagnosis of arrhythmias by QRS complex
|
wide and regular: VT, SVT aberration, WPW
wide and irregular: AF rarely narrow and regular: ST, PSVT, AFL narrow and irregular: AF, MAT |
|
|
torsades de pointes etiology
|
undulating QRS on EKG baseline initiated by long-QT arrhythmias; drugs:
quinidine procainamide disopyramide phenothiazines thioridazine tricyclics lithium hypokalemia hypomagnesemia subarachnoid or intracerebral hemorrhage |
|
|
torsades de pointes diagnosis and treatment
|
undulating QRS
recurrent dizziness syncope treat underlying disorder replace antiarrhythmic with lidocaine or phenytoin cardiac pacing isoproterenol (shortens QT) if hemodynamically unstable then electrical cardioversion |
|
|
ventricular fibrillation presentation
|
significant activity on EKG with completely disorganized pattern
dead person (no pulse, no breathing, etc…) with VF EKG |
|
|
ventricular fibrillation treatment
|
CPR, electrical cardioversion, epinephrine, amiodarone (follow ACLS pulseless arrest algorhythm)
|
|
|
definition of hypertension
|
multiple readings with systolic >140mmHg or diastolic >90mmHg in the absence of specific identifiable underlying cause
|
|
|
hypertension in those with diabetes or renal disease
|
defined as pressure > 130/80
|
|
|
hypertension stages
|
preHTN --> systolic 120-129, diastolic 80-89
stage I --> systolic 140-159, diastolic 90-99 stage II --> systolic >160, diastolic > 100 |
|
|
long term cardiac complications of hypertension
|
myocardial ischemia or infarction
CHF left ventricular hypertrophy aortic aneurysm dissection |
|
|
long term cerebrovascular complications of hypertension
|
transient ischemic atack or stroke
|
|
|
long term renal complications of hypertension
|
microscopic hematuria, elevation of BUN/creatinine which may need dialysis
|
|
|
long term eye complications of hypertension
|
retinopathy
hemorrhages exudates arteriolar narrowing papilledema results in blurred vision, scotomata, sometimes blindness |
|
|
hypertension diagnosis
|
allow patient to sit quietly for 5 minutes before pressure is measured
repeat reading 3-6 times over several months before labeling as hypertensive and giving treatment |
|
|
hypertension routine laboratory analysis
|
urinalysis for protein, glucose or red blood cells
cretinine/BUN hematocrit glucose and lipids (for athersoclerosis risk) serum potassium (exclude hyperaldosteronism) ECG for LVH |
|
|
who to treat
|
diastolic >90 after 3-6 months of nonpharmacologic therapy
|
|
|
what to use for hypertension
|
best initial treatment is diuretic such as hydroclorothiazide; stage III add ACEI, ARB, CCB or beta blocker; if not enough add another drug
|
|
|
specific antihypertensives for diabetics
|
ACEIs
goal is <130/80 (as in renal insufficiency, CHF, retinopathy or stroke) |
|
|
specific antihypertensives for post MI
|
beta blockers
|
|
|
specific antihypertensives for CHF or left ventricle dysfunction post MI
|
ACEIs and/or betablocker
|
|
|
specific antihypertensives for pregnant
|
alpha methyldopa, labetalol, hydralazine or CCB
ACEIs and ARB are absolutely contraindicated diuretics relatively contraindicated |
|
|
hypertensive emergency definition
|
diastolic >120 with end-organ damage
|
|
|
malignant hypertension definition
|
has encephalopathy or nephropathy with accompanying papilledema
|
|
|
hypertensive emergency neurologic presentation
|
encephalopathy
headache confusion seizures subarachnoid or intracerebral hemorrhage |
|
|
hypertensive emergency cardiac presentation
|
chest pain
MI palpitations dyspnea pulmonary edema jugular venous distention gallops |
|
|
hypertensive emergency nephropathy presentation
|
acutely progressive hematuria, proteinuria, renal dysfunction
|
|
|
hypertensive emergency retinopathy presentation
|
papilledema, hemorrhages, blurred vision
|
|
|
hypertensive emergency diagnosis
|
no concern for white coat artifact; EKG is first initial test to exclude MI; head CT to exclude hemorrhage
|
|
|
hypertensive emergency treatment
|
IV nitroprusside and labetalol
if MI, nitroglycerin is preferred IV enalaprilat is also being used do not reduce pressure more than 25% in 1-2 hours to not compromise cerebral or myocardial perfusion (keep it above 95-100 diastolic) |
|
|
causes of secondary hypertension
|
renal artery stenosis
Conn pheochromocytoma Cushing also oral contraceptives, acromegaly, glomerulonephritis |
|
|
renal artery stenosis
|
2dary hypertension
presents with upper abdominal bruit radiating laterally best initial screen is abdominal ultrasound captopril renogram is noninvasive to confirm best confirmation is arteriogram treat with percutaneous transluminal angioplasty or surgical resection |
|
|
secondary hypertension due to Conn syndrome
|
presents with hypertension + hypokalemia
muscular weakness nephrogenic diabetes insipidus diagnosis --> high aldosterone levels in blood and urine surgical resection of adenoma or spironolactone if hyperplasia |
|
|
secondary hypertension in pheochromocytoma
|
episodic hypertension with headaches, sweating, palpitations and tachycardia
best initial test is VMA, metanephrines and free urine catecholamines then do CT or MRI to locate tumor treat with alpha adrenergics blockers followed by surgery |
|
|
secondary hypertension in Cushing
|
present with hypertension, truncal obesity, buffalo hump, menstrual abnormalities, striae, etc… best initial tests are dexamethasone suppression test and 24-hour urine cortisol; treat with surgery
|
|
|
thiazide drugs
|
hydrochlorothiazide, chlortalidone, metolazone, indapamide
|
|
|
loop diuretic drugs
|
furosemide, bumetanide, torsemide
|
|
|
potassium sparing diuretics
|
spironolactone, amiloride, triamterene
|
|
|
specific indications of diuretics
|
CHF, edematous states, african-american patients, least expensive
|
|
|
side effects of diuretics
|
↓potassium
↓ magnesium ↑calcium ↑uric acid hyperglycemia ↑LDL gynecomasia |
|
|
relative contraindications of diuretics
|
diabetes, gout, hyperlipidemia
|
|
|
specific indications of beta blockers
|
myocardial infarction or ischemic heart disease
supraventricular arrhythmias migraines glaucoma anxiety diastolic heart failure |
|
|
side effects of beta blockers
|
bronchospasm
heart block, bradycardia, conduction defects depression impotence fatigue ↓HDL, ↑triglycerides masking of hypoglycemia |
|
|
relative contraindications of beta blockers
|
asthma or COPD
conduction defects systolic heart failure diabetes |
|
|
specific indications of ACEIs
|
diabetics (prevents neuropathy)
CHF (decreases afterload) postmyocardial infarction with systolic failure |
|
|
side effects of ACEIs
|
cough, angioedema, neutropenia, hyperkalemia, taste disturbance, anaphylactoid reaction
|
|
|
relative contraindications of ACEIs
|
less effective in african americans
|
|
|
absolute contraindications of ACEIs
|
bilateral renal artery stenosis, pregnancy
|
|
|
specific indications of calcium channel blockers
|
angina
supraventricular arrhythmia migraines Raynaud esophageal spasm |
|
|
side effects of calcium channel blockers
|
peripheral edema
constipation heart block reflex tachycardia |
|
|
relative contraindications of calcium channel blockers
|
AV conduction defects, CHF from systolic dysfunction
|
|
|
angiotensin receptor blocker specific indications
|
those intolerant to ACEIs (specially due to cough)
|
|
|
angiotensin receptor blockers side effects
|
fewer than ACEIs
|
|
|
angiotensin receptor blockers absolute contraindications
|
pregnancy
|
|
|
first-line drugs for hypertension
|
diuretics, betablockers, ACEIs, ARBs
|
|
|
second-line drugs for hypertension
|
central acting sympatholytics
direct vasodilators alpha adrenergic blockers |
|
|
central-acting sympatholytics drugs
|
clonidine, guanabenz, guanfacine, methyldopa
|
|
|
specific indications of central-acting sympatholytics
|
clonidine in opiate detox
|
|
|
central-acting sympatholytics side effects
|
depression
fatigue dry mouth impotence bradycardia heart block memory loss |
|
|
methyldopa specific side effects
|
hepatitis, Coombs+ hemolytic anemia
|
|
|
relative contraindications of central-acting sympatholytics
|
elderly or depressed patients
|
|
|
direct vasodilator drugs
|
hydralazine, minoxidil
|
|
|
specific indications of direct vasodilators
|
hydralazine in eclampsia; minoxidil in baldness
|
|
|
minoxidil specific side effects
|
fluid retention, pericardial effussion, hirsutism
|
|
|
hydralazine specific side effects
|
lupus-like syndrome
|
|
|
direct vasodilator relative contraindications
|
angina
|
|
|
alpha adrenergic blocker drugs
|
doxazosin, prazosin, terazosin
|
|
|
specific indications of alpha adrenergic blockers
|
lipid disorders (they ↓LDL and ↑HDL)
prostatic hypertrophy |
|
|
side effects of alpha adrenergic blockers
|
first-dose syncope, dizziness, headache
|
|
|
prerenal azotemia etiology
|
acute renal failure due to
hypovolemia (dehydration, burns, diuretic, vomitting, diarrhea, sweating, hemorrhage) hypotension (shock, anaphylaxis) third-spacing of fluids (peritonitis) osmotic diuresis low aldosterone (Addison) low cardiac output (CHF) low albumin (nephrotic syndrome) renal artery stenosis hepatorenal syndrome (hepatic failure, vasoconstriction of afferent) ACEi-induced (in susceptible patients, vasodilation of efferent) |
|
|
prerenal azotemia diagnosis
|
BUN/creatinine ratio 20:1
low urine sodium (<20) high urine osmolality (>500) low fractional Na (<1%) specific gravity >1.010 (RAA system retains water and concentrates urine) |
|
|
postrenal azotemia etiology
|
renal failure due to bilateral obstruction to urine flow
bladder stone or clot bladder cancer prostate hypertrophy or cancer bilateral ureteral disease (retroperitoneal fibrosis) neurogenic bladder |
|
|
postrenal azotemia pathogenesis
|
bilateral obstruction to urine outflow leads to postrenal azotemia
if obstruction takes a long time it can lead to tubular necrosis |
|
|
postrenal azotemia diagnosis
|
BUN/creatinine ratio can go as high as 20:1 but then starts to decrease
there's also concentrated urine and low fractional Na need to find distended bladder on physical OR bilateral hydronephrosis on renal sonogram or CT OR large volume of urine after Foley catheter |
|
|
acute tubular necrosis etiology
|
any cause of hypoperfusion or hypodrainage (pre or postrenal azotemia) can lead to tubular necrosis if prolonged;
|
|
|
acute tubular necrosis phases
|
prodromal (between injury and acute renal failure)
oliguric or anuric post oliguric (polyuria due to tubular death and lack of urine concentration function) |
|
|
acute tubular necrosis diagnosis
|
BUN/creatinine ration close to 10:1
low urine osmolarity (<350) high urine sodium (>40) high fractional Na (>1%) brown pigmented granular casts and epithelial casts |
|
|
acute tubular necrosis management
|
no effective medical therapy, just hydration and if life-threatening, dyalisis
dopamine or diuretics cannot reverse it |
|
|
allergic interstitial nephritis etiology
|
accounts for 10-15% of intrinsic renal failure
due to drug allergy in 70% penicillins, cephalosporins, sulfas, NSAIDs, allopurinol, rifampin, quinolones, CCBs, PPIs also caused by leptospira, legionella, CMV, ricketsia and strep |
|
|
allergic interstitial nephritis presentation
|
fever (90%)
rash (25-50%) hemolysis (95%, nonspecific) eosinophilia, eosinophiluria, proteinuria, increased IgE |
|
|
allergic interstitial nephritis diagnosis
|
initial test is urinalysis looking for WBCs then Hansel or Wright stain for eosinophils
also eosinophilia, eosinophiluria, proteinuria (<2g/24h), increased IgE |
|
|
allergic interstitial nephritis management
|
remove offending agent; if persistent failure then short course of steroids
|
|
|
renal failure from pigments etiology
|
hemoglobin and myoglobin are toxic to tubules and also precipitate
rhabdomyolisis can be caused by crush injury, seizures, severe exertion, statins, hypokalemia, hypophosphatemia, ABO incompatibility |
|
|
renal failure from pigments diagnosis
|
best intitial test --> urinalysis looking for positive blood dipstick but absence of red cells
confirm by extremenly high CPK levels also rapidly rising creatinine most important test is EKG or potassium level looking for peaked T waves which can lead to arrhythmia death |
|
|
renal failure from pigments management
|
if EKG abnormalities --> calcium chloride or gluconate is best initial therapy
hydration, manitol and urine alkalinization |
|
|
acute renal failure from oxalate
|
most commonly by ethylene glycol overdose in suicide attempt
intoxicated patient with anion gap metabolic acidosis and renal insuficiency confirm with oxalate crystals in urinalysis treat with ethanol or fomepizole, dyalisis and bicarbonate |
|
|
acute renal failure from urate
|
seen in tumor lysis syndrome of leukemia/lymphoma patients
treat with allopurinol and alkalinization of urine before chemo confirm with uric acid crystals in urinalysis |
|
|
renal failure from calcium
|
hypercalcemia is most common in hyperparathyroidism
surgical resection of parathyroids indicated if renal impairment |
|
|
aminoglycoside renal toxicity
|
10-20% of drug-induced nephrotoxocity and usually reversible; due to high trough levels, not peak levels therefore give once a day to allow same bactericidal effect (peak level) and low trough levels (less toxicity)
|
|
|
amphotericin B renal toxicity
|
leads to renal insufficiency and distal tubular acidosis after several days from cumulative dosing; find high creatinine; stop medication
|
|
|
atheroembolic renal failure
|
usually angioplasty patient after several days
presents with eosinophilia, low complement, bluish discoloration of fingers and toes, livedo reticularis |
|
|
contrast agent renal failure
|
onset is faster than other toxics (12-24 hours)
rise in creatinine in 3-5 days BUN/creatinine ratio may be as high as 20:1 diabetics, hypertensives and myeloma patients are predisposed |
|
|
nephrotoxic drugs
|
aminoglycosides
contrast agents pentamidine vancomycin cyclosporine lithium indinavir ampB NSAIDs cysplatine |
|
|
NSAID nephropathy
|
mechanisms: interstitial nephritis, direct toxic, papillary necrosis, membranous GN, inhibition of vasodilatory prostaglandins
risk factors are elderly, hypertension, diabetes or other renal impairment diagnose with history of NSAIDs + rise in BUN/creatinine and sterile pyuria |
|
|
papillary necrosis
|
risk factors are sickle cell, diabetes, urinary obstruction, chronic pyelonephritis and acutely precipitated by NSAIDs
flank pain, hematuria, pyuria, fever and necrotic cells in urinalysis most accurate diagnosis is bumpy countours of renal pelvis on CT |
|
|
prevention of contrast-induced renal failure
|
most importantly is hydration; then bicarbonate and N-acetyl cysteine have been shown to decrease it
|
|
|
glomerulonephritis general presentation
|
hematuria with dysmorphic red cells, edema, hypertension, proteinuria <2gm/24h
biopsy is extremely important for specific Rx |
|
|
glomerulonephritis from vascular causes
|
Wegener
Churg-Strauss Henoch-Schonlein PAN TTP HUS cryoglobulinemia |
|
|
glomerulonephritis from glomerular disease
|
Goodpasture
postinfectious GN IgA nephropathy RPGN Alport SLE hypertension amyloid diabetes (nodular or diffuse glomerulosclerosis) |
|
|
Wegener glomerulonephritis presentation
|
glomerulonephritis associated with rhinitis, sinusitis, nasal ulcers, cough and hemoptysis
it's systemic and also affects skin, joints, eyes nonspecific: ↑ESR, anemia, leukocytosis best initial test: c-ANCA (anti-proteinase-3) most accurate: biopsy of kidney or lung looking for granulomas treat with cyclophosphamide + steroids |
|
|
Churg-Strauss glomerulonephritis
|
glomerulonephritis with respiratory symptoms similar to Wegener
eosinophilia and adult-onset asthma are characteristic best initial tests are ↑eosinophils and p-ANCA (antimyeloperoxidase) definitive is lung biopsy showing granulomas treat with cyclo + steroids |
|
|
Goodpasture syndrome
|
glomerulonephritis + hemoptysis, cough and shortness of breath
no other organs are affected best intial test: anti-basement membrane Abs to type IV colagen confirm with biopsy showing hemosiderin-ladden macrophages (in lungs) and linear Ig deposits (kidneys) treat with plasmapheresis and steroids |
|
|
polyartheritis nodosa
|
involves every organ except lungs
kidney involvement presents as GN and renal insufficiency there are systemic nonspecific signs abdominal and joint pain are prominent best initial tet is p-ANCA (present only in minority) biopsy is confirmatory (usually sural nerve) treat with cyclo + steroids |
|
|
Henoch-Schonlein purpura
|
palpable purpura, arthralgias, abdominal pain and GN/renal insufficiency due to systemic IgA deposition
biopsy is confirmatory but not performed in majority of patients because it's self-limited treatment is supportive, steroids if severe |
|
|
IgA nephropathy (Berger)
|
most common glomerulopathy worldwide
IgA deposition that affects only kidney causing GN presents as hematuria 1-2 days following viral illness or pharyngeal infection 40-50% progress to end-stage renal disease initial test --> IgA (↑ in 50%) confirm with kidney biopsy showing IgA deposits no proven effective therapy |
|
|
postinfectious glomerulpnephritis
|
due to any organism but mostly from throat or skin infection with group A strep
hematuria, red cell casts, proteinuria, edema, hypertension initial test: ASO and anti-hyaluronic acid test biopsy --> humps on electron micro and granular IgG/C3 deposits on IF treat hypertension and proteinuria with ACEi or ARBs and penicillin for infection |
|
|
thrombotic thrombocytopenic purpura
|
pentad for clinical diagnosis
hemolytic anemia, uremia, thrombocytopenia, fever, neurologic findings intravascular hemolysis with schistocytes and fragmented RBCs, ↑LDH, ↑reticulocytes, ↓haptoglobin mild disease resolves, if severe --> plasmapheresis don't transfuse platelets or give antibiotics |
|
|
hemolytic uremic syndrome
|
E. coli 0157:H7
triad for clinical diagnosis --> hemolytic anemia, uremia, thrombocytopenia intravascular hemolysis with schistocytes and fragmented RBCs, ↑LDH, ↑reticulocytes, ↓haptoglobin mild disease resolves, if severe --> plasmapheresis don't transfuse platelets or give antibiotics |
|
|
cryoglobulinemia
|
renal diasease associated with hep B or C, joint pain, neuropathy and purpura; no GI involvement (different from HSP); ↑ESR, ↓complement and confirmation with cryoglobulins; treat underlying hepatitis with interferon and ribavirin; if severe --> pulse steroids and plasmapheresis
|
|
|
diabetic nephropathy
|
directly proportional to duration of diabetes
nodular (Kimmelstein-Wilson) or diffuse glomerulosclerosis screen for microalbuminuria and creatinine level treat with ACEi or ARB |
|
|
lupus nephritis
|
asymptomatic proteinuria or hematuria or severe renal disease requiring dialysis
initial test is dsDNA confirm and determine treatment with kidney biopsy if sclerosis --> no therapy needed if proliferative --> steroids with mycophenolate |
|
|
Alport syndrome
|
glomerular disease + congenital eye problems and sensorineural hearing loss
|
|
|
rapidly progressive glomerulonephritis
|
can be due to other glomerular diseases or idiopathic in which there's crescent formation
|
|
|
amyloidosis etiology
|
AL type is from Ig light chains in multiple myeloma
AA is from rheumatoid arthritis, IBD, myeloma |
|
|
amyloidosis presentation
|
glomerulonephritis
restrictive cardiomyopathy, arrhythmias, heart blocks macroglosia carpal tunnel syndrome malabsorption |
|
|
amyloidosis diagnosis
|
biopsy of involved organ such as kidney shows green birefringence in Congo red stain
|
|
|
amyloidosis treatment
|
control underlying disease; melphalan and prednisone can control protein production
|
|
|
nephrotic syndrome etiology
|
primary: membranous GN, Nil, membranoproliferative, focal-segmental GN
1/3 associated with diabetes, hypertension or myeloma any glomerulonephritis can convert to nephrotic syndrome if severe enough |
|
|
nephrotic syndrome presentation
|
proteinuria >3.5g/24h, edema, hyperlipidemia, hypoalbuminemia
can have hyperlipiduria (maltese cross) and hypercoagulable states (arterial or venous thrombosis from loss of antithrombin, proteins C and S) |
|
|
nephrotic syndrome diagnosis
|
initial test is proteinuria >3.5g/24h or albumin/creatinine ratio >3.5 on urinalysis
renal biopsy is most accurate |
|
|
nephrotic syndrome management
|
treat underlying disease
if primary --> steroids if unresponsive --> cyclo or mycophenolate ACEIs for all with proteinuria |
|
|
membranous glomerulonephritis
|
most common nephrotic syndrome in adults
associated with lymphoma, breast cancer, endocarditis, chronic hepatitis, lupus treat with steroids |
|
|
Nil lesion
|
minimal change disease most common in children, 15% adults
electron micro shows fusion of foot processes responds to steroids |
|
|
membranoproliferative glomerulonephritis
|
nephrotic syndrome associated with chronic hepatitis and hypocomplement
immunofluorescensce detects mesangial IgM deposits steroid-resistant, dipyridamole and aspirin are useful |
|
|
focal segmental glomerulonephritis
|
nephrotic syndrome associated with heroin use and HIV; limited response to steroids; ESRD over 5-10 years
|
|
|
things to check for in urinalysis
|
proteinuria, hematuria, nitrites, bacteriuria, casts
|
|
|
proteinuria
|
urine dipstick detects only albumin not Ig light chains
found in glomerular or tubular disease, glomerulonephritis, diabetes, fever, CHF, severe exercise, orthostatic microalbuminuria is 30-300g/24h in diabetic nephropathy |
|
|
hematuria
|
found in diseases of bladder or kidney; stones, cancer, bleeding disorders, trauma, cyclo, glomerulonephritis, cystitis, prostatitis
|
|
|
nitrites
|
gram negative bacteria reduce nitrate to nitrite and is marker for infection
|
|
|
bacteriuria
|
if isolated, has limited significance unless pregnant since they can develop pyelonephritis; >100,000 colonies indicates urinary infection
|
|
|
hyaline casts
|
dehydration; not necessarily disease
|
|
|
red cell casts
|
glomerulonephritis
|
|
|
broad, waxy casts
|
chronic renal failure
|
|
|
granular/muddy casts
|
acute tubular necrosis
|
|
|
white cells in urinalysis
|
pyelonephritis, interstitial nephritis
|
|
|
indications for dyalisis
|
life-threatening abnormalities such as refractory fluid overload, acidosis, pericarditis, encephalopathy, other neuropathies, hyperkalemia, uremia (nausea, vomitting, bleeding diathesis)
|
|
|
end-stage renal disease etiology
|
diabetic nephropathy
hypertension glomerulonephritis (15%) cystic disease (5%) interstitial nephritis (5%) requires dialysis |
|
|
anemia as ESRD complication
|
normo normo anemia from decreased production of erythropoietin; replace EPO
|
|
|
hypocalcemia as ESRD complication
|
from decreased production of 1,25 dihydroxy vitamin D (1-hydroxylase); vitamin D replacement
|
|
|
hyperphosphatemia as ESRD complication
|
from decreased ability to excrete
treat with calcium carbonate or calcium acetate cinacalcet in refractory cases aluminum-containing binders should not be used due to dementia and bone abnormalities risk |
|
|
osteodystrophy as ESRD complication
|
osteitis fibrosa cystica
bone cysts due to ↓vitamin D --> secondary hyperparathyroidism manage by improving calcium and treating hyperPTH |
|
|
hypertension and atherosclerosis as ESRD complication
|
acceleratd atherosclerosis not known why
most common COD for dialysis patients hypertension goal is 130/80 |
|
|
infection as ESRD complication
|
second most common COD
white cells don't function well under uremia staph is most common due to catheters |
|
|
bleeding as ESRD complication
|
uremia-induced platelet dysfunction increases bleeding time
treated with desmopressin to increase vWB and factor VIII |
|
|
minor signs present in ESRD
|
pruritus
hyperuricemia decreased libido weakness fatigue glucose intolerance not indications for dialysis |
|
|
dietary treatment in ESRD
|
restricted Na, K, protein, magnesium, phosphate
|
|
|
renal transplant
|
survival
live related donor 95%/1 year, 72%/5years cadaver donor 88%/1 year, 58%/5 years dialysis alone 30-40%/5 years average wait for transplant is 2-4 years graft rejection prevention with cyclosporine, tacrolimus, mycophenolate |
|
|
renal tubular acidosis type I etiology
|
problem in distal tubules
usually sporadic or secondary to autoimmune disease, ampB, lithium, NSAIDs, nephrocalcinosis, sickle cell, familial, chronic hepatitis |
|
|
renal tubular acidosis type I presentation
|
inability to develop ↑[H+] in urine
urine pH >5.4 secondary hyperaldosteronism nephrocalcinosis nephrolithiasis hypokalemia |
|
|
renal tubular acidosis type I diagnosis
|
Acid load test: give amonium chloride which should lower urine pH, with disease urine pH remains high; serum bicarbonate ~10; hypokalemia
|
|
|
differentiate RTA from diarrhea acidos
|
urine anion gap = (Na + K) - Cl
both have normal serum anion gap metabolic acidosis but diarrhea has negative urine anion gap (↑ urine Cl-) and RTA type I cannot excrete H+ so Cl- will be low and urine anion gap is positive |
|
|
renal tubular acidosis type I treatment
|
oral bicarbonate because proximal tubule reabsoprtion is intact and potassium replacement
|
|
|
renal tubular acidosis type II etiology
|
inability to absorb bicarbonate in proximal tubules
Fanconi, Wilson, amyloidosis, myeloma, acetazolamide, vitD deficiency, secondary hyperPTH, chronic hypocalcemia |
|
|
renal tubular acidosis type II presentation
|
initial urine pH is basic but then becomes <5.4
hypokalemia serum bicarbonate 18-20 malabsorption of glucose, amino acids, urate, phosphate osteomalacia/rickets |
|
|
renal tubular acidosis type II diagnosis
|
sodium bicarbonate IV is not reabsorbed; basic urine in presence of acidemia; bicarbonate in urine
|
|
|
renal tubular acidosis type II treatment
|
potassium, thiazides and large amounts of HCO3
|
|
|
difference between type I and type II RTA
|
type I is inability to excrete H+ and has nephrolithiasis
type II inability to reabsorb HCO3 and has osteomalacia/rickets |
|
|
renal tubular acidosis type IV etiology
|
aldosterone deficiency or adrenal insensitivity to angiotensin II
diabetes (50%) Addison sickle cell renal failure |
|
|
renal tubular acidosis type IV presentation
|
asymptomatic hyperkalemia
mild to moderate renal failure hyperchloremic (nonanion gap) metabolic acidosis |
|
|
renal tubular acidosis type IV diagnosis
|
high urine sodium with oral salt restriction is diagnostic
|
|
|
renal tubular acidosis type IV treatment
|
fludrocortisone has mineralocorticoid effect
|
|
|
types of kidney stones
|
calcium oxalate (70%)
calcium phosphate (10%) Mg/aluminum/phosphate (struvite) uric acid cysteine indinavir |
|
|
causes of hypercalciuria
|
increased absorption: vitamin D intoxication, ↑vitamin D from sarcoidosis or granulomatous diseases; familial, idiopathic; resorptive: hyperPTH, multiple myeloma
|
|
|
causes of hyperoxaluria
|
primary familial, enteric; fat malabsorption binds calcium and leaves oxalate to be reabsorbed
|
|
|
causes of uric acid stones
|
acid tubules and high uric acid from gout, hematologic malignancies, Crohn
radiolucent on x-rays |
|
|
causes of struvite stones
|
infections with urease-producing proteus, pseudomonas, klebsiella; highly alkaline urine
|
|
|
nephrolithiasis presentation
|
constant flank pain, hematuria, pain radiating to groin
stones < 5mm should pass spontaneously |
|
|
nephrolithiasis diagnosis
|
plain x-ray is rarely used
ultrasound, spiral CT strain the urine check serum and urine calcium never do intravenous pyelogram |
|
|
nephrolithiasis treatment
|
analgesia, hydration, bed rest
shockwave lithotripsy for stones <2cm but fragments may obstruct ureteroscopy percutaneous removal (anesthesia and hospital stay) |
|
|
adult polycystic kidney disease presentation
|
flank pain, hematuria, palpable mass, UTIs, calculi
hypertension hepatic cysts (40%) colonic diverticula intracraneal aneurysm mitral valve prolapse |
|
|
adult polycystic kidney disease diagnosis and treatment
|
ultrasound and CT; treatment is nonspecific with management of hypertension, UTIs and calculi
|
|
|
simple cysts
|
cysts with irregular walls or debris should be aspirated to exclude malignancy
dialysis can cause cysts |
|
|
serum osmolality formula
|
(2 x sodiun) + (BUN / 2.8) + (glucose / 18); if glucose and BUN are normal then ~ 2 x Na + 10
|
|
|
hyponatremia specific etiologies
|
pseudohyponatremia, hypervolemic state, hypovolemic state, euvolemic states, SIADH
|
|
|
hypovolemic hyponatremia causes
|
dehydration (with free water replacement)
vomitting diarrhea sweating (with free water replacement) diuretics ACEIs renal salt waste Addison cerebral sodium waste |
|
|
hypervolemic hyponatremia causes
|
CHF, nephrotic syndrome, cirrhosis, renal insufficiency
|
|
|
hyponatremia general presentation
|
Na < 135mEq; symptoms depend on how fast it drops
neurologic in nature forgetfulness --> disorientation --> obtundation --> seizure --> coma |
|
|
hyponatremia management
|
if asymptomatic --> fluid restriction
mild symptoms --> normal saline + furosemide seizure or coma --> 3% hypertonic saline avoid central pontine myelinolysis by correcting Na at 0.5-1mEq/hour or 2mEq if seizure or coma |
|
|
pseudohyponatremia
|
total Na is normal, serum Na is low
for every 100mg/dL of hyperglycemia there's 1.6mEq/L decrease in Na hyperlipidemia causes Na lab artifact |
|
|
euvolemic hyponatremia
|
psychogenic polydipsisa, hypothyroidism, diuretics, ACEIs, endurance exercise, SIADH
|
|
|
SIADH etiology
|
small cell lung CA, pancreas CA, ectopic ADH secretion
TB, lung abscess head injury, CVA, encephalitis chlorpropamide, clofibrate, vincristine, vinblastine, cyclophosphamide, carbamazepine |
|
|
SIADH presentation
|
water retention
ECF expansion without edema or hypertension (natriuresis) hyponatremia concentrated urine signs of cerebral edema when hyponatremia is severe (irritability, confusion, seizures, coma) |
|
|
SIADH diagnosis
|
hyponatremia <130mEq/L
urine sodium > 20mEq/L maintained hypervolemia ↓RAA low electrolytes in blood (BUN, creatinine, uric acid) low albumin |
|
|
SIADH management
|
treat underlying cause
fluid restriction to 800-1000mL/d demeclocycline (AVP inhibitor) in case of cerebral edema: hypertonic 3% saline 200-300mL IV in 3-4h |
|
|
insensible water losses and hypernatremia
|
↑skin loss (sweating, burns, fever, exercise), respiratory infections
|
|
|
gastrointestinal water losses and hypernatremia
|
osmotic diarrhea from gluten or lactose intolerance, some infectious diarrhea
|
|
|
transcellular water shift and hypernatremia
|
rhabdomyolysis or seizures cause muscle to take up lots of water
|
|
|
renal disease and hypernatremia
|
diabetes insipidus or osmotic diuresis (diabetic KA, nonketotic hyperosmolar coma, mannitol, diuretics
|
|
|
central diabetes insipidus etiology
|
neoplastic/infiltrative lessions in hypothalamus or pituitary adenomas, craniopharyngiomas, leukemia, sarcoid histocytosis
surgery, radiotherapy, trauma, anoxia, hypertension, meningitis, encephalitis, TB, syphillis could also be idiopathic |
|
|
nephrogenic diabetes insipidus etiology
|
idiopathic or secondary to
hypercalcemia hypokalemia sickle cell amyloidosis myeloma pyelonephritis sarcoidosis Sjogren lithium demeclocycline colchicine |
|
|
diabetes insipidus presentation
|
polyuria, polydipsia
hypernatremia, urine specific gravity <1,010 severe dehydration, weakness fever, altered mental state prostration, nocturia |
|
|
diabetes insipidus diagnosis
|
plasma/urine osmolarity ratio falls to the right of shaded area; then if vasopressin response is normal --> central diabetes insipidus, else nephrogenic
|
|
|
diabetes insipidus differential
|
primary polydipsia
drug-induced polydipsia from chlorpromazine, anticholinergics, thioridazine hypothalamic disease |
|
|
diabetes insipidus management
|
CDI: ADH hormone replacement or ADH secretion stimulators (chlorpropamide, clofibrate, carbamazepine); NDI: HCTZ or amiloride or chlortalidone as well as correction of calcium balance
|
|
|
hypokalemia from GI losses
|
vomitting, diarrhea, tube drainage
|
|
|
hypokalemia from transcellular shift
|
alkalosis, ↑insulin, B12 replacement, ↑beta-adrenergeic activity (trauma)
|
|
|
hypokalemia from urinary losses
|
diuretics, ↑aldosterone states (Conn, licorice, Barter, Cushing, renal artery stenosis), ↓magnesium, type I and II RTA
|
|
|
hypokalemia presentation
|
muscular weakness to paralysis; arrhythmias; rhabdomyolisis
|
|
|
hypokalemia diagnosis
|
normal levels is 3.7-5.2mEq/L; in emergencies do EKG looking for T-wave flattening and U-waves
|
|
|
hypokalemia treatment
|
treat underlying cause
give 4-5mEq/Kg/point; IV max 10-20mEq/h don't use dextrose containning fluids complication is fatal arrhythmia |
|
|
hyperkalemia from transcellular shift
|
pseudohyperkalemia (secondary hemolysis, mechanical trauma from venipuncture, platelets >1,000,000, WBCs >100,000)
acidosis insulin deficiency tissue breakdown (rhabdomyolisis, tumor lysis, seizures) |
|
|
hyperkalemia in acidosis
|
for every 0.1 in pH potassium increases 0.7 points
|
|
|
hyperkalemia from renal causes
|
renal failure, hypoaldosteronism (ACEIs, type IV RTA, adrenal enzyme deficiency, heparin), Addison, amiloride, spironolactone
|
|
|
hyperkalemia presentation
|
muscular weakness when K > 6.5
abnormal cardiac conduction hypoventilation |
|
|
hyperkalemia diagnosis
|
normal levels 3.7-5.2mEq/L; ECG: peaked T waves, wide QRS, short QT or prolonged PR
|
|
|
hyperkalemia management
|
if ECG abnormalities -->
calcium chloride (membrane stabilizer) sodium bicarbonate (alkalosis, not in same IV line as calcium) glucose/insulin (30-60 minutes to work) cation exchange resin (absorbs 1mEq og K/gram) dialysis |
|
|
anion gap formula
|
(Na + K) - (HCO + Cl); normal = 8-14
|
|
|
low anion gap metabolic acidosis
|
myeloma (myeloma proteins are cations, HCO and Cl go up)
↓albumin (for every 1 point, 2 point decrease in anion gap) lithium (decreases Na level) "MAL" |
|
|
normal anion gap metabolic acidosis
|
diarrhea, renal tubular acidosis, uretero sigmoidoscopy "DiREct (ureter sigmo)"
|
|
|
increased anion gap metabolic acidosis
|
lactate
aspirin methanol uremia diabetic ketoacidosis paraldehyde propylene glycol ethylene glycol |
|
|
respiratory acidosis
|
hypoventilation of any cause
COPD pickwickian obesity suffocation opiates sleep apnea kyphoscoliosis myopathies neuropathy effusion aspiration |
|
|
metabolic alkalosis from H+ loss
|
steroids
GI loss (vomitting, nasgastric suction) renal loss (Conn, Cushing, ↑ACTH, licorice) ↓Cl intake, diuretics |
|
|
metabolic alkalosis from HCO3 retention
|
bicarbonate administration, contraction alkalosis, milk-alkali syndrome
|
|
|
metabolic alkalosis from transcellular shift
|
hypokalemia
|
|
|
respiratory alkalosis
|
hyperventilation of any cause
anemia pulmonary embolus sarcoid anxiety pain "SAAPP" |
|
|
gram+ catalase+ cocci
|
coagulase+: stah aureus
caogulase-: staph epidirmidis (novobiocin sens), staph saprophyticus (novobiocin res) |
|
|
gram+ catalase- cocci
|
alpha hemolytic -->
pneumococcus (optochin sens) viridans (optochin res) beta hemolytic --> group A strep pyogenes (bacitracin sens) group B stret agalactiae (bacitracin res) |
|
|
gram+ rods
|
bacillus, clostridium, corynebacterium, listeria
|
|
|
gram- cocci
|
meningococcus (maltose fementer), neisseria gonorrheae (maltose non fermenter)
|
|
|
gram- cocobacillus
|
Haemophilus
brucella pastereulla bordetella |
|
|
gram- rods
|
lactose fermenters --> e. coli, klebsiella
lactose nonfermenter oxidase- --> salmonella, shigella, proteus lactose nonfermenter oxidase+ --> campylobacter, pseudomonas, vibrio, H. pylori |
|
|
DNA viruses
|
HHAPPPPy: herpes, hepadna, adeno, parvo, papilloma polyoma, pox
|
|
|
RNA+ viruses
|
Calici (Norwalk), PEeCoRnA, Flavi (hepC, dengue, yellow fever, WNV), Toga (rubella), Corona, Retro. "Call Pico and Flava To Come Rap"
|
|
|
RNA- viruses
|
PaRaMyxo, Rhabdo, Arena, Filo, Orthomyxo (influenza), Bunya, Delta
"Para Rabiar in the Arena, Fill OR Buny" |
|
|
arbovirus
|
Togavirus, flavivirus, bunyavirus
|
|
|
meningitis etiology
|
bacterial: pneumococcus (adults), mningococcus (children/adolescents), agalactiae (neonates)
listeria is more common in immunosupressed staph aureus (neurosurgery) cryptococcus (HIV) RMSP (geographic) Lyme (borrelia, geographic) TB, syphilis viral: coxackie, HIV, herpes simplex |
|
|
meningitis presentation
|
photophobia, headache, nuchal rigidity
fever, nausea, vomitting altered mental status, seizures, neurological deficits (specially CN VIII) petechial rash (meningococcus) writs/ankle centripetal rash (RMSF) facial nerve palsy (Lyme) abnormal chest x-ray (TB) |
|
|
meningitis diagnosis
|
lumbar puncture is initial procedure
if papilledema, focal motor deficits, seizures, mental status changes, or HIV --> do CT of head first CSF analysis: ↑WBCs (neutrophils) --> bacterial; ↑WBCs (lymphocytes) --> viral, ricketsia, Lyme, TB, syphilis; ↑proteins (mostly in bacterial, but any) ↓glucose (mostly bacterial) Lyme and RMSF have specific serology cryptococcus detect with India ink test and serum/CSF cryptococcal antigen syphilis with VDRL or FTA-ABS TB with culture or PCR |
|
|
meningitis treatment
|
empirical: vancomycin + ceftriaxone +- ampicillin (HIV, steroids, pregnancy or malignancies)
listeria is resistant to all cephalosporins vancomycin if resistant pneumococcus Lyme --> ceftriaxone cryptococcus --> amphotericin + fluconazole neurosyphilis --> high-dose penicillin dexamethasone as adjuvant in bacterial meningitis |
|
|
encephalitis etiology
|
most commonly by HSV-1
also by VZV, CMV, coxackie and encephalitis viruses HSV-1 has predilection for temporal lobes |
|
|
encephalitis presentation
|
altered mental status with fever and headache are main clues; can also have stiff neck
|
|
|
encephalitis diagnosis and treatment
|
due lumbar puncture first
PCR of CSF is sensitive and specific for HSV-1 CT or MRI to exclude other diseases and may see temporal lobe involvement IV acyclovir or gancyclovir/foscarnet for CMV |
|
|
brain abscess etiology
|
organisms spread to brain from
otitis media, sinusitis, mastoiditis, dental infections, endocarditis, pneumonia, HIV most common --> strep pneumonia (60-70%) bacteroides (20-40%) enterobacteriacea (25-35%) staph (10%) toxoplasmosis in AIDS can often by polymicrobial |
|
|
brain abscess presentation
|
headache is most common symptom
fever focal neurologic deficits (60%) seizures |
|
|
brain abscess diagnosis
|
initial test is contrast CT
MRI is more accurrate precise etiology is with examination of abscess fluid 90% of HIV brain abscess is from toxoplasma or lymphoma and diagnosis is made if it responds to 10-14 days with pyrimethadine or sulfadiazine |
|
|
brain abscess treatment
|
stereotactic aspiration (preferred) or surgical excision
antibiotics are also given in combination depending on etiology if toxoplasmosis --> pyrimethadine and sulfadiazine else give combo; example: penicillin for strep, metronidazole for anaerobes and third-gen ceph for gram- |
|
|
otitis media etiology
|
preceeded by viral upper respiratory infection with edema of eustachian tube
strep pneumo (35-40%) H. influenzae (25-30%) moraxella (15-20%) rest is viral etiology same breakdown as sinusitis and bronchitis |
|
|
otitis media presentation
|
ear pain
fever decreased hearing red bulging tympanic membrane on physical |
|
|
otitis media diagnosis
|
physical exam of ear
|
|
|
otitis media treatment
|
amoxicillin is DOC
can also use second-gen ceph penicillin allergies --> azi/clarithromycin quinolones have broader spectrum than required |
|
|
sinusitis etiology
|
strep pneumo (35-40%)
H. influenzae (25-30%) moraxella (15-20%) rest is viral etiology same breakdown as otitis media and bronchitis |
|
|
sinusitis presentation
|
facial pain, headache, postnasal, purulent drainage; fever in 50%
|
|
|
sinusitis diagnosis
|
clinical diagnosis
routine imaging is not recommended if in doubt or no response to treatment --> CT sinus puncture may be necessary |
|
|
sinusitis treatment
|
if mild or uncomplicated --> oral pseudoephedrine, oxymetazoline
if severe --> amoxicillin is DOC can also use second-gen ceph penicillin allergies --> azi/clarithromycin viral sinusitis resolves within 10 days with symptomatic treatment (antihistamines, NSAIDs, decongestants) |
|
|
pharyngitis etiology
|
majority are viral
S. pyogenes is only 15-20% but is most important due to complications |
|
|
pharyngitis presentation
|
sore throat
cervical adenopathy fever pharynx inflammation and exudate are suggestive of S. pyogenes (or EBV) horaseness and cough are not suggestive of pharyngitis |
|
|
pharyngitis diagnosis
|
rapid strep antigen test are unsensitive but specific and diagnostic but absence doesn't exclude
|
|
|
pharyngitis treatment
|
penicillin; macrolides if allergic
|
|
|
influenza
|
influenza A or B virus leads to coryza, nonproductive cough, sore throat, conjunctival injection and systemic symptoms as fever, myalgia, headache and fatigue
diagnosis confirmation is with rapid antigen detection treat symptoms with acetaminophen and antitussives specific treatment is oseltamivir and zanamivir vaccination is recommended in older than 50, lung or cardiac diasease, immunosupressed, diabetics |
|
|
bronchitis etiology
|
vast majority are caused by viruses
then strep pneumo, nontypable Haemophilus, moraxella, mycoplasma cigarette smoke is predisposing factor |
|
|
bronchitis presentation and diagnosis
|
cough and sputum production with normal x-ray confirms diagnosis
lungs are clear to auscultation fever may occur bacterial etiology is suggested by discolored sputum |
|
|
bronchitis treatment
|
mild cases require no treatment
acute exacerbations of chronic bronchitis are treated with amoxicillin, doxycycline or TMP-SMX repeated infections: amoxicillin/clavulanate, clarithromycin, azithromycin, 2nd or 3rd-gen cephs or quinolones |
|
|
lung abscess etiology
|
90% have oral anaerobes peptostrep, prevotella and fusobacterium
45% only anaerobic, 45% mixed, 10% aerobes aerobics found are staph, e. coli, klebsiella, pseudomonas associated oral periodontal disease or predisposition to aspiration |
|
|
lung abscess presentation
|
fever, cough, sputum, chest pain, putrid odor, chronic course with weight loss, anemia, fatigue
|
|
|
lung abscess diagnosis
|
sputum Gram stain will not show anaerobes
chest x-ray may show cavitary lesion most commonly in lower lobes or posterior segmenet of right upper lobe aspiration and analysis of abscess fluid confirms |
|
|
lung abscess treatment
|
empiric drug is clindamycin; drainage is not required
|
|
|
pneumonia etiology
|
in children <5 viruses are most common
older than 5, pneumococcus is leading cause typical agents (40-60%) S. pneumoniae, Haemophilus, moraxella atypicals: legionella, mycoplasma, chlamydia |
|
|
pneumonia predisposing factors
|
cigarette smoking, diabetes, alcoholism, malnutrition, obstruction from tumors, immunosupression
|
|
|
pneumonia associations: haemophilus
|
smokers and COPD patients
|
|
|
pneumonia associations: mycoplasma
|
atypical presentation in young otherwise healthy patients
|
|
|
pneumonia associations: legionella
|
epidemic; older smokers
associated with infected water sources and air conditioning systems |
|
|
pneumonia associations: pneumocystis jiroveci
|
HIV+ <200 CD4
|
|
|
pneumonia associations: coxiella
|
Q fever; exposure to animals specially specially when they are giving birth
|
|
|
pneumonia associations: klebsiella
|
alcoholics
|
|
|
pneumonia associations: staph aureus
|
following viruses or viral bronchitis, specially influenza
|
|
|
pneumonia associations: coccidioidomycosis
|
southwestern deserts
|
|
|
pneumonia associations: chlamydia psittaci
|
birds
|
|
|
pneumonia associations: histoplasma
|
bird droppings and spelunking
|
|
|
pneumonia associations: bordetella
|
cough with inspiratory whoop and post-tusive vomitting
|
|
|
pneumonia associations: francisella
|
hunters or exposure to rabbits
|
|
|
pneumonia associations: SARS/avian flu
|
travel to south east asia
|
|
|
pneumonia associations: anthrax, yersinia, francisella
|
bioterrorism
|
|
|
pneumonia presentation
|
cough, fever, sputum production, pleuritic chest pain, tachypnea
viral and atypicals produce a non-productive dry cough on physical: rales, ronchi, dullness to percusion, bronchial breath sounds, increased fremitus, egophony bacterial sputum is purulent and can be mixed with blood (rusty, pneumococcus) or blood and mucous (currant-jelly, klebsiella) |
|
|
pneumonia diagnosis
|
chest x-ray is first --> localized or diffuse infiltrates and alveolar or interstitial pattern
next --> sputum Gram stain and culture (most specific for lobar pneumonia) atypicals don't show in Gram stain or culture mycoplasma --> cold agglutinins legionella --> antigen tests and charcoal yeast culture pneumocystis --> increased LDH in bronchoalveolar lavage chlamydia pneumonia, coxiella, coccidiodes all have specific antibody titers |
|
|
pneumonia major severity signs
|
hypoxia (PO2<60mmHg)
O2 saturation <94% respiratory rate >30/min confusion, uremia, hypotension |
|
|
pneumonia minor severity signs
|
high fever
hypothermia leukopenia pulse >125/min hyponatremia dehydration determined by high BUN |
|
|
empiric treatment for pneumonia outpatients
|
azithromycin or clarithromycin are DOC
alternative are levofloxacin, moxifloxacin, gatifloxacin |
|
|
empiric treatment for pneumonia inpatients
|
new quinolones OR 2nd/3rd gen ceph with macrolide or doxyclycline
|
|
|
empiric treatment for hospital-acquired pneumonia
|
3rd gen ceph with antipseudomonal activity OR imipenem OR piperacillin/tazobactam
should also cover MRSA with vancomycin or linezolid |
|
|
haemophilus pneumonia specific treatment
|
2nd or 3rd gen ceph
|
|
|
mycoplasma pneumonia specific treatment
|
macrolides, doxycycline or new quinolone
|
|
|
legionella pneumonia specific treatment
|
macrolides, doxycyline or new quinolone
|
|
|
pneumocystis pneumonia specific treatment
|
TMP-SMX
add steroids if PO2<70mmHg or A-a >35mmHg if allergic to sulfa use IV pentamidine or atovoquone prophylaxis with dapsone or atovoquone |
|
|
coxiella pneumonia specific treatment
|
doxycycline
|
|
|
staph pneumonia specific therapy
|
oxacillin, nafcillin, etc… if MRSA --> vacomycin or linezolid
|
|
|
coccidioides pneumonia specific therapy
|
only need treatment if diseminated disease
mild diseasse --> fluconazole or itraconazole severe disease --> ampB |
|
|
pneumococcal vaccine indications
|
older than 65
serious lung, cardiac, liver or renal disease steroid patients HIV+ splenectomized patients diabetics leukemia/lymphoma patients |
|
|
tuberculosis etiology
|
25% of world population is exposed; higher risk of exposure in alcoholics, healthcare workers, prisoners, homeless shelters, nursing homes, HIV, steroids, organ transplant, leukemia, lymphoma
|
|
|
tuberculosis presenation
|
cough, sputum, fever, weight loss, night sweats and abnormal lung exam
may also involve any organ specially lymph nodes, meninges, GI and GU |
|
|
tuberculosis diagnosis
|
chest x-ray is best initial test in symptomatic patients, PPD in asymptomatic
x-ray shows apical infiltrates and sometimes cavitations, adenopathy and calcifications (Ghon complex) acid-fast stain of sputum (3 smears >90% sensitive) culture is specific and needed for bug sensitivity testing if acid-fast is unrevealing can do thoracentesis, gastric aspirate in children, biopsy or needle aspiration of organ involved or lumbar puncture in meningitis pleural biopsy is most sensitive look for casseating granulomas |
|
|
tuberculosis treatment
|
empiric treatment is combo of INH/pyridoxine, rifampin, pyrazinamide, ethambutol for first 2 months or until sensitivty testing; then INH + rifampin for another 4 months
if sensitivity is not known give also ethambutol TB meningitis add steroids + 12 months TB in pregnancy 9 months |
|
|
tuberculosis drugs side effects
|
all cause liver toxicty except streptomycin
INH --> peripheral neuropathy (give pyridoxine) ethambutol --> optic neuritis rifampin --> red/orange metabolites pyrazinemide --> benign hyperuricemia |
|
|
PPD test generalities
|
used to screen asymptomatic populations at risk of TB to see if they have been exposed; consits of intradermal injection of the PPD with induration of the skin 48-72 hours after
if test is <10mm, do a second test to rule out false negative if positive do chest x-ray and acid-fast stain positive PPD with no evidence of active disease receive prophylaxis with INH+pyridoxine for 9 months |
|
|
PPD test > 5mm induration
|
considered positive if
close contacts of active TB cases HIV+ abnormal chest x-ray steroids or organ transplant |
|
|
PPD test > 10mm induration
|
considered positive if
children < 4 leukemia or lymphoma injection drug users prisoners homeless healthcare worker immigrants (recent) nursing home residents diabetics dialysis CLIP HINDuration |
|
|
PPD test > 15mm induration
|
considered positive for people with no risk factors for TB
|
|
|
food poisoning/infectious diarrhea etiology
|
campylobacter is most common
salmonella (raw eggs and poultry) e. coli (traveler's diarrhea, undercooked hamburger meat) B. cereus (reheated fried rice) giardia, cryptosporidia (contaminated water) V. parahemolyticus (contaminated shellfish) V. fulnificus (raw shellfish) rotavirus, Norwalk agent (children) C. difficile (antibiotics) C. botulinum (canned food) C. perfringes (unrefrigerated meats) |
|
|
food poisoning/infectious diarrhea presentation
|
most importantly is presence of blood and specific symptoms
bloody diarrhea --> salmonella, shigela, yersinia, invasive e. coli, campylobacter watery diarrhea --> protozoans except entamoeba, clostridium, vibrio, viruses, B. cereus, staph predominantly nausea/vomitting --> B. cereus, staph |
|
|
food poisoning/infectious diarrhea diagnosis
|
if there's no blood in stool then check for leukocytes in stools with methylene blue test
then do culture for specific etiology for protozoans direct stool examination for parasites or ova |
|
|
food poisoning/infectious diarrhea treatment
|
empiric antibiotics until stool culture and if there's abdominal pain, bloody stools and fever or hypotension; high-volume stools and dehydration don't justify antibiotics
empirical treatment is ciprofloxacin or fluoroquinolone+metronidazole scombroid is treated with antihistamines giardia with metronidazole isospora with TMP/SMX doxycycline for vibrio |
|
|
acute viral hepatitis presentation
|
jaundice, dark urine, light-colored stools, fatigue, malaise, weight loss, tender liver, hepatomegaly
indistiguishable from drug-induced hepatitis; hep b and C can also have serum sickness, arthritis, rash; PAN is associated with hep B |
|
|
acute viral hepatitis diagnosis
|
all hepatitis gives ↑total and ↑direct bilirubin
ALT > AST in viral AST>ALT in drug-induced alkaline phosphatase and GGTP may not be elevated unless canalicular damage |
|
|
viral hepatitis serology
|
IgM indicates acute infection with A, C, D or E viruses
IgG antibody to A, C, D or E indicates old, resolved disease hep C activity is followed with PCR viral load hep B acute diagnosis: ↑HbsAg, ↑IgM-HbcAb and HbeAg (infectivity) resolution is indicated by ↓HbsAg, ↑HbsAb, ↑HbcAb-IgG (only marker in window-period), ↑HbeAb-IgG |
|
|
acute viral hepatitis treatment
|
ne effective treatment for acute viral hepatitis
chronic hep B --> either interferon, entecavir, adefovir, lamiduvine chronic hep C --> combo of interferon and ribavirin treatment for cirrhosis is transplant after needlestick with hep B and if no adequate levels from vaccine --> HBIg + hep B vaccine; no post-exposure prophylaxis for hep C |
|
|
urethritis
|
by gonococcus or chlamydia, ureaplasma, mycoplasma, trichomona or HSV
purulent urethral disharge, dysuria, urgency, frequency diagnose with gram stain showing coffee bean-shaped diplococci or fluorescent antibodies for chlamydia (on urethral swab or urine) treat with single-dose ceftriaxone IM and single-dose azithromycin orally |
|
|
pelvic inflammatory disease
|
gonococcus, chlamydia, mycoplasma, enterobacteria
lower abdominal pain on palpation of cervix, uterus or adnexa cervical motion tenderness is key fever, leukocytosis and discharge also do gram stain of discharge and culture on Thayer-Martin do pregnancy test diagnosis is clinical; laparoscopy is definitive may do culdocentesis or sonography treat with doxycycline and cefoxitin (inpatient) or single-dose ceftriaxone and doxycyline for two weeks for outpatient |
|
|
syphilis presentation
|
primary --> chancre (1-3 weeks) and regional nontender lymphadenopathy
secondary --> cutaneous rashes (6-12 weeks) on flexor areas, lympahdenopathy and condylomata lata (papules at mucocutaneous junctions) latent stage --> may persist for life tertiary --> 1/3 of patients, gummas lead to tabes dorsalis and Argyll-Robertson pupil |
|
|
syphilis diagnosis
|
screening: VDRL, RPR
specific: FTA-ABS, MHA-TP, darkfield exam false positive VDRL in EBV, collagen vascular disease, TB, subacute bacterial endocarditis |
|
|
syphilis treatment
|
2.4 million units if IM benzathine penicilline given once for primary and secondary and once a week 2 weeks for latent (VDRL >1:8 without symptoms); tertiary is treated with 10-20 million units/day IV for 10 days; if allergic give doxycycline but desensitize for tertiary and pregnancy
|
|
|
chancroid
|
caused by Haemophilus ducreyi
small, soft, painful papules that coalesce and become ulcers with ragged edges tender and enlarged inguinal nodes diagnosis is clinical Gram stain and culture to confirm treat with single-dose azithromycin or ceftriaxone OR erythromycin for 7 days OR cipro for 3 days |
|
|
lymphogranuloma venereum presentation
|
small, transient, nonindurated lesion that ulcerates and heals quickly producing unilateral inguinal node enlargement, multiple drainning sinuses that persist or recur; also fever, malaise, joint pains, headaches
|
|
|
lymphogranuloma venereum diagnosis and treatment
|
clinical diagnosis
high or rising titer of complement fixing antibodies isolate chlamydia trachomatis from pus in buboes treat with doxycycline |
|
|
granuloma inguinale
|
painless red nodule that turns into elevated granulomatous mass by donovantia granulomatis
looks like conylomata lata or carcinoma diagnose with Giemsa or Wright stain, punch biopsy treat with doxycyline or ceftriaxone |
|
|
gential herpes
|
vesicles on genital area or mucous membranes that become eroded ulcers with red areola; itching and soreness; can have inguinal lymphadenopathy; diagnose with Tzanck test and culture; treat with acyclovir, famcyclovir, valacyclovir or foscarnet; explain relapsing nature
|
|
|
genital warts
|
papilloma virus causes condylomata acuminata which are warm, moist, pink pedunculated swellings with cauliflower appearance
clinical diagnosis treatment: destruction (curettage, sclerotherapy, trichloroacetic acid), cryotherapy, podophyllin, imiquimod, laser removal |
|
|
painless papules and pustules that ulcerate near genital areas
|
condylomata lata; syphilis
|
|
|
painful small soft papules that become ulcers with ragged edges and coalesce
|
chancroid; H. ducreyi
|
|
|
painless small transient nonindurated lesion that ulcerates and heals quickly leaving scar
|
lymphogranuloma venereum; C. trachomatis
|
|
|
painless red nodule develops into elevated granulomatous mass
|
granuloma inguinale; donovania granulomatis, calymmatobacterium granulomatis
|
|
|
painful vesicles on skin or mucous membranes that become ulcers with red areola
|
genital herpes; HSV
|
|
|
painless soft moist redish swellings that grow rapidly into pedunculated masses with califlower appearance
|
genital warts
condylomata acuminata papilloma virus |
|
|
painful genital lesions
|
chancroid
genital herpes |
|
|
painless genital lessions
|
condylomata lata
lymphogranuloma venereum granuloma inguinale condylomata acuminata |
|
|
cystitis etiology
|
infection of bladder by E. coli, proteus, klebsiella
predisposed by urinary stasis, tumors, stones, strictures, prostatic hypertrophy, neurogenic bladder, sexual intercourse |
|
|
cystitis presentation
|
dysuria, frequency, urgency and suprapubic (but not flank) tenderness
may also have hematuria, low fever |
|
|
cystitis diagnosis and treatment
|
screening test is urinalysis looking for WBCs, RBCs, protein or bacteria
nitrites indicate gram- bacteria urine culture with >100,000 colonies per mL of urine is confirmation treat with 3 days of TMP/SMX or any quinolone (not pregnancy) 7 days for diabetics |
|
|
acute bacterial pyelonephritis etiology
|
ascension of E. coli, klebsiella, proteus
predisposed by female sex, obstruction due to strictures, tumors, calculi, prostatic hypertrophy, neurogenic bladder, vesicouretheral reflux, catheter; catherterized immunocompromised patients are predisposed to candida |
|
|
acute bacterial pyelonephritis presentation
|
fever, chills
frequeny, dysuria flank pain, costovertebral angle tenderness nausea/vomitting |
|
|
acute bacterial pyelonephritis diagnosis
|
clinical diagnosis with confirmation by clean-catch urinalysis and culture >100,000 bacteria/mL
if patient does not improve in 3 days or complications are suspected --> ultrasound or CT is indicated |
|
|
acute bacterial pyelonephritis treatment
|
10-14 days with fluoroquinolone OR
ampicillin + gentamycin OR third-gen ceph if can't tolerate medication --> hospitalization |
|
|
perinephric abscess etiology
|
abscess from kidney cortex to surrounding areas due to E. coli, klebsiella, proteus
predisposed by kidney stones (20-60%) strictures prostatic hypertrophy neurogenic bladder trauma diabetes |
|
|
perinephric abscess presentation
|
insidious onset (2-3 weeks) of fever, flank pain, palpable flank mass, abdominal pain, and persistence of symptoms after pyelonephritis treatment
|
|
|
perinephric abscess diagnosis and treatment
|
urinalysis and culture of urine
then ultrasound and aspiration of abscess for definitive etiology and sensitivity quinolone, ampicillin/gentamycin, third-gen ceph drainage is necessary |
|
|
impetigo etiology
|
superficial pustular infection with due mainly to staph aureus and group A strep
|
|
|
impetigo presentation
|
maculopapules that progress to vesicles, pustules and bullae with golden crusts
can lead to lymphangitis, furunculosis or cellulitis more common on limbs and face, may follow trauma to skin |
|
|
impetigo diagnosis and treatment
|
clinical diagnosis
treat with first-gen ceph OR oxacillin, cloxacillin, dicloxacillin can also use topical mupirocin or bacitracin in mild cases if allergic use macrolides |
|
|
erysipelas
|
superficial cellulitis due to group A strep
tender, demarcated, shiny red, indurated, edematous lesions on limbs or face treat with semisynthetic penicillin or first-gen ceph if undistinguishable with cellulits, else penicillin for Group A strep |
|
|
tinea etiology
|
dermatophytes: microsporum, trichophyton, epidermophyton
|
|
|
tinea presentation
|
corporis: papulosquamous lesions with riased border in the body; pedis: macerated and scaling borders; unguium: thickened nails; capitis: small scaly semibold graysish patched on head; cruris: ringed lesions on crural folds and inner thighs; barbae: on face
|
|
|
tinea diagnosis and treatment
|
potassium hydroxide preparation; culture as definitive test; treat with terbinafine or itraconazole orally for capitis, corporis and unguium; topical clotrimazole/ketoconazole for cruris, pedis and mild corporis
|
|
|
candidiasis etiology
|
candida infection more frequently in:
systemic antibacterial therapy obesity diabetes corticosteroid or antimetabolites pregnancy malignancies blood dyscrasias HIV |
|
|
intertriginous candidiasis presentation
|
intertriginous: well-demarcated, erythematous, itchy, exudative patches rimmed with red small pustules; in groin, gluteal folds (diper rash), axilla, umbillicus, inframmary areas
|
|
|
vulvovaginitis presentation
|
candidiasis with white or yelloish discharge with inflammation of the vaginal wall and vulva; common in pregnancy and diabetes
|
|
|
oral candidiasis
|
also known as thrush; white patches of exudates on tongue or bucal mucosa
|
|
|
candidal paronychia
|
painful red swelling around the nail
|
|
|
candidiasis diagnosis and treatment
|
potassium chloride on slide, culture is definitive
treat with topical nystatin or azoles if serious infection or paronychia use amphotericin and fluconazole |
|
|
tinea versicolor
|
pityrosporum orbiculare (malassezia furfur) leads to tan/brownish scaling macules that coalesce on neck, face and abdomen; diagnose with KOH showing spaghetti and meatballs; treat with topical selenium sulfide or azoles
|
|
|
scabies
|
due to itch mite or sarcoptes scabiei; pruritus, burrows and papules on skin folds; immunocompromised and Down patients can have malodorous discharge; diagnose by showing parasites in scrapings with mienral oil; treat with permethrin, lindane or ivermectin
|
|
|
pediculosis
|
due to pediculus humanus capitis, pediculus humanus corporis, phthirus pubis; itching, excoriations, erythematous macules and papules may have secondary bacterial infection; diagnose with direct analysis of hair-bearing surfaces; treat with permethrin, lindane
|
|
|
molluscum contagiosum
|
small waxy papules with central umbilication due to poxvirus
specially in children and HIV clinical diagnosis treat by cryotherapy, curettage, electrocautery |
|
|
osteomyelitis etiology
|
most common organism is staph
acute hematogenous: in children occurs mostly in metaphysis of tibia and femur, in adults in the vertebral bodies secondary to contiguous infection: recent trauma or prosthetic (could be polymicrobial) vascular insufficiency: diabetics over 50, small bones of lower limb and majority are polymicrobial |
|
|
osteomyelitis presentation
|
pain, erythema, swelling and tenderness over affected bone; in vascular insuf. May have ulcer; sometimes also drainning tract
|
|
|
osteomyelitis diagnosis
|
plain x-ray is usually first test but takes at least 2 weeks to show periosteal elevation
technetium scan and MRI detect it much earlier a normal ESR strongly excludes osteomyelitis bone biopsy and culture is best diagnostic test and its needed |
|
|
osteomyelitis treatment
|
empiric: semisynthetic penicillin or vancomycin + aminoglycoside or third-gen ceph
then specific treatment total is 6-12 weeks adults also need drainage and debridment |
|
|
septic arthritis etiology
|
joint infection mostly by gonococcus but also by gram+ (85%, staph 60%)
other gram- (10-15%) or polymicrobial (5%) main risk factor for gonococcal is sexual activity nongonococcal is mostly hematogenous spread by bites, direct inoculation by surgery or trauma, RA, OA, prothesis, gout, sickle cell, IV drug use, diabetes, HIV |
|
|
septic arthritis presentation
|
gonococcal: polyarticular (50%) swollen, tender, erythematous joint with decreased range of motion also with tenosynovitis, migratory polyarthralgia, and petechiae or purpura
non-gonococcal is mostly monoarticular and doesn't have systemic involvement |
|
|
septic arthritis management
|
joint aspiration along with empiric nafcillin combined with aminoglycoside or third-gen ceph
for gonococcal: ceftriaxone |
|
|
gas gangrene etiology
|
80% C. perfringens associated with trauma, war and motor vehicle accidents; the wound must be deep, necrotic and without exit to surface
|
|
|
gas gangrene presentation
|
pain, swelling and edema 1-4 days after incubation
later hypotension, tachycardia, fever, crepitation and renal failure |
|
|
gas gangrene diagnosis
|
gram+ rods on stain without white cells, culture and gas bubble on x-ray are suggestive
direct visualization of pale, dead muscle with sweet-smelling discharge is definitive diagnosis |
|
|
gas gangrene management
|
24 million units of penicillin/day or clindamycin if allergic + debridment or amputation
hyperbaric oxygen might be of benefit |
|
|
infective endocarditis predisposing factors
|
dental procedures
oral and upper respiratory surgery some GI procedures GU surgery prosthetic heart valves valvular heart disease catheters to heart IV drug abuse |
|
|
top 5 organisms of endocarditis in native valves
|
strep viridans (50-60%)
staph aureus (20-30%) other strep (15-20% enterococci (5-15%) staph epidermidis (1-3%) |
|
|
top 3 organisms of endocarditis in narcotic addicts
|
staph aureus (60-95%), streptococci (10-20%), staph epidermidis (5-10%)
|
|
|
top 3 organisms of endocarditis in prosthetic valves
|
staph epidermidis (40-50%, 10-20 days later)
staph aureus (15-20%, 40-60 days later) strep viridans (5-20%, 20-30 days later) |
|
|
acute endocarditis etiology
|
bactermia with staph aureus seeds previously healthy valves and produces large vegetations, fever, spesis, splenomegaly
|
|
|
subacute endocarditis etiology
|
strep viridans is most common
low virulence seeding of abnormal valves with small vegetations made of fibrin, platelets, debris and bacteria |
|
|
infective endocarditis presentation
|
fever + new heart murmur + anemia
chills, sweats, weakness, dyspnea, anorexia, cough, embolic events (petechiae, splinter hemorrhages, Janeway lesions), skin manifestation, splenomegaly, FROM JANE |
|
|
infective endocarditis major diagnostic criteria
|
positive blood culture and abnormal echo; need both or 1 major/3minor for diagnosis
|
|
|
infective endocarditis minor criteria
|
cardiac lesion from IV drug use
vascular events (arterial emboli, septic lung infarcts, Janeway) immunologic events (Osler, Roth, GN, rheumatoid factor) microbiologic evidence (active infection consistent with endocarditis) need 3 minor and 1 major or 2 major for diagnosis |
|
|
infective endocarditis empiric treatment
|
antistaph (nafcillin) + antistrep (penicillin/ampicillin) + gentamicin
change as soon as specific agent is known by blood culture |
|
|
infective endocarditis specific treatment for strep viridans
|
4 weeks penicillin OR if allergic, 4 weeks of ceftriaxone or vancomycin OR 2 weeks of penicillin or ceftriaxone + gentamicin
|
|
|
infective endocarditis specific treatment for native valve/staph aureus
|
if methicillin sensitive:
4-6 weeks of nafcillin + 5 days gentamicin OR cefazolin or vancomycin + 5 days of gentamicin if allergic for methicillin resistant: 4-6 weeks of vancomycin |
|
|
infective endocarditis specific treatment for enterococcus
|
4-6 weeks of penicillin/ampicillin + gentamicin OR vacomycin + gentamicin
|
|
|
major criteria for infective endocarditis surgery
|
progressive or unresponsive CHF
recurrent systemic emboli persistent bacteremia despite antibiotics fungal etiology extravalvular infection prosthetic valve dehiscence or obstruction recurrence despite therapy |
|
|
minor criteria for infective endocarditis surgery
|
resolved CHF with therapy
single systemic embolic event large aortic or mitral vegetations on echo prosthetic valve infection other than penicillin sensitive strep gram- tricuspid endocarditis persistent fever new regurgitation |
|
|
indications of prophylaxis for infective endocarditis
|
when there's serious cardiac defect and procedure causing bacteremia; for dental procedures give amoxicillin or clindamycin/macrolide if allergic
|
|
|
cardiac conditions that indicate infective endocarditis prophylaxis
|
prosthetic heart valves
previous bacterial endocarditis most congenital cardiac malformations |
|
|
conditions that don’t require infective endocarditis prophylaxis
|
surgically corrected systemic pulmonary shunts, rheumatic valve dysfunction, hypertrophy cardiomyopathy, mitral valve prolapse with regurgitation, surgical repaired intracardiac defects
|
|
|
acute pericarditis etiology
|
any infectious agent
coxsackie and ECHO viruses are most common viruses vascular --> SLE, RA, scleroderma 1/3 of uremic patients neoplasia adjacent to heart hypothyroidism mediastinal irradiation rheumatic fever injury to heart |
|
|
acute pericarditis presentation
|
sharp pleuritic chest pain improved by leaning forward; friction rub heard at apex; low fever
|
|
|
pericardial tamponade presentation
|
signs and symptoms of perdicarditis plus pulsus paradoxus, distended neck veins, tachycardia, hypotension
|
|
|
acute pericarditis diagnosis
|
diffuse ST elevation and maybe PR depression
echo normal in viral but used to detect effusion pericardiocentesis for microbiology |
|
|
acute pericarditis therapy
|
treat underlying cause; if viral give indomethacin or ibuprofen or prednisone if no response or if TB; pericardiocentesis for large effusions
|
|
|
myocarditis etiology
|
any infectious agent but coxackie B is very common
also radiotherapy, drugs, vascular disease, hyperthyroidism |
|
|
myocarditis presentation
|
asymptomatic or any presentation
signs of myocardial dysfunction (dyspnea, fatigue) or rapid progression to chest pain and arrhythmia may have S3 and murmurs |
|
|
myocarditis diagnosis
|
any EKG alteration like ST-T wave changes, heart blocks
elevated cardiac enzymes may be found may have left ventricular systolic dysfunction on echo viruses may be isolated from body fluids or titers of serum antibodies are found |
|
|
myocarditis treatment
|
supportive for viral (resolves spontaneously); steroids can be damaging
|
|
|
Lyme disease presentation
|
80% develop erythema migrans rash 3-30 days after bite
flulike illness occurs in 50% neurologic symptoms develop weeks later in 10-20% (facial paralysis, meningitis, encephalitis or headaches) heart block, arrhythmia, myocarditis or pericarditis in <10% migratory polyarthritis develops months to years later in 60%; |
|
|
Lyme disease diagnosis
|
diagnostic criteria are presence of rash with at least one late manifestation + ELISA and western blot looking for anti borrelia antibodies (serum studies may not false negative early when rash is still present)
|
|
|
Lyme disease treatment
|
rash, facial palsy and joint pain with doxycyline
if serious neurologic or cardiac --> IV ceftriaxone |
|
|
AIDS etiology
|
decrease in CD4 count by HIV; in US transmitted mostly by men who have sex with men or in heterosexuals; in developing world is transmitted mostly by heterosexuals; takes 5-10 years to drop CD4 from 700 to 200
|
|
|
principal opportunistic infections in AIDS
|
pneumocystis jirovecii, cytomegalovirus, mycobacterium avium, toxoplasma, cryotococcus
|
|
|
pneumocystis jirovecii pneumonia presentation
|
pneumonia, dyspnea on exertion, dry cough, fever, chest pain when CD4>200/uL
|
|
|
pneumocystis jirovecii pneumonia diagnosis
|
bronchoscopy with bronchoalveolar lavage for direct indentification; chest x-ray may be normal or bilateral interstitial infiltrates; elevated serum LDH
|
|
|
pneumocystis jirovecii pneumonia management
|
TMP-SMX (first-line, may cause rash) OR dapsone/trimethoprim OR primaquine/clindamycin; pentamidine (may cause pancreatitis); steroids if severe pneumonia (PaO2<70mmHg or A-a >35mmHg
|
|
|
pneumocystis jirovecii pneumonia prophylaxis
|
used if CD4>200/mm3; TMPSMZ (most effective) OR dapsone OR atovaquone
|
|
|
CMV retinitis
|
blurry vision, double vision, any visual disturbance in patients with CD4<50/uL; treat with oral valganciclovir and intravitreal ganciclovir
|
|
|
CMV colitis
|
diarrhea in patients with CD4<50/uL; treat with oral valganciclovir
|
|
|
CMV esophagitis
|
odynophagia, fever, retrosternal pain; shallow ulcers in distal esophagus seen with upper GI endoscopy; do biopsy; treat with oral valganciclovir
|
|
|
CMV encephalitis
|
altered mental status and cranial nerve deficits with CD4 <50/uL; treat with IV ganciclovir
|
|
|
CMV prophylaxis in AIDS
|
oral valganciclovir for maintenance
|
|
|
CMV therapy side effects
|
ganciclovir: neutropenia; foscarnet: renal toxicity; cidofovir: renal toxicity
|
|
|
mycobacterium avium complex presentation
|
fevers, night sweats, bacteremia, wasting, anemia, diarrhea in patients with CD4<50/uL
|
|
|
mycobacterium avium complex diagnosis and therapy
|
blood culture or culture of bone marrow, liver or other tissue or fluid; treat with clarithromycin + ethambutol +- rifabutin; prophylaxis if CD<100/uL with weekly azithromycin or clarithromycin twice daily
|
|
|
toxoplasmosis presentation
|
brain mass lesion, headache, confusion, seizures, focal neurologic deficits in patient with <100 CD4/uL
|
|
|
toxoplasmosis diagnosis
|
ring enhancing lesion on CT or MRI with edema and mass effect; shrinkage after 2 weeks of therapy is diagnostic; also toxoplasma serology an CSF PCR; brain biopsy may be necessary if no shrinkage
|
|
|
toxoplasmosis treatment
|
pyrimethamine + sulfadiazine; if sulfa allergy substitute with clindamycin; prophylaxis with TMP/SMX OR dapsone/pyrimethamine
|
|
|
cryptococcosis presentation
|
mainly meningitis, fever, headache, malaise in patient with CD4<100/uL
|
|
|
crytocococcal meningitis diagnosis
|
india ink of CSF and specific cryptococcal antigen testing in CSF and serum
|
|
|
cryptococcal meningitis therapy
|
IV ampB 10-14 days followed by oral fluconazole for maintenance; fluconazole is not recommended for general use prophylaxis
|
|
|
vaccinations in HIV+
|
all should receive pneumococcus, influenza and hepatitis B vaccines
|
|
|
diseases with CD4 200-500/uL
|
oral thrush, Kaposi sarcoma, TB, zoster, lymphoma
|
|
|
diseases with CD4 100-200/uL
|
pneumocystis pneumonia, dementia, PML, disseminated histoplasmosis, coccidiomycosis
|
|
|
diseases with CD4 <100/uL
|
toxoplasmosis, cryptococcal meningitis, cryptosporidiosis, disseminated herpes
|
|
|
diseases with CD4 <50/uL
|
CMV, mycobacterium avium complex, CNS lymphoma
|
|
|
HIV viral load monitoring
|
to monitor response to antiretrovirals, determine risk of complications and prognosis; higher load indicates CD4 will drop more rapidly
|
|
|
nucleoside reverse transcriptase inhibitors
|
zidovudine (AZT, ZDV), didanosie, stavudine, lamivudine, emtricitabine, tenofovir, abacavir, zalcitabine
|
|
|
zidovudine
|
NRTI; leukopenia, anemia, gastrointestinal
|
|
|
didanosine
|
NRTI; pancreatitis, peripheral neuropahty
|
|
|
stavudine
|
NRTI; peripheral neuropathy
|
|
|
lamivudine
|
NRTI; nothing additional to placebo
|
|
|
emtricitabine
|
NRTI; nothing additional to placebo
|
|
|
tenofovir
|
NRTI; nucleotide instead of nucleoside
|
|
|
abacavir
|
NRTI; hypersensitivity reaction; discontinue immediately and don't restart
|
|
|
zalcitabine
|
NRTI; pancreatitis, peripheral neuropathy, lactic acidosis
|
|
|
protease inhibitors
|
nelfinavir, indinavirm ritonavir, saquinavir, amprenavir, lopinavir, atazanavir; all cause hyperlipidemia, hyperglycemia and elevated liver enzymes plus specific effects
|
|
|
nelfinavir
|
PI; GI side effects
|
|
|
indinavir
|
PI; nephrolithiasis, hyperbilirubinemia
|
|
|
ritonavir
|
PI; severe GI disturbance
|
|
|
saquinavir
|
PI; GI effects
|
|
|
lopinavir
|
PI; diarrhea
|
|
|
atazanavir
|
PI; diarrhea, asymptomatic hyperbilirubinemia
|
|
|
non-nucleoside reverse transcriptase inhibitors
|
noncompetitive inhibitors; efavirenz, nevirapine, delavirdine
|
|
|
efavirenz
|
NNRTI; neurologic effects, somnolence, confusion, psychiatric
|
|
|
nevirapine
|
NNRTI; rash, hepatotoxicity
|
|
|
delavirdine
|
NNRTI; rash
|
|
|
when to start antiretroviral therapy
|
CD4 <350/uL or viral load by PCR-RNA >55,000 by RNA
|
|
|
which antiretrovirals to start with
|
2 NRTI + PI or NNRTI OR 2 NRTI + efavirenz OR 2 nrti + 2 PI
|
|
|
antiretroviral contraindicated in pregnancy
|
efavirenz
|
|
|
what is considered adequate therapy
|
any combo that decreases viral load near or to undetectable amounts and increases CD4; in the first month viral load should drop at least 50%
|
|
|
HIV management in pregnant women
|
25-30% of children will be truly HIV+ if no treatment is given; recommended is AZT + NRTI + PI; C-section indicated if viral load >1,000 at time of delivery; should not breastfeed
|
|
|
HIV post-exposure prophylaxis
|
recommended AT + lamiduvine + nelfinavir OR any fully suppressive combo for 4 weeks
|
|
|
Q fever
|
coxiella by inhalation and found in placenta of cattle, sheep and goats; can cause febrile illness, atypical pneumonia, hepatitis, hepatomegaly, endocarditis; diagnose with specific serology; treat with doxycyline
|
|
|
Rocky Mountain spotted fever
|
ricketsia transmitted by wood tick in south, upper south and midwest; abrupt onset fever, headache, erythematous maculopapules with centripetal spread and neurological deficits; differential with syphilis; serology and biopsy; treat with doxycyline
|
|
|
tetanus etiology and presentation
|
neurotoxin by C. tetani in 1-7 days; tonic spasms, respiratory arrest, dysphagia, stiff body, lockjaw, arm flexion and leg extension
|
|
|
tetanus diagnosis and treatment
|
clinical diagnosis; tetanus toxoid (10-year boosters), surgical debridment; tetanus immunoglobulin antitoxin, 10-14 days of penicillin
|
|
|
aspergillosis etiology
|
most common is aspergilus fumigatus causes pulmonary disease in immunocompromised; risk factors are neutropenia <500, steroids and cytotoxics
|
|
|
aspergillosis presentation
|
allergic asthma-like signs, mycetoma with hemoptysis
|
|
|
aspergillosis diagnosis
|
abnormal chest x-ray and aspergillus in sputum; eosinophilia and elevated IgE; positive skin testing; if invasive, biopsy necessary
|
|
|
aspergillosis treatment
|
allergic: steroids and asthma medications, not antifungals; mycetoma: surgical removal; if invasive: voriconazole and caspofungin
|
|
|
drawbacks of screening
|
iatrogenia, expensive, unpleasant, inconvenient, harmful, stigma
"screening-HESIItant" |
|
|
valid screening test
|
shown to decrease overall mortality in screened population in randomized double-blind trial
|
|
|
malignancies to regularly screen for
|
colon, breast and cervix cancers
|
|
|
screening for colon cancer, no significant family history
|
after age 50: annual fecal occult blood, sigmoidoscopy every 5 years and barium enema. Preferred modality: colonoscopy every 10 years
|
|
|
screening for colon cancer, high-risk patients
|
colonoscopy every 5 years starting at age 40 or 10 years younger than at the age at which youngest affected relative was diagnosed
|
|
|
screening for breast cancer
|
mammography every 1-2 years from age 40
breast exam by physician every 3 years from ages 20-30 self breast exam is no longer recommended patients with strong family history should receive prophylactic tamoxifen |
|
|
screening for cervix cancer
|
Pap smear annually starting 3 years after becoming sexually active or at age 21
patients <30 screen annually if conventional methods or every 2 years if using liquid-based patients >30 screen every 2 years if >3 normal annual Pap smears |
|
|
vaccinations for travelers
|
Hep A
Hep B malaria rabies yellow fever typhoid fever polio meningococcal meningitis depending on case |
|
|
Hep A vaccination
|
if traveler is leaving within 2 weeks of being seen give Hep A vaccine plus immune serum globuline; booster after 6 months confers immunity for 10 years; also recommended for day-care employees, homosexual men and chronic liver disease
|
|
|
Hep B vaccination
|
for travelers who will work closely with indigenous population or will engage in sexual intercourse, receive medical or dental care and those who plan to remain abroad for over 6 months; also IV drug users, male homosexuals, contact with carriers, frequent exposure to blood or chronic liver disease
|
|
|
prophylaxis for malaria
|
for patients traveling to Mexico, Central America or Caribbean: chloroquine
for areas with chloroquine resistance: mefloquine or doxycyline (2nd line) for pregnant: atovaquone plus proguanil |
|
|
prophylaxis for rabies
|
patients travelling to Mexico, India, Asia
intradermal vaccine or intramuscular in case patient is also receiving malaria prophylaxis not routine for most |
|
|
yellow fever vaccine
|
for patients travelling to sub-saharan Africa and some south American countries
|
|
|
typhoid vaccination
|
travelers to developing countries; live atenuated vaccine is contraindicated in HIV patients; intramuscular polysacchride vaccine is preferred
|
|
|
polio vaccination
|
given to unvaccinated travelers to developing countries
three doses of inactivated vaccine or one-time booster if previously immunized |
|
|
meningococcal meningitis vaccine
|
travelers to endemic or epidemic areas (Nepal, sub-Saharan Africa, northern India); required for pilgrims to Mecca; patients with functional asplenia or terminal complement deficiencies
11-12 years |
|
|
tetanus and diptheria immunization
|
unvaccinated adults should receive three doses
first 2 are 1-2 months apart and third dose 6-12months later booster every 10 years 2, 4, 6 months; 15-18 months; booster 10 years |
|
|
influenza vaccination
|
recommended annually for all healthy adults after age 50
patients with history of cardiopulmonary disease diabetes hemoglobinopathy pregnant women will be in 2nd or 3rd trimester during influenza season |
|
|
pneumococcal vaccination
|
Revaccination recommended for all over 65
or at any age in case of: sickle-cell patients, splenectomy, cardiopulmonary disease, alcoholism, cirrohsis, immunocompromised (hematologic malignancies, chronic renal failure, HIV, etc.) Patients with high risk of fatal infections should be revaccinated every 5 years "enCCApSSIlated over 65" |
|
|
varicella vaccine
|
live attenuated recomemded for all adults who lack childhood history of varicela except immunocompromised or pregnant
|
|
|
MMR vaccine
|
live attenuated vaccine given to children or unvaccinated adults born after 1956; except HIV or pregnant;
given at 12-15 months with pre-school booster 4-6 years |
|
|
smoking cessation
|
responsible for 1/5 of deaths in US
Ask Advise Attempt Assist Arrange follow-up |
|
|
osteoporosis prevention
|
women older than 65 should receive DEXA scan
if low body weight or fracture risk start screening at 60 |
|
|
abdominal aortic aneurysm screening
|
ultrasound to male smokers older than 65
no screening necessary for male non-smokers and women regardless of smoking history |
|
|
hypertension screening
|
patients older than 18, at every visit, at least every 2 years
|
|
|
cholesterol screening
|
start screening at age 35 in men and 45 in women without risk factors
patients with risk factors for atherosclerosis screen routinely after 20 years of age |
|
|
diabetes screening
|
if risk factors are present (obesity, impaired fasting glucose, high-risk ethnicity, positive family history, hypertension, hyperlipidemia)
two fasting glucose above 126mg/dL or random measure greater than 200 w/symptoms are diagnostic |
|
|
alcohol abuse screening
|
two "yes" answers to CAGE questionare
Cut down Annoyed Guilty Eye opener |
|
|
important considerations in evaluating arthritis
|
1. distribution and number of joints involved
2. acute or chronic 3. systemic symptoms 4. signs of inflammation |
|
|
important tests in rheumatologic disease
|
joint aspiration (cell count, crystals, cultures, Gram)
antinuclear antibodies rheumatoid factor antineutrophil cystoplasmic antibodies antiphospholipid antibodies |
|
|
joint aspiration test
|
arthrocentesis; synovial fluid tests to run:
cell count crystals cultures Gram stain hemogram (anemia) ESR if <2,000 WB consider OA or trauma if 5,000-50,000 WBCs probable inflammatory etiology but also consider septic if > 50,000 WBCs consider septic etiology; |
|
|
ANAs
|
seen in 5% of normal people
95% of SLE as well as Sjogren, CREST, systemic sclerosis, MCTD ANA subsets: anti-ds-DNA (60% of SLE, indicates diseae activity and nephritis) anti-Smith (SLE 25-30%) anti-histone (drug-induced lupus, 95%) anti-Ro/SSA (neonatal lupus, Sjogren, ANA-negative lupus) anti-LA/SSB (Sjogren) anti-centromere (CREST) anti-RNP (MCTD, 100%) |
|
|
rheumatoid factor
|
IgM against Fc portion of IgG found in 70% of patients of RA and 5% of healthy adults
neither sensitive nor specific for RA but has prognostic significance |
|
|
ANCAs
|
cANCA are diffuse antibodies against neutrophils seen in 90% of Wegner cases
pANCA are localized in around the neutrophil nucleus and atacks myeloperoxidase and it's seen in PAN and Churg-Strauss |
|
|
antiphospholipid antibodies
|
also called lupus anticoagulant or anticardiolipin antibodies
associated with hypercoagulable state of antiphospholipid syndrome high PTT false-positive VDRL spontaneous abortions thromboembolism |
|
|
rheumatoid arthritis etiology
|
unknown (most cases) or due to mycoplasma or parvovirus infection
|
|
|
rheumatoid arthritis presentation
|
need four of the following criteria:
morning stiffness > 1h swelling of wrists, MCPs and PIPs swelling of three joints symmetric involvement joint erosions on x-rays RF positive rheumatoid nodules constitutional symptoms: fatigue, anorexia, weight loss, generalized wekness DIPs and lower back joints are not involved signs: radial deviation of wrist with ulnar deviations of digits Boutonniere and Swan-neck deformities nodules are usually on olecranon, occiput or Achilles tendon Felty syndrome (RA, splenomegaly, neutropenia) Caplan syndrome (RA, pneumoconiosis) |
|
|
rheumatoid arthritis management
|
aspirin
celecoxib (other COX-2 recalled due to increased risk of cardiac ischemia and stroke) glucocorticoids disease modifying agents: hydroxychloroquine gold salts methotrexate TNF inhibitors (infliximab, adalimumab, ethanercept) |
|
|
rheumatoid arthritis complications
|
alantoaxial subluxation
pannus formation at C1-C2 with neurologic symptoms (paraplegia, paresthesias of hands and feet, myelopathy) cervical x-ray is initial screening test rupture of Baker cyst manifests with swollen painful calf |
|
|
systemic lupus erythematosus presentation and diagnosis
|
four diagnostic criteria are needed:
malar rash discoid rash photosensitivity oral ulcers arthritis serositis renal involvement neurologic disorder hematologic disorder (hemolytic anemia, leukopenia, thrombocytopenia) immunologic disorder (anti-ds DNA, anti-SM) best screening test: ANAs anti-ds-DNA and anti-SM are specific for SLE |
|
|
systemic lupus erythematosus management
|
symptomatic
NSAIDs for arthritis corticosteroids for rashes cytotoxics (azathiorpine, cyclophosphamide) for severe synptoms (nephritis, endocarditis, pleuritis, hemolytic anemia, CNS) also wear sunglasses and sunscreen |
|
|
drug-induced lupus
|
reactions to hydralazine, isoniazid, procainamide and quinidine
presents with fever, arthritis, fatigue and rarely plurisy severe symptoms of lupus are not seen including skin disease and photosensitivity anti-histone antibodies are present in hydralazine-induced lupus only 1/3 have anti-histone antibodies present manage by withdrawing causing drug which confirms diagnosis when symptoms subside within 2 weeks |
|
|
diffuse scleroderma presentation
|
raynaud phenomenon
skin thickening throughout the body esophageal dysmotility achalasia intestinal hypomotility malabsorption large intestine diverticula lung fibrosis malignant hypertension acute renal failure Scl-70 antibodies are present |
|
|
limited scleroderma presentation
|
CREST syndrome: calcinosis, raynaud, esophageal dysmotility, sclerodactily, telangiectasia
skin involvment is in distal extremities pulmonary artery hypertension in 25-50% interstitial lung disease in 10% anticentromere antibodies are present |
|
|
scleroderma management
|
d-penicillamine for skin; CCB for raynaud; ACEIs for hypertension
"sCleroDermA" Calcium, D-penicilamine, ACEIs |
|
|
Sjogren syndrome
|
lymphocytic infiltration of exocrine glands seen alone or in association with RA, PBC, SLE
presents with itchy eyes with sandy feeling (keratoconjunctivitis sicca) and difficulty swallowing food, parotid enlargement and dental caries advanced stages affects lungs and kidneys and predisposes to malignant lymphoma screen with anti-Ro/La antibodies confirm with biopsy of salivary glands |
|
|
diseases associated with symmetrical polyarthritis
|
RA (involves mostly the joints), SLE, scleroderma, Sjogren
also parvoB19 and hepB |
|
|
seropositive arthropathies
|
RA, SLE, scleroderma, Sjogren
|
|
|
seronegative arthropathies
|
associated with HLA-B27 allele; ankylosing spondylitis, reactive arthritis, psoriatic arthritis, enteropathic arthropathy; PAIR
|
|
|
ankylosing spondylitis
|
3-4 times more common in men; 90% HLA-B27+
presentation --> chronic back pain and morning stiffness lasting >1h improves with exercise, decreased spine mobility, no lumbar lordosis anterior uveitis, aortic insufficiency and 3rd degree heart block X-rays show fusing of sacroiliac joint, sacroilitis, bamboo spine diagnose with clinical and x-ray, no HLA-B27 treat with NSAIDs, physical therapy, exercise and possibly TNF inhibitors "BEHNkylosing spondylitis needs x-ray" |
|
|
reactive arthritis
|
Reiter: nongonococcal urethritis (chlamydia, ureaplasma) with mucocutaneous manifestations (keratoderma blenorrhagica, circinate balanitis, genital ulcers, conjunctivits, arthritis)
ReA: after infectious diarrhea from campylobacter, shigella, salmonella diagnosis is clinical with x-ray findings of seronegative arthropathy |
|
|
osteoarthritis etiology
|
idiopathic (most common)
or secondary due to: gout, diabetes, acromegaly, hemochromatosis, mechanical factors |
|
|
osteoarthritis presentation
|
affects elderly with chronic asymetrical pain of weight bearing joints or PIPs, DIPs, which increases with excersise and decreases with rest
morning stiffness <30m crepitation no systemic nor inflammatory symptoms |
|
|
osteoarthritis diagnosis
|
clinical presentation + x-ray findings:
osteophytes and unequeal joint space osteophytes in PIPs are Bouchard nodules in DIPs are Heberden's nodules |
|
|
osteoarthritis management
|
reduce joint load, physiotherapy
NSAIDs specially acetaminophen (4,000mg/d, 1st line) ibuprofen (1,200mg/d) celecoxib used for patients with gastric side effects capsaicin cream depletes local nerves of substance P intraarticular hyaluronic acid injections are used also if no improvement or decreased quality of life then joint arthroplasty |
|
|
gout presentation
|
acute monoarthritis afecting first MTP (podagra) or other joints
signs of inflammation over joint precipitated by alcohol, trauma, surgery, steroid withdrawal and drugs (HCTZ, furosemide, pyrazinamide, ethambutol) chronic gout may involve monosodium urate deposition in connective tissue and kidneys |
|
|
gout diagnosis
|
clinical signs
erosive calcifications on x-ray negatively birefringent needle-shaped monosodium urate crystal in synovial fluid 5,000-50,0000 WBCs first step in diagnosis: joint aspiration |
|
|
acute gout management
|
indomethacin 50mg/8h
colchicine 0.6mg until symptoms resolve or GI upset if elderly with low NSAID toleration or renal impairment give steroids without NSAIDs or colchicine if previously using allopurinol, do not withdraw |
|
|
chronic gout management
|
low purine diet, limitation of alcohol and diuretics
if recurrent attacks: probenecid in undersecretors or allopurinol in undersecretors or overproducers or renal failure goal is to lower uric acid levels so monitor plasma uric acid |
|
|
pseudogout
|
same presentation as gout
diagnose with synovial fluid showing positively birefringent romboid calcium pyrophsphate crystals and condrocalcinosis in x-rays pseudogout raises suspicion of hyperparathyroidism, hemochromatosis, hypophsphatemia, hypomagnesemia management same as gout |
|
|
septic arthritis
|
due to gonococcus (young people) or staph (elderly) infection
presents with sudden onset monoarticular arthritis and signs of inflammation diagnose with arthrocentesis (gram stain, negative culture, no crystals and > 50,000 WBCs) treat with ceftriaxone (gonorrhea) or nafcillin/vancomycin (staph) |
|
|
Wegener granulomatosis
|
small vessel vasculitis
presents with rhinitis, sinusitis, nasal ulcers, hemoptysis, dyspnea, kidney involvement and arthritis cANCA+ diagnosis is made with biopsy of affected area treat with prednisone + cyclophosphamide |
|
|
polyarteritis nodosa
|
medium vessel vasculitis; presents with
nonspecific signs fever, malaise, anorexia, weight loss, abdominal pain does not affect lungs peripheral neuropathy (tingling, numbness, pain, mononeuritis) GI bleeds, 30% hepB kidney involvement diagnose with biopsy; can do angiogram |
|
|
Churg-Strauss syndrome
|
affects medium vessels
adult-onset asthma, eosinophilia, neuropathy and non-specific symptoms diagnose with biopsy treat with prednisone + cyclophosphamide |
|
|
temporal arteritis
|
affects large vessels of head and neck
headache, jaw claudication, visual disturbances 25% polymyalgia rheumatica first test is ESR, if high give prednisone then biopsy of temporal arteries looking for giant cells |
|
|
polymyositis/dermatomyositis
|
proximal muscle weakness without eye muscle compromise (different than myasthenia and EDS)
dermatomyositis has heliotrope rash over face and eyelids screening: aldolase and CPK; anti-Jo-1 diagnose with electromyography (short-duration, low amplitude potentials) confirm with muscle biopsy treat with steroids |
|
|
spinal cord compression etiology
|
acute --> trauma, hematoma
subacute --> cancer (lymphoma, multiple myeloma, prostate, lung, breast, kidney, colon), epidural abscess chronic --> herniated disk |
|
|
spinal cord compression presentation
|
back pain (96%)
history of cancer, fever bowel or bladder dysfunction insidious onset of mild sensory disturbance lower limb weakness or rigidity |
|
|
spinal cord compression diagnosis
|
plain x-rays are 84-94% sensitive
gold standard is MRI if MRI is contraindicated --> CT myelogram |
|
|
spinal cord compression management
|
high-dose dexamethasone immediately upon suspicion
surgical decompression in trauma, herniated disk or epidural abscess radiotherapy in case on cancer |
|
|
syringomyelia etiology
|
central cavitation of spinal cord
communicating is associated with Arnold-Chiari non-communicating is associated with trauma or spinal cord tumors |
|
|
syringomyelia presentation
|
cervical and upper limb pain and temperature loss
may have lower motor neuron deficits in upper limbs and upper motor neuron deficits in lower limbs |
|
|
syringomyelia diagnosis and treatment
|
MRI is gold standard; surgery is unsatisfactory
|
|
|
subacute combined degeneration
|
B12 deficiency results in
corticospinal --> upper motor neuron signs, flaccid/spastic paralysis dorsal columns --> ataxia, vibration and propioception deficits, distal paresthesia diagnosis --> low serum B12 and high methylmalonic acid treatment --> B12 replacement |
|
|
anterior spinal artery occlusion
|
bilateral paralysis
pain, temperature and autonomic loss below lession conserved vibration and propioception |
|
|
Brown-Sequard syndrome
|
ipsilateral upper motor neuron signs below lesion
ipsilateral vibration and propioception loss below lesion contralateral pain/temerature loss 1-2 levels below lesion bilateral flaccid paralysis and anesthesia at level of lesion ipsilateral Horner syndrome if above T1 |
|
|
anterior cerebral artery irrigation
|
medial surface of frontal and parietal lobes
1 inch of supero-lateral surface of frontal and parietal lobes anterior limb of internal capsule caudate nucleus anterior 4/5 of corpus callosum |
|
|
anterior cerebral artery stroke presentation
|
contralateral lower limb paralysis
contralateral lower limb sensory loss urinary incontinece, behavioral disturbances |
|
|
middle cerebral artery irrigation
|
lateral surfaces of frontal, parietal and temporal lobes except superior inch
genu and posterior limb of internal capsule globus pallidus putamen |
|
|
middle cerebral artery stroke presentation
|
contralateral hemiplegia, contralateral anesthesia
contralateral homonymous hemianopia with eye deviation toward lesion contralateral central facial paralysis aphasia if left, apraxia and spacial disturbance if right |
|
|
posterior cerebral artery irrigation
|
cerebellum, brain stem, pons, occipital lobe
|
|
|
posterior brain circulation arteries
|
posterior cerebral artery
basilar artery cerebellar arteries paramedian branches vertebral artery |
|
|
posterior cerebral artery stroke
|
contralateral homonymous hemianopia
visual hallucinations agnosia associated Weber or Benedikt syndromes |
|
|
Weber syndrome
|
results from occlusion of penetrating branches of PCA
contralateral hemiplegia and CNIII palsy |
|
|
Benedikt syndrome
|
results from occlusion of penetrating branches of PCA
CNIII palsy with contralateral ataxia or athetosis |
|
|
paramedian branches of basilar artery stroke
|
quadriparesis with intact vertical eye movement
|
|
|
PICA stroke
|
Wallenberg / lateral medullary syndrome -->
lateral spinothalamic --> contralateral pain/temperature loss trigeminal nucleus --> ipsilateral facial sensory loss vesticular nucleus --> vertigo, nystagmus, nausea ambigus nucleus --> dysarthria, dysphagia, gag reflex inferior cerebellar peduncle --> ataxia descending sympathetics --> Horner syndrome |
|
|
Wallenberg syndrome
|
results from posterior cerebellar artery occlusion
lateral spinothalamic --> contralateral pain/temperature loss trigeminal nucleus --> ipsilateral facial sensory loss vesticular nucleus --> vertigo, nystagmus, nausea ambigus nucleus --> dysarthria, dysphagia, gag reflex inferior cerebellar peduncle --> ataxia descending sympathetics --> Horner syndrome |
|
|
cerebellar artery stroke
|
vertigo
vomitting nystagmus ipsilateral limb ataxia |
|
|
stroke diagnosis
|
initial test is noncontrast CT to diffeentiate between ischemic or hemorrhagic
CT will be normal in ischemic stroke in first 48 hours if ischemic --> check for embolic sources with echocardiogram, carotid duplex, 24-hour Holter and check for hypercoagulability if hemorrhagic --> do EKG for inverted T-waves |
|
|
tPA use in ischemic stroke
|
use if onset <3 hours in ischemic stroke
contraindications --> history of intracranial hemorrhage stroke or head trauma within 3 months hemorrhage within 3 weeks surgery within 2 weeks arterial puncture within 1 week lumbar puncture within 1 week BP > 185/110 anticoagulants thrombocytopenia PT > 15s |
|
|
stroke treatment
|
ischemic --> tPA if onset <3h; then aspirin +- dypiridamole OR clopidogrel +- endarterectomy
hemorrhagic --> nimodipine +- craniotomy or coiling or shunt |
|
|
seizures/epilepsy etiology
|
"VITAMINS" -->
Vascular (stroke, bleed, AVM) Infections (meningitis, encephalitis) Trauma Autoimmune Metabolic (hyponatremia, hypocalcemia, hypoglycemia, hypoxia, drug overdose) Idiopathic Neoplasm pSychiatric |
|
|
seizures/epilepsy general presentation
|
sudden onset of convulsions with or without aura
postictal symptoms --> disorientation, sleepiness, aching muscles associated signs --> incontinence, tongue biting, headache patients with syncope don’t have postictal symptoms or signs |
|
|
partial simple seizure
|
focal deficits without loss of consciousness
|
|
|
partial complex seizure
|
focal deficits with loss of consciousness
|
|
|
partial seizure with secondary generalization
|
begins as partial and converts to generalized
|
|
|
generalized tonic-clonic seizure
|
tonic contractions followed by clonic relaxation of muscles
first line --> valproic second line --> phenytoin, carbamazepine, lamotrigine |
|
|
absence seizures
|
sudden brief loss of consiousness without loss of postural tone
treat with ethusuximide or valproic |
|
|
atonic seizures
|
sudden loss of postural tone for 1-2 seconds
|
|
|
myoclonic seizures
|
sudden brief muscle contraction
|
|
|
status epilepticus
|
recurrent continuous seizures lasting at least 5-30min
|
|
|
epilepsy diagnosis
|
EEG is test of choice
abnormal EEG alone is not diagnostic (2-18% of population has abnormal EEG) first rule out reversible causes of seizures checking electrolytes, glucose, toxicology, arterial blood gases and structural lesions with CT or MRI |
|
|
acute management of seizures
|
1) secure ABCs
2) evaluate precipitating causes 3) medications in order: lorazepam/diazepam, phenytoin, phenobarbital, midazolam/propofol |
|
|
maintenance treatment of epilepsy
|
tonic-clonic --> valproic acid is first OR lamotrigine, carbamazepine, phenytoin
partial --> carbamazepine, phenytoin first OR lamotrigine, valproic second absence --> ethosuximide or valproic myoclonic and atonic --> valproic pregnant --> carbamazepine |
|
|
vertigo etiology
|
Meniere
labyrinthitis positional vertigo traumatic vertigo perilymphatic fistula cervical vertigo |
|
|
vertigo presentation
|
patient feels room is spinning without any real movement, nausea and vomitting
differentiate from presyncope which is described as lightheadedness and feeling of blackout vertigo is neurologic presyncope is cardiologic |
|
|
central vertigo Vs. peripheral vertigo
|
central --> gradual onset, absent tinnitus and hearing loss, diplopia, cortical blindness, dysarthria, weakness, vertical nystagmus
peripheral is contrary |
|
|
Meniere disease
|
endolymphatic pressure changes
peripheral episodic vertigo 1-8 hours common causes are syphillis and head trauma |
|
|
labyrinthitis
|
follows respiratory tract infection
peripheral vertigo lasts for several days |
|
|
benign paroxysmal positional vertigo
|
peripheral vertigo exacerbated by head movements lasts 10-60 seconds
|
|
|
central vertigo
|
due to cerebellar or brain tumor, bleed, bleed, drug toxicity or multiple sclerosis
|
|
|
vertigo treatment
|
peripheral --> symptomatic with meclizine or diazepam
Meniere --> low-salt diet and diuretics benign paroxysmal --> head maneuvers |
|
|
headache etiology
|
primary --> migraine (15% of population), cluster, tension
secondary --> hemorrhage, brain tumor, meningitis, temporal arteritis, glaucoma |
|
|
meningitis headache
|
accompanied with fever and nuchal rigidity
|
|
|
intracranial hemorrhage headache
|
associated with nuchal rigidity, sudden onset, severe and without fever
|
|
|
brain tumor headache
|
deep, dull, aching pain disturbs sleep
|
|
|
posterior brain fossa tumor headache
|
history of vomitting weeks before, or induced by coughing, lifting or bending
|
|
|
temporal arteritis headache
|
unilateral pounding, dull headache associated with visual disturbances, jaw claudication, weight loss, arthritis, increased ESR
|
|
|
migraine presentation
|
pain described as pulsatile, throbbing, unilateral, aggravated by movement
nausea and vomitting photophobia, phonophobia may have aura or not aura --> scintillating scotoma, flashes of light, motor, sensory or visual symptoms |
|
|
tension headahces presentation
|
tight, band-like, bilateral headaches
builds slowly, may persist for days and is not exacerbated by movement may have tightness of posterior neck muscles |
|
|
cluster headache presentation
|
excrutiating, unilateral, pulsatile, periorbital headache that begins without warning and peaks in intensity within 5 minutes; lasts 30 minutes to 3 hours, 1-3 times/day for a 4-8 week period; associated with rhinorrhea, reddening of the eye, lacrimation and nasal stuffness
|
|
|
headache diagnosis
|
clinical history and tests to exclude secondary causes
if severe, sudden onset of first time headache --> head CT |
|
|
acute management of migraines
|
mild --> NSAIDs
severe, first line --> triptans (contraindicated in heart disease) severe, 2nd line --> ergotamine + caffeine |
|
|
prophylaxis of migraines
|
first line --> propranolol, timolol, valproic acid, topiramate
second line --> verapamil, tricyclics, SSRIs |
|
|
treatment of tension headaches
|
relaxation + acetaminophen/NSAIDs +- muscle relaxant
|
|
|
treatment of cluster headaches
|
100% O2, prednisone and lithium
may use sumatriptan, ergotamine, verapamil |
|
|
pseudotumor cerebri etiology
|
8-10x more common in women
associated with obesity, COPD, Addison, oral contraceptives, tetracyclines, vit A toxicity |
|
|
pseudotumor cerebri presentation
|
headache, diplopia, abducens palsy, papilledema
CT/MRI are normal CSF is normal beyond increase in pressure |
|
|
pseudotumor cerebri treatment
|
weight loss
removing offending agent diuretics (acetazolamide, furosemide) prednisone may be useful as well as repeated lumbar punctures |
|
|
trigeminal neuralgia presentation
|
sudden, severe, sharp pain starts near mouth and progresses towards ear, eye or nostril and lasts few seconds; can be a manifestation of multiple sclerosis or posterior fossa tumors
|
|
|
trigeminal neuralgia treatment
|
carbamazepine
may also try phenytoin, baclofen or gabapentin |
|
|
Guillain-Barre syndrome presentation
|
progressive paralysis
arreflexia pain or tingling autonomic instability history of recent infection (campylobacter, herpes, CMV, EBV) lack of constitutional symptoms |
|
|
Guillain-Barre syndrome diagnosis
|
history + lumbar puncture looking for ↑proteins and normal cell count
(best initial test, 48 hours after onset) electromyography is most specific |
|
|
Guillain-Barre syndrome treatment
|
IV immunoglobulin or plasmapheresis are equally effective
glucocorticoids are not effective early respiratory support to prevent death |
|
|
What are the basic molecules used in serological classification of streptococcie?
(serological classification = using serum antibodies to identify similar and different types of bacteria) pg 281 |
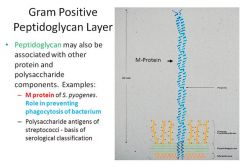
presence of POLYSACCHARIDE antigens associated with the gram POSITIVE peptidoglycan layer
|
|
|
myasthenia gravis diagnosis
|
best initial test --> acetylcholine receptor antibodies
most specific test --> electromyography (decrease in contraction on repetitive stimulation) edrophonium test is sensitive but not specific should do x-ray or CT to exclude thymoma |
|
|
Eaton-Lambert or botulism difference with myasthenia
|
Eaton-Lambert and botulism improve weakness with repetitive stimulation
myasthenia gets worse |
|
|
myasthenia gravis treatment
|
symptomatic relief --> pyridostigmine, neostigmine + plasmapheresis
thymectomy indicated in postbubertal and <60 with generalized myasthenia if thymectomy fails then steroids +- azathioprine mycophenolate is newer immunosuppressive avoid aminoglycosides |
|
|
amyotrophic lateral sclerosis presentation
|
upper motor neuron and lower motor neuron signs concomitantly is unique presentation
fasciculations, tongue atrophy, renervation after denervation on biopsy also nerve palsies (dysphagia, difficulty chewing, decreased gag reflex, etc) respiratory involvement with intact cognitive, sensory and autonomic function |
|
|
amyotrophic lateral sclerosis diagnosis
|
physical exam + electromyogram
CSF and MRI are normal |
|
|
amyotrophic lateral sclerosis management
|
riluzole slows progression
|
|
|
multiple sclerosis presentation
|
young female with relapsing remitting episodes of
weakness numbness tingling urinary urgency or retention blurry/double vision episodes resolve spontaneously |
|
|
multiple sclerosis diagnosis
|
clinical diagnosis + MRI of brain and spine
evoked potentials are rarely used CSF shows mild pleocytosis and mildly elevated proteins CSF for oligoclonal IgG banding is recommended when clinical suspicion remains after unconfirmatory MRI |
|
|
multiple sclerosis treatment
|
remitting relapsing disease --> interferon-B1a, interferon-B1b, glatiramer
secondary progressive disease --> interferon-B1b and mitoxanthrone (2nd-line) primary progressive disease --> no effective therapy acute exacerbations --> IV glucocorticoids spasticity --> baclofen trigeminal neuralgia --> carbamazepine bladder hyperactivity --> oxybutynin urinary retention --> bethanecol |
|
|
reversible causes of dementia
|
hypothyroidism
B12 deficiency hepatic encephalopathy CNS vasculitis syphilis brian abscess brain tumor anticholinergics apnea trauma subdural hematoma normal pressure hydrocephalus depression |
|
|
irreversible causes of dementia
|
Alzheimer (most common)
multifocal leukoencephalopathy Lewy bodies frontotemporal degeneration (Pick) vascular dementia Creutzfeld-Jakob |
|
|
dementia definition
|
memory loss along with impairment of other cognitive functions that interferes with social functioning
|
|
|
Alzheimer
|
memory loss + aphasia or apraxia or agnosia; inability to make plans and execute them
|
|
|
Pick disease
|
personality changes precede memory loss; patient lacks insight into condition
|
|
|
dementia with Lewy bodies
|
fluctuating cognitive impairment
|
|
|
Creutzfeld-Jakob
|
short, aggressive progression of dementia, myoclonus, ataxia and 14-3-3 protein in CSF
|
|
|
multi-infarct dementia
|
stepwise progression associated with discrete cerebrovascular events
|
|
|
Binswanger
|
slowly progressive vascular dementia that affects subcortical white matter
|
|
|
normal pressure hydrocephalus dementia
|
associated with gait abnormalities early in the course and urinary incontinence
|
|
|
dementia diagnosis
|
assesment of cognitive impairment with mini mental exam
CBC, electrolytes, calcium, creatinine, liver function tests, glucose, TSH, B12, RPR, HIV brain imaging in cases of focal deficits, seizures, gait abnormalities |
|
|
Alzheimer treatment
|
anticholinestrase inhibitors donepezil, rivastigmine, galantamine improve cognitive function
memantine is disease modifying used in advanced disease alone or in combo |
|
|
Huntington
|
chorea + behavioral disturbances (irritability, anger, paranoia, depression)
diagnosed with genetic testing for CAG triplet repeat expansion cerebral atrophy (cortex, basal ganglia) can be seen in brain imaging |
|
|
Parkinson etiology
|
structural lesions in basal ganglia
survivors of encephalitis neuroleptics (haloperidol, chlorpromazine) metoclopramide methyldopa reserpine |
|
|
Parkinson presentation
|
Bradykinesia
cogwheel Rigidity postural Instability resting Tremor "BRITish" |
|
|
Parkinson+ syndromes
|
parkinsonism + vertical gaze palsy --> supranuclear palsy
parkinsonism + ataxia --> olivopontocerebellar atrophy parkinsonism + orthostatic hypotension --> Shy-Drager syndrome |
|
|
diseases that mimic parkinsonism
|
severe depression
essential tremor normal pressure hydrocephalus Huntington |
|
|
Parkinson diagnosis
|
clinical diagnosis
|
|
|
Parkinson treatment with intact functional status
|
anticholinergics --> amantadine are first-line, then the rest
|
|
|
Parkinson treatment with compromised functional status
|
initial therapy is carbidopa/levodopa
if dyskinesia, akathisia or on-off --> add pramipexole, selegiline or COMT inhibitor (tolcapone) |
|
|
essential tremor
|
improves with alcohol; treat with propranolol
|
|
|
pemphigus vulgaris etiology
|
antibodies against desmosomes of epidermal cells; mostly idiopathic but also ACEIs and penicillamine
|
|
|
pemphigus vulgaris presentation
|
young patient with skin erosions and thin bullae that are painful
mouth erosions are prominent Nikolsky sign |
|
|
pemphigus vulgaris diagnosis
|
skin biopsy with immunofluorescence shows deposits of IgG and C3 in the epidermis
|
|
|
pemphigus vulgaris treatment
|
systemic glucocorticoids
if not effective --> azathioprine, mycophenolate or clyclophosphamide, rituximab, IVIG |
|
|
Nikolsky sign
|
removal of skin like a sheet with slight pressure
seen in pemphigus vulgaris, staph scalded syndrome, toxic epidermal necrolysis |
|
|
blistering diseases
|
pemphigus vulgaris
bullous pemphigoid pemphigus foliaceous porphyria cutanea tarda |
|
|
pemphigus foliaceous
|
more superficial than vulgaris with no oral lesions or intact bullae; same diagnosis and treatment as vulgaris
|
|
|
bullous pemphigoid presentation
|
autoantibodies against hemidesmosome at dermo-epidermal junction/basement membrane result in tense bullae that don't rupture easily in elderly; oral lesions are rare
|
|
|
bullous pemphigoid diagnosis and treatment
|
lesion biopsy with immunofluorescence shows depostis at basemanet membrane
systemic steroids alternative --> tetracycline or erythromycin combined with nicotinamide |
|
|
porphyria cutanea tarda etiology
|
deficiency of uroporphyrinogen decarboxulase results in accumulation of porphyrins and photosensitive reaction; there may be history of HIV, alcoholism, liver disease, chronic hepatitis C or oral contraceptives
|
|
|
porphyria cutanea tarda presentation
|
fragile, nonhealing blisters on sun-exposed areas with hyperpigmentation and hypertrichosis
|
|
|
porphyria cutanea tarda diagnosis
|
urinary uroporphyrins are elevated
|
|
|
porphyria cutanea tarda treatment
|
initial management is to stop alcohol and discontinue estrogens
barrier sun protection (not sunscreen) if insufficient --> phlebotomy, deferoxamine, chloroquine |
|
|
urticaria etiology
|
local skin anaphylaxis (IgE/mast cell mediated) without hypotension due to
drugs --> aspirin, NSAIDs, penicillins, morphine, codeine, quinolones foods --> peanuts, shellfish, tomatoes, strawberries insect bites and contact with latex |
|
|
urticaria presentation
|
acute --> wheals and hives and itching within 30 minutes last for <24h
chronic --> skin reactions last >6 weeks associated with pressure on skin, cold or vibration |
|
|
urticaria treatment
|
acute --> H1 antihistamines (diphenhydramine, cyproheptadine)
if life-threatening --> add H2 antihistamines + steroids chronic --> nonsedating antihistamines loratadine, desloratadine, fexofenadine, cetirizine most dangerous/avoid --> terfenadine, astemizole desensitization --> when trigger can't be avoided, beta blockers must be stopped before |
|
|
morbilliform rash
|
generalized maculo-papular rash that blanches with pressure (resembles measles), secondary to drug allergy; can appear days after exposure and after medication has been stopped; lymphocyt-mediated; treat antihistamines, steroids rarely necessary
|
|
|
hypersensitivity rashes
|
urticaria
morbilliform erythema nodosum erythema multiforme Stevens-Johnson toxic epidermal necrolysis fixed drug reaction |
|
|
erythema multiforme
|
most commonly due to herpes or mycoplasma infections
target-like lesions on palms and soles don't involve mucous membranes treat with antihistamines and underlying infection |
|
|
Stevens-Johnson
|
<10-15% of body surface area with mucous membrane involvement in 90% of cases
treat with early admission to burn unit and if needed, mechanical ventilation |
|
|
toxic epidermal necrolysis
|
involves 30-100% of body surface area; Nikolsky sign is present; clinical diagnosis; spesis is common cause of death but antibiotics are not used prophylactically; steroids not effective
|
|
|
fixed drug reaction
|
localized allergy to drugs; round, shaprly demarcated lesions that leave hyperpigmented spot after they resolve; treat with topical steroids
|
|
|
erythema nodosum etiology
|
localized skin reaction secondary to infections or inflammation
strep, coccidioides, histoplasma, syphilis, hepatitis Crohn, UC, sarcoidosis |
|
|
erythema nodosum presentation, diagnosis and treatment
|
multiple painful red raised nodules on anterior surface of lower limbs that do not ulcerate
ASO titers in case of strep treat underlying disease and give NSAIDs and analgesics |
|
|
tinea presentation
|
corporis: papulosquamous lesions with riased border in the body; pedis: macerated and scaling borders; unguium: thickened nails; capitis: small scaly semibold graysish patched on head; cruris: ringed lesions on crural folds and inner thighs; barbae: on face
|
|
|
tinea diagnosis and treatment
|
potassium hydroxide preparation
culture as definitive test capitis, corporis, unguium --> treat with oral terbinafine or itraconazole cruris, pedis, mild corporis --> topical clotrimazole/ketoconazole |
|
|
oral and IV anti-staph drugs
|
oral --> dicloxacillin, cefadroxil (preferred); IV --> cefazolin (preferred), oxacillin, nafcillin
|
|
|
impetigo
|
most commonly by staph or also by strep; affects only epidermis; lesions have purulent drainning material; treat with topical antibiotics (muciprocin, retapamulin) or oral if not effective (dicloxacillin, cephalexin)
|
|
|
erysipelas
|
most commonly by group A strep
involves dermis and epidermis with bright red swollen lesion, fever, chills and bacteremia treat with oral or IV penicillins or cephalosporins |
|
|
cellulitis
|
affects dermis and subcutaneous tissue; redness, swelling, warmth, tenderness without drainning lesions; treat with dicloxacillin or cefadroxil or if hypotension/sepsis --> IV oxacillin, nafcillin or cefazolin
|
|
|
folliculitis, furuncles, carbuncles
|
different stages of severity; carbucles are several confluent furuncles
furuncles and carbuncles are extremely tender treat with systemic antistaph drugs and surgical drainage of carbuncles |
|
|
necrotizing fascitis
|
by strep and clostridium
very high fever, portal of entry into skin, pain out of proportion, bullae and palpable crepitus diagnose with elevated CPK and image that shows air in the tissue and necrosis best initial step is surgery, then antistaph drugs |
|
|
toxic shock syndrome presentation and diagnosis
|
3 or more:
fever >102 systolic pressure <90 desquamative rash vomitting involvement of mucous membranes hyperbilirubinemia theombocytopenia there can also be increased CPK and liver enzymes, confusion and hypocalcemia |
|
|
toxic shock syndrome treatment
|
fluid resuscitation + dopamine
empiric --> clindamycin + vancomycin specific depending on methicillin resistance |
|
|
staph scalded skin syndrome
|
from staph toxin; Nikolsky sign is present; normal blood pressure and no involvement of viscera; treat with antistaph IV drugs
|
|
|
anthrax
|
woolsorters and bioterrorism
papule that becomes inflamed and develops central necrosis confirm with Gram and culture treat with penicillin V or doxycycline if terrorism treat with criprofloxacin |
|
|
seborrheic keratosis
|
hyperpigmented lesions with stuck-on appearance on face, shoulders, chest and back of elderly; no malignant potential; removed for cosmetic issues with liquid nitrogen or curettage
|
|
|
actinic keratosis
|
asymptomatic lesions on sun-exposed areas of elderly can progress to SCC
treat with sunscreen and remove with cryotherapy, 5FU, imiquimod, topical retinoic acid, curettage |
|
|
melanoma
|
malignant lesions grow in size, have irregular borders, uneven shape and incosistent coloring; full-thickness sample for biopsy; treat with excision
|
|
|
squamous cell carcinoma of skin
|
develops on sun-exposed areas of elderly
ulceration is common metastases rare diagnose with biopsy treat with surgery |
|
|
basal cell carcinoma
|
most common skin cancer
shiny or pearly lesion rare metastases diagnosis --> excisional biopsy treatment --> surgery |
|
|
kaposi sarcoma
|
purplish lesions on skin of HIV patients caused by HHV-8; treat with antiretrovirals; if CD4 doesn’t raise --> doxorubicin or vinblastine
|
|
|
psoriasis presentation
|
silvery scales on extensor surfaces, local or extensive, nail pitting, lesions with epidermal injury
|
|
|
psoriasis treatment
|
salicylic acid to remove scaly material
if localized --> topical steroids severe diseases --> add coal long-term --> calcipotriene (vitD) and tazarotene (vit A) if large area --> UV light if extensive and severe --> methotrexate new agents --> alefacept, efalizumab, etanercept, infliximab all patients should use emollients |
|
|
atopic dermatitis presentation
|
allergy with high levels of IgE result in extremely pruritic, red, plaques on flexor surfaces
children may have it on cheeks and scalp adults may have lichenification |
|
|
atopic dermatitis treatment
|
preventive --> moist skin, emollients, avoid drying sopas, cotton clothes
active diseae --> topical steroids, antihistamines, coal and phototherapy tacrolimus and pimecrolimus to decrease steroid use itching --> doxepin |
|
|
seborrheic dermatitis
|
scaly, greasy, flaky skin on scalp and face due to sebaceous secretion and pytirosporum ovale; treat with topical hydrocortisone or shampoos (ketoconazole, zinc pyrithione)
|
|
|
stasis dermatitis
|
hemosiderin hyperpigmentation from lower limb venous incompetence
prevent progression with elevation of legs |
|
|
contact dermatitis
|
hypersensitivity to soap, detergents, latex, sunscreen, jewelry, nickel
linear streaked vesicles confirm diagnosis with patch testing treat with topical steroids and antihistamines |
|
|
pityriasis rosea
|
pruritic, erythematous, salmon colored lesions spare palms and soles
clinical diagnosis, VDRL is negative treat with topical steroids |
|
|
scaling diseases
|
psoriasis, atopic dermatitis, seborrheic dermatitis, stasis dermatitis, contact dermatitis, pityriasis rosea
|
|
|
decubitus pressure ulcers
|
chronic sores where bone is close to skin in immobilized patients; stage I --> nonblanchable lesion; stage II --> superficial epidermis, partial dermis; stage III --> full skin thickness ecept fascia; stage IV --> all the way to bone; never culture or drain unless in surgery room for debridement; relieve pressure and if truly infected use antibiotics
|
|
|
alopecia areata
|
autoimmune destruction of hair follicles; treat with localized steroid injections
|
|
|
telogen effluvium
|
hair loss in response to big stress such as cancer or malnutrition
|
|
|
acne presentation
|
propionibacterium acne causes closed comedones, open comedones, pustules and cysts
|
|
|
acne treatment
|
mild --> topical clyndamycin, erythromycin, benzoyl peroxide, topical retinoids
moderate --> benzoyl peroxide with retinoids (tazarotene, tretinoin, adapalene) severe --> systemic tetracyclines and isotretinoin |
|
|
normal PA chest x-ray quality
|
1) centralized --> trachea and spinous apophysis are midway between clavicles 2) fully inhaled --> at least 10 ribs 3) exposure --> can see verterbra behind heart
|
|
|
x-ray for pneumothorax
|
should be expiratory looking for small lung fields and air in pleural space
|
|
|
anterior mediastinal masses on x-ray
|
seen on lateral view
thymus, thyroid, lymph nodes, teratoma |
|
|
posterior mediastinal masses on x-ray
|
seen on lateral view; more likely a neurally derived tumor
|
|
|
detection of small pleural effusions on x-ray
|
blunting of costophrenic angle can start to show with 50mL on lateral chest x-ray; need 100mL for PA view
|
|
|
lateral chest x-ray hemidiaphragm
|
right hemidiaphragm crosses the heart
|
|
|
decubitus x-ray
|
with patient laying on his side; taken after PA or lateral film shows blunting of costophrenic angles; effusions will move with gravity, alveolar infiltrates do not
|
|
|
interstitial lung syndromes seen on x-ray
|
"**** FACED": Sarcoidosis, Histiocitosis, IPF, Tumor, Failure, Asbestosis, Collagen disorders, Environmental, Dust, Drugs; also pneumocystis, mycoplasma, viruses and chlamydia
|
|
|
emphysema x-ray
|
hyperinflation of lung fields, flattening of diaphragm, elongated heart, increased antero-posterior diameter (barrel chest)
|
|
|
pneumonia on x-ray
|
alveolar infiltrate makes lobes look whiter
silhouette sign --> border between affected lobe and denser surrounding area is obscured lower lobe --> silhouette over hemidiaphragms right-middle lobe --> obscures right heart border upper lobe --> will not pass major fissure interstitial pneumonia --> fine, lacy appearance in most lobes chronic lung fibrosis --> reticulo-nodular pattern and honeycombing due to membrane thickening |
|
|
congestive heart failure x-ray
|
cephalization --> apical blood vessels become prominent due to excess fluid; cardiomegaly, effusions and Kerley B-Lines
|
|
|
endotracheal tube chest x-ray
|
should be 1-2cm above carina
|
|
|
central venous line on chest x-ray
|
tip of catheter should be at junction of SVC and right atrium, where right mainstem bronchus is seen; not inside atrium
|
|
|
air under the diaphragm on x-ray
|
hyperlucidity seen over liver and spleen and under diaphragm in upright position
chest x-ray is initial test in perforation |
|
|
high res CT indications
|
to detect lung parenchymal changes
1) symptomatic patients with normal x-ray 2) detecting metastatis, solitary nodules, bullae, bronchiectasis, diffuse parenchymal disease 3) guide for biopsy type and site |
|
|
abodminal x-ray
|
used to detect obstruction such as voluvulus or Hirchsprung
|
|
|
uses of ultrasound
|
colelithiasis, nephrolithiasis (except retroperitoneal ureters), abdominal and pelvic masses, ascites, pregnancy, patients with contraindication of IV contrast agents, endoscopic ultrasound for pancreatic pathology
|
|
|
endoscopic retrograde cholangiopancreatography
|
catheter through sphicter of Oddi injects contrast materal
excellent for pancreatic strictures, stones and neoplastic masses can perform removal of stones, dilate strictures and perform biopsy |
|
|
barium studies
|
used for esophageal strictures, webs, Zenker
not as accurate as endoscopy for esophageal cancer (needs biopsy) not as accurate as manometry for achalasia or muscular disorders not as accurate as colonoscopy for colon |
|
|
capsule endoscopy
|
used specially to visualize jejunum and ileum; if upper or lower endoscopy don't reveal source of bleeding then capsule endoscopy
|
|
|
HIDA
|
nuclear scan to visualize gallbladder for chocystitis; abnormal/positive --> no viasualization of gallbladder; normal/negative --> visualizes gallbladder
|
|
|
pet scanning
|
detects malignant versus benign thoracic cancers (after CT) by absorption of fluorodeoxyglucose; to ***** cancer resection (if benign lung mass, more likely to be successful resection)
|
|
|
MRI
|
superior than CT for detection of stroke, cancer, multiple sclerosis, infection and visualize brainstem and cerebellum; stroke is visible in first 24 hours on MRI
|
|
|
CT scan
|
superior than MRI for detenction of blood so indicated for head trauma; to exclude hemorrhagic stroke if patient presents within 3 hours (to ***** use of thrombolytics); detection of subarachnoid hemorrhage
|
|
|
contrast CT
|
used to detect abscess and infection which shows ring-enhancing lesion due to extravasation of blood through blood-brain barrier
|
|
|
bone scans
|
x-ray is first test for trauma and fracture; if suspicion of esteomyelitis then do x-ray first looking for elevation of periosteum; if its negative and still suspicious then do MRI
|
|
|
nonproliferative diabetic retinopathy
|
dilation of veins, microaneurysms, retinal edema, retinal hemorrhages due to glycolyzation of endothelial lining
|
|
|
proliferative diabetic retinopahty
|
neovascularization and vitreous hemorrhages
|
|
|
diabetic retinopathy diagnosis
|
yearly screening eye exam by opthalmologist for diabetics; fluorescein stain identifies vessels that should undergo laser photocoagulation
|
|
|
diabetic retinopathy treatment
|
tight control of glucose, blood pressure and lipids
aspirin, clopidogrel and antiplatelet therapy doesn’t work |
|
|
retinal detachment etiology
|
spontaneous or trauma; predisposing factors: myopia, surgical extraction of cataracts, proliferative retinopathy, retinal vein occlusion, age-related macular degeneration
|
|
|
retinal detachment presentation
|
unilateral blurry vision without pain or redness, floaters and flashes in periphery vision
|
|
|
retinal detahcment diagnosis
|
opthalmologic exam
|
|
|
retinal detahcment treatment
|
lean head back
mechanical reatachment by photocoagulation, cryotherapy or injection of expansile gas into vitreal cavity if all fails then remove vitreous humor and surgically reatach to sclera |
|
|
age-related macular degeneration presentation
|
dry form --> slow progressive visual loss in elderly with presence of drunsen; wet --> rapid visual abnormalities due to abnormal growth of choroid vessels with subretinal exudative retinal detachment
|
|
|
age-related macular degeneration treatment
|
dry type --> no clear treatment; zinc and antioxidants may help
wet type --> laser photocoagulation and photodynamic therapy |
|
|
photodynamic therapy
|
verteporfin is injected IV which is a photosensitive agent then photoactivating laser is applied
|
|
|
central retinal artery occlusion presentation
|
sudden, painless unilateral loss of vision without redness
opthalmoscopy shows pale retina and cherry-red spot at fovea |
|
|
central retinal artery occlusion diagnosis
|
opthalmoscopic exam + carotid artery imaging
echocardiogram and evaluation of thrombophilia |
|
|
central retinal artery occlusion etiology
|
carotid artery embolic disease
temporal arteritis cardiac thrombi from myxoma diseases of thrombophilia |
|
|
central retinal artery occlusion treatment
|
similar to stroke or TIA
give O2 and occular masage acetazolamide and thrombolytics may be used |
|
|
central retinal vein occlusion
|
sudden, painless unilateral loss of vision without redness
funduscopy shows disk swelling, venous dilation, tortuosity and importantly retinal hemorrhages (difference with central retinal artery occlusion) no specific treatment |
|
|
glaucoma etiology
|
precipitated by anticholinergics such as ipratropium and tricyclics
|
|
|
open-angle glaucoma presentation and diagnosis
|
accounts for 90% of glaucoma
mostly asymptomatic cup-to-disk ratio >0.3 confirmed by elevation of intraocular pressure by tonometry |
|
|
open-angle glaucoma treatment
|
↓aqueous humor -->
betablockers (timolol, betaxolol, levobunolol) alpha agonists (apraclonidine, brimonidine) carbonic ahydrase inhibitors (dorzolamide, brinzolamide) ↑outflow --> prostaglandins (latanoprost, travoprost) and pilocarpine if medical treatment doesnt work --> laser trabeculoplasty, surgical trabeculectomy |
|
|
closed-angle glaucoma presentation
|
eye is red
painful hard to palpation fixed midpoint pupil clouded cornea diminished visual acuity |
|
|
closed-angle glaucoma treatment
|
opthalmologic emergency
IV azetazolamide, urea, osmotic diuretics pilocarpine to open canal of Schelmm betablockers to decrease production of aqueous humor if all fails --> laser trabeculoplasty |
|
|
cataracts
|
opacification of lens results in slow progressive blurry vision; diagnose with physical exam and slit lamp; treatment is surgical removal of lens with intraocular lens placement
|
|
|
conjunctivitis
|
bacterial --> unilateral red eye with discharge and little itching
treat with topical erythromycin, sulfacetamide, fluoroquinolones viral --> more often bilateral, red eyes with severe itching symptomatic treatment |
|
|
subconjunctival hemorrahge
|
most commonly due to trauma
hematoma stops at limbus without intraocular or intravitreal damage no impairment of vision no specific therapy |
|
|
herpes simplex keratitis
|
severe pain in the eye
dendritic pattern over cornea on fluorescein stain therapy is oral acyclovir, famicyclovir, valacyclovir and topical trifluridin 1% |
|
|
periorbital cellulitis
|
by staph or strep invading dermis surrounding the eye
treat with antistaph penicillins or first-gen ceph if allergy |
|
|
uveitis etiology
|
psoriasis, sarcoidosis, syphilis, Reiter, inflammatory bowel disease
|
|
|
uveitis presentation
|
unilateral painful red eye with marked photophobia
|
|
|
uveitis diagnosis and treatment
|
inflammation of iris, cilliary body and choroid is visible by slit lamp
keratic precipitates may be visible in cornea treat with topical or systemic steroids |
|
|
anemia generalities
|
presentation --> fatigue, tiredness, exercise intolerance, dyspnea, tachycardia, angina, palpitations, lightheadedness, confusion
Hct < 41% in men or 36% in women hemoglobin <13.5mg/dL in men or 12mg/dL in women MCV < 80 --> microcytic; MCV >100 --> macrocytic |
|
|
anemia general etiology
|
microcytic --> iron deficiency, thalassemia, sideroblastosis, lead poisoning
macrocytic --> folate or B12 deficiency, alcohol, liver disease, methotrexate, AZT, phenytoin normocytic --> sickle cell, paroxysmal nocturnal hemoglobinuria, hereditary spherocytosis, G6PDH deficiency, drug-induced AOCD can be micro or normocytic |
|
|
anemia general diagnosis
|
determine hematocrit and hemoglobin
if anemia --> MCV then iron levels, reticulocyte count, peripheral smear, RDW, Coombs, B12/folate levels or marrow biopsy depending on on the case |
|
|
anemia general treatment
|
packed red blood cells to maintain hematocrit > 25-30%
hematocrit rises 3 points for every unit of red blood cells |
|
|
iron deficiency anemia
|
general anemia symptoms plus brittle spoon-shaped nails, glossitis, pica
ferrtin<10ng/mL is highly specific but low sensitivity ↓serum iron, ↑TIBC, ↓MCV, ↓reticulocytes ferrous sulfate tablets or parenteral iron in some cases |
|
|
anemia of chronic disease
|
can't use storage iron of reticuloendothelial system with consequent excess
due to neoplasia, systemic inflammation or infection general symptoms of anemia normal or ↑ferritin, ↓serum iron and TIBC treat underlying disease iron or erythropoietin will not help except in renal failure or chemotherapy |
|
|
sideroblastic anemia
|
defect in Hb synthesis with trapped iron in mitochondria of RBCs
genetic --> ALA deficiency or defect in B6 metabolism acquired --> chloramphenicol, isoniazid, alcohol, lead poisoning can be associated with myelodysplastic syndromes and can progress to AML initial tests --> ↑ferritin, ↑serum iron, ↓TIBC confirmation --> marrow smear shows ringed sideroblasts in Prussian blue stain treatment --> remove causing agent, lead and iron chelators, B6 in some cases |
|
|
alpha thalassemia presentation
|
1 gene deletion is asymptomiaic
2-gene deletion presents with mild anemia (Hct 30-40%) and profound microcytosis 3-gene deletion presents with severe anemia (Hct 20-30%) and profound microcytosis 4-gene deletion patients die in utero |
|
|
alpha thalassemia diagnosis and treatment
|
anemia with profound microcytosis and target cells are clues
normal iron studies with microcytosis make diagnosis Hb electrophoresis determines type and has normal HbF and HbA2 with HbH in 3 or 4 gene deletion no specific treatment required |
|
|
beta thalassemia presentation
|
beta thalassemia minor --> mild anemia and profound microcytosis
beta thalassemia major --> profound anemia and microcytosis, symptoms start when HbF decreases 6 months after birth; growth failure, bone deformities, hepatosplenomegaly, jaundice beta thalassemia major requires monthly transfusions which lead to iron overload (managed with deferasirox), hemochromatosis, cirrhosis, CHF |
|
|
beta thalassemia diagnosis and treatment
|
anemia + microcytosis
electrophoresis shows increased HbA2 and HbF beta thalassemia major requires monthly transfusions and deferasirox for iron overload may do splenectomy or marrow transplant |
|
|
B12 deficiency etiology
|
atrophic gastritis, gastrectomy, Crohn, sprue, pancreatic insuficiency, D. latum
|
|
|
B12 deficiency presentation
|
anemia of varying severity and neurologic symptoms of any kind alone or in combination
may have glositis, diarrhea or abdominal pain |
|
|
B12 deficiency diagnosis and treatment
|
made by showing anemia and macrocytosis
anti-intrinsic factor antibodies in pernicious anemia hypersegmented neutrophils, macro-ovalocytes hypercellular marrow, pancytopenia ↑LDH, ↑billirubin, ↑iron may do Schilling test treat --> intramuscular B12 |
|
|
Folic acid deficiency
|
due to ↓intake (diet, alcoholics)
↑requirements (pregnancy) ↑loss (eczema, dialysis, phenytoin) general anemia presentation depending on severity diagnosis --> ↓Hb and ↓folic acid levels may show macro-ovalocytes, hypersegmented neutrophils |
|
|
sickle cell disease etiology
|
autosomal recessive substitution of valine for glutamic acid at sixth amino acid of beta globin chain; painful crisis can be spontaneous or precipitated by fever, acidosis, dehydration, infection and fever
|
|
|
sickle cell disease presentation
|
symptoms of anemia
chronic manifestations --> isothenuria, ulcerations of the skin of the legs, bilirubin gallstones, asceptic necrosis of femoral head, osteomyelitis, retinopathy, recurrent pneumococcus or Haemophilus infections, growth retardation, splenomegaly/splenectomy acute painful crisis --> back, rib, chest and leg pain acute chest syndrome --> indistiguishable from pneumonia, severe chest pain, fever leukocytosis, hypoxia, x-ray lung infiltrates, pripapism, blindness, MI, abortions |
|
|
sickle cell disease diagnosis
|
mild to moderate anemia plus normal MCV
sickle cells on peripheral smear high reticulocyte count ↑bilrubin, ↑LDH microhematuria leukocytosis electrophoresis is the most specific test also sickle cell prep test |
|
|
sickle cell disease management
|
acute pain crisis --> fluids, analgesics, oxygen
if fever/leukocytosis --> ceftriaxone or cefotaxime severe manifestations such as priapism and cardiac --> packed RBCs if hematocrit is low or exchange transfusion if high chronic management --> folic acid, pneumococcus and influenza vaccinations and hydroxyurea to decrease frequency of vaso-oclusive/pain crisis |
|
|
autoimmune/drug-induced hemolytic anemia etiology
|
IgG antibodies against RBC membrane with destruction mostly in spleen by macrophages
idiopathic or secondary to leukemias (CLL), lymphoma, viral infections collagen vascular diseases, lupus penicillins, cephs, sulfas, quinidine, methyldopa, procainamide, rifampin, thiazides |
|
|
autoimmune/drug-induced hemolytic anemia presentation
|
symptoms related to severity
sudden onset may have fever, syncope, CHF, hemoglobinuria, weakness, pallor, jaundice, dark urine |
|
|
autoimmune/drug-induced hemolytic anemia diagnosis and treatment
|
normocytic anemia, reticulocytosis, ↑LDH, ↓haptoglobin, ↑indirect bilirubin
Coombs test is specific mild disease does not require specific treatment steroids in more severe disease splenectomy if unresponsive |
|
|
cold agglutinin anemia etiology
|
IgM against RBC membrane in response to lymphoma, Waldenstrom, mycoplasma or mononucleosis, ulcerative colitis
RBCs destroyed in liver |
|
|
cold agglutinin anemia presentation
|
symptoms related to severity
cyanosis in nose, ears, fingers and toes weakness, pallor jaundice, dark urine |
|
|
cold agglutinin anemia diagnosis and treatment
|
normocytic anemia, reticulocytosis, ↑LDH, ↓haptoglobin, ↑indirect bilirubin, often spherocytes
Coombs test is specific mild disease does not require specific treatment steroids or splenectomy won't work managed by avoiding cold weather or with azathiorpine, cyclosporine, cyclophosphamide, rituximab (anti-CD20 Ab) |
|
|
hereditary spherocytosis etiology
|
autosomal dominant defect in spectrin of RBC membrane;
|
|
|
hereditary spherocytosis presentation
|
mild to moderate symptoms of anemia, spherocytes
splenomegaly and jaundice sometimes cholecystitis |
|
|
hereditary spherocytosis diagnosis and treatment
|
anemia, normal MCV, ↑LDH, ↑reticulocytes, ↑indirect bilirubin
spherocytes and negative Coombs test positive osmotic fragility test treat with folate or splenectomy |
|
|
paroxysmal nocturnal hemoglobinuria etiology
|
red cell membrane defect in phosphatidyl inositol glycan A leads to increased complement lysis and intravascular hemolysis
|
|
|
paroxysmal nocturnal hemoglobinuria presentation
|
symptoms of anemia acording to severity
hemoglobinuria (specially in morning urine) thrombosis (specially hepatic vein, Budd-Chiari) |
|
|
paroxysmal nocturnal hemoglobinuria diagnosis and treatment
|
↓DAF, hematuria
normal MCV, ↑LDH, ↑reticulocytes, ↑indirect bilirubin, ↓haptoglobin specific tests are sugar-water test and acidified hemolysis test treat with folate, corticosteroids and anticoagulation for thrombosis |
|
|
G6PDH deficiency
|
enzyme deficiency leads to ↓NADPH, ↓gluthathione peroxidase activity and ↑unmetabolized H2O2 which precipitates Hb (Heinz bodies)
precitpitated by infections, sulfa drugs, primiquine, quinidine, dapsone, nitrofurantoin presentation --> sudden-onset anemia symptoms, jaundice, dark urine normal MCV, ↑indirect bilirubin, ↑LDH, ↑reticulocytes, ↓haptoglobin, hemoglobinuria, Heinz bodies, bite cells definitive test is ↓G6PDH treat with hydrration |
|
|
aplastic anemia etiology
|
most common is idiopathic; radiation, benzene, NSAIDs, chloranphenicol, alcohol, alkylating agents; infections: hepatitis, HIV, CMV, EBV, ParvoB19;
|
|
|
aplastic anemia presentation
|
bleeding from thrombocytopenia
fatigue, anemia and may have infections from neutropenia may have history of using precipitating drugs |
|
|
aplastic anemia diagnosis and treatment
|
screening --> pancytopenia
confirm --> bone marrow biopsy showing absence of marrow cells, fat and no signs of cancer, infection or fibrosis in marrow treat --> bone marrow transplant; if not, antithymocyte globulin, cyclosporine and prednisone |
|
|
acute leukemia etiology
|
most have no apparent cause; associated with radiation, benzene, melphalan, etoposide, retroviruses, Down and Klinefelter, myelodysplasia and sideroblastic anemia
|
|
|
acute leukemia presentation
|
fatigue, anemia and bleeding from thrombocytopenia +- leukopenia or leukocytosis
ALL --> in children, hepatosplenomegaly, lymphadenopathy, bone pain AML --> DIC (promyelocytic M3), CNS meningitis-like (monocytic M4, M5) |
|
|
acute leukemia diagnosis
|
pancytopenia although leukocytes can be up, down or normal
leukemic blasts in peripheral blood bone marrow biopsy showing >20% blasts confirms diagnosis to differentiate --> AML --> Auer rods (specially M3), myeloperoxidase and esterase ALL --> CALLA and TdT specific types of leukemia are diagnosed with monoclonal antibodies |
|
|
acute leukemia treatment
|
AML --> AraC with danourubicin or idarubicin
ALL --> daunorubicin, vincristine and prednisone add all-trans-retinoic acid in promyelocytic leukemia remission is removal of 99.9% of leukemic cells and elimination of blasts in peripheral blood |
|
|
differential diagnosis for pancytopenia
|
marrow --> aplastic anemia, metastatic cancer to marrow, myelofibrosis
infectious --> parvirus, retrovirus auto-immune --> B12 deficiency, SLE, hypersplenism drugs --> chloramphenicol acute leukemia is only one that shows blasts in peripheral blood |
|
|
chronic myelogenous leukemia etiology
|
clonal disorder of myelocytes associated in 95%with translocation t(9,22) (Philadelphia chromosome) which produces an enzyme with tyrosine kinase activity
|
|
|
chronic myelogenous leukemia presentation
|
leukocytosis and sometimes thrombocytosis lead to
fatigue, night sweats, low-grade fever abdominal pain, splenomegaly, bone pain rare --> lymphadenopathy, infection or bleeding leukostasis has dyspnea, blurry vision, priapism, thrombosis, stroke |
|
|
chronic myelogenous leukemia diagnosis
|
leukocytosis (mostly neutrophils)
↓LAP (difference with leukemoid reaction) absent or very low blast count if leukocytosis and ↓LAP --> check for Philadelphia chromosome |
|
|
chronic myelogenous leukemia treatment
|
imatinib is an inhibitor of the tyrosine kinase produced by disease
90% hematologic response and 60-70% loose Philadephia chromosome if imatinib doesn’t work --> bone marrow transplant |
|
|
chronic lymphocytic leukemia presentation
|
older patients can be asymptomatic
0 --> lymphocytosis alone 1 --> lymphadenopathy 2 --> splenomegaly 3 --> anemia 4 --> thrombocytopenia infection and bleeding are unusual survival of stage 0-1 is 10-12 years survival of 3-4 is 1-2 years |
|
|
chronic lymphocytic leukemia diagnosis
|
suspected in older patient with leukocytosis (80-98% lymphocytes)
bone marrow biopsy confirms leukemic lymphocytes smudge cells on peripheral smear |
|
|
chronic lymphocytic leukemia treatment
|
stages 0-1, no specific treatment
symptomatic patients are given fludarabine (DOC) or chlorambucil prednisone for autoimmune hemolysis and thrombocytopenia pentostatin for relapses |
|
|
multiple myeloma presentation
|
bone pain (specially back, ribs), lytic lessions, osteoporoosis, pathologic fractures
hypercalcemia (polyuria, polydipsia, altered mental status) renal failure (Bence Jones light chains) infection with encapsulated bugs anemia |
|
|
multiple myeloma diagnosis
|
normo normo anemia, hypercalcemia, ↑BUN, ↑creatinine
lytic bone lessions on x-rays Bence Jones protein ↑serum microglobulin B2 (75%) electrophoresis with monoclonal IgG spikes cofirmation --> bone marrow biopsy showing >10%plasma cells confirms |
|
|
multiple myeloma treatment
|
younger patients --> transplant (pre-treat with thalidomide, dexamethasone)
older patients --> melphalon, prednisone, thalidomide treat hypercalcemia with loop diuretics |
|
|
monoclonal gammopathy of uncertain origin
|
overproduction of clonal immunoglobulin by plasma cells without systemic manifestations
patient is asymptomatic clue to diagnosis is elevated serum protein monoclonal Ig spike on protein electrophoresis no bone lessions, no anemia, no renal failure, no hypercalcemia no treatment necessary |
|
|
Hodgkin disease presentation
|
nontender lynmphadenopathy
cervical, supraclavicular or axillary nodes are most common B symptoms are drenching night sweats, 10% weight loss, fever |
|
|
Hodgkin disease diagnosis
|
first step --> excisional lymph node biopsy showing Reed-Sternberg cells
second step --> determine staging with CT if CT is unrevealing and radiotherapy is contemplated then do laparotomy also anemia, leukocytosis, eosinophillia, ↑LDH, ↑ESR (adverse prognosis) may be seen |
|
|
Hodgkin disease adverse prognostic factors
|
large mediastinal lymphadenopathy
age older than 40 B symptoms ↑ESR |
|
|
Hodgkin disease treatment
|
stage I and II --> radiotherapy
B symptoms or stage III or IV --> ABVD chemo (adriamycin, bleomycin, vinblastine, dacarbazine) has less side effects than MOPP chemo (meclorethamine, oncovin/vincristine, prednisone, procarbazine) potential side effects --> permanent sterility, cancer, leukemia, aplastic anemia, peripheral neuropathy |
|
|
non-Hodgkin lymphoma etiology
|
HIV, hepatitis C, EPV, HTLV-1, H. pylori
HIV and EPV are associated with Burkitt and high-grade high-stage lymphomas |
|
|
non-Hodgkin lymphoma presentation
|
nontender lymphadenopathy with rubbery consistency
B symptoms --> drenching night sweats, 10% weight loss, fever cervical/supraclavicular --> 10-20% more likley to involve extra-lymphatic sites |
|
|
non-Hodgkin lymphoma diagnosis
|
first test --> excisional lymph node biopsy which excludes Reed-Sternberg cells
staging --> CT; laparotomy is not needed may do marrow biopsy also anemia, leukocytosis, eosinophillia, ↑LDH, ↑ESR may be seen |
|
|
non-Hodgkin lymphoma treatment
|
stages I and II --> radiotherapy
B symptoms or stages II or III --> CHOP chemo (cyclophosphamide, hydroxy-adriamycin, oncovin/vincristine, prednisone) if CNS lymphoma give radiotherapy with CHOP treat relapse with bone marrow transplant |
|
|
Hodgkin and non-Hodgkin staging
|
stage I --> one lymphatic group or extra-lymphatic tissue
stage II --> two lymphatic groups or extra-lymphatic tissue on same side of diaphragm stage III --> lymph nodes on both side of diaphragm or extralymphatic involvement contiguous to primary site stage IV --> widespread lymph involvement or diffuse extra lymphatic sites |
|
|
idiopathic thrombocytopenic purpura
|
antibodies against platelets leads to destruction and bleeding
epistaxis, bruising, petechiae, echymoses hematuria, dysfunctional uterine bleeding, GI bleeding thrombocytopenia is found and splenomegaly is absent exclude HUS, TTP, DIC --> peripheral smear without schistocytes and normal creatinine exclude marrow thrombocytopenia --> marrow biopsy with normal megakaryocytes treat with prednisone or splenectomy if unresponsive |
|
|
von Willebrand disease etiology
|
autosomal dominant defect in factor VIII production results in inability of platelets to adhere to vascular endothelium; aggregation is normal
|
|
|
von Willedrand disease presentation
|
petechiae, echymoses, epistaxis, bruising
hematuria, dysfunctional uterine bleeding, GI bleeding increased with aspirin |
|
|
von Willebrand disease diagnosis
|
platelet count is normal, ↑PTT, ↑BT
↓factor VIII antigen (vWB factor) abormal ristocetin test |
|
|
von Willebrand disease treatment
|
desmopressin used in mild bleeding and before minor surgery
if moderate to severe symptoms give factor VIII avoid aspirin |
|
|
causes of prolonged PT only
|
inherited --> factor VII deficiency
acquired --> vitamin K deficiency, liver disease, warfarin |
|
|
causes of prolonged PTT only
|
inherited --> vWF, factors VIII, IX, XI or XII deficiencies
acquired --> heparin, antiphospholipid antibody |
|
|
causes of prolonged PT and PTT
|
inherited --> prothrombin, fibrinogen, factors V or X deficiencies
acquired --> liver disease, vitamin K deficiency, DIC, supratherapeutic heparin or warfarin, inhibitors (thrombin, prothrombin, fibrinogen, factor V or factor X) |
|
|
hemophilia etiology
|
x-linked recessive; manifests in males; females are carriers
|
|
|
hemophilia presentation
|
obvious by age 2, apparent at time of circumcision
mild deficiencies --> asymptomatic severe deficiencies (<5-10% activity) --> factor-type bleeding, hemarthrosis, hematoma, GI or urinary bleeding, bruising or CNS bleeding |
|
|
hemophilia diagnosis
|
prolonged PTT, normal PT
mixing study indicates deficiency when PTT corrects to normal in 50:50 mixture patient and control blood if it doesn't correct, factor inhibitor is cause, not deficiency specific factor VIII or IX levels are necessary for precise diagnosis |
|
|
hemophilia treatment
|
mild hemophilia A is treated with desmopressin
severe deficiencies treated with specific factor replacement desmopressin doesn't work in hemophilia B |
|
|
vitamin K deficiency
|
decreased factors 2, 7, 9, 10 due to dietary deficiency of vitamin K, malabsorption or antibiotics
presentation --> hemarthrosis, hematoma, GI or urinary bleeding evident as oozing at venapuncture sites PT and PTT are elevated diagnosis --> confirmed after vitamin K injection and PT/PTT correction treat severe bleeding with fresh frozen plasma and vitamin K infusion |
|
|
liver disease coagulopathy
|
decreased clotting factors except 8 and vWB
due to severe liver disease or cirrhosis presents with bleeding, elevation of PT and PTT clinically indistinguishable from vitamin K deficiency except that it doesn’t correct with infusion low platelets due to acompanying hypersplenism treat with fresh frozen plasma and management of liver condition |
|
|
disseminated intravascular coagulation etiology
|
idiopathic
sepsis pancreatitis promyelocytic leukemia rhabdomyoloysis adenocarcinomas heatstroke transfusion reactions burns trauma abruptio placenta amniotic fluid embolism snakebites |
|
|
disseminated intravascular coagulation presentation
|
factor-type and platelet-type bleeding at any site
hemolysis can lead to acute renal failure, jaundice, confusion |
|
|
disseminated intravascular coagulation diagnosis
|
↑PT/PTT
↓platelets ↓fibrinogen ↑fibrinogen split products and d-dimers schistocytes present in peripheral smear |
|
|
disseminated intravascular coagulation treatment
|
fresh frozen plasma and maybe platelet transfusions; correct underlying disorder
|
|
|
pulmonary function tests
|
spirometry (mechanical ventilation)
Dlco (gas exchange) methacholine challenge test (bronchial hyperreactivity) TLC |
|
|
restrictive pattern
|
FEV1/FVC > 80%
|
|
|
obstructive pattern
|
FEV1/FVC < 80%
seen in emphysema, chronic bronchitis, asthma, bronchiectasis |
|
|
↓DLco
|
if FEV1/FVC < 80% suggests emphysema
if FEV1/FVC > 80% suggests interstitial lung disease or mild left heart failure |
|
|
↑DLco
|
suggests hemorrhage such as in Goodpasture
|
|
|
methacholine test
|
bronchoprovocation in patients with cough or wheezing who have normal pulmonary function tests, for possible asthma
do basal and postprovocation spirometry postitive test if baseline FEV1 decreased >20% |
|
|
A-a gradient formula
|
150 - (1.25 x PaCO2) - PaO2 normal: 5-15mmHg; increases with age and all forms of hypoxemia except hypoventilation and high altitude
|
|
|
solitary pulmonary nodule
|
1/3 are malignant
first step in management is looking for previous image study if none available then consider if patient is high or low risk for cancer low risk nonsmoker <35 --> x-ray every 3 months for 2 years, if no growth stop follow-up high risk smoker >50 --> open-lung biopsy and removal due to cancer risk |
|
|
transudative pleural effusion
|
↓hydrostatic pressure or ↓oncotic pressure; usually bilateral and equal
low LDH and proteins in fluid and serum (200, 0.6, 0.5) need all three values for diagnosis, else exudate |
|
|
exudative pleural effusion
|
due to local process; usually unilateral; need further investigation; high LDH and proteins in fluid and serum (200, 0.6, 0.5); don't need all three values high to make diagnosis
|
|
|
transudative causes of pleural effusion
|
heart failure
nephrotic syndrome liver disease pulmonary embolism atelectasis |
|
|
exudative causes of pleural effusion
|
pneumonia
cancer (lung, breast or lymphoma) pulmonary embolism drug-induced pancreatitis TB RA SLE |
|
|
transudative pleural effusion with no apparent cause
|
consider pulmonary embolism which can be either transudative or exudative
|
|
|
indications of thoracocentesis
|
any new and unexplained pleural effusion --> rule out empyema
decubitus x-ray --> <1cm free-flowing fluid --> minimal risk if non-free fluid need ultrasound guidance |
|
|
malignant pleural effusions
|
due mostly to breast cancer, lung cancer and lymphoma
send thoracocentesis fluid for cytologic exam also |
|
|
hemorrhagic pleural effusion
|
seen in mesothelioma, metastatic lung or breast cancer, pulmonary embolism with infarction and trauma
|
|
|
lymphocytic-predominant pleural effusions
|
suggests TB due to tuberculin hypersensitivity
check ↑adenosine deaminase and postivie PCR for TB acid-fast and culture of fluid are only positive in 30% |
|
|
respiratory compromise and distress
|
presents with shortness of breath, dyspnea, tachypnea (>30) and associated symptoms such as agitation, confusion or ↓consciousness
|
|
|
evaluation of respiratory distress
|
ensure patent airway
focus on quickness of onset and associated symptoms most important lab test is arterial blood gases then B-natriuretic peptide and chest x-ray |
|
|
acute respiratory distress with fever, cough or sputum
|
suggests infectious etiology
|
|
|
acute respiratory distress without systemic symptoms
|
suggests airway obstruction, cardiac disease or thromboembolism
|
|
|
chronic respiratory distress
|
suggests interstitial lung disease or COPD
|
|
|
common lung physical exam findings
|
diffuse wheezing --> asthma
localized wheezing --> foreign object rales --> pneumonia, interstitial disease, heart failure dull percusion --> pneumonia or atelectasis normal exam --> pneumocystis jirovecci, central respiratory problems |
|
|
B-natriuretic peptide in acute dyspnea
|
elevation is sensitive for heart failure but can also be elevated in cor pulmonale and acute right ventricular failure (thromboembolism)
|
|
|
chest x-ray without parenchymal infiltrates in acute dyspnea
|
suggests thromboembolism
central respiratory depression neuromuscular disease upper airway obstruction |
|
|
chest x-ray hyperinflation in acute dyspnea
|
suggests asthma and COPD
|
|
|
chest x-ray with focal infiltrates in acute dyspnea
|
suggests bacterial, viral or fungal pneumonia, aspiration or pulmonary hemorrhage
|
|
|
chest x-ray with diffuse edema in acute dyspnea
|
suggests heart failure or ARDS
|
|
|
ICU indications in respiratory failure
|
persistent hypoxemia --> hospitalization
ICU indications --> need for mechanical ventilation close monitoring increasing oxygen demand continuous nursing |
|
|
indications for intubation and/or mechanical ventilation
|
respiratory acidosis and hypercapnia in asthmatic patient
upper airway injury (burns, laryngeal edema, trauma) neurologic airway depression (often with loss of gag and cough reflexes) |
|
|
respiratory distress in hospitalized patients
|
inpatient who develops dyspnea, tachypnea and/or hypoxemia should raise possiblity of pulmonary embolism or aspiration
|
|
|
types of asthma
|
intrinsic (50%) is secondary to nonimmunologic stimuli (infections, irritating inhalants, cold air and emotional); extrinsic (20%) due to allergens
|
|
|
asthma stimuli
|
infections (RSV, rhinovirus), drugs (aspirin/NSAIDs, coloring agents, betablockers), allergens, cold air, emotions
|
|
|
asthma presentation
|
tachypnea, tachycardia, diffuse wheezing, use of accesory muscles, diminished breath sounds, hyperresonance, intercostal retractions
|
|
|
asthma poor prognosis factors
|
fatigue
diaphoresis pulsus paradoxus inaudible breath sounds decreased wheezing cyanosis bradycardia |
|
|
asthma diagnosis
|
initial tests for acute attacks --> ↓PaCO2, ↑pH, normal or ↓PaO2
severe attack -->↓PaO2, ↑PaCO2, ↓pH chest x-ray to rule out infection as cause spirometry --> obstructive pattern that reverses with beta agonist (FEV1 reverses by 12%) methacholine test --> ↓FEV1/FVC of 20% |
|
|
acute asthma management
|
O2
metered inhaled beta agonists --> albuterol/salbutamol, terbutaline salmeterol is long-lasting for nocturnal variant catecholamines may be used but not routinely aminophylline and theophyline have modest potency and are not routine anticholinergics (ipratropium) if heart disease (slow onset, medium potency) |
|
|
chronic asthma management
|
acute exacerbations: systemic prednisone 10-14 days along with inhaled albuterol; inhaled corticosteroids are first line maintenance; cromolyn is first line maintenance in children and prophylaxis in adults; zileuton, zafirlukast, mmonteleukast for severe asthma resistant to maximum doses of inhaled steroids
|
|
|
mild asthma definition and treatment
|
symptoms ~2 days/week and rare night symptoms
FEV1 is normal no long-term control needed only inhaled beta agonists for attacks |
|
|
moderate asthma definition and treatment
|
symptoms on most days and at least 5 nights/month with FEV1 60-80%
treat with daily inhaled steroids (also cromolyn specially in children) maybe also salmeterol |
|
|
severe asthma definition and treatment
|
daily symptoms, frequent night symptoms and hospital emergencies with FEV1 <60%; daily inhaled steroids, daily inhaled salmeterol along with antileukotriene drug and possibly low-dose oral steroid
|
|
|
physical exam in emphysema
|
distant breath sounds
pink skin thin barrel chest accesory muscles symptoms of right heart failure and clubbing |
|
|
physical exam in chronic bronchitis
|
rhonchi and wheezes
signs of cyanosis weight gain symptoms of right heart failure and clubbing |
|
|
chest x-ray findings in COPD
|
chronic bronchitis --> increased pulmonary markings
emphysema --> bilateral hyperinflantion, diaphragm flattening, small heart size, increase in retrosternal space |
|
|
COPD diagnosis
|
↓FEV1/FVC
FEF 25-75 ↑RV and TLC emphysema has ↓DLco and chronic bronchitis has normal DLco FEV1/FVC after bronchodilation will stay the same |
|
|
COPD complications
|
hypoxemia with nocturnal desaturation
secondary erythrocytosis cor pulmonale chronic ventilatory failure CO2 retention |
|
|
maintenance treatment for COPD
|
first-line --> ipratropium via metered inhaler; inhaled beta agonists can be used concomitantly; inhaled corticosteroids are not used in COPD; if above fails --> theophylline (watch for cytochrome inhibitors and inducers)
|
|
|
only treatment that reduces mortality in COPD
|
home O2 supplementation and smoking cessation
home oxygen for hypoxemia (PaO2<55mmHg or saturation <88%) pneumococcal vaccine every 5 years, influenza vaccine yearly and haemophilus vaccine if unvaccinated |
|
|
COPD exacerbation general management
|
1) measure O2 saturation (pulse oximetry)
2) arterial blood gases 3) chest x-ray 4) check theophylline levels 5) CBC and ECG 6) hospital admission if significant hypercapnia or hypoxemia 7) consider intubation and mechanical ventilation 8) specific treament spirometry is NOT done or useful in exacerbation |
|
|
COPD exacerbation specific treatment
|
1) O2 supplementation
2) inhaled bronchodilators and anticholinergics concomitantly 3) IV or oral prednisone for 2 weeks 4) antibiotics despite normal x-ray 5) council on smoking cessation 6) teach optimal use of MDI no benefit in IV theophylline and avoid opiates and sedatives |
|
|
bronchiectasis etiology
|
secondary to recurrent pneumonias, TB, fungal or abscess
cystic fibrosis, immotile cilia syndrome (50% Kartagener) |
|
|
bronchiectasis presentation
|
suspect in anyone with
chronic cough foul-smelling sputum hemoptysis recurrent pulmonary infections sinusitis immune deficiencies presents with purulent copious sputum, wheezes, crackles and history of recurrent pneumonias (specially gram- and pseudomonas) |
|
|
bronchiectasis diagnosis
|
early chest x-ray may be normal or severe cases show 1-2cm cysts and crowding of bronchi; chest CT is best noninvasive test
|
|
|
bronchiectasis treatment
|
bronchodilators, chest physical therapy, postural drainage, rotating gram- antibiotics
surgery in cases of localized bronchiectasis or massive hemoptysis yearly influenza vaccine and pneumococcal vaccine with booster at 5 years |
|
|
bronchiectasis complications
|
massive hemoptysis, amyloidosis, cor pulmonale, visceral abscesses
|
|
|
interstitial lung disease general presentation
|
exertional dyspnea
nonproductive cough crackles pulmonary hypertension clubbing restrictive pattern |
|
|
interstitial lung diseases
|
idiopathic pulmonary fibrosis
sarcoidosis pneumoconiosis --> asbestosis, silicosis, coal pneumoconiosis |
|
|
idiopathic pulmonary fibrosis presentation
|
exercise intolerance, dyspnea, coarse crackles
|
|
|
idiopathic pulmonary fibrosis diagnosis
|
reticular or reticulonodular pattern on chest x-ray
restrictive pattern on PFTs increased macrophages on bronchoalveolar lavage (nonspecific) |
|
|
idiopathic pulmonary fibrosis treatment
|
steroids with or without azathioprine works in 20%; the rest develop fatal lung disease
|
|
|
idiopathic pulmonary fibrosis prognosis
|
20-40% 5-year survival; best prognostic factor is response to steroids as evidenced in PFTs
|
|
|
sarcoidosis presentation
|
"GRAIN"
gammaglubilinemia rheumatoid arthritis ACE increase interstitial fibrosis non-casseating granuloma hilar and left paratracheal adenopathy hypercalcemia due to vitamin activation by macrophages uveitis/conjunctivitis in >25% chest x-ray findings restrictive or normal PFTs |
|
|
chest x-ray findings in sarcoidosis
|
four stages found (not progressive)
bilateral hilar adenopathy hilar adenopathy with reticulonodular parenchyma reticulonodular parenchyma alone honeycombing of bilateral lung fields with fibrosis |
|
|
sarcoidosis diagnosis
|
biopsy of affected tissue showing noncasseating granulomas; all patients should have ophthalmologic exam
|
|
|
sarcoidosis prognosis
|
80% remain stable or spontaseoulsy resolves; 20% progress to organ compromise
|
|
|
sarcoidosis treatment
|
no treatment is effective
if organ compromise may use trial of high-dose steroids if uveitis, CNS involvement or hypercalcemia --> steroids are mandatory |
|
|
pneumoconiosis general presentation
|
dyspnea, shortness of breath, cough, sputum, cor pulmonale, clubbing, restrictive pattern, ↓DLco, hypoxemia with ↑A-a
|
|
|
ocupations associated with asbestosis
|
mining, milling, foundry work, shipyards, pipes, break linings, insulation, boilers; history of exposure necessary for Dx
|
|
|
asbestosis x-ray findings
|
diffuse or local pleural thickening, pleural plaques, calcifications near diaphragm, pleural effusions, lower lobe interstitial infiltrate
|
|
|
asbestosis associated cancers
|
lung adenocarcinoma or SCC
pleural mesothelioma is less common |
|
|
asbestosis diagnosis
|
history of exposure + lung biopsy showing barbell-shaped asbestos fibers
|
|
|
asbestosis treatment
|
no effective treatment; must stop smoking due 75x increased risk of cancer
|
|
|
ocupations associated with silicosis
|
mining, quarrying, tunneling, glass and pottery making, sandblasting
|
|
|
silicosis x-ray findings
|
1-10mm nodules throughout the lungs, most prominent in upper lobes
in progressive massive fibrosis nodules are >10mm and coalesce |
|
|
silicosis diagnosis
|
history of exposure + lung biopsy showing silica particles
pathologic lesion is the hyaline nodule |
|
|
silicosis treatment
|
no effective treatment; should have yearly PPD test and if >10mm --> INH prophylaxis for 9 months
|
|
|
Lofgren syndrome
|
acute sarcoidosis presentation with erythema nodosum, arthritis, hilar adenopathy
|
|
|
Heefordt-Waldenstrom syndrome
|
acute sarcoidosis presentation with fever, parotid enlargement, uveitis and facial palsy
|
|
|
Caplan syndrome
|
rheumatoid nodules in periphery of lung, rheumatoid arthritis and coesxisting pneumoconiosis (usually CWP)
|
|
|
coal worker's pneumoconiosis x-ray findings
|
small round parenchymal densities
usually in upper half of lungs progressive massive fibrosis has 1cm densities in whole lung |
|
|
coal worker's pneumoconiosis immunologic findings
|
↑IgA, ↑IgG, ↑C3, ANA and rheumatoid factor
|
|
|
pulmonary embolus site of origin
|
most are from above-the-knee deep veins which result from distal deep vein thrombosis; in patients with catheters it can originate from upper limb, subclavian and internal jugular veins
|
|
|
criteria for high-risk pulmonary embolism patients
|
recent surgery (specially orthopedic, knee replacement has 70% risk); cancer history (prostate, breast, pelvic, abdominal); immobilized patients; acquired thrombophilia (lupus anticoagulant, nephrotic syndrome); oral contraceptives; inherited thrombophilia (factor V Leiden, protein C/S deficiency, antithrombin III deficiency); pregnancy; need 1 risk factor and consistent signs and symptoms for high-risk label
|
|
|
signs and symptoms consistent with pulmonary embolism
|
sudden onset of dyspnea, tachypnea, thigh/calf swelling, pleuritic chest pain, hemoptysis, tachycardia, ↑P2
|
|
|
when to consider pulmonary embolism
|
all patients with dyspnea and normal chest x-ray
|
|
|
nonspecific routine tests for dyspnea; may suggest PE
|
arterial blood gases show hypoxemia with ↑A-a
chest x-ray (normal in PE) ECG (to exclude others) shows S1, Q3, T3, tachycardia |
|
|
specific tests for pulmonary embolism
|
best initial test is spiral CT scan; V/Q scan (if normal excludes PE); angiogram is gold standard
|
|
|
deep venous thrombosis specific tests
|
best intial test is compression or duplex ultrasound; venogram is rarely done; MRI
|
|
|
tests for DVT and PE
|
D-dimer is most sensitive; can only exclude thromboembolism if normal levels
may also be high in surgery, infection, trauma, pregnancy and DIC normal D-dimer and CT scan rule out thromboembolism in 98% of low-risk patients |
|
|
tests results that exclude pulmonary embolism
|
normal CT + normal D-dimer in low-risk patients
normal CT + normal doppler in low-risk patients V/Q scan is completely normal |
|
|
generalities of pulmonary embolism diagnosis
|
all patients should be on heparin during diagnosis and imaging; if PE is suspected start CT scan right after chest x-ray; if all tests are negative but it's high-risk patient --> angiogram; normal CT + normal D-dimer or doppler excludes PE in low-risk patients
|
|
|
pulmonary embolism treatment
|
1) O2
2) start heparin before confirmation and during work-up 3) concomitant warfarin 4) if hemodynamically unstable or massive PE --> thrombolytics (tPa, streptokinase) |
|
|
heparin considerations in pulmonary embolism
|
if LMWH then no need to follow PTT and less chance of heparin-induced thrombocytopenia
HIT is associated with more thrombotic events, not bleeding diathesis, and is treated with new anticoagulants (argatroban, lepirudin) start heparin immediately |
|
|
warfarin considerations in pulmonary embolism
|
monitor PT
titrate to INR of 2-3 skin necrosis can occur if protein C deficiency already present contraindicated in pregnancy (use LMWH 6 months instead) |
|
|
contraindications of anticoagulation therapy in PE
|
contraindicated in patients with recent neurosurgery or eye surgery; use inferior vena cava filter instead
|
|
|
post thrombotic syndrome
|
pain
edema hyperpigmentation skin ulceration in 2/3 of PE patients compression stockings can prevent it |
|
|
fat embolism
|
acute dyspnea, petechiae in neck or axilla, confusion, 3 days after long bone fracture or after CPR; no anticoagulation necessary
|
|
|
ARDS etiology
|
sepsis
trauma DIC Goodpasture SLE drug overdose toxin inhalation drowning |
|
|
ARDS presentation
|
dyspnea, tachypnea, diffuse rales and ronchi
|
|
|
ARDS diagnosis
|
chest x-ray --> diffuse interstitial or alveolar infiltrates
ABGs --> ↓PaO2, ↑PaCO2 Swan-Ganz --> normal cardiac output and capillary wedge pressure but ↑pulmonary artery pressure |
|
|
ARDS treatment
|
treat underlying cause; mechanical ventialtion with positive end-expiratory pressure
|
|
|
ARDS prognosis
|
70% mortality
|
|
|
sleep apnea
|
cessation of airflow >10s at least 10-15/hour of sleep + daytime somnolence
confirm with polysomnography treat obstructive with weight loss and nasal continuous positive airway pressure (CPAP) treat central with acetazolamide, progesterone and O2 |
|
|
lung cancer etiology
|
90% of cases are directly related to cigarette smoke; nonsmokers develop adenocarcinoma; all lung cancers are associated with smoking; active smokers have 10x greater risk; 40 pack-year history increases risk 60-70x; asbestos increases risk 75x
|
|
|
types of lung cancer
|
most common is adenocarcinoma (40%); squamous cell carcinoma, small cell and large cell
|
|
|
centrally located lung cancers
|
squamous cell and small cell
|
|
|
peripheral located lung cancers
|
adenocarcinoma and large cell
|
|
|
lung cancer paraneoplastic syndromes
|
SCC --> hypercalcemia (PTH-like peptide)
small cell --> SIADH and Eaton-Lambert |
|
|
lung cancer metastasis
|
SCC --> direct extension to hilar node and mediastinum
small cell and adenocarcinoma --> liver, adrenals, brain, bones |
|
|
lung cancer presentation
|
cough
weight loss dyspnea hemoptysis chest pain recurrent pneumonic processes hoarseness |
|
|
lung cancer diagnosis
|
sputum cytology (specially SCC)
bronchoscopy for centrally located lessions needle aspiration biopsy if highly suspicious and nonspecific bronchoscopy findings or peripheral lession |
|
|
symptoms of unresectable lung cancer
|
weight loss >10%
bone pain extrathoracic metastasis CNS symptoms SVC syndrome hoarseness contralateral mediastinal adenopathy |
|
|
lung cancer treatment
|
resectable small cell --> VP16 (etoposide, platinum); resectable non-small --> CAP (cyclo, adriamycin, platinum) and radio
|
|
|
lung cancer prognosis
|
5-8% 5-year survival
after resection of SCC --> 30-35% after resection of large-cell and adeno --> 25% |
|
|
atelectasis etiology
|
most common is postsurgery; also mucuous plug, foreign body or tumor
|
|
|
atelectasis presentation
|
tachycardia, dyspnea, fever, hypoxemia
|
|
|
atelectasis diagnosis
|
ipsilateral trachea deviation --> upper lobe
mediastinal deviation --> massive atelectasis elevation of hemidiaphragm --> lower lobe atelectatic lobe looks denser, consolidated and smaller than normal contralateral lobe |
|
|
basic life support measures
|
1) assess responsiveness
2) call for help 3) postiion face up on flat surface 4) open the airway 5) assess breathing (if no breathing, perform 2 rescue breaths) 6) check carotid pulse 5-10 seconds (if no pulse, give 30 compressions and two ventilations until help arrives) |
|
|
asystole and dysrhythmia etiology
|
"Hi 5, T5": hypoxia, hypo/hyperkalemia, hypothermia, hypoglycemia, hypoveolemia, trauma, toxins, tamponade, tension pneumothorax, thrombosis
|
|
|
advanced cardiac support
|
if pulseless + shockable --> shock + 5 cycles of CPR + 1mg epi every 3-5min until pulse present
if pulseless + not shockable --> 5 cycles of CPR + 1mg epi + 1mg atropine until electrical activity then check pulse; |
|
|
shockable rhythms
|
ventricular fibrillation and ventricular tachycardia
|
|
|
unshockable rhythms
|
asystole, pulseless electrical activity
|
|
|
signs of hemodynamic instability
|
hypotension, chest pain, altered mental status, CHF
|
|
|
general measures of tachycardia with pulses
|
ABC, O2, identify rhythm on ECG, identify reversible causes
|
|
|
hemodynamically unstable patient with pulse and tachycardia
|
perform immediate cardioversion
IV access and sedation until stable |
|
|
hemodynamically stable patient with pulse and tachycardia, narrow QRS, regular rhythm
|
vagal maneuvers or adenosine
if converts --> probable SVT, treat recurrence with adenosine if doesn’t convert --> probable atrial flutter, ectopic atrial tachycardia control rate with diltiazem or betablockers |
|
|
hemodynamically stable patient with pulse and tachycardia, narrow QRS, irregular rhythm
|
probable A-fib or MAT; control rate with diltiazem or betablockers
|
|
|
hemodynamically stable patient with pulse and tachycardia, wide QRS, regular rhythm
|
if VT --> amiodarone 150mg IV over 10min, repeat as needed
if SVT --> adenosine and check for rhythm conversion |
|
|
hemodynamically stable patient with pulse and tachycardia, wide QRS, irregular rhythm
|
if WPW --> avoid nodal blocking agents adenosine, digoxin, CCB
consider amiodarone 150mg over 10min |
|
|
basic algorhythm for tachycardia with pulses
|
general measures --> check if stable --> check QRS --> check rhtyhm regularity
|
|
|
miosis as sign of toxicity
|
sugests clonidine, barbiturates, opiates, cholinergics, pontine stroke
|
|
|
mydriasis as sign of toxicity
|
sugests sympathomimetics, anticholinergics
|
|
|
dry skin as sign of toxicity
|
sugests anticholinergics
|
|
|
wet skin as sign of toxicity
|
cholinergics, sympathomimetics
|
|
|
blisters as sign of toxicity
|
barbiturates, carbon monoxide
|
|
|
common signs of toxicity
|
miosis, mydriasis, dry skin, wet skin, blisters
|
|
|
measures for toxic ingestion management
|
induced vomiting
lavage charcoal whole bowel irrigation dialysis cathartics forced diuresis naloxone/dextrose/thiamine |
|
|
induced vomitting
|
ipecac can only be used 1-2 hours after toxic ingestion (limited use)
not indicated in children or for caustic substances |
|
|
lavage
|
indicated in those with mental status
preceded by intubation used 1 hour after ingestion (limited use) contraindicated for caustic substances |
|
|
charcoal
|
used if patient arrives more than 1-2 hours after ingestion; decreases absorption and increases removal of absorbed substance
|
|
|
whole bowel irrigation
|
used when many pills are seen on x-ray; 1-2 liters/hour of GoLytely via gastric tube
|
|
|
dialysis for toxicity management
|
used for ehtylene glycol, lithium overdose, methanol poisoning, aspirin overdose, theophyline overdose and there is coma, hypotension or apnea
|
|
|
cathartics
|
useful only when charcoal is used; generally wrong answer
|
|
|
forced diuresis
|
alkaline diuresis is only useful for salicylates and phenobarbital
|
|
|
naloxone/dextrose/thiamine administration
|
given to any patient who ingested substance and has altered mental status
|
|
|
acetaminophen toxicity stages
|
gastritis, nausea, vomitting 12-24 hours after ingestion; 24-48 hours: asymptomatic period with subclinical elevation of transaminases and bilirubin; 48-72 hours: jaundice, abdominal pain, hepatic encephalopathy, renal failure and death
|
|
|
acetaminophen toxicity treatment
|
N-acetyl-cysteine preferably within first 8 hours
activated charcoal no gastric emptying after 24 hours of ingestion no treatment can prevent or reverse toxicity |
|
|
methanol ingestion sources
|
paint thinner, sterno, photocopier fluid, solvents, windshield washer solution
|
|
|
ethylene glycol ingestion sources
|
car antifreeze
|
|
|
methanol and ethylene glycol metabolism
|
methanol + alcohol dehydrogenase --> formaldehyde + formic acid
ethylene glycol + alcohol dehydrogenase --> oxallic acid/oxalate |
|
|
general signs of alcohol intoxication
|
confusion, ataxia, lethargy, drowsiness, slurred speech
|
|
|
isopropyl alcohol intoxication
|
ketonuria, ketonemia, without acidosis and no increased anion gap
|
|
|
methanol intoxication specific signs
|
visual disturbances, blindness
|
|
|
ehtylene glycol intoxication specific signs
|
renal failure and oxalate crystals/stones in urine
|
|
|
alcohol intoxication diagnosis
|
determine specific alcohol levels in blood
oxalate crystals in urine and ↑BUN/creatinine are characteristic of ethylene glycol ethylene glycol and methanol produce increased anion gap metabolic aciosis different from isopropyl alcohol which is normal |
|
|
alcohol intoxication treatment
|
fomepizole is alcohol dehydrogenase inhibitor which decreases toxic metabolites
|
|
|
carbon monoxide poisoning presentation
|
dyspnea, tachypnea, shortness of breath, headache, nausea, dizziness, confusion, syncope, chest pain, arrhythmia, hypotension
|
|
|
carbon monoxide poisoning diagnosis
|
carboxyhemoglobin levels
arterial blood gases (metabolic acidosis with normal PO2) ↑CPK pulse oximetry not helpful CO poisoning might present similar to hypoglycemia, if glucose is normal, raise suspicion of CO |
|
|
carbon monoxide poisoning treatment
|
removal from source of exposure, 100% O2, hyperbaric O2 if CNS or chest pain
|
|
|
caustic substance intoxication presentation
|
oral pain, drooling, odynophagia, abdominal pain
esophageal injury and gastric perforation may occur |
|
|
caustic substance intoxication diagnosis
|
by history of exposure and upper endoscopy if ingested
|
|
|
caustic substance intoxication management
|
wash out mouth, eyes or skin with large volumes of cold water
follow eye wash out with fluorescein corneal exam don't induce emesis or neutralize substance charcoal and steroids are not effective |
|
|
digoxin toxicity etiology
|
from suicide attempt or accidental overdose; hypokalemia predisposes to toxicity
|
|
|
digoxin toxicity presentation
|
nausea, vomitting, diarrhea, anorexia
blurred vision, color abnormalities hallucinations confusion arrhythmia |
|
|
digoxin toxicity diagnosis
|
history + ECG looking for any arrhythmia
check for hyperkalemia |
|
|
digoxin toxicity management
|
repeated doses of charcoal, digoxin antibodies, potassium correction
pacemaker might be necessary for refractory bradycardia or 3rd degree heart block |
|
|
opiate intoxication
|
respiratory depression
respiratory acidosis miosis constipation bradycardia hypothermia hypotension treat with naloxone |
|
|
cocaine intoxication
|
hypertension, hemorrhagic stroke, MI, arrhythmia, seizures
pulmonary edema is specific to crack treat with benzodiazepines for acute agitation combined alpha/beta blockers such as labetalol or alpha blockers such as phentolamine avoid beta blockers |
|
|
benzodiazepine intoxication
|
somnolence, dysarthria, ataxia, stupor
death is not from respiratory depression but concomitant ethanol or barbiturates flumazenil antidote is not always used due to seizures from withdrawal |
|
|
barbiturate intoxication
|
hypothermia, loss of deep tendon reflexes
loss of corneal reflexes, coma and death from respiratory depression no EEG activity can be seen no specific antidote but increase urinary excretion with bicarbonate |
|
|
hallucinogens
|
marijuana, LSD, mescaline, peyote, psilocybin, PCP (angel dust)
|
|
|
hallucinogen toxicity
|
delirium and bizarre behavior
anticholinergic effects (flushed skin, dry mouth, dilated pupils, urinary retention) PCP may cause seizures treat severe intoxication with benzodiazepines |
|
|
lead sources
|
ingested paint, soil, dust, drinking water
|
|
|
lead metabolism
|
absorbed from GI tract, skin or inhalation
5-10% in blood (mostly in RBC) 80-90% in bones, remainder in brain and kidneys |
|
|
lead poisoning presentation
|
adults: abdominal pain, anemia, renal disease, neurologic manifestations
children: abdominal pain, anemia, lethargy, seizures, coma, irreversible mental retardation and cognitive damage |
|
|
lead poisoning diagnosis
|
best test is blood lead levels (<10ug/dL is normal)
lead lines at metaphyseal plate of long bones in children anemia azotemia |
|
|
lead poisoning treatment
|
removal of source
chelators (EDTA, dimercaprol, penicillamine or succimer) acute poisoning: charcoal + urination |
|
|
mercury poisoning
|
interstitial pneumonitis from inhalation
irreversible neurologic symptoms (tremors, excitability, memory loss, delirium, insomnia) GI symptoms from ingestion treat with succimer or dimercarprol |
|
|
salicylates intoxication presentation
|
tinnitus
nausea, vomitting, gastritis hyperventilation, noncardiogenic pulmonary edema hyperthermia, CNS toxicity lactic metabolic acidosis with increased anion gap |
|
|
salicylates intoxication diagnosis
|
most specific test is aspirin level
suggestive is elevated anion gap metabolic acidosis but blood may have ↑pH, ↓pH or normal chest x-ray may be normal or pulmonary edema |
|
|
salicylates intoxication management
|
if within 1 hour of ingestion, gastric decontamination + charcoal
mainstay of therapy is alkalinization of urine with aggressive fluid resuscitation dialysis is sometimes used |
|
|
tricyclic antidepressant intoxication presentation
|
anticholinergic (dry mouth, tachycardia, dilated pupils, flushed skin)
cardiac (wide QRS, ventricular tachycardia) CNS (altered mental status, seizures) |
|
|
tricyclic antidepressant intoxication diagnosis
|
serum drug levels is most specific but EKG is more important to do first
|
|
|
tricyclic antidepressant intoxication management
|
within hours --> charcoal
bicarbonate if cardiac toxicity don't use flumazenil to reverse concomitant benzodiazepine overdose because it leads to seizures |
|
|
head trauma presentation
|
headache, amnesia, loss of consciousness
focal findings are most common with epidural hematomas, then subdural hematomas and contusion |
|
|
head trauma diagnosis
|
CT scan always
hemorrahge is visible immediately subdural hematoma is crescent-shaped epidural hematoma is lens-shaped if focal findings consistent with radiculopathy or spinal tenderness --> cervical spine x-ray concussion diagnosis is loss of consiousness + normal head CT |
|
|
head trauma treatment
|
if intracrannial hemorrhage --> hyperventilation to a PCO2 of 30-35
osmotic diuretics and elevation of head of the bed maintain cerebral perfusion by keeping blood pressure 110-160mmHg |
|
|
subarachnoid hemorrhage presentation
|
acute --> sudden headache, loss of consiousness (50%), focal neurologic symptoms (30%)
long-term --> focal deficits, seizures, rebleeding, hydrocephalus, stroke |
|
|
subarachnoid hemorrhage diagnosis
|
intial best test is CT scan which has 90-95% sensitivity within first 24 hours
if CT is normal and SAH is still suspect --> lumbar puncture for absence of red cells angiography to determine site for surgery inverted or enlarged T-waves on ECG are not alarming |
|
|
subarachnoid hemorrhage management
|
maintain blood pressur at 110-160mmHg
nimodipine to prevent spasm and stroke angiography to determine site of bleeding for surgical correction shunt if hydrocephalus is present |
|
|
skin burns classification
|
first-degree --> skin is intact
second-degree --> blister formation third-degree --> destruction of skin appendages and pain receptors which result in relative lack of pain |
|
|
burn presentation
|
altered mental status, dyspnea, headache and chest pain suggest carbon monoxide poisoning
stridor, hoarseness and dyspnea suggest laryngeal edema soot in nose and mouth suggests impending airway compromise |
|
|
rule of nines for burns
|
arms and head are 9% each
chest, back and legs are 18% each patchy burns estimated with width of hand which is 1% watch out for circumferential burns which compromise circulation |
|
|
diagnosis work-up of burns
|
aside from actual burn, determine carboxyhemoglobin levels in severe burns
chest x-ray and/or bronchoscopy to determine respiratory injury extent |
|
|
definition of severe burns
|
combined second and third-degree burns >20% in adults or >10% in old or young
OR third-degree burns >5% of body surface |
|
|
burn injury management
|
if signs of respiratory injury --> intubation is initial step
if carboxyhemoglobin is elevated --> 100% O2 Ringer lactate fluid rescucitation using Parkland formula H2 blocker prophylaxis, topical silver sulfadiazine to prevent infections grafts as needed |
|
|
Parkland formula
|
4ml of ringer lactate for each % BSA burned per Kg; give 1/2 in first 8 hours, 1/4 in second 8 hours, 1/4 in third
|
|
|
heat stroke
|
lost ability to romeve heat from body
excessive body temperature elevation confusion, disorientation, nausea, blurred vision, seizures hemoconcentration, ↑BUN/creatinine, rhabdomyolysis, anuria, DIC, lactic acidosis place body in cool temperature, water and fan + IV fluid replacement |
|
|
malignant hyperthermia
|
idiopathic reaction to any anesthetic specially halothane and succinylcholine
rhabdomyolysis and hyperthermia treat with dantrolene |
|
|
neuroleptic malignant syndrome
|
reaction to phenothiazines, chlorpromazine, haloperidol
muscular rigidity, hyperthermia, ↑CPK, encephalopathy, rhabdomyolysis treat by removing agent + bromocriptine or dantrolene |
|
|
hypothermia
|
core body temperature <35C
lethargy, confusion, weakness, arrhythmias with J-wave elevation (may mimic ST elevation) treat with warm bed, bath or blankets rescucitation efforts from pulselessness can go on beyond 10 minutes until temperature >35C |
|
|
nonionizing radiation
|
infrared, ultraviolet and microwave; present primarily as burns
|
|
|
ionizing radiation
|
bone marrow depression with infections and bleeding
permanent sterility in males around 4-5Gy nausea and vomitting 100% at 3Gy supportive therapy with antiemetics, transfusions, colony-stimulating factors, antibiotics as needed |
|
|
electrocution presentation
|
local 1st, 2nd and 3rd degree burns
ventricular fibrillation (AC current) aystole (DC current, lightning) respiratory arrest (injury to medulla or respiratory muscle paralysis) neurologic damage loss of consiousness and amnesia in 75% of lightning cases renal failure from dehydration and rhabdomyolysis cataracts in 5-30% |
|
|
electrocution treatment
|
cardiopulmonary resuscitation, fluid replacement, local wound care
|
|
|
types of drowinig
|
dry drowning from laryngospasm, fresh water drowning, sea water drowning
|
|
|
fresh water drowning
|
hypotonic water alters surfactanct and causes collapse
water is absorbed and results in hypervolemia, hemodilution and hemolysis lungs have little water |
|
|
sea water drowning
|
hypertonic water draws fluid into lungs resulting in pulmonary edema, systemic hypovolemia, hemoconcentration
|
|
|
near drowning presentation
|
coma
agitation cyanosis coughing sings of pulmonary edema (tachypnea, tachycardia, rales) |
|
|
near drowning lab exams
|
arterial blood gases show hypoxia and hypercabia and metabolic acidosis
|
|
|
drowning management
|
removal from water
ABCs (first step) endotracheal intubation O2 positive pressure mechanical ventilation (most effective) |
|
|
drowning ineffective treatments
|
abdominal thrusts, antibiotics, steroids
|
|
|
anaphylaxis presentation
|
hives rash (urticaria), angioedema and swelling, dyspnea, stridor, tachycardia, hypotension, hemodynamic collapse
|
|
|
anaphylaxis management
|
antihistamine diphenhydramine
if hemodynamic instability --> epinephrine, IV fluids, antihistamines and steroids |
|
|
cat and dog bites
|
treat with exploration, debridement, irrigation, proper wound care
prohylactic antibiotic of choice is amoxicillin/clavulanate |

