![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
92 Cards in this Set
- Front
- Back
|
Measurement in the lower extremities may be ____ to ______ mm Hg higher in the systolic reading than that of the upper extremities.
|
10 to 40
|
|
|
What signs or symptoms do you expect to find with a patient who is febrile?
|
• Increased body temperature
• Flushed, dry, warm skin • Chills • Feeling of malaise • Tachycardia |
|
|
What interventions are indicated for a febrile patient?
|
•Assessment of vital signs, especially temperature
•Observation of patient response, including skin color and temperature, and chills •Promotion of patient comfort, responding to chills, thirst •Collection of appropriate specimens, such as blood cultures •Promotion of rest and reduction of activities that increase heat production •Promotion of heat loss by removing coverings and keeping the patient dry •Provision of care to meet increased metabolic demands, including oxygen, nutrition, and fluid requirements •Monitoring of ongoing status |
|
|
(def)
Hypotension |
Decrease of systolic and diastolic pressure below normal
|
|
|
(def)
Febrile |
Another word for fever
|
|
|
(def)
Hyperventilation |
Rate and depth of respiration increases
|
|
|
(def)
Vasodialation |
Widening of blood vessels
|
|
|
(def)
Bradycardia |
Pulse rate less than 60 beats per minute for an adult
|
|
|
(def)
Hypertension |
140/90 mm Hg for two or more readings
|
|
|
(def)
Tachypnea |
abnormally rapid rate of breathing
|
|
|
(def)
Hypothermia |
Decreased body temperature
|
|
|
Apnea
|
No respirations for several seconds
|
|
|
(def)
Bradypnea |
abnormally slow rate of breathing
|
|
|
(def)
Eupnea |
Normal breathing
|
|
|
(def)
Auscultatory gap |
Temporary disappearance of sounds between Korotkoff sounds
|
|
|
Give conversion for Fahrenheit to centigrade and
centigrade to Fahrenheit |
(F-32) X 5/9 = C
(9/5 x C)+ 32 =F |
|
|
The nurse is alerted to temperature alterations of above ______ F or below _____ F on an oral Fahrenheit thermometer, and measurements above ______or below ________on an oral centigrade scale.
|
100.4° F or below 96.8° F
38° C or below 36° C |
|
|
Rectal temperature readings may be _____F or ____ C higher than oral measurements, with axillary readings ranging this same number of degrees lower than oral temperatures.
|
0.9° F or 0.5° C higher
|
|
|
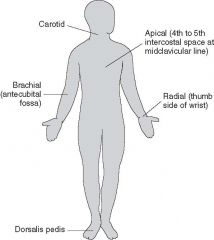
Locate pulse points
Carotid Brachial Radial Apical Dorasalis pedis |
|
|
|
True or False
Vital signs may not be delegated to unlicensed assistive personnel |
False
|
|
|
Interventions that reduce body temperature are:
|
a. Conduction: ice packs, tepid baths
b. Convection: fans |
|
|
The thermometer of choice for a patient in isolation is a ______________________ thermometer.
|
disposable chemical dot
|
|
|
A pulse deficit is assessed by two nurses who synchronize their measurement of the patient’s ____and ______ pulses.
A deficit is found if there is a ________between the two readings. |
apical and radial
difference |
|
|
For a patient who has had a right mastectomy, the _________ or ________ extremities should be used for blood pressure measurement.
|
left arm or lower extremities
|
|
|
Vital signs are usually recorded on a ______or _______sheet.
|
graphic or flow sheet.
|
|
|
Decreasing hemoglobin levels will __________ the respiratory rate.
|
increase
|
|
|
A pulse oximeter may be applied to the ____________, _____________, ______________ .
|
earlobe, finger, or bridge of the nose.
|
|
|
The expected SpO2 level is ______________________
|
greater than 90%.
|
|
|
The correct techniques for blood pressure measurement include;
|
1. cuff is 40% of the circumference of the limb being used
2. cuff is deflated at a rate of 2 to 3 mm Hg per second 3.cuff is inflated to 30 mm Hg above the point where the pulse disappears. 4. systolic blood pressure is identified as the first onset of Korotkoff sounds |
|
|
The appropriate action is to wait _________ minutes before measuring the temperature if the patient has smoked, chewed gum, or ingested hot or cold liquid or food.
|
15 to 30 minutes
|
|
|
A patient’s blood pressure may need to be palpated if the patient's
|
arterial sensations are too weak to create Korotkoff sounds, (e.g. as with severe blood loss)
|
|
|
How are the following vital signs measured differently in children?
a. Temperature: b. Blood pressure |
a. Temperature: Sites for measurement will vary depending on the child’s age and condition. For example, it is contraindicated to take a tympanic membrane temperature on a child with otitis media.
Tympanic membrane: Used in children age 2 and older Axilla: Used with newborns and children of any age Temporal artery: Used in premature infants, newborns, and children b. Blood pressure: An infant or child younger than 5 years of age lies supine with the arm supported at heart level. Older children sit. It is important for the child to be relaxed and calm. Allow at least 15 minutes for children to recover from recent activity or excitement before taking a reading. It may be helpful to have a parent present. You prepare the child for the BP cuff’s unusual sensation during inflation. The cuff needs to be the appropriate width: infant cuff is 21⁄2 to 31⁄4 inches; child cuff is 4 3⁄4 to 51⁄2 inches. |
|
|
Discuss the correct techniques for a tympanic temperature measurement are a, b, and f.
|
1. Using the right ear if the pt has been lying down on his/her left side in bed
2. Pointing the probe midpoint between the eyebrows and sideburns for children younger than 3 years of age 3. Waiting 2 to 3 minutes before repeating the measurement in the same ear |
|
|
A patients pulse is expected to be increased in the presence of which following factors
|
1. Anxiety
2. Presence of asthma 3. Hemorrhage |
|
|
Adult vital signs
Pulse= Blood pressure normal= pre hypertension= hypertension= Respiration = |
Pulse 60 to 100 beats per minute
Blood pressure normal 120/80 pre hypertension= 120- 139 (systolic) 80- 89 (diastolic) hypertension=140- 159 (systolic) 90- 99 (diastolic) Respirations 12 to 20 breaths per minute |
|
|
Child vital signs (age 1 to 8 years)
Pulse = Blood pressure = Respirations = |
Pulse 80 to 100 beats per minute
Blood pressure 105/65 mmHg Respirations 20 to 30 breaths per minute |
|
|
Infant vital signs
Pulse Blood pressure Respirations |
Pulse 120 to 160 beats per minute
Blood pressure 85/54 mm Hg Respirations 30 to 50 breaths per minute |
|
|
A patients body temperature may be reduced after ?
1. Exercise 2. Emotional stress 3. Periods of sleep 4. Cigarette smoking |
3. Periods of sleep
|
|
|
A decrease in the pt's pulse rate is a result of
1. Hemorrhage 2. Hyperthyroidism 3. Respiratory difficulty 4. Epinephrine administration |
2. Hyperthyroidism
|
|
|
A patient is being treated for Hyperthermia what is the patients response to this condition?
1.Generalized pallor 2. Bradycardia 3. Reduced thirst 4. Diaphoresis |
4. Diaphoresis
( profuse sweating) |
|
|
What would you give a patient that is slightly Hypothermic
1. Soup 2. Coffee 3. Cocoa 4. Brandy |
1. Soup
|
|
|
A patient that is febrile - what type of antipyretic medication is ordered
1. Digoxin 2. Prednisone 3. Theophylline 4. Acetaminophen |
4. Acetaminophen
|
|
|
When taking VS, the nurse is alert to the greater possibility of tachycardia for the patient with:
1. Anemia 2, Hypothyroidism 3, a temp of 95° F 4. A pt-controlled analgesic pump (PCA) w/ morphine drip |
1. Anemia
|
|
|
With a hypotensive patient the nurse should be checking to see if the pt is experiencing:
1. Lightheartedness 2. A decreased heart rate 3. An increased urinary output 4. increased warmth to the skin |
3. An increased urinary output
|
|
|
Vital signs that need immediate report of findings are:
1. Pulse pressure of 40 mm Hg 2. Apical pulse of 78,80,76 beats per min 3. Apical pulse of 82 beats per min; radial pulse of 70 beats per min 4. BP of 140/80 LA , 136/74 RA |
3. Apical pulse of 82 beats per min; radial pulse of 70 beats per min
|
|
|
Pulse Adult
Normal range = Tachycardia = Bradycardia = |
normal = 60-100
>100 = tachycardia <60 = bradycardia |
|
|
A tympanic temp assessment is indicated for which pt:
1. After rectal surgery 2. wearing a hearing aid 3. Experiencing otitis media 4. After an exercise session |
1. After rectal surgery
|
|
|
Otitis media
|
An ear infection, most often bacterial or viral infection affects the middle ear
|
|
|
Taking BP on a cardiac care unit- what type of patient should you use a automatic BP device on
1. An irregular heart beat 2. Parkinson disease 3. Peripheral vascular disease 4. A systolic BP great than 104 mmHg |
4. A systolic BP great than 104 mmHg
|
|
|
34 yr old pt annual physical exam- the nurse alerts the Dr to vital findings of:
1. T: 37.6 C 2. P: 120 bpm 3. R: 18 bpm 4. BP: 116/78 mmHg |
2. P: 120 bpm
|
|
|
Where would you check the pulse rate of a child 1 1/2 yr old:
1. Radial artery 2. Apical artery 3. Politeal artery 4. Femoral artery |
2. Apical artery
|
|
|
Pt pulse rate is significantly lower that it has been during the past week. The nurse reassesses and finds that the pulse rate is 46 bpm. The nurse should first:1. 1. Document the measurement
2. Administer a stimulant medication 3. Inform the charge nurse or physician 4. Apply 100% O2 at max flow rate |
3. Inform the charge nurse or physician
|
|
|
The most important sign of heat stroke is:
1. Hot, dry skin 2. Nausea 3. Excessive thirst 4. Muscle cramping |
1. Hot, dry skin
|
|
|
The most accurate temp measurement fro an adult pt experiencing tachypenea and dyspnea is:
1. Oral 2. Rectal 3. Axillary 4. Tymphanic |
4. Tymphanic
|
|
|
what is the correct number of inches for insertion of a rectal thermometer
adult= child= infant= |
adult= 1 to 1 1 1/2
child= 1/2 to 1 infant= 1/2 |
|
|
Intermittent fever is observed by:
1. A constant body temp greater than 38° C (100.4°F) 2. A fever that spikes and falls but does not return to normal 3. Long periods of normal temps with febrile episodes 4. Spikes in readings mixed with normal temps. |
4. Spikes in readings mixed with normal temps.
|
|
|
What is the correct pulse pressure for a pt with a blood pressure of 170/90?
|
80
|
|
|
For a pt that is experiencing a febrile state the nurse should:
1. Ambulate the pt 2. Restrict fluid intake 3. Keep the patient warm 4. Provide oxygen as ordered |
4. Provide oxygen as ordered
|
|
|
A nurse anticipates that bradycardia will be evident if a patient is:
1. Exercising 2. Hypothermic 3. Asthmatic 4. Extremely anxious |
2. Hypothermic
|
|
|
A nurse anticipates that a pt with hypertension will be receiving:
1. Diuretics 2. Antipyretics 3. Narcotic analgesics 4. Anticholinergics |
1. Diuretics
|
|
|
To determine arterial blood flow to a pt feet the nurse should assess which artery?
|
Dorsalis pedis artery
|
|
|
A nurse anticipates an increase in BP for the pt who is:
1. Sleeping 2. Overweight 3. Taking narcotics 4. Hemorrhaging |
2. Overweight
|
|
|
(def)
Body temperature |
•Heat produced minus heat loss = body temp
|
|
|
(def)
Radiation |
Transfer of heat between objects without physical contact
|
|
|
(def)
Conduction: |
Transfer heat from one object to another with direct contact
|
|
|
(def)
Convection: |
Transfer of heat away by air movement
|
|
|
(def)
Evaporation: |
Transfer of heat energy when liquid is exchanged to a gas
|
|
|
give two other words for Fever
|
pyrexia and ‘febrile’
|
|
|
Hypothermia=
Environmental = Intentional = |
temp below normal
winter, frost bite- cold water drowning surgery - cool (metabolic rate) brains and tissues don't need O2 |
|
|
Hyperthermia=
Environmental = Malignant = |
temp above normal
dehydration trauma, medication |
|
|
Advantages of assesing Temps
Fast = Easy access = Responds quickly to changing core temp = Most accurate (not subject to user error or environmental factors) = |
Fast - tympanic, temporal
Easy access – oral, tympanic, temporal Responds quickly to changing core temp – oral, tympanic, temporal Most accurate (not subject to user error or environmental factors) – rectal |
|
|
Rectal temp is ______ degree C > than oral (highest)
Oral temp is ______ degree C > than axillary (lowest) |
0.5 degree C > than oral (highest)
0.5 degree C > than axillary (lowest) |
|
|
S1 (lub) + S2 (dub) = ______ beat
|
1
|
|
|
(def)
Pulse deficit |
difference between apical and peripheral count
|
|
|
Pulse rate ___________________ with age
|
decreases
|
|
|
Blood pressure starts lower in __________________as we age.
|
increases
|
|
|
How do you measure to make sure BP cuff is correct for patient
|
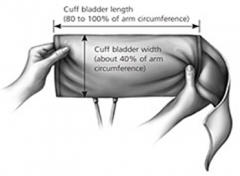
Cuff width (40-60% arm circumference)
Bladder length (80-100% arm circumference) |
|
|
How much do you Inflate the cuff above usual systolic pressure.
|
quickly to 30 mm Hg
|
|
|
What happens - to a
Cuff that is too small Cuff too loose Arm held below heart Arm not supported |

False high:
Heart overpowers cuff. Sounds are heard early |
|
|
What happens - to a
Cuff that is too big Arm held above the heart |
False low:
Cuff overpowers heart. Sounds are heard late |
|
|
Inhalation + exhalation =
|
1 respiration
|
|
|
Normal respiration
|
12 to 20 breaths per minute in a smooth, uninterrupted pattern
|
|
|
(def)
eupnea |
Normal rate and depth -
|
|
|
(def)
tachypnea |
Rapid respiration
|
|
|
(def)
bradypnea |
Slow respiration
|
|
|
(def)
dyspnea |
Labored respiration
|
|
|
Respiration and pulse go ________as the person gets older
|
down
|
|
|
Blood pressure goes _______ as the person gets older
|
up
|
|
|
Temperature _________ as the person gets older
|
stays the same
|
|
|
(def)
Systolic |
Peak pressure when heart is contracting
|
|
|
(def)
Diastolic |
Relaxation, lowest pressure exerted
|
|
|
(def)
Pulse pressure |
Difference between systolic and diastolic pressures
|

