![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
358 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
Bilirubin metabolism?
|
Senescent RBCs--->destroyed by splenic macrophages--->
Heme degraded----> UCB--->UCB +abumin----> hepatocytes----> UCB + glucoronic acid----> CB--->heptaic ducts--->GB/CBD--->duodenum---intestinal bacteria--->UBG---> Urobilin---> brown stools --->absorbed in intestines ---> excreted in urine or recycled in liver |
|
|
|
Liver function test: all components?
|
1. ALT
2. AST 3. GGT 4. ALP 5. CB 6. Urine bilin 7. Urine UBG 8. Albumin 9. PT 10. BUN 11. NH3(sr) 12. IgM 13. Antimitochondrial AB 14. Anti-smooth muscle AB 15. ANA 16. AFP |
|
|
|
LFTs indicating liver necrosis?
|
ALT
AST 1. ____(ALT/AST) is located in mitochodria 1. ____(ALT/AST) is located in cytosol |
AST in michondria
ALT in cytosol aLt in cytosoL |
|
|
Condition affecting AST>ALT
|
Alcoholic hepatitis
|
|
|
|
Condition affecting ALT>AST
|
Viral hepatitis
|
|
|
|
Increased GGT indicates which 2 conditions?
|
1. Obstructive jaundice
2. Induction of P450(alcohol) Another liver enzyme indicating liver obstruction? |
Sr. ALP
|
|
|
ALP: sources?
|
1. Liver
2. Bone |
|
|
|
Increased ALP indicates which 2 conditions?
|
1. Obstructive jaundice
2. Osteocalstic activity of bone ***Remember***: ALP + GGT increase indicates cholestasis(obstructive jaundice) |
|
|
|
CB fraction in:
1. Unconjugated hyperbilirubinemia 2. Mixed hyperbilirubinemia 3. Conjugated hyperbilirubinemia? |
1. Unconjugated hyperbilirubinemia:CB<20%
2. Mixed hyperbilirubinemi: CB 20-50% 3. Conjugated hyperbilirubinemia: CB >50% |
|
|
|
Increased urine bilrubin is seen in?
|
1. Viral hepatitis
2. Extravascular hemolytic anemia |
|
|
|
Markers for liver function?
|
1. Sr. albumin
2. Prothrombin time 3. BUN 4. Sr. NH3 Abnormal levels of the above indicate what? |
Severe liver dysfunction (eg.cirrhosis)
|
|
|
Markers for immune related liver functions/ABs etc?
|
1. Sr igM
2. Antimichondrial AB 3. Antismooth muscle AB 4. Antinuclear AB |
|
|
|
Increase of each of the following indicate what?:
1. Sr igM 2. Antimichondrial AB 3. Antismooth muscle AB 4. Antinuclear AB 5. AFP |
1. Sr. IgM: Primary biliary cirrhosis
2. Antimitochondiral AB: Primary biliary cirrhosis 3. Anti smooth muscle AB: Autoimmune hepatitis 4. ANA: Autoimmune hepatitis 5. AFP: hepatocellular carcinoma |
|
|
|
Phases of viral hepatitis?
|
1. Prodrome:
a. Fever, b. Increased transmainase c. Atypical lymphocytosis 2. Jaundice 3. Recovery When does maximum(peak) increase in liver enzymes (transaminase) occur? |
Peak in transaminase: Happens just before jaundice occurs
|
|
|
Microscopic findings in acute viral hepatitis?
|
1. Lymphocytic infiltrate
2. Apoptosis of hepatocytes---form---> Councilman bodies 3. Fibrosis If fibrosis occurs what does it indicate? |
1. It indicates progression to post-necrotic cirrhosis
2. Fibrosis is an unfavorable sign |
|
|
MCC of jaundic
|
Viral hepatitis
|
|
|
|
Fraction of uncojugated bilirubin recycled in liver and kidney?
|
20%
|
|
|
|
Type of hyperbilirubinemias?
|
Unconjugated
Mixed Obstructive |
|
|
|
Increased UCB?
|
Extravascular hemolysis
Spherocytosis (increased UCB production) Gilbert's syndrome Crigler Najjal syndrome Physiologic jaundice of new born Breast milk jaundice |
|
|
|
Gilbert syndrome?
|
Impaired glucoronyl transferase activity
|
|
|
|
In Gilbert syndrome sr UCB rarely exceed ____mg/dl
|
5 mg/dl
|
|
|
|
Gilbert syndrome: rx?
|
None needed
|
|
|
|
Crigler Najjar syndrome?
|
No glucoronyl transferase activity
|
|
|
|
Physiologic jaundice of new born begins on ___day of life
|
3rd
Mechanism of physiologic jaundice of new born? |
Increased macrophage mediated destruction of RBCs---> inability of the liver to handle the excess load
|
|
|
Breast milk jaundice due to?
|
Pregnane-3alpha-20alhpa diol
|
|
|
|
Mixed CB : observed in?
|
Viral hepatitis
why mixed bilirubinemia? |
Since uptake and conjugation both are affected
|
|
|
Obstructive CB: associated conditions?
|
Intrahepatic:
1. Dubin Johnson 2. Rotor syndrome 3. Primary biliary cirrhosis 4. OCP induced Extrahepatic: 1. Gallstones in CBD 2. Ca head of pancreas Extrahepatic Gallstones Ca head of pancreas |
|
|
|
Dubin Johnson syndrome?
|
Defective secretion into the bile ducts- black pigment in hepatocytes
|
|
|
|
Congenital defect hepatocellular defect associated with :
1. Impaired glucoronyl activity? 2. Black pigmentation of hepatocytes 3. Jaundice with alcohol/barb consumption? 4. no rx needed(safe) 5. with no enzyme activity(fatal) 6. AR pattern 7. AD pattern 8. MCC of hereditary jaundice? |
1. Impaired glucoronyl trasnferase activity: Gilbert syndrome
2. Black pigmentation: Dubin-Johnson syndrome 3. Jaundice with alcohol/barb consumption: Gilbert syndrome 4. No rx needed: Gilbert syndrome 5. With no enzyme activity: Crigler Najjal syndrome 6. AR: Gilbert, Rotor, DJ syndrome 7. AD pattern: Gilbert syndrome 8. MCC of hereditary jaundice: Gilbert syndrome |
|
|
|
In Gilbert syndrome: jaundice seen with?
|
1. Fasting
2. Alcohol 3. Phenobarbital |
|
|
|
In extravascular hemolysis: AST/ALT/GGT/ALP is increased?
|
AST
|
|
|
|
Is bilrubin- direct/indirect a normal finding?
|
NO-
Urobilin however is |
|
|
|
First marker for hepatitis infection?
|
HBsAg
|
|
|
|
Marker for hepatitis that appears after appearance of HBsAG and disappears before it?
|
HBeAg
|
|
|
|
Hepatitis marker that persists during "window phase" aka "Serologic gap"?
|
Anti-HBV core AB
Is Anti-HBV core AB protective? |
No
|
|
|
Marker for immunization for HBV?
|
Anti-HBV surface surface AB
Is Anti-HBV surface AB protective? |
YES
|
|
|
HBsAg appears after _____weeks following exposure
|
2-8 weeks
|
|
|
|
How long does HBsAg persist following in acute hepatitis?
|
For 4 months
Persistance of HBsAg indicates ____ |
Chronic hepatitis
|
|
|
Acute hepatitisAnti-HBV core AB : IgM/IgG?
|
IgM
Converts to IgG after 6 months |
|
|
|
Healthy chronic carrier of Hep B: Marker status?
|
Presence of:
1. HBsAg 2. anti-HBc IgG 3. No DNA and e AG |
|
|
|
Infective chronic carrier: marker status?
|
Presence of:
1. HBsAg 2. anti-HBc IgG 3. DNA and e AG |
|
|
|
MCC of jaundice in US?
2nd MCC of jaundice in US? |
#1 Viral hepatitis
#2 Gilbert syndrome |
|
|
|
Hepatitis A virus: route of transmission?
|
Feco-oral route
|
|
|
|
Hepatitis A: symptoms?
|
1. Jaundice
2. Fever 3. Nausea/vomiting 4. Abdominal pain |
|
|
|
Hepatitis A: patient population affected?
|
1. Day care centers
2. Prisons 3. Homosexuals 4. Travelers |
|
|
|
Hepatitis B: Clinical findings?
|
1. Painful hepatomegaly
2. Serum sickness 3. Vasculitis- PAN 4. Urticaria 5. Polyarthritis 6. Membranous glomerulonephritis (Diffuse membranous glomerulonephritis) nephrotic syndrome |
|
|
|
serum sickness?
|
Type III allergic reaction (to prots)
1. Lymphadenopathy 2. Arthralgia 3. Rash 4. Hypotension |
|
|
|
Hepatitis B: complications?
|
1. Chronic/carrier state
2. Fulminant hepatitis following co-infection with hep D |
|
|
|
Rx of hep B?
|
IFN-alpha
Lamivudine Liver transplant |
|
|
|
MCC of liver transplant in United states?
|
Hep C
|
|
|
|
Hepatitis not associated with carrier state/chronic state?
|
Hep A
|
|
|
|
MCC of blood borne related infectious transmission?
|
Hep C
|
|
|
|
Hep C: Causes?
|
1. IVDA
2.Post-transfusion (rare after 1987) |
|
|
|
Hep C: maternal-fetal transmission: rare/frequent?
|
Rare (unlike HIV)
|
|
|
|
Hepatitis C: Clinical findings?
|
1. Subclinical hepatitis
2. Jaundice(rare) Clinical associations with hep C? |
1. Type I RPGN
2. Porphyrea cutanea tarda 3. Lichen planus 4. B cell lymphoma |
|
|
Hepatitic C: Rx?
|
1. IFN-alpha
2. Liver transplant |
|
|
|
Hepatitis D: Associated with which infection?
|
Superinfects Hep B infection
Chronic infection develops in ____% of people infected |
60-85%
|
|
|
Jaundice is observed in which viral hepatitides?
|
1. Hep A
2. Hep B 3. Hep C (uncommonly seen) |
|
|
|
Hepatitis E: population group affected most?
|
Pregnant women
Hepatitis E is fatal/non fatal in women? |
Fatal in women
|
|
|
MCC of liver transplantation in the US?
|
Hep C
|
``
|
|
|
Routes of transmission:
Hepatitis A Hepatitis B Hepatitis C Hepatitis D Hepatitis E? |
Hep A:
Feco-oral Hep B: Parenteral Oral Sexual Vertical Hep C: Parenteral Sexual Hep D: Parenteral Sexual Hep E: Fecal-oral |
|
|
|
Hepatitis with:
1. Feco-oral route transmission 2. Complication of hepatocellular carcinoma 3. No preventive vaccine available 4. IVDA as a major cause 5. No carrier/chronic state 6. PAN 7. polyarthritis 8. Porphyria 9. aka "infectious hepatitis" 10. aka "serum hepatitis" 11. membranous glomerulopathy 12. Type I RPGN 13. Cryoglobulinemia 14. Serum sickness syndrome 15. B cell lymphoma 16. Fulminant in pregnancy 17. Lichen planus 18. Rx with alpha-IFN? |
1. Feco-oral route transmission: Hep A
Hep E 2. Complication of hepatocellular carcinoma: Hep B, HepC 3. No preventive vaccine available: Hep C 4. IVDA as a major cause: Hep C 5. No carrier/chronic state: Hep A 6. PAN: Hep B 7. polyarthritis: Hep B 8. Porphyria: Hep C 9. aka "infectious hepatitis": Hep A 10. aka "serum hepatitis": Hep B 11. Membranous glomerulopathy: Hep B 12. Type I RPGN: Hep C 13. Cryoglobulinemia: Hep C 14. Serum sickness syndrome: Hep B 15. B cell lymphoma: Hep C 16. Fulminant in pregnancy: Hep E 17. Lichen planus: Hep C 18. alpha-IFN: |
|
|
|
Cryoglobulinemia is associated with which clinical conditions?
|
1. Multiple myeloma
2. Hep C |
|
|
|
HCV: Confirmatory test?
|
Step 1: EIA---> if +ve---->
Step 2: Recombinant blot immunoassay |
|
|
|
Gold standard for diagnosing HCV?
|
PCR
Detects virus after ____weeks after infection |
1-2 weeks
|
|
|
+ve RIBA and +ve HCV RNA indicates what?
+ve RIBA and -ve HCV RNA indiacates what? |
+ve RIBA and +ve HCV RNA indicates: Active infection
+ve RIBA and -ve HCV RNA indicates: Recent recovery from infection |
|
|
|
Anti-HDV IgG in HDV is ____(protective/non protective)
|
IgG in HDV is "nonprotective"
"igg in hDv is Defective so non protective" |
|
|
|
Anti-HEV IgG in HEV virus is ____(protective/non protective)
|
IgG in HEV is "protective"
"igg in hEv is Effective so protective" |
|
|
|
Markers for HV?
|
1. HBsAg
2. HBeAg/HBV DNA 3. Anti-HBc-IgM 4. Anti-HBc-IgG 5. Anti-HBs |
|
|
|
Tumor marker configuration for:
1. Earliest acute HBV 2. Acute infection 3. Window phase/serologic gap 4. Recovery 5. Immunized 6. "Healthy" carrier 7. Infective carrier? |
1. Earliest phase:
HBsAg +ve HBeAg/HBV DNA -ve Anti-HBc-IgM -ve Anti-HBc-IgG -ve Anti-HBs -ve 2. Acute infection: HBsAg +ve HBeAg/HBV DNA +ve Anti-HBc-IgM +ve Anti-HBc-IgG -ve Anti-HBs -ve 3. Window phase: HBsAg -ve HBeAg/HBV DNA -ve Anti-HBc-IgM +ve Anti-HBc-IgG -ve Anti-HBs -ve 4. Recovery: HBsAg -ve HBeAg/HBV DNA -ve Anti-HBc-IgM -ve Anti-HBc-IgG +ve Anti-HBs +ve 5. Immunized: HBsAg -ve HBeAg/HBV DNA -ve Anti-HBc-IgM -ve Anti-HBc-IgG -ve Anti-HBs +ve 6. Healthy carrier HBsAg -ve HBeAg/HBV DNA -ve Anti-HBc-IgM +ve Anti-HBc-IgG +ve Anti-HBs -ve 7. Infective carrier: HBsAg +ve HBeAg/HBV DNA +ve Anti-HBc-IgM -ve Anti-HBc-IgG +ve Anti-HBs -ve |
|
|
|
Type of hyperbilirubinemia observed in hepatitis?
|
Mixed
|
|
|
|
Trend (increased/decreased) observed in hepatitis for following:
1. CB blood 2. UCB blood 3. UBG urine 4. Sr. AST 5. Sr. ALT |
1. Increased CB in blood
2. Increased UCB in blood 3. Increased UBG in urine 4. Sr.ALT>Sr. AST |
|
|
|
Infectious hepatitides of liver: Name em + causative agents
|
1. Ascending cholangitis: E-coli
2. Liver abscess: E-coli B-fragilis S-faecalis 3. Granulomatous hepatitis: M.Tb Histoplasma 4. Sponatneous peritonitis: E-coli(adutls) S.pneumonia(children) 5. Leptospirosis: L.interrogans 6. Amebiasis: E.histolytica 7. Clonorchiasis: Clonorchis sinensis 8. Schistosomiasis: S. mansoni 9. Echinococcosis: E.Granulosus |
|
|
|
Ascending cholangitis?
|
Infection of bile ducts
Occurs concurent to _____ Causative agent:____ |
Concurrent to "Bile duct obstruction(bile stone)"
Causative agent: E-coli |
|
|
Ascending cholangitis: symptom triad?
|
1. Fever
2. Jaundice 3. RUQ pain |
|
|
|
Ascendng cholangitis: Complications?
Rx? |
Complication: Multiple liver abscess
Rx? |
Decompression and drainage of abscess
For infection: Piperacillin-tazobactam |
|
|
Liver abscess: causative agents?
|
1. Ecoli
2. B.fragilis 3. S.faecalis |
|
|
|
Liver abscess: modes of spread
|
1. Ascending cholangitis
2. Intra-abdominal infection 3. Direct extension(empyema of GB) 4. Hematogenous spread |
|
|
|
Liver abscess: Ix?
|
1. MRI
2. Ultrasound 3. CT scan Liver abscess: rx? |
Ceftriaxone + metronidazole
|
|
|
MCC of multiple liver abscesses?
|
Ascending cholangitis
Remember the triad: 1. Fever 2. Jaundice 3. RUQ pain |
|
|
|
Granuloatous hepatitis: Causative agents?
|
M.tb
Histoplasma capsulatum |
|
|
|
Spontaneous peritonitis in children: causes?
Rx? |
1. E-coli(adults)
2. S.pneumoniae(children) rx: cefotaxime |
|
|
|
Leptospirosis: Causative agent?
|
Leptospira interrogans
|
|
|
|
Leptospirosis: Clinical features?
|
Biphasic disease:
Fever Jaundice Hemorrhagic diathesis Intersititial nephritis Conjunctivitis Photophobia Meningitis Immune phase: Presence of organisms in urine |
|
|
|
Leptospirosis: Dx? Rx?
|
Dark field microscopic examination of urine.
Presence of numerous organisms in the urine- 1. tightly wound (look like fusilli) 2. crook ends Rx: penicillin G |
|
|
|
Liver abscess from amebiasis: MC site in liver?
|
Right lobe
|
|
|
|
Clonorchiasis: causative agent?
|
Clonorchis sinensis
|
|
|
|
Clonorchiasis:
Intermediate host? Definitive host? |
Intermediate host:
1st intermediate host: Snail 2nd intermediate host: fish Definitive host: humans |
|
|
|
Clonorchiasis: Pathogenesis?
|
Larvae ---> superior mesenteric vein ---> Portal vein ---> adult worms ---> lay eggs ---> concentric fibrosis (vessel wall) ---> cirrhosis ---> portal HTN ---> ascites ---> esophageal varices
|
|
|
|
Clonorchiasis: Rx?
|
Praziquantel
|
|
|
|
Echinococcosis: Causative agent?
|
E. granulosis
(sheepherder's disease) |
|
|
|
"Pipestem cirrhosis"
|
Observed in clonorchiasis:
Concentric fibrosis due to host reaction against egg deposition IN VESSEL WALL |
|
|
|
Echinococcosis: sites of cysts/organs affected?
|
#1 Liver
2 Lung 3 Brain |
|
|
|
Echinococcosis:
Definitive host Intermediate host? |
Definitive host:
1. Sheep Intermediate host: 1. Humans 2. Sheep Sheep-->Dog-->Humans(forms hydatid cyst) |
|
|
|
Hydatid cyst: layers?
|
1. Outer layer of fibrosis(host)
2. Inner layer of fibrosis(parasite) 3. Inner germinal layer 4. Protoscolices |
|
|
|
Hydatid cyst: where are the larvae located?
|
Located in the inner germinal layer
(larvae aka protoscolices) |
|
|
|
Hydatid cyst: complications?
|
Rupture of cyst--> anaphylaxis
|
|
|
|
Hydatid cyst: Rx?
|
Drainage of cyst
Albendazole Praziquantel |
|
|
|
Autoimmune hepatitis: variations in severity?
|
1.Symptomatic with increased transaminase
2. Fulminant 3. Cirrhosis |
|
|
|
Autoimmune hepatitis: Population affected?
|
Women
|
|
|
|
Autoimmune hepatitis: important clinical associations?
HLA associations? |
1. Hashimoto's thyroiditis
2. Grave's disease HLA DR3 and HLA DR4 |
|
|
|
Types of autoimmune hepatitis?
|
Type 1 and Type 2 (?)
|
|
|
|
Laboratory findings for type 1 autoimmune hepatitis?
|
1. ANA
2. Antismooth muscle antibodies 3. Increased serum transaminase 4. Decreased sr. albumin 5. Increased sr. transaminase |
|
|
|
Autoimmune hepatitis: rx?
|
Corticosteroids + Azothioprine
Liver transplantation |
|
|
|
MCC of neonatal hepatitis?
|
Idiopathic
|
|
|
|
Viral associations of neonatal hepatitis?
|
CMV
|
|
|
|
Neonatal hepatitis: Inborn error of metabolism as a possible cause?
|
Alpha-1-antitrypsin deficiency
|
|
|
|
Neonatal hepatitis: Microscopic features?
|
1. Multinucleate giant cells
|
|
|
|
Reye syndrome: Postinfectious triad?
|
1. Encephalopathy
2. Microvesicular fatty change 3. Transaminase elevation |
|
|
|
Reye syndrome: common age group of incidence?
|
Age<4yrs
|
|
|
|
Reye syndrome: Pathogenesis?
|
1. Mitochondrial damage-->
2. Defective B-oxidation of fats 3. Disruption of urea cycle (both B-oxidation of fats and urea cycle take place in the mitochondria) |
|
|
|
Reye syndrome: Microscopic findings?
|
1. Microvesicular steatosis:
i Cytoplasmic fat globules ii. Do NOT displace the nucleus iii. No inflammatory inflitrate |
|
|
|
Reye syndrome: Clinical findings?
|
Initial:
1. Afebrile 2. Quiet 3. Liver dysfuction with hepatomegaly Encephalopathy- progression in order: 1. Lethargy/sleepy-responsive 2. Stupor, seizures, decorticate rigidity- pupillary reflexes intact 3. Coma- Decerebrate rigidity- fixed dilated pupils 4. Deep Coma- Flaccidity, loss of deep tendon reflexes (fixed diated pupils) 5. Death |
|
|
|
Reye syndrome: Labratory findings?
|
1. Increased transaminases
2. Increased PT 3. Hypoglycemia 4. Increased NH3 5. Increased bilirubin |
|
|
|
Reye's syndrome: Rx?
|
1. Mannitol/ glycerol/hyperventilation]]==>
all to reduce cerebral edema (Hyperventilation--> alkalosis--->induces vasoconstriction |
|
|
|
Acute fatty liver of pregnancy: cause?
|
B-oxidation of fatty acids
|
|
|
|
Pre-eclampsia: Pattern of liver damage?
|
Liver necrosis around portal triads (zone 1): increased serum transaminase
|
|
|
|
HELLP syndrome?
|
1. Hemolytic anemia
2. Elevated liver enzymes 3. Low platelets |
|
|
|
Fulminant hepatic failure: causes?
|
Viral hepatitis
Drugs Reye syndrome |
|
|
|
Fulminant hepatic failure: MCC?
|
Viral hepatitis
|
|
|
|
Fulminant hepatitis: MCC (drug) associated with it?
|
Acetaminophen
|
|
|
|
Fulminant hepatitis: Gross findings?
|
1. Wrinkled capsular surface
2. Dull red/yellow necrotic parenchyma Wrinkled capsular surface due to? |
Loss of liver parenchyma
|
|
|
Fulminant hepatitis: Clinical findings?
|
Hepatic encephalopathy
Jaundice |
|
|
|
Fulminant hepatitis: Lab findings?
|
1. Decrease in transaminase
2. Increased in PT and NH3 |
|
|
|
Liver infarction: causes?
|
1. Transplant rejection
2. PAN |
|
|
|
Portal vein thrombosis: causes?
|
1. Pyelophlebitis
2. PCV 3. Hepatocellular carcinoma (tumor invasion into portal vein) |
|
|
|
MCC of intrahepatic obstruction to blood flow?
|
Cirrhosis
|
|
|
|
Intrahepatic obstruction to sinusoids: causes?
|
1. Cirrhosis
2. Peliosis hepatis 3. Centrilobular hemorrhagic necrosis 4. Sickle cell anemia |
|
|
|
Centrilobular hemorrhagic necrosis: causes?
|
1. RHF(congestion)
2. LHF(decreased perfusion) Area around central vein most commonly affected since it is farthest from the portal triad therefore most susceptible to ischemia |
|
|
|
"Nutmeg liver"?
|
1. Enlarged liver with mottled appearance
2. Necrosis of hepatocytes around central vein |
|
|
|
Clinical findings in nutmeg liver?
|
1. Painful hepatomegaly
2. Jaundice 3. Increased transaminase 4. Fibrosis around central vein (cardiac cirrhosis) |
|
|
|
Hepatic condition associated with Bartonella henselae?
|
Peliosis hepatis: sinusoidal dilatation due to blood
|
|
|
|
Peliosis hepatis: causes?
|
1. Anabolic steroids
2. Bartonella henselae--> bacillary angiomatosis seen commonly in HIV |
|
|
|
Posthepatic obstruction to blood flow: causes?
|
1. Hepatic vein thrombosis:
I. Hypercoagulable states i. PCV, ii. OC pills, iii. Prot C/S deficiency, iv. Antiphospholipid syndrome) II. Hepatocellular carcinoma 2. Veno-occlusive disease: Occurs as a complication of_____ where ______happens |
Occurs as a complication of BM transplantation
Collagen develops around the central vein |
|
|
Hepatic vein thrombosis: clinical findings?
|
1. Enlarged painful liver
2. Portal hypertension/ascites/splenomegaly |
|
|
|
Hepati vein thrombosis: first line Dx?
|
#1 Ultrasound with pulsed Doppler
MRI(second line) |
|
|
|
Alcohol related disorders for liver?
|
1. Fatty liver
2. Alcoholic hepatitis 3. Cirrhosis |
|
|
|
Fatty liver: pathogenesis?
|
Substrates of alcohol metabolism are used for synthesis of triglycerides.
|
|
|
|
Fatty liver: clinical findings?
|
Tender hepatomegaly without fever/neutrophilic leukocytosis
|
|
|
|
Fatty liver: Rx?
|
Alcohol rehabilitation
|
|
|
|
Alcohol hepatitis: pathogenesis:
|
1. Actealdehyde---> damage to hepatocytes
2. Collagen synthesis stimulation around venules |
|
|
|
Alcoholic hepatitis: Microscopic findings?
|
1. Fatty change with neutrophilic infiltration
2. Mallory bodies |
|
|
|
Mallory bodies?
|
1. Microscopic finding in alcoholic hepatitis
2. Damaged cytokeratin filaments of hepatocytes 3. Perivenular fibrosis |
|
|
|
Alcoholic hepatitis: clinical findings?
|
1. Painful hepatitis
2. Fever, neutrophilic leucocytosis 3. Ascites 4. Hepatic encephalopathy |
|
|
|
Alcoholic hepatitis: Laboratory findings?
|
1. AST>ALT
2. increased ALP 3. Increased GGT 4. GGT>ALP 5. Thrombocytopenia 6. Hypoglycemia |
|
|
|
Alcoholic hepatitis: Rx?
|
Corticosteroids
Stop drinking |
|
|
|
Types of cholestasis?
|
Intrahepatic
Extrahepatic |
|
|
|
Drugs causing cholestasis?
|
Mainly intrahepatic cholestasis:
1. OC pills 2. Anabolic steroids |
|
|
|
Intrahepatic cholestasis: causes?
|
1. Drugs
2. Pregnancy 3. Neonatal hepatitis |
|
|
|
Extrahepatic cholestasis: causes?
|
1. Stone
2. Ca head of pancreas 3. Primary sclerosing cholangitis 4. Biliary atresia |
|
|
|
Cholestasis:
Gross liver findings? Microscopic findings? |
Gross: Enlarged green liver
Microscopic: Bile ducts distended with bile- (bile lakes) |
|
|
|
Obstructive liver disease:
Clinical findings? Lab findings? |
Jaundice
Pruritis Malabsorption Xanthelasma/xanthoma Light colored stools Lab findings: CB>50% Increased ALP + GGT Absent urine UBG Bilirubinemia |
|
|
|
Intrahepatic cholestasis in pregnancy: fatal/non fatal
cause? |
Non fatal(benign)
Due to estrogen mediated inhibition of bile secretion |
|
|
|
Common indication of liver transplant in the US?
Common indication of liver transplant in children in US? |
Adults: Hep C
Children: Extrahepatic biliary atresia |
|
|
|
Primary sclerosing cholangitis: Clinical associations?
|
Inflammatory bowel disease:
Ulcerative colitis Crohn's Disease (UC>CD) |
|
|
|
Primary sclerosing cholangitis: Cause?
|
Genetic predisposition
|
|
|
|
Drug induced liver tumors?
|
1. Angiosarcoma
2. Cholangiocarcinoma 3. Hepatocellular carcinoma 4. Liver cell adenoma |
|
|
|
Which tumors do these drugs cause?:
1. OC pills 2. Aflatoxin 3. Arsenic 4. Vinyl chloride 5. Thorium dioxide? |
1. OC pills: Liver adenoma
2. Aflatoxin: Hepatocellular carcinoma 3. Arsenic: Angiosarcoma 4. Vinyl chloride: Angiosarcoma, Hepatocellular carcinoma 5. Thorium dioxide: Cholangiocarcinoma Angiosarcoma |
|
|
|
Liver diseases caused by:
1. Amiodarone 2. Methotrexate 3. Retinoic acid 4. Isoniazid 5. OC pills 6. Halothane 7. Acetaminophen 8. Anabolic steroids 9. Methyldopa |
1. Amiodarone: Fatty change, Fibrosis
2. Methotrexate: fatty change, Fibrosis 3. Retinoic acid: Fibrosis 4. Isoniazid: Acute hepatitis 5. OC pills: Cholestasis 6. Halothane: Acute hepatitis 7. Acetaminophen: Acute hepatitis 8.Anabolic steroids: Cholestasis 9. Methyl dopa: Acute hepatitis |
|
|
|
Primary sclerosing cholangitis: Complications?
Clinical findings? Dx? |
Complications:
Cirrhosis Cholangiocarcinoma Clinical findings: 1. Jaundice 2. Pruritis 3. Hepatosplenomegaly |
|
|
|
Primary sclerosing cholangitis:
Dx? Rx? |
Dx: ERCP:
Shows "BEADING" with dye study Rx: 1. Corticosteroids 2. Azathioprine 3. Methotrexate Requires Liver transplant invariably |
|
|
|
Cirrhosis: regenerative nodules?
|
Loss of liver archtitecture
Bands of fibrosis surrounding hepatocyte---> Compress the central veins and sinusoidal veins |
|
|
|
Causes of Cirrhosis?
|
Alcoholic liver disease
Post necrotic cirrhosis Autoimmune hepatitis Primary biliary cirrhosis Hemochromatosis Wilson's disease Alpha-1 antitrypsin deficiency Galactosemia MCC of cirrhosis in adults? MCC of cirrhosis in children? |
Adults: Alcoholic liver disease
Children: AAT deficiency |
|
|
Complications of cirrhosis?
|
Hepatic failure
Portal hypertension Ascites Hepatorenal syndrome Hyperestrinism |
|
|
|
Signs of hepatic failure?
|
1. Coagulation defects
2. Hypoalbuminemia (pitting edema, ascites) 3. Hepatic encephalopathy |
|
|
|
Hypoalbuminemia produces: pitting/non pitting type of edema?
|
Pitting edema
|
|
|
|
Causes of non pitting edema?
|
Lymphatic obstruction
Lipoedema Myxedema |
|
|
|
The two causes of hepatic encephalopathy?
|
1. Aromatic AA(tryptophan, tyrosine, phenylalanine) ---converted---> GABA (false neurotransmitters)
2. NH3 does not get detoxified(dysfunctional urea cycle) |
|
|
|
Factors precipitating encephalopathy?
|
1. Increased protein
2. Alkalosis 3. Sedatives 4. Portasystemic shunts why?(provide reason for each) |
Increased protein--> increased bacterial conversion to NH3 in the gut
Alkalosis keeps NH3 from converting to ionic (NH4+ state) Sedatives have additive effects Portasystemic shunts shunt the portal vein into systemic circulation |
|
|
Clinical findings due to hepatic encephalopathy?
|
1. Altered mentation
2. Disordered sleep rhythm 3. Asterixis(flapping tremors) 4. Coma and death |
|
|
|
Portal hypertension: pathogenesis?
|
Resistance to intrahepatic blood flow due to intrasinusoidal hypertension
|
|
|
|
Complications of portal hypertension?
|
1. Ascites
2. Congestive splenomegaly 3. Esophageal varices 4. Hemorrhoids 5. Caput medusae |
|
|
|
Shunts used in portal hypertension?
|
1. Portacaval: portal vein to IVC
2. Mesocaval: sup.mesenteric to IVC 3. Splenorenal: splenic to renal 4. TIPS: portal with hepatic vein |
|
|
|
Most physiologic shunt?
|
1. Splenorenal shunt
why? |
1. pH gets regulated (reduces)
2. Reduces bleeding from varices without bypassing the liver |
|
|
Transjugular intrahepatic portosystemic shunt?
|
1. Metal stents connect portal vein with hepatic vein
2. Reduces portal vein pressure |
|
|
|
TIPS: disadvantage?
|
1. Increases risk for hepatic encephalopathy
|
|
|
|
Ascites: pathogenesis?
|
1. Portal hypertension
2. Hypoalbuminemia 3. Hyperaldosteronism ( i. Decreased CO stimulates aldosterone synthesis ii. Liver fails to metabolize aldosterone |
|
|
|
Hepatorenal syndrome?
|
Reversible renal failure without renal parenchymal disease
**Creatinine clearance <40ml/minute** |
|
|
|
Charactersitic lab findings in renal failure of hepatorenal syndrome?
|
1. Preservation of renal tubular function
2. Random Na<20mEq/L 3. Absence of proteinuria(<500mg/day) |
|
|
|
Hyperestrinism in males: pathogenesis?
|
Liver fails to degrade:
1. Estrogen 2. 17-ketosteroids (androstenedione) (androtenedione---> estrogen) Clinical findings: 1. Gynecomastia 2. Spider telegectasia 3. Female hair pattern distribution |
|
|
|
Primary biliary cirrhosis: Pathogenesis?
|
Granulomatous destruction of bile ducts in portal triads
|
Other sutoimmune conditios
|
|
|
Primary biliary cirrhosis:
Clinical associations? |
Sjogren's syndrome
|
|
|
|
Primary biliary cirrhosis: age group commonly affected?
|
1. Women
2. 40-50yrs age group |
|
|
|
Primary biliary cirrhosis: Complications?
|
1. Chronic inflammation--->
2. Cirrhosis(PH) 3. Hepatocellular carcinoma |
|
|
|
Primary biliary cirrhosis:
Pathogenesis? |
Environmental insult--->
Stimulates T-cells---> Autoantibodies against mitochondrial membrane complex |
|
|
|
Primary biliary cirrhosis:
Clinical findings |
1. Pruritis
2. Jaundice 3. Inflammatory arthropathy 4. Xanthelasma 5. KF ring in cornea |
|
|
|
Primary biliary cirrhosis:
Laboratory findings |
1. Antimitochondrial antbodies
2. ANA +ve 3. Increased sr IgM 4. Increased ALP and GGT 5. Increased sr cholesterol |
|
|
|
Primary biliary cirrhosis:
Rx? |
1. Budesonide + ursodeoxycholic acid0
2. Cholestryramine (pruritis) 3. Liver transplant |
|
|
|
Secondary biliary cirrhosis: causes?
|
Secondary to extrahepatic bile duct obstruction
(Cystic Fibrosis) NO INCREASE IN AMA/IGM |
|
|
|
Hereditary hemochromatosis: Inheritance pattern?
|
AR
Linked to gene on _____arm of chromosome_____ |
Short arm of chromosome 6
|
|
|
Hereditary hemochromatosis: HLA association?
|
HLA-A3 association
|
|
|
|
Hereditary hemochromatosis: Population commonly affected?
|
Males
Northern European ancestry 5th decade(40-50yrs) |
|
|
|
Hereditary hemochromatosis: Why does it occur later in women?
|
Since menses is protective (causes loss of excess Fe that is absorbed)
|
|
|
|
Hereditary hemochromatosis: Pathogenesis?
|
Mutations of HFE gene(C282Y and H63D)--->
Increased "mucosal" absorption of Fe in duodenum---> Increased Fe---> Hydroxyl free radicals---> Fibrosis |
|
|
|
Hereditary hemochromatosis: Function og HFE gene product?
|
HFE gene product facilitates binding of transferrin to transferrin receptors
|
|
|
|
Hereditary hemochromatosis: Organs affected?
|
1. Liver
2. Pancreas 3. Heart 4. Skin 5. Pituitary 6. Joints |
|
|
|
Hereditary hemochromatosis:
|
Acquired hemochromatosis
|
|
|
|
Hemosiderosis: Causes?
|
1. Blood transfusion
2. Alcohol abuse 3. Well water |
|
|
|
Hereditary hemochromatosis: Clinical findings?
|
1. Cirrhosis
2. Bronze diabetes 3. Degenerative joint disease (chondrocalcinosis) 4. Malabsorption(Exocrine pancreatic function) 5. Restrictive cardiomyopathy (Fe-->fibrosis) 6. Amenorrhea 7. Testicular atrophy |
|
|
|
Hereditary hemochromatosis:
Laboratory findings? |
I. Fe studies:
1. Increased serum Fe 2. Increased percent saturation 3. Increased ferritin 4. Decreased transferrin 5. Decreased percent saturation II. Liver biopsy III. Decreased LH and FSH |
|
|
|
Hereditary hemochromatosis: Microscopic findings?
|
"Prussian Blue" stain used
Hepatocytes filled with blue Fe granules |
|
|
|
Hereditary hemochromatosis:
Best screening test? Best confirmatory test? Screening test for relatives? |
Best screening test: Transferrin saturation
Best confirmatory test: Liver biopsy Screening test relatives: HFE gene testing for C282Y mutations |
|
|
|
Hereditary hemochromatosis: Rx?
|
Phlebotomy
Deferoxamine(Fe chelator) Phlebotomy to be continued until serum serum ferritin falls below ___ and saturation falls below ___ |
Ferritin below 50ug/ml
Saturation<30% |
|
|
For transferrin saturation: what levels (%) indicate that further evaluation is necessary?
|
>45%
|
|
|
|
Wilson'd disease: Inheritance pattern?
|
AR
|
|
|
|
Wilson's disease: Patient population affected?
|
Late childhood
|
|
|
|
Wilson's disease: pathogenesis?
|
1. Defective excretion of copper into bile
2. Defective incorporation of copper into ceruloplasmin ----> Unbound copper increased---> Eventually accumulates (free copper induces fibrosis) |
|
|
|
Free copper accumulation and eventual damage: organs affected?
|
1. Brain
2. Eyes 3. Kidneys 4. Liver (Fe accumulation in: Pancreas, Liver, Skin, Pituitary, Heart) |
|
|
|
Wilson' disease:
Areas of brain affected? Area of the eye affected |
Area of the brain affected:
1. Putamen 2. Subthalamic nucleus 3. Cerebral cortex Area of the eye affected: 1. Cornea |
|
|
|
Wilson's disease: Clinical findings in the eye?
|
KF ring in cornea
What part of the cornea is affected? |
Descemet's membrane
|
|
|
Wilson's disease: renal effects?
|
Renal tubular acidosis
(Fanconi syndrome) |
|
|
|
Wilson's disease: Dx?
|
1. Increased serum free copper
2. Decreased serum copper 3. Decreased serum ceruloplasmin |
|
|
|
Wilson's disease:
Test to detect it in early stages? Test to detect it in late stages? |
Early: Sr ceruloplasmin (Decreased)
Late: Sr. copper(free) (Increased) |
|
|
|
Wilson's disease: Rx?
|
1. Penicillamine (copper chelation)
2. Zinc(inhibits cu absorption) 3. NH4 tetrathiomolybdate 4. Liver transplantation |
|
|
|
Substance that competes with Cu absorption in intestines?
Substance that chelates copper? |
Cu competitor: NH4 tetrathiomolybdate
Copper chelator: Penicillamine |
|
|
|
Alpha-1-antitrypsin deficiency: Inheritance pattern?
|
AD
"Codominance": Each allele expresses itself |
|
|
|
Alpha-1-antitrypsin deficiency:
Variant patterns? |
Variant pattern:
M allele (normal) S allele (abnormal) Z allele (abnormal) |
|
|
|
Alpha-1-antitrypsin deficiency:
Normal pattern? Most severe variant pattern? |
Normal: MM pattern
Most severe: ZZ variant |
|
|
|
ZZ pattern Alpha-1-antitrypsin deficiency:
Levels of AAT in blood? (% wise) |
<15%
|
|
|
|
Alpha-1-antitrypsin:
Associated with _____ and _____ |
1. Emphysema
2. Cirrhosis of liver Type of emphysema associated with alpha-1-antitrypsin deficiency? |
Panacinar
|
|
|
AAT deficiency: Microscopic findings?
|
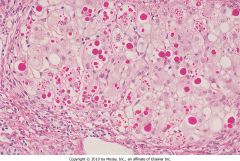
PAS +ve globules in hepatocytes
|
|
|
|
Liver : Focal nodular hyperplasia: Gross findings?
|
1. Poorly encapsulated nodule
2. Central Depressed stellate scar 3. Fibrous septae radiate to periphery |
|
|
|
Liver : Focal nodular hyperplasia: Cause?
|
Reaction to injury
|
|
|
|
Liver : Focal nodular hyperplasia: Rx?
|
Leave it alone (None needed)
|
|
|
|
Liver : Focal nodular hyperplasia: Ix?
|
Ct scan
Observation on CT scan? |
Hypervascular mass with arteriovenous connection
|
|
|
Liver: Benign tumors: Name em?
|
1. Cavernous hemangioma
2. Liver adenoma |
|
|
|
MC liver benign tumor?
|
Cavernous hemangioma
|
|
|
|
Cavernous hemangioma: Best modality for dx?
|
Enhanced CT
|
|
|
|
Cavernous hemangioma: Complication?
|
Intraperitoneal hemorrhage
|
|
|
|
Liver cell adenoma: Causes?
|
1. OC pills
2. Anabolic steroids 3. Von Gierke's disease (glucose-6-phosphatase deficit) Another condition caused by OC pills and anabolic steroids? |
Intrahepatic cholestasis
Anabolic steroids also cause--> peliosis hepatis Another cause of peliosis hepatis? Bartonella henselae (common in HIV) |
|
|
Liver cell adenoma: Gross anatomy?
|
Highly vascular
|
|
|
|
Liver cell adenoma: Complications?
|
Rupture---> Intraperitoneal hemorrhage
What condition is likely to produce rupture of Liver cell adenoma? |
Pregnancy
|
|
|
Malingant liver cell tumors: Name em
|
1. Hepatocellular carcinoma
2. Angiosarcoma |
|
|
|
MC Liver cancer?
|
Mets
|
|
|
|
Liver mets: MC primaries from?
|
Lungs
Other sites? |
GI
Breast |
|
|
MC primary liver malignancy?
|
Hepatocellular carcinoma
|
|
|
|
Hepatocellular carcinoma: MC due to?
|
Hepatitis C(chronic-postnecrotic)
|
|
|
|
Hepatocellular carcinoma: Causes?
|
Most often due to pre-existing cirrhosis:
1. Hep B and Hep C: (Post necrotic) 2. Alcoholic cirrhosis 3. Aflatoxin 4. Hereditary hemochromatosis 5. Wilson's disease 6. Primary biliary cirrhosis 7. AAT deficiency |
|
|
|
Hepatocellular carcinoma: Commonly involves ___vessels?
|
1. Portal vein
2. Hepatic vein |
|
|
|
Hepatocellular carcinoma: Gross findings?
|
1. Maybe focal/multifocal- diffusely infiltrating
2. Portal and hepatci vein invasion |
|
|
|
Hepatocellular carcinoma: Microscopic finding: CHARACTERISTIC finding?
|
Bile in neoplastic cells
|
|
|
|
Hepatocellular carcinoma: Clinical findings?
|
1. Asymptomatic
2. Abdominal pain 3. *Fever* 4. Enlarged liver |
|
|
|
Hepatocellular carcinoma: %of people that present as asymptomatic?
|
33%
|
|
|
|
Hepatocellular carcinoma: Initial clinical presentation?
|
Abdominal pain
|
|
|
|
Hepatocellular carcinoma: Cause of fever?
|
Due to liver cell necrosis
|
|
|
|
Hepatocellular carcinoma: Associated tumor marker?
|
AFP
|
|
|
|
Hepatocellular carcinoma: Lab findings?
|
1. AFP increase
2. ALP increase 3. GGT increase 4. EPO increase 5. Insulin like factor increase 6. PTH increase |
|
|
|
Hepatocellular carcinoma: Ectopic hormones produced?
Effects? |
1. EPO ---> Polycythemia
2. Insulin-like factor ---> Hypoglycemia 3. PTH ---> Hypercalcemia |
|
|
|
Hepatocellular carcinoma: MC metastatic site?
|
Lung (to and from)
|
|
|
|
Hepatocellular carcinoma: Dx?
|
1. CT scan
2. Ultrasound 3. Angiography |
|
|
|
Hepatocellular carcinoma: Rx?
|
1. Liver tranplantation
2. Sx Remember : Chemotherapy/radiation therapy are NOT effective |
|
|
|
Angiosarcoma: Causes?
|
1. Vinyl chloride
2. Arsenic 3. Thorium dioxide (Short sweet and **HY**) |
|
|
|
MC cause of cyst in biliary tract in children?
|
Choldeocal cyst
|
|
|
|
Choledocal cyst: mc age group affected?
|
Children <10yrs
|
|
|
|
Choledocal cyst: Clinical Dyad?
|
1. Abdominal pain
2. Intermittent pain |
|
|
|
Choledocal cyst: Complications?
|
1. Cholelithiasis
2. Cholangiosarcoma 3. Cirrhosis |
|
|
|
Choledocal cyst: Dx?
|
1. Ultrasound
2. ERCP |
|
|
|
Choledocal cyst: Screening test of choice?
|
Ultrasound
|
|
|
|
Choledocal cyst: Test for identifying sites of obstruction?
|
ERCP
|
|
|
|
Caroli disease: Inheritance pattern?
|
AD/AR: both
|
|
|
|
Caroli: disease: pathology?
|
1. Segmental dilation of intrahepatic ducts
2. Portal tract fibrosis |
|
|
|
Caroli disease: Important clinical association?
|
Juvenile polycystic kidney disease
|
|
|
|
Caroli disease: Complications?
|
1. Cholangiocarcinoma
2. Chlonagitis 3. Cholelithiasis 4. Hepatic abscess 5. Portal hypertension |
|
|
|
Caroli disease: Intrahepatic complications?
|
1. Hepatic abscess
2. (portal Htn) |
|
|
|
Caroli disease: Biliary tree related complications?
|
1. Cholangitis
2. Cholangiocarcinoma 3. Cholelithiasis |
|
|
|
Caroli disease: Rx?
|
1. Sx resection
2. Liver transplantation |
|
|
|
MC bile duct malignancy?
|
Cholangiocarcinoma
|
|
|
|
Cholangiocarcinoma: MCC?
|
1. Primary sclerosing cholangitis
Other causes? |
1. Clonorchis sinensis
2. Thorotrast 3. Choledocal cyst 4. Caroli disease |
|
|
Cholangiocarcinoma: MC site?
|
1. Common bile duct
2. Ampulla |
|
|
|
Klatskin's tumor?
|
Cholangiocarcinoma at the junction of right and left bile ducts
|
|
|
|
Cholangioscarcinoma: clinical findings?
|
1. Obstructive jaundice
2. Palpable GB (Courvoisier's sign) 3. Hepatomegaly |
|
|
|
Cholangiocarcinoma: Dx?
|
1. Ultrasound
2. ERCP |
|
|
|
Bile: components?
|
1. Bile salts/acids
2. Phospholipids 3. Water 4. Proteins 5. CB 6. Free CH |
|
|
|
Does bile have free cholesterol?
What is the major form of CH in bile? |
Yes
Major form of CH: bile acids/salts Does bile have CB? Does bile have UCB? |
Has CB but no UCB
|
|
|
Function of bilesalts/acids?
|
Detergent action renders CH water soluble
|
|
|
|
Function of phospholipids?
|
renders CH soluble in bile
|
|
|
|
Types of gall stones?
|
1. Cholesterol stone
2. Pigment stone MC type of stone? |
Cholesterol stone
|
|
|
Cholesterol stones: Radiolucent/Radiopaque?
|
Radiolucent
When are gallstones radiopaque? |
When they contain calcium carbonate
|
|
|
Cholesterol stones are most often pure: true/false?
|
False- they are most often of the mixed variety
(contain ca-bilirubinate) |
|
|
|
Pigment stones: Types?
|
Black and
Brown |
|
|
|
Black pigment stones: cause?
|
Hemolytic anemia
(extravascular hemolysis) |
|
|
|
Brown pigment stones: cause?
|
Infection in common bile duct
|
|
|
|
Pathogenesis of cholesterol stones?
|
Supersaturation of cholesterol in bile
(decreased bile salts/acids) |
|
|
|
Cholesterol stones: population commonly affected?
|
Fat Fertile Female in forty
Use of OC pills People on statins Rapid weight loss |
|
|
|
MOA of estrogen in terms of gall stone pathogenesis?
|
1. Estrogen increases HDL production-->
Increased deposition of cholesterol in bile---> Increased CH in bile---> Stone 2. Increases LDL receptor synthesis 3. Increases Hmg-CoA reductase activity |
|
|
|
Gallstones complications?
|
1. Cholecystitis
2. CBD obstruction 3. Gallbladder cancer(?) 4. Acute pancreatitis |
|
|
|
Acute cholecystitis: important clinical association?
|
Gallstone disease: 95%
|
|
|
|
Stages of development of cholecystitis?
|
Stage 1: Stone lodges in cystic duct
Stage 2: Stone impaction Stage 3: Bacterial invasion (of GB Wall) Stage 4: Perforation |
|
|
|
Cholecystitis: stage 1: Clinical features?
|
1. Midepigastric colicky pain
2. NV without pain relief 3. |
|
|
|
Cholecystitis: stage 2: Clinical features?
|
Shift of pain to RUQ
Radiation to____ |
Scapula
|
|
|
MC bacteria involved in cholecystitis?
|
#1. E.coli
2. B.fragilis 3. Clostridium |
|
|
|
Stage 2 cholecystitis: Pathogenesis following impaction?
|
Accumlation of mucus--> chemical irritation of mucus--> Bacterial overgrowth
|
|
|
|
Stage of cholecystitis associated with invasion?
|
Stage 3
|
|
|
|
Stage 3 cholecystitis: Bacterial invasion of _____
|
GB wall
|
|
|
|
Stage 3 cholecystitis characterisitc findings?
|
1. Rebound tenderness
2. Positive Murphy sign (Pain with catch in breath on inspiration during physical examination) |
|
|
|
Stage 4 cholecystitis?
|
Perforation (d/t distension ---> gall bladder wall perforation)
(rare since majority fall out into gut) |
|
|
|
Cholecystitis : causes?
|
#1 Gallstones
2 CMV infection (HIV) 3 Cryptosporidium (HIV) 4 Dehydration |
|
|
|
Is gall bladder palpable in cholecystitis?
|
Non
(very rarely) |
|
|
|
Cholecystitis: laboratory findings?
|
Neutrophilic leukocytosis
Increased AST/ALP Increased serum amylase Increased serum bilirubin |
|
|
|
Cholecystitis: gold standard test?
|
Ultrasound
Detects stone only if _____ |
if stone size> 12 mm in diameter
|
|
|
Ultrasound uses in detecting stones(besides identifying gallstones)?
|
1. Evaluates GB wall thickness
2. Detects sludge |
|
|
|
Tests used to detect stones besides ultrasound?
|
1. Plain X-ray
2. Hepatobiliary Iminodiacetic acid radionuclide scan (HIDA): NO TRACER in duodenum indicates gall stones |
|
|
|
Indication of CBD exploration in cholecystitis?
|
1. Jaundice
2. GB dilation>12mm 3. Acute pancreatitis 4. No stones in GB |
|
|
|
Cholecystitis: rx?
|
1. Cholecystectomy
2. ERCP with sphincterectomy 3. Meperidine for pain (never use morphine) 4. Penicillin-tazobactam |
|
|
|
Chronic cholecystitis: clinical findings and Ix?
|
1. Severe persistent pain 12 hrs post prandially
2. Pain radiation to right scapula 3. Recurrent espigastric distress 4. Belching/bloating |
|
|
|
Cholesterosis: where does the cholesterol deposit?
gross appearance? |
1. In macrophages
2. Yellow speckled mucosal surface |
|
|
|
Porcelain GB?
|
GB with dystrophic calcification
|
|
|
|
GB adenocarcinoma: Pathogenesis/cause?
|
1. Chronic cholelithiasis
2. Porcelain GB |
|
|
|
Annular pancreas: Pathology?
|
Small bowel obstruction
(dorsal and ventral bud around duodenum) |
|
|
|
Location of abberant pancreatic tissue?
|
1. Stomach wall
2. Duodenum 3. Jejunum 4. Meckel diverticulum |
|
|
|
Acute pancreatitis:
Causes? |
1. Alcohol abuse
2. Gall stones |
|
|
|
Acute pancreatitis: pathogenesis?
|
Obstruction of pancreatic duct or terminal CBD--->
Chemical/infectious/mechanical injury Chemical: Thiazides Alcohol TGs Infectious injury of acinar cells: CMV Mumps Coxsackie Metabolic: Hypercalcemia Ischemia Shock |
|
|
|
Acute pancreatitis:
Associated drugs? Associated viruses? Associated electrolyte abnormality? Associated mechanical problems? |
Drugs:
1. Thiazides 2. Alcohol Viruses: Coxsackie Mumps CMV Electrolyte defect: Hypercalcemia Mechanical problems: Gallstones |
|
|
|
Acute pancreatitis: Enzyme associated with activation of proenzymes?
|
Trypsin
|
|
|
|
Proenzymes responsible for pancreatits and effects?
|
Protease-->acinar cell structure damage
Lipase--> Fat necrosis Phospholipase-->Fat necrosis Elastase-->hemorrhage |
|
|
|
Acute pancreatitis enzymes resposible for following:
1. Hemorrhage 2. Fat necrosis 3. Acinar cell structure damage |
1. Hemorrhage: Elastase
2. Fat necrosis: Lipase and phospholipase 3. Acinar cell structure: Protease |
|
|
|
Pancreatitis: clinical findings?
|
1. Fever
2. Nausea-Vomiting 3. Midepigastric pain 4. Hypoxemia 5. Grey Turner sign 6. Cullen sign 7. DIC 8. Tetany |
|
|
|
Acute pancreatitis: Hypoxemia- pathogenesis?
|
Dueto circulating phospholipase---destroys--> surfactant ---> atelectasis-->
Hypoxemia |
|
|
|
Acute pancreatitis: Findings due to hemorrhage? site?
|
1. Grey-Turner's sign: flanks
2. Cullen's sign: Periumbilical |
|
|
|
Acute pancreatitis: DIC- pathogenesis?
|
Activation of prothrombin by trypsin
|
|
|
|
Acute pancreatitis: Tetany- pathogenesis?
|
Calcium binds to fatty acids (from enzymatic fat necrosis)--> decreased ionized Ca--> hypocalcemia
|
|
|
|
Pancreatitis: complications?
|
1. Pancreatic abscess
2. Pancreatic pseudocyst 3. Pancreatic necrosis 4. Pancreatic ascites |
|
|
|
How do you identify pancreatitis clinically?
|
High fever
High neutrophilia |
|
|
|
Pancreatic pseudocyst dx?
|
1. Abdominal mass with persistence of of serum amylase
|
|
|
|
Pancreatic pseudocyst: ?
|
Collection of pancreatic tissue around the pancreas
|
|
|
|
Pancreatic pseudocyst: diagnostic clue?
|
1. Abdominal mass
2. Persistence of serum amylase longer than 10 days |
|
|
|
Pancreatic pseudocyst: Rx?
|
If <5cm ---> observe (CT)
If>5cm ---> Percutaneous drainage with CT/ultrasound guidance |
|
|
|
Pancreatic abscess: cause?
|
E.coli / Pseudomonas
|
|
|
|
Pancreatic abscess: dx?
|
Radiolucent bubbles in retroperitoneum on CT scan
Aspiration(CT guided) for identifying organism(?) |
|
|
|
Pancreatic abscess: Rx?
|
Imipenem-cilastin
|
|
|
|
Pancreatic ascites: Cause?
|
Secondary to pseudocyst
|
|
|
|
Acute pancreatitis: Laboratory findings?
|
1. Serum amylase
2. Serum lipase 3. Serum trypsin 4. Neutrophilic leukocytosis 5. Hypocalcemia 6. Hyperglycemia(B cell destruction) |
|
|
|
Enzymes specific for acute pancreatitis?
|
Trypsin
Lipase |
|
|
|
Amylase: excretion?
|
In urine:
In pancreatitis renal excretion of amylase is increased |
|
|
|
Serum trypsin is used as a screening test in new born for dx of ________
|
Cystic fibrosis
|
|
|
|
Serum immunotrypsin levels in:
Acute pancreatitis- observed trend Chronic pancreatitis-observed trend? |
Acute pancreatitis:
Increases 5-10 times Chronic pancreatitis: Decreases |
|
|
|
Gold standard for dx of pancreatitis?
|
CT
|
|
|
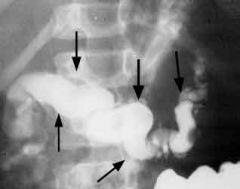
What is the Xray observation due to?
|
Dilation of bile ducts
(repeated attacks of chronic pancreatitis)--> Chain of lake appearance |
|
|
|
Plain abdominal x-ray: findings in acute pancreatitis?
|
1. Left sided plural effusion containing amylase
|
|
|
|
Acute pancreatitis: Rx?
|
1. NPO
2. Crystalloid solution for hypotension 3. Meperidine 4. Nasogastric suction 5. Oxygen |
|
|
|
Acute pancreatitis: hypotension: cause?
|
Third spacing of fluids
|
|
|
|
Chronic pancreatitis: MCC?
|
Idiopathic
|
|
|
|
Chronic pancreatitis: MC known cause?
|
Alcohol
|
|
|
|
Chronic pancreatitis: MCC in children?
|
Cystic fibrosis
|
|
|
|
Chronic pancreatitis:
Causes? |
#1 Idiopathic
#2 Alcohol 3 Cystic fibrosis 4 Malnutrition 5 Autoimmune |
|
|
|
Chronic pancreatitis: typical xray observation?
|
"Chains of lake" appearance
d/t dilated bile ducts |
|
|
|
Chronic pancreatitis: clinical findings?
|
1. Severe pain radiating to back
2. Malabsorption 3. Type I Diabetes 4. Pseudocyst |
|
|
|
Chronic pancreatitis: Lab findings
|
1. Increased amylase
2. Increased lipase 3. Increased immunoreactive trypsin Tests for insufficiency: 1. Secretin stimulation test 2. Bentiromide test (Cleaved to PABA and excreted in urine) |
|
|
|
Chronic pancreatitis: CT scan
|
CT scan shows dystrophic calcification
|
|
|
|
Chronic pancreatitis: Rx?
|
1. NSAIDs
2. Pancreatic enzymes 3. Fat soluble vitamins 4. Octreotide for pain relief(?) |
|
|
|
Pancreatic cancer: type?
|
Adenocarcinoma
|
|
|
|
Adenocarcinoma pancreas: Causes?
|
1. Smoking
2. Chronic pancreatitis 3. Hereditary pancreatitis 4. DM 5. Obesity 6. Cirrhosis |
|
|
|
Adenocarcinoma pancreas: pathogenesis?
|
Association with K-RAS gene mutation
Mutation of suppressor genes (TP16 and TP53) |
|
|
|
Adenocarcinoma pancreas: Clinical findings?
|
1. Obstructive cholestasis signs
2. Palpable GB 3. Virchow's node 4. Superficial migratory thrombophlebitis(trosseau's sign) 5. Periumbilical node(Sister Mary Joseph nodule) 6. Increased ____tumor marker? |
CA19-9
|
|
|
Adenocarcinoma pancreas: Dx?
|
Helical CT
Biopsy (CT guided) Helical CT: Observation? |
C sign in Ca head of pancreas
(Pancreas indents duodenum-looks like C) |
|
|
Adenocarcinoma pancreas: Rx?
|
Chemorads
Sx Name the sx? |
whipple's procedure
|
|
|
Whipple's sx: parts resected?
|
1. Head
2. Neck of pancreas (Distal pancreas with islets kept intact) 3. Part of CBD |
|
|
|
Pancreatic ca: gold standard test for dx?
|
CA 19-9
|
|

