![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
42 Cards in this Set
- Front
- Back
|
define lichen planus? where does it occur IO and EO? |
idiopathic chronic inflammatory mucocutaneous disease affecting stratified squamous epithelium often affects skin can affect genitals, anus, pharynx conjunctival and oesophageal involvement rarely occur |
|
|
what causes LP? (5 reasons) |
genetic predisposition immune mediated more common in HCV seropositive drugs dental materials also link with HEP C |
|
|
what is the pathogenesis of LP? what kind of reaction? what cells are damaged by what? |
cell mediated immunological reaction, precise trigger unknown basal keratinocytes are damaged by langerhans cells, T lymphocytes and macrophages |
|
|
what are the variants of LP? |
reticular (most common) papular plaque like atrophic erosive (2nd commonest) bullous (rare) desquamative gingivitis (descriptive term) |
|
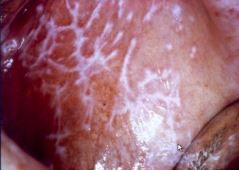
what form of LP is this? |
reticular |
|
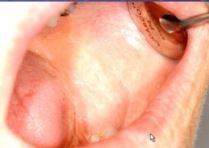
what form of LP is this? |
reticular- mild |
|
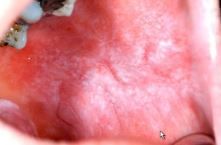
what form of LP is this? |
papular |
|
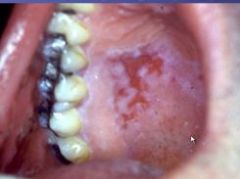
what form of LP is this? |
erosive |
|
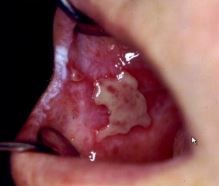
what form of LP is this? |
erosive (buccal) and plaque like (commissure) |
|
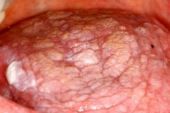
what form of LP is this? |
plaque like |
|
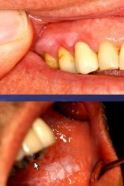
what form of LP is this? |
plaque like |
|
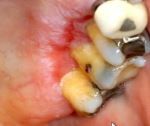
what form of LP is this? |
erosive |
|
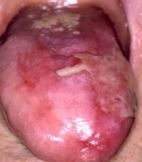
what form of LP is this? |
bullous different from erosive as at bullous stage its like a blister that quickly bursts to form erosive |
|
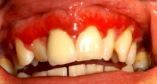
what is this form of LP? what other conditions get this? |
desquamative gingivitis immunobullous diseases (pemphigus/pemphigoid/linear IgA disease) |
|

where is LP on the skin common? what is it like? what induces it? is it permanent? |
flexor surfaces of wrists, a. lower leg, scalp, back puritic (itchy) purply papules lines go through papules- wickhams striae can be induced by trauma- koebner phenomenon resolves leaving hyperpigmentation |
|
|
what do LP genital lesions look like? |
white/erosive lesions |
|
|
what do LP nail lesions look like? |
longitudinal ridging and fissures nail plate thinning (10% of cases) |
|
|
what do scalp LP lesions look like? |
scarring allopecia |
|
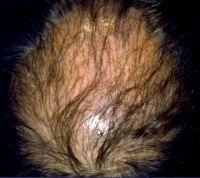
what is this? |
lichen planopilaris hair is thin rather than receded |
|
|
what is likely to get LP? |
middle aged/elderly F>M 2:1 |
|
|
what is the differential diagnosis for LP? |
lichenoid reactions leukoplakia keratosis CHC lupus erythematous immunobullous disease dysplasia/cancer (biopsy)
|
|
|
when do you do blood tests for LP? |
atrophic, erosive or bullous types rule out any anaemia or haematinic deficiency |
|
|
what is the differential diagnosis for desquamative gingivitis? |
lichen planus pemphigus pemphigoid linear IgA disease |
|
|
how is LP managed (general)? |
OHI (desquamative gingivitis) avoid risk factors- smoking and alcohol manage symptoms refer to dermatologist (EO lesions) long term rv |
|
|
how is very mild and mild LP treated? |
asymptomatic- nil V.mild- avoid e.g. spicy food, vinegar.. mild- CHX gluconate 0.2% MW -benzydamine hydrochloride 0.12% MW/spray hydrocortisone sodium succinate 2.5mg (corsodyl, difflam, corlan) |
|
|
how is moderate LP treated? |
stronger topical steroids (not licensed) betamethansone sodium phosphate 0.5mg beclometasone diprionate 50ug x2qds budesonide 64ug qds triamcinolone rinse and antifungal therapy (prevent candiosis) (betnesol, becotide, rhinocort)
|
|
|
what is betnesol? |
betamethasone sodium phosphate moderate strength steroid now on dentist formulary |
|
|
what is becotide? |
beclometasone dipropionate moderate strength steroid |
|
|
what is rhinocort? |
budesonide moderate strength steroid |
|
|
how is severe LP treated? |
systemic prednisolone (check weight, BP, blood glucose and osteoporosis risk)- short term azathioprine other immunomodulators (long term)- retinoids, methotrexate, topical tacrolimus |
|
|
does LP go into remission? |
wax and wane skin lesions remiss earlier |
|
|
is there malignant risk with LP? which types are more at risk? |
1-3% chance of malignancy atrophic and erosive |
|
|
what drugs cause lichenoid drug eruptions? |
antihypertensives esp. ACE inhibitors NSAIDs oral hypoglycaemics gold salts antimalarials carbamazepine can only be confirmed if lesion resolves when its removed |
|
|
what causes lichenoid reactions? |
dental materials- amalgam, gold |
|
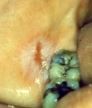
whats this? |
lichenoid reaction (amalgam) must be directly touching/adjacent to source |
|
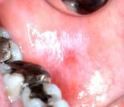
whats this? |
lichenoid reaction (amalgam) |
|
|
what the treatment for lichenoid reaction? |
change restoration if its bothering them if not leave |
|
|
what is lupus erythematosis? what causes it? who gets it? |
autoimmune connective tissue disease autoantibodies against nuclear components uncommon, young adults, F>M |
|
|
what are the types of lupus erythematosis? |
discoid lupus erythematous systemic lupus erythematous |
|
|
what are the symptoms of DLE? |
skin- scaly red patches, scarring, alopecia oral lesions usually on the lops, erythema with white margin |
|
|
what are the symptoms of SLE? |
skin- photosensitive butterfly rash, alopecia joints- pain and swelling heart- raynauds, pericarditis, myocarditis, libman-sacks endocarditis BM- anaemia, thrombocytopenia lungs- pleurisy kidneys- nephritis, hypertension
|
|
|
what are general features of LP? |
usually bilateral, buccal mucosa most commonly but can occur anywhere, rare on palate after the cheeks the tongue and gingiva are most common |

