![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
162 Cards in this Set
- Front
- Back
|
Types of dependent transfers
|
Three-person carry/lift
Two-person lift Dependent squat pivot transfer Hydraulic lift |
|
|
Assisted transfers
|
Sliding board transfer
Stand pivot transfer (lead w uninvolved side) Stand step transfer |
|
|
Which patients should use sliding board transfer?
|
Patient with some sitting balance, some UE strength, and can follow directions.
They should push-up and scoot across the board Avoid skin friction |
|
|
Wheelchair fitting - Seat height / leg length
|
from heel to popliteal fold and add 2 inches to allow clearance of the footrest
|
|
|
Wheelchair fitting - Seat depth
|
from posterior buttock, along lateral thigh to popliteal fold; then subtract 2 inches to avoid pressure from the front edge of the seat against the popliteal speace
|
|
|
Wheelchair fitting - Seat width
|
widest aspect of buttocks, hips, or thighs and add 2 inches to provide space for bulky clothing and clearance of trochanters
|
|
|
Wheelchair fitting - Back height
|
from seat of the chair to the floor of the axilla with user's shoulders flexed to 90 degrees
Then subtract 4 inches for learance of inferior angles of scapula Consider seat cushion height |
|
|
Wheelchair fitting - Armrest height
|
from seat of chair to olecranon process with elbows flexed to 90, then add 1 inch
|
|
|
Where should patients grasp the parallel bars?
|
4-6" in front of the body
|
|
|
Proper fit of axillary crutches
|
Place crutches six inches in front and two inches lateral to the patient.
Crutch height should be no greater than 3 finger widths from axilla Handgrip should be aligned with ulnar styloid (20-25 degrees of elbow flexion) |
|
|
Lofstrand crutches
|
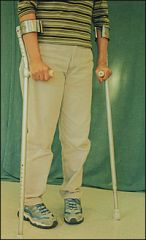
Require highest level of coordiantion for proper use.
Arm cuff should be 1-1.5" below the olecranon so it does not interfere with elbow flexion |
|
|
Cane
|
Provides minimal stability
Straight cane should not be used for PWB Quad cane is better for limiting WB and improving balance Used in opposite side of involved LE Handgrip should be aligned with ulnar styloid (20-25 degrees of elbow flexion) |
|
|
Guarding during ambulation
|
Stand to the affected side and slightly behind patient.
Grasp gait belt with one hand, other hand is on patient's shoulder (not the arm) Move the lead foot when the patient moves |
|
|
Ascending stairs with assistive device
|
AD turned sideways
Walker - one hand on AD, one on handrail Crutches or cane - one hand holds handrail and same hand holds AD Up with good, then bad, then AD Down with bad, then good, then AD |
|
|
If the patient loses and cannot regain balance when ascending stairs
|
Transition the patient toward the handrail or lower the patient slowly toward the stairs
|
|
|
If the patient loses and cannot regain balance when descending stairs
|
Move them into a sitting position
|
|
|
Gastric tube
|
Small incision in abdomen into the stomach for long-term feeding
Jejunostomy tube also for long-term feeding |
|
|
What is an arterial line used for?
|
Measure BP or obtain blood samples
|
|
|
What is a central venous pressure catheter used for?
|
Measures pressure in R atrium or superior vena cava.
Used to evaluate the right ventricular function, right atrial filling pressure, and circulating blood volume |
|
|
What is a R atrial catheter (Hickman) used for?
|
For long-term administration of substances into the venous system.
Inserted through the cephalic or internal jugular vein and threaded into the superior vena cava and right atrium. |
|
|
What is a pulmonary artery (Swan-Ganz catheter) used for?
|
Provides continuous measurements of pulmonary artery pressure.
Is a soft, flexible catheter that is inserted through a vein into the pulmonary artery |
|
|
What is the max flow of a nasal cannula?
How far is it inserted? |
6 L per min
Approximately 1 cm into each nostril. |
|
|
What type of images does a CT scan produce?
|
Cross-sectional
|
|
|
What does an electroencephalography measure?
|
Electrical activity of the brain
|
|
|
What does a MRI provide an image of?
|
bone and soft tissue
|
|
|
Conduction
|
Gain or loss of heat from direct contact
Hot pack, cold pack, paraffin, ice massage, cryo cuff |
|
|
Convection
|
Gain or loss of heat resulting from air or water moving in across the body, such as blood flowing
Fluidotherapy, whirlpool |
|
|
Conversion
|
When non-thermal energy is absorbed into tissue and transformed into heat
Requires a medium Diathermy, ultrasound |
|
|
Evaporation
|
Vapocoolant spray
|
|
|
Radiation
|
Transfer of heat from a radiation energy source of higher temperature to one of cooler temperature
Laser, UV light, infrared lamp |
|
|
Stages of cryotherapy perceived by patient
|
Cold, burning, aching, analgesia
Should be continued until patient reports analagesia |
|
|
Ice massage - use and parameters
|
Anti-inflammatory effects
Can be used to enhance contraction 5-10 minutes is typically adequate Maintain skin temperature above 59 degrees to decrease risk of frostbite Most rapid cooling |
|
|
Temperature at risk for frostbite
|
59 degrees F
|
|
|
Storage of cold packs - temperature
|
25 degrees
30' cooling between uses recommended two or more hours of cooling before initial use |
|
|
Cold packs cool tissue how deeply
|
2 cm after ~20 minutes
|
|
|
How long to apply cold packs to decrease spasticity
|
30'
|
|
|
Temperature of water bath and duration of tx
|
55-64 degrees F
15-20' |
|
|
What are hot packs filled with?
|
bentonite
|
|
|
Temperature of hot pack storage
|
158-167 degrees
|
|
|
How many layers of towels to use with hot packs
|
6-8 layers
Typical hot pack cover = 2 or 3 layers |
|
|
Should patients lie on a hot pack?
|
No. This removes some water from the hot pack which can result in accelerated heating and increased risk of burns
|
|
|
Temperature of fluidotherapy unit
Treatment time |
100-118 degrees F
Usually 15-20 minutes |
|
|
Infrared lamp - uses and parameters
|
Enhances soft tissue healing
Should be placed 20 inches from patient Heats first few mm of human tissue Generally 15-30 minutes Tends to dry the skin; heating is non-uniform |
|
|
Paraffin bath temperature
|
133 - 122 degrees F
|
|
|
Methods of paraffin application
|
Dip-wrap - dip in bath 6-10 times, remove, then wrap w plastic
Dip-reimmersion - after 6-10 dips, leave it in Paint application - Used for body parts that can't be submerged |
|
|
How often to change paraffin
|
6 months or whenever it becomes contaminated
|
|
|
Deep thermotherapy - agents and depth of heating
|
Ultrasound - 3 MHz - 1-2 cm
Ultrasound - 1 MHz - up to 5 cm Diathermy Heats by conversion |
|
|
Underwater ultrasound
|
Rubber or plastic basin
0.5-3.0 cm away from skin Increased intensity required (up to 50%) |
|
|
Can you use ultrasound with a stationary technique?
|
Yes. When you have a very small treatment area or when pulsed ultrasound is used with low intensity
|
|
|
ERA
|
Effective radiating area - area of the transducer that transmits ultrasound energy
Always smaller than total size of transducer head |
|
|
BNR
|
Beam nonuniformity ratio- ratio between the spatial-peak intensity and spatial-average intensity
Based on qualities of the piezoelectric crystal. Lower BNR is more favorable since patients will be less likely to experience hot spots and discomfort during treatment. Listed on the device Should range from 2:1 to 8:1 Higher ratio - more critical to keep transducer moving |
|
|
Depth of ultrasound is determined by which variable?
|
Frequency
Higher frequency is absorbed more rapidly than lower frequency 1 MHz - deep (up to 5 cm) 3 MHz - superficial (1-2 cm) |
|
|
What primarily determines thermal vs non-thermal ultrasound?
|
Duty cycle = (on time / on time+off time) x 100
20% or less = non-thermal Continuous = 100% duty cycle Pulsed = not 100% |
|
|
Duration of US to heat tissue 2-3x size of transducer head
|
5'
|
|
|
How large of an area should you treat with US?
|
Not more than 4x larger than ERA of transducer
|
|
|
Diathermy dosing
|
Dose 1 - No sensation of heat
Dose 2 - Mild Dose 3 - Moderate Dose 4 - Vigorous heating that is tolerable before the pain threshold 20' for thermal effects |
|
|
Lowboy tank
|

Allows for long sitting up to mid-thoracic
|
|
|
Highboy tank
|

chest-high water with hips and knees flexed
|
|
|
Hubbard tank
|
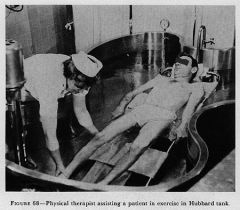
full body immersion
|
|
|
Whirlpool
|
provides agitation and aeration
Allows therapist to direct flow of water directly toward or away from body part being treated Variety of sizes for isolated body part or full body immersion |
|
|
GFCI
|
Ground fault circuit interrupter
Required for all hydrotherapy units Designed to cut off electrical supply to equipment when any form of leakage or ground-fault is identified |
|
|
What position should you place a patient for traction to treat a lumbar disk protrusion?
|
Prone
|
|
|
What % of patient's body weight needs to be included to overcome the force of friction?
|
25%
Split table - eliminates majority of friction |
|
|
Lumbar traction - % body weight for soft tissue stretch?
|
25% - treats muscle spasm, disc protrusion
|
|
|
Lumbar traction - % of body for vertebral separation?
|
50%
|
|
|
Typical duration of treatment for lumbar traction
|
10' up to 30'
|
|
|
Cervical traction - amount of head flexion to target different vertebral segments?
|
Upper - 0-5 degrees
Mid - 10-20 degrees Lower - 25-35 degrees |
|
|
Which structure should the traction force be applied to?
|
Occiput
Not the chin |
|
|
Cervical traction - required force for soft tissue stretch?
|
7-10% body weight
11-15 pounds |
|
|
Cervical traction - required force for vertebral separation?
|
13-20% body weight
20-30 pounds Never over 30 |
|
|
Duration of cervical traction
|
5-30 minutes
Disk - 10' or less Up to 30' for other conditions Based on patient tolerance and symptom response |
|
|
How does compression work?
|
Keeps venous and lymphatic flow from pooling in venous system and interstitial space
|
|
|
What is the difference between long stretch and short stretch bandages?
|
Long stretch - greatest resting pressure; very little working pressure. Used for immobile patient
Short stretch - low resting pressure; high working pressure. Used most often during exercise |
|
|
Intermittent compression - pneumatic pump pressure value
|
30-80 mm Hg
|
|
|
Amplitude is measured in
|
volts, microvolts, millivolts
|
|
|
Frequency measured in
|
Hertz
= Number of pulses delivered through each channel per second |
|
|
FES
|
Functional electrical stimulation
Used to create or enhance the performance of a functional activity Example - stimulating anterior tibialis during gait to enhance dorsiflexion |
|
|
NMES - electrode placement
|
Aligned in parallel
Separated by minimum of 2" One over motor point |
|
|
NMES - parameters
|
Pulse duration - must be high to illicit contraction because muscle fibers are deep. Shorter pulse duration more comfortable for smaller muscles; longer pulse durations for large muscles
Frequency - Must be sufficient to produce a tetanus contraction - 35-50 pps Tx time - 10-20 contractions at least 3x per week |
|
|
Which mode of electrical stim uses 4 electrodes?
|
Interferential current
|
|
|
Iontophoresis - Dose
|
Multiply current x amplitude = milliam minutes
40-80 mA-min Example - 4.0 mA x 10 min = 40 mA-min |
|
|
What type of current is used for iontophoresis
|
Continuous direct current
|
|
|
Cathode vs anode
|
Cathode -
Anode + |
|
|
Iontophoresis - Under which electrode is at risk for an acidic reaction?
|
Anode - Positive - hydrochloric acid formation
|
|
|
Iontophoresis - Under which electrode is at risk for an alkaline reaction?
|
Cathode - Negative - sodium hydroxide formation
|
|
|
Positive polarity Ions / meds
|
Copper sulfate (fungal infection)
Lidocaine (analgesia, inflammation) Magnesium sulfate (muscle spasms, ischemia) Zinc oxide (healing, dermal ulcers, wounds) |
|
|
Negative polarity ions / meds
|
Acetic acid (calcific deposits, myositis ossificans)
Calcium chloride (Scar tissue, keloids, muscle spasms) Dexamethasone (Inflammation) Iodine (scars, adhesive capsulitis) Salicylates (muscle and joint pain, plantar warts) |
|
|
EMG - normal relaxed muscle exhibits
|
electrical silence
|
|
|
Fibrillation potentials
|
LMN disease
|
|
|
Positive sharp waves
|
denervated muscle at rest
Primarily muscular dystrophy |
|
|
Fasciculations
|
Irritation/degeneration of anterior horn cell, nerve root compression, muscle spasms
|
|
|
Repetitive discharges
|
Myopathies, lesion of anterior cell, peripheral nerves
|
|
|
Biofeedback setup
|
Two active electrodes parallel to muscle fibers and close to each other
Reference/ground electrode placed anywhere on the body, usually between two active electrodes |
|
|
Biofeedback - high versus low sensitivity
|
High - detects extremely small amounts of electrical activity - for relaxation
Low - detect only large amounts of electrical activity - for muscle re-education |
|
|
Tapotement
|
rapid alternating movements such as tapping, hacking, cupping, slapping
Used to enhance circulation and stimulate peripheral nerve endings |
|
|
How to decrease liklihood of a burn using iontophoresis
|
Increase size of cathode relative to anode
Decrease current density Increase space between electrodes |
|
|
Workstation Recommendations
|
18-20" monitor
Split Monitor display 10 degrees below horizontal Monitor 20" away from eyes Hands-free telephone set 30" exercise break every hour Space under desk: - 30" wide - 19" deep - 27" high - 2-3" between top of thighs and the desk |
|
|
What is a half-kneeling lift?
|
Begins in half-kneeling - bottom leg positioned behind and to the side of the object
Object is lifted onto the knee and then up |
|
|
Mode of transmission for infections
|
- Cause - pathogen, virus, etc
- Reservoir - human, animals, objects etc - Portal of exit - Mode of transmission - airborne, contact, vector, etc - Portal of entry - Susceptible host |
|
|
Standard Precautions
|
Hand washing
Gloves - when touching all body fluids, blood secretions, excretions, and contaminated items Mask - For protection during activities that are at risk for splashing of any body fluids Gown - for protection during activities that are at risk for splashing of any body fluids Patient care equipment - properly sanitized Occupational Health and Bloodborne Pathogens - vigilance with sharps -> puncture resistant containers; mouthpieces over mouth-to-mouth resuscitation |
|
|
Airborne Precautions
|
- Private room with monitored air pressure
- 6-12 air changes in room per hour - Room door should remain closed with pt remaining in room - Respiratory protection worn when entering room - Patient wears mask during transport |
|
|
Examples of conditions requiring airborne precautions
|
Measles
Varicella Tuberculosis |
|
|
Droplet precautions
|
- Private room
- Maintain 3' distance, otherwise wear mask - May leave door open - Patient should wear a mask during transport |
|
|
Examples of conditions requiring airborne precautions
|
Influenza, meningitis, pneumonia, pertussis, strep, mumps, rubella
|
|
|
Contact precautions
|
Direct - Transmission through skin-to-skin contact
Indirect - Involves contaminated intermediate object - Private room - Gloves - Gown if you will have close contact |
|
|
Examples of conditions requiring contact precautions
|
GI, respiratory, skin, or wound infections
C-diff e-coli hep A herpes simplex virus scabies ebola |
|
|
Sterile field guidelines
|
Don't talk, sneeze, cough
Don't turn your back on sterile field as back of gown is not sterile Any item that falls below waist level is considered contaminated Other guidelines p 489 |
|
|
Proper hand washing
|
- Warm water
- Remove jewelry - at least 30" (happy birthday twice) - don't touch contaminated surface - rinse thoroughly - turn off water with paper towel |
|
|
PPE
|
Personal protective equipment
- items that are worn and used as barriers to protect someone who is assisting a patient with a potentially infectious disease - gowns, lab coats, masks, gloves, goggles, spill kits, mouthpieces |
|
|
What is the % grade for wheelchair ramp?
|
8.3%
12" rise for 1" run |
|
|
How wide should a wheelchair ramp be?
|
at least 36"
|
|
|
When does a wheelchair ramp need a handrail?
|
If the rise is greater than 6"
Or the run is greater than 72" |
|
|
If the ramp changes direction, what is required?
|
A landing of at least 5' x 5'
|
|
|
Minimum doorway width and depth
|
32" wide
24" deep |
|
|
Maximum height of threshold
|
Less than 3/4 in for sliding doors
Less than 1/2 in for other doors |
|
|
Maximum height of carpet
|
1/2"
|
|
|
Minimum hallway clearance
|
36"
|
|
|
Wheelchair turning radius
|
60" width
|
|
|
Forward reach in wheelchair
|
Low - 15"
High - 48" |
|
|
Side reach in wheelchair
|
24"
|
|
|
Bathroom sink
|
Max height 29"
40" max height of paper towels 17" min depth under sink to wall |
|
|
Toilet height
|
17-19" from floor to top of toilet
|
|
|
Grab bar for toilet
|
not less than 36" length
1.25 - 1.5 " diameter 1.5" spacing between bar and wall 33-36" high |
|
|
In a hotel, what % of rooms should be accessible
|
2%
|
|
|
Parking space dimensions
|
96" width
240" length 2% of total spaces should be accessible |
|
|
Purposes of documentation
|
- Communicate with other treating professionals
- Assistance w discharge planning - Reimbursement - Assistance with utilization review - Legal document regarding the course of therapy |
|
|
How do you make corrections in a chart?
|
Hand-written - single line through error, initial and date
Electronic - must clearly indicate a change was made without deletion of the original record |
|
|
Top 10 tips for defensible documentation
|
1. Limit use of abbreviations
2. Date and sign all entries 3. Document legibly 4. Report progress toward goals regularly 5. Document at the time of visit when possible 6. Clearly identify note types (progress reports, daily notes, etc) 7. Include all related communications 8. Include missed or cancelled visits 9. Demonstrate skilled care 10. Demonstrate discharge planning through the episode of care |
|
|
Top 10 Payer Complaints Regarding Documentation
|
1. Poor legibility
2. Incomplete documentation 3. No documentation for date of service 4. Abbreviations - too many, cannot understand 5. Does not demonstrate skilled care 6. Does not support the billing code 7. Does not support medical necessity 8. Does not demonstrate progress 9. Repetitious daily notes showing no change in patient status 10. Interventions with no clarification of time, frequency, duration |
|
|
Requires that the wishes of competent individuals most be honored. Often referred to as self-determination
|
Autonomy
|
|
|
A moral obligation of health care providers to act for the benefit of others
|
Beneficence
|
|
|
Related to confidentiality and is defined as the moral duty to keep commitments that have been promised
|
Fidelity
|
|
|
The obligation of health care providers to above all else, do no harm
|
Nonmaleficence
|
|
|
A term used when someone fails to recognize another individual's rights and autonomy
|
Paternalism
|
|
|
The ability to take advantage of a moral entitlement to do something or not to do something
|
Rights
|
|
|
Obligation of healthcare providers to tell the truth
|
Veracity
|
|
|
Agencies responsible for quality improvement
|
JCAHO - Joint Commission on Accreditation of Healthcare Organizations
PSRH - Professional Standards Review Organization CARF - Commission of Accreditation of Rehabilitation Facilities NCQA - National Committee for Quality Assurance |
|
|
What does ICF stand for
|
International Classification of Functioning, Disability, and Health
|
|
|
Unacceptable one-sided termination of services by a healthcare professional without patient consent or agreement
|
Abandonment
|
|
|
Failure to exercise the skills that would normally be exercised by other members of the profession with similar skills and training.
|
Malpractice
|
|
|
Failure to do what a reasonable and prudent person would ordinarily have done under the same circumstances
|
Negligence
|
|
|
The ADA and Family and Medical Leave Act are examples of
|
Statutory law
|
|
|
A private or civil wrong or injury, involving omission and/or commission
|
Tort
|
|
|
Responsibilities that must be borne solely by the physical therapist
|
- Interpret referrals when available
- Exam, eval, diagnosis, prognosis - Develop and modify plan of care - Goals and outcomes - Determine when it may be appropriate to use PTA - Re-examination - D/C planning - Oversight of all documentation |
|
|
Subscribers utilize health care providers that are contracted by the insurance company at a lower cost
|
Managed care
- HMO or PPO |
|
|
Subscribers to these insurance plans agree to receive all of their health care services through predetermined providers
|
Health maintenance organization - HMO
|
|
|
Subscribers can choose their health care services from a list of providers
|
Preferred provider organization - PPO
|
|
|
A law passed that requires an employer to allow and employee to remain under an employer's group plan for a period of time after the loss of a job, death of a spouse, or decrease in hours or divorce
|
COBRA - Consolidated Omnibus Budget Reconciliation Act
|
|
|
Medicare Part A
|
Hospitals, outpatient diagnostic services, extended care facilities, hospice, and short-term care at home
Automatic enrollment - paid by taxes |
|
|
Medicare Part B
|
Outpatient care, physician services, medical equipment, supplies
Voluntary enrollment - funded through premiums paid by beneficiaries and some taxes |
|
|
Medicare - what % of hospital cost is covered by patient?
|
20%
|
|
|
How long will Medicare pay for extended care facility stay?
|
100 days
|
|
|
Used by PTs and other healthcare professionals to describe the interventions that were provided to a given patient
|
CPT
Most PT codes are in 97000 series |
|
|
Maslow's Hierarchy of Needs
|
Self-actualization needs - realize one's full potential
Esteem needs - to feel respected, recognized, appreciated Affiliative needs - security, stability Physiological needs - basics |
|
|
Classical Conditioning
|
Pavlov
Stimulus paired w response |
|
|
Operant Conditioning
|
B.F. Skinner
Positive reinforcement Negative reinforcement - removing desirable consequences Extinction Punishment - Administering negative consequences |
|
|
Stages of Change
(Trans-theoretical Model) |
Precontemplation - not intending to change
Contemplation - Intending to change behavior in the near future Preparation - making a plan to change behavior Action - implementing plan Maintenance - continuation of bahavior change |
|
|
Health Belief Model
|
1) Perceived susceptibility - you're at risk for a problem
2) Perceived severity - the problem is serious 3) Perceived benefit- changing behavior will reduce the threat 4) Perceived barriers - understanding obstacles to change 5) Cues to action - strategies for change 6) Self-efficacy |
|
|
Domains of learning - Primarily concerned with attitudes, values, emotions
|
Affective domain
|
|
|
Domains of learning - Primarily concerned with knowledge and understanding
|
Cognitive domain
|
|
|
Domains of learning - primarily concerned with physical action or motor skills
|
Psychomotor domain
|
|
|
Stages of dying
|
Denial
Anger Bargaining Depression Acceptance |

