![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
49 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
Upper airways |
Nose, orophaynx, larynx |
NOL |
|
|
Lower airway |
Below larynx |
Bl |
|
|
LAYERS OF AIRWAY |
1. Epithelium 2. Smooth muscle 3.Connective tissue |
|
|
|
Gas exchange units |
ALVEOLUS , PULMONARY CAPILLARY NETWORK SURROUNDS THE ALVEOLI |
Pc |
|
|
Alveolus |
Primary gas exchange unit THIN WALLED. Of epithelial cell layer and thin, elastic basement membrane |
|
|
|
Type 1 alveolar epithelial cell-aka (pneumocytes) |
Extremely thin and provide surface for gas exchange. Covers 90 to 95% of alveolar surface |
Part of alveolus |
|
|
Type 2 alveolar epithelial cell |
SURFACTANT PRODUCTION. Lipoprotein that coats the inner surface of the ALVEOLI. B. Lowers alveolar surface tension and prevents collapse at end expiration. Capable of cell division. Type 1and 2 cell replacement |
4 things |
|
|
Pulmonary CAPILLARY NETWORK SURROUNDS THE alveoli |
Endothelial cells with thin badement membrane. Often fuse with basement membrane of alveolus |
|
|
|
Alveolocapilary membrane |
Very thin, but surface area 70 to 10 ..will cover half a tennis court, if spread out. Very little desperation between gas in the alveolus and blood in the CAPILLARY. Easily damaged |
Vvc |
|
|
Ventilation |
Movement of air between the atmosphere and ALVEOLI |
Air |
|
|
Diffusion |
Movement of gases across a membrane..aka..gas exchange....difusing process ALVEOLI, CAPILLARY, membrane...o2 to co2... |
Gas exhange, passive transport |
|
|
Diffusion of oxygen from ALVEOLI to capillary |
Down it concentration gradient from high PAO2 to lower PaO2....pressure gradient..how much gas, air we breathe |
|
|
|
Diffusion at the tissues across the capillary wall |
Oxygen unloaded down it's concentration gradient from blood-( measure of partial pressure. ) goes To tissues. Co2 picked up moving from high concentration in tissue to low concentration in blood...mitocobdria produce co2 by product of apt production Diffusion of c02 from pulmonary capillary network |
Ocd |
|
|
Perfusion |
Flow of blood through the pulmonary capillary network |
|
|
|
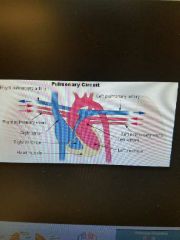
Pulmonary circulation (perfusion) |
Pulmonery arteries brings deoxygenated blood to lung from right heart Pulmonary veins. Brings oxygenated blood from lungs back to left heart |
Pv, pa |
|
|
Bronchial circulation ( perfusion) |
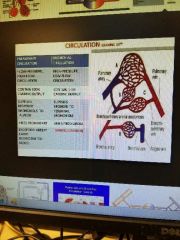
Arterial branch..oxgenated blood to conducting airways, nerves, lymph node, pleura Venous branch. Brings deoxygenated blood back to systemic system or pulmonary veins |
|
|
|
Regulation of flow in response to local factors..perfusion |
Decrease PAO2 to hypoxic pulmonary vasconstriction ....send good blood to alveli to pick up 02.send blood to where concentration gradient is better. |
|
|
|
Regulation of flow don't. Acidosis |
Vasoconstriction....need more blood and oxygen |
|
|
|
Reg of flow. MEDIATORS |
Vasodilators (more blood)and vasoconstrictors(less blood) |
|
|
|
Regulation of flow physiologic effect |
Diverts blood to area of the lung with more adequate ventilation. Can affect more than one area of the entire lung.....opposite of system circulation |
|
|
|
Regulation of flow (Pathophisiologic) |
Pulmonary hypertension |
|
|
|
Perfusion 3 part |
Pulmonary circulation Bronchial circulation Regulation of flow in response to local factors |
|
|
|
Ventilation/Perfusion MATCHING |
Alveolocapilary units receive almost equal amount of ventilation and perfusion |
|
|
|
Ventilation/ Perfusion MISMATCHING |
Abnormal distribution of ventilation and perfusion with respect to each other....pulmonary disease |
|
|
|
V/Q VENTILATION AND PERFUSION MISMATCHING MOST COMMON CAUSE OF ... |
hypoxEMIA |
|
|
|
Ventilation perfusion abnormalties 4 part |
LOW VENTILATION TO PERFISION RATIO VERY LOW HIGH V/Q SILENT UNIT |
|
|
|
LOW V/Q ratio..and Examples |
Alveolar ventilation is impaired but blood flow continues. Chronic bronchitis Asthma |
|
|
|
Very LOW V/Q ratio(Shunt).and Examples |
Alveolus completed unventilated but blood flow continues Atelectasis. Collapse ARDS PNEUMONIA..full of crud, no gas exchange, ventilation low |
|
|
|
High V/Q ratio.(dead space).and Examples |
Alveolus is ventilated but no blood flow thru capillary Pulmonary embolism Low flow states |
|
|
|
Silent unit.....V/Q |
Poor ventilation and poor perfusion |
|
|
|
Dyspnea |
Difficult or labored breathing |
|
|
|
Orthopnea |
Person must be in an upright position to breathe deeply or comfortably |
|
|
|
Paroxysmal nocturnal dyspnea |
Attacks of severe SOB and coughing that generally occurs at night. |
|
|
|
Hemoptysis |
Coughing up blood mixed with sputum |
|
|
|
Kussmaul respiration |
Deep , labored breathing pattern often associated with severe metabolic acidosis, DkA, but also kidney failure |
|
|
|
Cheyne Stokes respiration |
Abnormal patterns of breathing..deeper, faster, temporarily stop breating..apnea |
|
|
|
Cyanosis |
Blueish discoloration. Deoxygenated hemoglobin in blood |
|
|
|
Clubbing |
Deformity of fingers or toe nails associated with a number of diseases mostly heart and lung |
|
|
|
Alterations in PaCO2 concentration(Arterial blood) |
Hypercapnia and hypocapnia, respiratory acidosis |
|
|
|
Hypercapnia |
Elevated CO2 levels. Hypoventilation of the alveoli...not breathing dealt or fast enough Co2 build up in blood |
|
|
|
Hypercapnia Etiology |
Increased airway resistance Decreased drive to breathe Disorder of nervous system function, respiration muscle weakness or paralysis Loss of structural integrity/ elasticity of chest wall or lungs. Result..respiratory acidosis. Myocardial depression , electrolyte abnormalties |
IDDL |
|
|
Increased airway resistance (Hypercapnia ) |
Material within lumen.mucous plugging 2. Thickening or contraction of airway ( broncospasm) 3. Pressure from outside airway. ( tumor) |
|
|
|
Decreased drive to breathe (hypercapnia) |
Drugs acting on can Administration of oxygen, copd to someone who gas list sensitivity to c02 levels as stimulus to breathe and depend on hypoxic drive |
|
|
|
Disorders of nervous system (hypercapnia) |
Infection or i inflammation Trauma Disease of neuromuscular junctions |
|
|
|
Result of hypercapnia |
Respiratory acidosis. Myocardial depression and electrolyte abnormalties |
|
|
|
Hypocapnia |
LOW levels of co2. |
|
|
|
Hypocapnia result |
Respiratory alkalosis...cns irritability and electrolyte abnormalties |
|
|
|
Hypocapnia etiology |
Severe anxiety Traumatic brain injury HypoxEMIA...less oxygen in blood |
|
|
|
HypoxEMIA |
Less oxygen in blood |
|

