![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
58 Cards in this Set
- Front
- Back
- 3rd side (hint)
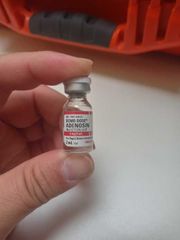
adenosine (Adenocard, Adenoscan) |
Classification: Antidysrhythmic
Action: Slows atrioventricular conduction
Indication: • Supraventricular tachycardia • Wolff-Parkinson-White (WPW) syndrome • Monomorphic wide-complex tachycardia Contraindications: • Atrial fibrillation • Atrial flutter • Polymorphic ventricular tachycardia (Torsades de Pointes) • Second-degree and third-degree heart block
dose: • 6.0 mg RAPID bolus over 1 to 3 seconds followed by 20 mL normal salineflush • If no response to the initial bolus after 1 to 2 minutes, administer 12 mgRAPID bolus over 1 to 3 seconds followed by 20 mL normal saline flush PEDIATRIC• 0.1 mg/kg (up to 6.0 mg) RAPID bolus over 1 to 3 seconds followed by5 to10 mL normal saline flush • If no response to the initial bolus after 1 to 2 minutes, administer 0.2 mg/kg(up to 12 mg) RAPID bolus over 1 to 3 seconds followed by 5.0 to 10 mLnormal saline flush Route: iv onset 20-30 seconds duration 30s
|
|
|
atropine
|
Classification: anticholinergic parasympathetic blocker, antidote
Contraindications: • Known hypersensitivity to the drug • Tachycardia • Hypothermia-induced hemodynamically significant bradycardia
Indication: • Hemodynamically significant bradycardia • Organophosphate poisoning • Carbamate poisoning • Nerve agent exposure Action: • Blocks the action of acetylcholine • Increases the heart rate • Reverses the symptoms of cholinergic poisoning
Dose:
ADULT• Hemodynamically significant bradycardia: 1.0 mg • May repeat the dosage every 3 to 5 minutes to maximum dosage 3.0 mg • Organophosphate poisoning/carbamate poisoning/nerve agentexposure:1.0 to 4.0 mg • May double the dosage every 5 minutes • ET: 2.0 to 2.5 mg diluted in 10 mL normal saline PEDIATRIC DOSAGES • Hemodynamically significant bradycardia: 0.02 mg/kg • May repeat the dosage every 3 to 5 minutes to maximum dosage 1.0 mg inchildren and 2.0 mg in adolescents • Organophosphate poisoning/carbamate poisoning/nerve agentexposure: 0.03 to 0.05 mg/kg every 10 to 20 minutes route: • IV• IO• ET
|
|
|

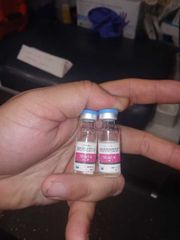
amiodarone (Cordarone) |
Class: antiarrhythmic
Action: • Blocks sodium, potassium, and calcium channels • Prolongs the action potential and repolarization • Slows the sinus rate • Increases the length of the PR interval and QT interval
Indication: • Ventricular fibrillation • Pulseless ventricular tachycardia • Wide complex tachycardia
Contraindications: • Cardiogenic shock • Hemodynamically significant bradycardia • Second-degree and third-degree heart block • Hemodynamically significant hypotension
ADULT DOSAGES • Cardiac arrest: 300 mg • If no response, administer 150 mg over 3 to 5 minutes • Tachydysrhythmias: 150 mg in 50 mL D5W infused over 10 minutes • Infusion: 1.0 mg/minute PEDIATRIC DOSAGES • Ventricular fibrillation: 5.0 mg/kg • May repeat the dosage every 5 minutes twice • Maximum dosage 300 mg • Ventricular tachycardia: 5.0 mg/kg over 20 minutes • May repeat the dosage twice
Route: • IV• IO• Infusion on set: • 1 to 3 minutes |
|
|

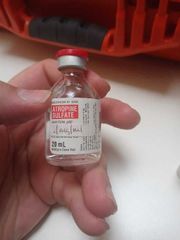
albuterol sulfate (Proventil) |
Class: • Sympathomimetic • Bronchodilator • Beta2 agonist
Contraindications: hypersenstitivity to the drug
Action: relatively selective beta 2 adrenergic bronchodilator. Beta 2 agonist that relaxes bronchial smooth muscle resulting in bronchial dilation. Some beta 1 overlap w/clinically significant cardiac effect such as tachy. Shift potassium intracellular, resulting in lower serum potassium.
Indication: treatment for bronchospasm and hyperkalemia
Route and dose: svn 2.5 in 3ml per bullet |
|
|
|
acetylsalicylic acid, asa (Bayer Aspirin) |
Classification: • Platelet aggregator inhibitor • Nonsteroidal anti-inflammatory Action: inhibits prostaglandin and disrupts platelet function. it also has a mild analgesic & anti-inflammatory. Indication: suspect acute coronary syndrome Contraindications: active gi bleed. allergy and have already taken 324mg Dose: 325mg max Route: oral |
|
|

calcium chloride |
Classification: electrolyte
Action: increases extracellular & intracellular calcium levels. stimulates release of catecholamines. increase cardiac contractile state( +intropic effect) essential to a # physiologic processes including transmission of nerve impluses, contraction of cardiac, smooth and skeletal muscle. has stabilizingeffect on mycardial cell membranes in sitting of hyperkalemia
Indication: suspected hyperkalemia and calcium channel blocker overdose
Contraindication: do not use in setting of suspected digoxin toxicity. hypercalcemia suspected serve hypokalemia (life threatening cardiac arrhythmias may occur) & allergy
ADULT DOSAGES • 500 to 1,000 mg (0.5 to 1.0 Gm) • May repeat the dosage in 10 minutes
PEDIATRIC DOSAGES • 0.2 to 0.25 mL/kg 10% solution
Route: iv/ io |

|
|
|
calcium gluconate 2.5 topical gel |
Classification:Electrolyte Action: used after contact with hydrofluoric acid to neutralizethe floride ion, forming insoluble calcium floride. this helps stop the floride ion from penetrating into the tissue & bone, preventing further damage. the gel does not treat or heal hf burns that have already developed. Indication:used after contact with hydrofluoric acid to mitigate or preventing the related pain and potential tissue burns & bone damage Contraindications: for cutaneous/skin application only & allergy Dose: If possible, the patient should wash the affected area and massage the gel into the skin Route: |
|
|
|
calcium gluconate |
Classification: Action: increases the extracellular & intracellular calcium levels stimulates release of catecholamines. increases cardiac contractile state (+inotropic effect).essential to a # of physiologic processes including transmission of nerve impulses, contraction of cardiac, smooth & skeletal muscles. has stabilizing effects on the myocardial membranes in setting of hyperkalemia. Indication: suspected hyperkalemia. calcium channel blocker overdose. Contraindication: allergy, do not use in the setting of suspected digoxin toxicity. hypercalcemia, saroidosis, suspected severe hypokalemia(life threat cardiac arrhythmais my occur) Dose:ADULT DOSAGES• Hyperkalemia: 1.0 Gm• May repeat the dosage Route: iv |
|
|
|
dexamethasone sodium phosphate -( Prednisone, Decaron) |
Classification: Corticosteroid• Glucocorticoid• Anti-inflammatory Action: improves lung function & myocardial performance. stabilization of lysosomal and membranes, inhibition of compliment-induced granulocyte aggregation. rightward shift in o2 -hemoglobin dissociation curve. inhibition of the prostaglandin and leukotriene production, increase in surfactant production, decrease in pulmonary edema, relaxation of bronochspasm Indication: reactive airway disease: acute exacerbation of bronchial asthma. anaphylaxis Contraindication: systemic fungal infections. preterm infants. allergy Dose:ADULT DOSAGES • 8.0 to 24 mg Route: iv, im |
|
|

Dextrose |
Classification: carbohydrate, antihypoglycimic
Action: rapidly increases blood glucose.
Indication: hypoglycemia
Contraindication: allergy, none in the prehospital setting.
Dose:ADULT DOSAGES• 12.5 to 25 Gm
Route: IV IM |
|
|

diazepam (Valium) |
Classification: • Benzodiazepine • Anticonvulsant • Sedative • Hypnotic
Action: benzo drug, sedative, amnestic effect also deceases seizures by increasing the seizure threshold.
Indication: active seizures. sedation prior to cardioversion, etc
Contraindication: severe respiratory depression, allergy
Dose:adult: 2.0 mg increments over 2 minutes
Route:• IV• IO• IM• Rectal |
|
|
|
diliazem (Cardizem) |
Classification: • Calcium channel blocker • Antidysrhythmic Action: • Slows extracellular calcium ion influx across myocardial cell membranes • Slows conduction through the sinoatrial node and the atrioventricular node • Slows ventricular conduction rates in atrial fibrillation and atrial flutter Indication: narrow complex tachyarrhythmias- afib/flutter. svt not responding to adenosine Contraindication: heart block/bradycardia. systolic bp <90mmhg. sick sinus syndrome. vtach. allergy Dose: • 0.25 mg/kg (usually 20 mg) over 2 minutes • May repeat the dosage 0.35 mg/kg (usually 25 mg) in 15 minutes • Infusion: 5.0 to 15 mg/hour Route: iv/io/infusion |
|
|
|
diphenhydramine (Benadryl) |
Classification: antihistamine Action: histamine h1-receptors antagonist(blocks histamine receptors) of effector cell in repiratory tract, blood vessels, & gi smooth muscles. also has anticholinergic actions, making it useful in treating or preventing acute dystonic reactions to antipsychotic drugs. these reactions include: to antipsychotic drugs: oculogyric crisis, acute torticollis,& facial grimacing Indication: treatment of allergic reaction. treatment or prevention of acute dystonic reaction to antipsychotic drugs Contraindication: known hypersensitivity. newborns. allergy Dose:• Allergic reaction/anaphylaxis: 25 to 50 mg • Phenothiazine reaction with extrapyramidal symptoms: 10 to 50 mg Route: iv/io/im |
|
|
|
dopamine (Intropin) |
Classification: Sympathomimetic • Vasopressor Action: endogenous catecholamine. acts both on dopaminergic and adrenergic neurons. dose dependent effects: 1-2mcg/kg/min- dilates renal and mesenteric blood vessels, typically no effect on HR orBP. 2-10mcg/kg/min- beta effects on heart which increases cardiac output w/o gr8ly increasing HR or BP.10-20- alpha peripheral effects causing peripheral vasocontriction, which results in increase in systemic vascular resisitance(svr) & increase BP.20-40- alpha effects reverse dilatation or renal & mesenteric vessels with resultant decrease flow. increase HR & spo2 demand to undesirable limits Indication: Treatment of refractory cardiogenic or distributive shock Contraindication: Hypovolemia, or allergy Side effects: May induce tachyarrhythmias, in which case infusion should be decreased or stopped. High doses ( 10mcg/kg) may cause peripherial vasoconstriction. Should not be added to sodium bicarb or other alkaline solution since dopamine will be inactivated in alkaline solutions. Consider hypovolemia and treat this with appropriate fluids before administration of dopamine. Dopamine is best administered by an infusion pump to accurately regulate rate. It may be hazardous when used in the field without an infusion pump. Monitor closely Dose: THERAPEUTIC DOSAGE RANGE & RESPONSES• 2.0 to 5.0 mcg/kg/minute:o Negligible beta-adrenergic response• 5.0 to 10 mcg/kg/minute:o Beta-adrenergic responses Positive chronotropic effects Positive inotropic effects• 10 to 20 mcg/kg/minute:o Alpha-adrenergic responses Vasoconstriction Increased blood pressure Increased preload• > 20 mcg/kg/minute:o May increase the heart rate and myocardial oxygen demand toundesirable limitsADULT DOSAGES• Infusion: 2.0 to 20 mcg/kg/minute (reference the Dopamine Dosage Table) Route: infusion |
|
|
|
epinephrine (Adrenaline) |
Classification: Sympathomimetic Action: catecholamine with alpha and beta effects which increases heart rate and BP. potent bronchodilator. Indication: cardiac arrest, bradycardia, anaphylaxis, shock, im for serve refractory wheezing, neb for croup and bronchiolitis Contraindication: uncontrolled hypertentionis a relative contraindication. allergy Side effects: increases cardiac work and can precpitate angina, myocardial infraction or major dysrhythmias in an individual with ischemic heart disease Dose:• Cardiac arrest: 1.0 mg (1:10,000) IV/IO • May repeat the dosage every 3 to 5 minutes during resuscitation • Cardiac arrest: 2.0 to 2.5 mg (1:1,000) ET diluted in 10 mL normal saline • May repeat the dosage every 3 to 5 minutes during resuscitation • Hemodynamically significant bradycardia: 2.0 to 10 mcg/minute infusion • Hemodynamically significant hypotension: 2.0 to 10 mcg/minute infusion • Bronchospasm associated with chronic bronchitis andemphysema/allergic reaction/anaphylaxis: 0.3 to 0.5 mg (1:1,000) IMo Adult EpiPen® auto-injector 0.3 mg IM Route: • IV/IO/IM/ET/Infusion |
|
|
|
etomidate (Amidate) |
Classification: • Anesthesia induction agent • Hypnotic • Sedative Action: sedative and hypnotic. appears to act similar gaba by depressing the activity of the brain stem reticular activating system no analgesic properties Indication: induction of anesthesia for rapid sequence intubation. Contraindication: hypersensitivity and allergy Side effects: not intended for prolonged infusion due to suppression of cortisol and aldosterone production. Dose: 0.2 to 0.6 mg/kg (usually 20 mg) over 30 to 60 seconds Route: iv/io |
|
|
|
fentanyl (Durgesic) |
Classification: Action: opioid agonist-analgesic. inhibits ascending pain pathways, thus altering response to pain, increases pain threshold. produces analgesia, respiratory depression and sedation. Indication: serve pain of any etiology. Contraindications: spo2 lower than 90% or significant respiratory depression and allergy side effects: causes neurologic and respiratory depression. may be worse in pt w/ underlying lung disease or concomitant use of other depressant drugs such asbenzo or alcohol. respiratory support must be available when administering fentanyl. can be reversed with naloxone (narcan). when given to treat pain, the goal is reduction of pain not total elimination. dose: 1mcg/ kg max initial 100mcg with max of 200mcg total. route: iv, |
|
|
|
glucagon (Glucugen) |
Classification: Action: increases serum glucose by releasing glycogen in the liver. will only work if there are sufficient stores of glycogen in the liver, and will not work if pt is malnourished. counteracts effects of beta blocker or calcium channel blocker overdose. Indication: hypoglycemia, symptomatic brady from beta blocker or calcium channel blocker overdose. Contraindication: glucagon is not the 1st line treatment for hypoglycemia and should only be used in pt with symptomatic hypoglycemia when the emct is unable to obtain iv access. allegery Side effects: maybe cause nausea and vomiting. slower onset than iv dextrose. Dose: 1mg may repeat in 7-10min Route: im |
|
|
|
hydroxocobalamin (Cyanokit) |
Classification: antidote Action: precursor to vitamin b12. it binds cyanide ions to form cyanocobalamin (vitamin b12) which is then excreted in the urine Indication: know or suspected cyanide poisoning. closed-space smoke inhalation with: shock, arrest or aloc Contraindication: allergy Side effects: may cause transient elevation of bp. will cause red colored urine ( for up to 5 weeks) and red colored skin (about 2weeks. the red color of the blood serum and urine will interfere with colorimetric laboratory test for several days. Dose: 5.0 Gm over 15 minutes Route: IV, IO |
|
|
|
ipratropium bromide (Atrovent) |
Classification: Anticholinergic Bronchodilator Action: antagonizes action of acetylcholine on the bronchial smooth muscle int he lungs, causing bronchodilation. Indication: brochoconstriction- asthma and copd. ipratropium may be giving in a combination with albuterol is indicated. Contraindication: allergy Side effects: use with caution in pt with narrow angle glaucoma. may include palpitations, dizziness, anxiety, headache, eye pain, urinary retention Dose: • 500 mcg (0.5 mg) in 2.5 mL normal saline (unit dose) via small volumenebulizer (SVN)• In-line with a bag-valve mask (BVM): 500 mcg (0.5 mg) in 2.5 mL normalsaline (unit dose) via SVN• May repeat the dosage Route: Svn |
|
|
|
ketemine (Ketalar) |
Classification: Sedative• Anesthetic• Analgesic Action:• Blocks pain receptors• Produces a dissociative state• Produces anesthesia Indication: excited delirium. induction agent for intubation and pain control Contraindication: angina, chf, pregnancy and allergy Side effects: transient periods of apnea (1-2min) have occured with iv ketamine administration, especially with rapid infusion. may cause laryngospasm - hypersalivation, increased airway secretions - emergence reaction - nystagmus - use with caution in pt with schizophrenia Dose: IV/IO: 1.0 to 2.0 mg/kg over 1 minute• IM: 2.0 to 4.0 mg/kg Route: iv, im |
|
|
|
lidocaine (Xyolcaine) |
Classification: Antidysrhythmic Action: antiarrhythmic drug that decreases automatically by slowing the rate of depolarization. terminates re-entry by decreasing conduction in re-entrant pathways. local anesthesia for pain control caused by infusion of fluids or meds via an IO Indication: cardiac arrest due to vfib of pulseless vtac. wide comlex tac with a pulse. pain management after io insertion in conscious pt. contraindication: bradycardia and allergy Side effects: at higher doses may cause cns stimulation, seizure, depression, and respirtory failure. toxicity is more likely in elderly pt and pt with chf or impaired liver function. Dose:• VF and pulseless VT: 1.0 to 1.5 mg/kg• May repeat the dosage 0.5 to 0.75 mg/kg every 3 to 5 minutes duringresuscitation• Maximum dosage 3.0 mg/kg• Ventricular dysrhythmias with a pulse: 1.0 to 1.5 mg/kg• May repeat the dosage 0.5 to 0.75 mg/kg in 5 to 10 minutes• Maximum dosage 3.0 mg/kg• Maintenance infusion: 2.0 to 4.0 mg/minute• ET: 2.0 to 2.5 times the bolus dosage diluted in 10 mL normal saline Route: • IV• IO• ET• Infusion |
|
|
|
lorazepam (Ativan) |
Classification:• Benzodiazepine• Anticonvulsant• Sedative• Hypnotic Action: benzo that functions as a cns depressant, anticonvulsant and sedative. Indication: seizures - sedation -agitation/ excited delirium - uncontrolled shivering in hyperthermia Contraindication: neurologic or respiratory depression. acute angle glaucoma. allergy Side effects: respiratory depression and/ or hypotension can occur, the pt should be monitored closely. most likely to produce respiratory depression in pt who have taken other depressant drugs, especially alcohol and barbiturates, or when given rapidly. elderly pt may have more profound respiratory and/ or cns depression, half dose should be adminisitered Dose: ADULT DOSAGES• Seizure IV/IO: 2.0 to 5.0 mg over 2 minutes• Seizure IM: 2.0 to 5.0 mg• Procedural sedation IV/IO: 2.0 mg over 2 minutes• Procedural sedation IM: 4.0 mg• Maximum dosage: 10 mg Route: iv, im |
|
|
|
Magnesium sulfate |
Classification: Electrolyte• Anti-inflammatory• Tocolytic (labor suppressant) Action:• Decreases ventricular irritability• Decreases release of acetylcholine that inhibits muscular excitability• Causes uterine relaxation• Relaxes bronchial smooth muscle resulting in bronchodilation• Raises the seizure threshold in eclampsia and preeclampsia Indication: Seizures caused by toxicity of pregnancy (toxemia)• Pregnancy induced hypertension (pre-eclampsia and eclampsia)• Pre-term labor• Torsades de Pointes (polymorphic ventricular tachycardia)• Ventricular fibrillation and pulseless ventricular tachycardia refractory toamiodarone or lidocaine• Reactive airway conditions including bronchoconstriction and bronchospasm Contraindication:Hemodynamically significant heart block Side effects: Central nervous system depression• Drowsiness• Hypotension• Respiratory depression• Dysrhythmias Dose:• Torsades de pointes infusion: 1.0 to 2.0 Gm in 50 to 100 mL over5 minutes• May repeat the dosage 1.0 to 2.0 Gm over 1 hour• Pre-term labor/pre-eclampsia/eclampsia infusion: 3.0 to 6.0 Gm in100 mL over 10 to 20 minutes• May repeat the initial dosage• Maintenance infusion: 1.0 to 4.0 Gm/hour• Reactive airway conditions: 2.0 Gm in 50 mL over 5 to 10 minutes• Cardiac arrest IV/IO: 1.0 to 2.0 Gm over 1 to 2 minutes Route:• IV• IO• Infusion |
|
|
|
methylprednisolone sodium succinate (Soleu Medrol) |
Classification:• Corticosteroid• Glucocorticoid• Anti-inflammatory Action:• Suppresses acute and chronic inflammation• Produces immunosuppressive effect• Stabilizes cellular membranes Indication:• Asthma• Chronic bronchitis• Emphysema• Other reactive airway conditions• Anaphylaxis• Burns involving the airway Contraindication: none Side effects: Dose: 125mg Route: IV.IO |
|
|
|
midazolam ( Versed) |
Classification: benzodiazepine, seditive hyponatic, a Action: Benzo that functions as a CNS depressant, anitconvulsant, and sedative Indication: seizures, sedation, agitation/excited delirium, uncontrolled shivering in hyperthermia Contraindication:Known hypersensitivity to the drug Dose: • Seizure IV/IO: 0.1 mg/kg• Maximum dosage: 4.0 mg• Seizure IM: 0.2 mg/kg• Maximum dosage: 10 mg• Procedural sedation IV/IO: 0.5 to 2.5 mg• Maximum dosage: 0.1 mg/kg• Chemical restraint IV/IO: 0.05 to 0.1 mg/kg• Chemical restraint IM: 0.1 to 0.15 mg/kg Route: IV/IO: 2 to 5 minutes• IM: 15 to 30 minutes |
Benzo |
|
|
morphine sulfate (MS roxon |
Classification:• Narcotic analgesic• Narcotic agonist Action:Alleviates pain by depressing the central nervous system• Depresses brainstem respiratory centers• Decreases venous return to the heart• Decreases preload• Decreases afterload Indication: Pain management• Chest pain and/or signs and symptoms suggestive of the acute coronarysyndrome• Acute cardiogenic pulmonary edema Contraindication:Known hypersensitivity to the drug• Head injury• Decreased level of consciousness• Hemodynamically significant hypotension Side effects: Dose: IV• IO• IM Route:1.0 to 4.0 mg increments over 1 to 5 minutes |
|
|
|
naloxane (Narcan) |
Classification:Narcotic antagonist
Action: Acts as a competitive antagonist at opiate receptors in the central nervoussystem• Reverses the effects of narcotics and synthetic analgesic drugso central nervous system depressiono respiratory depressiono respiratory arrest Indication: Narcotic and synthetic analgesic overdoses including morphine (MSContin® ) heroin oxycodone (OxyContin®) methadone codeine meperidine (Demerol®) fentanyl (Sublimaze®) hydrocodone (Vicodin ®) hydromorphone Unconsciousness of unknown etiology Contraindications: none Side effects: Dose:• 2.0 mg• May repeat the dosage every 2 minutes • ET: 4.0 mg diluted in 10 mL normal saline • Intra-nasal (IN): 1.0 mg sprayed in each nostril with a mucosal atomizerdevice (MAD) • May repeat the dosage every 2 minutes Route: IV• IM• IO• ET• Intra-nasal (IN) |
|
|
|
nitroglycerin (Nitro-bid, Nitrostat) |
Classification:• Vasodilator • Antianginal • Nitrate Action:• Relaxes vascular smooth muscle• Dilates coronary arteries resulting in increased blood flow to the myocardium• Decreases workload on the heart• Decreases myocardial oxygen demand• Decreases preload• Decreases afterload Indication:• Chest pain and signs/symptoms suggestive of the acute coronary syndrome• Congestive heart failure with pulmonary edema Contraindication:• Hemodynamically significant hypotension• Hypovolemia• The patient has taken an erectile dysfunction medication in the previous 48hours including sildenafil (Viagra®) tadalafil (Cialis®) vardenafil (Levitra®) Other phosphodiesterase-5 inhibitor medications Not recommended for use with pediatric patients Side effects: Dose: ADULT DOSAGES• Tablet: 0.4 mg • Single spray: 0.4 mg • May repeat the dosage in 3 to 5 minutes twice after the initial dosage Route: Sublingual |
|
|
|
norepinephrine (Levophed) |
Classification:• Sympathomimetic Action:• Alpha-adrenergic responseo Vasoconstriction• Beta1-adrenergic responseso Increases the heart rateo Increases myocardial contractility Indication:• Severe hypotension refractory to IV boluses caused byo Cardiogenic shocko Septic shocko Neurogenic shock Contraindication:• Hypotension caused by hypovolemia Side effects: Dose: Infusion: 0.1 to 2.0 mcg/kg/minute, titrated to effect Route:Infusion |
|
|
|
ondansetron (Zofran) |
Classification: antiemetic
Action: selectively blocks serotonin5-h73 receptors in the brain Primary effect in the GI tract No effect on dopemine receptors & therefore does not cause extrapymidal symtoms
Indication: nausea & vomiting
Contraindications: pt w/ pronlong qt Pt <1month old Allergy to ondansetron
Side effects: may cause QT prolongation, avoid use in pt w pronlonged QT syndrome Route: IV,IO,PO,SL Dose: 4mg/2ml |
|
|
|
oxytocin (Pitocin) |
Classification:• Pituitary hormone• Uterine stimulant Action:• Binds to oxytocin receptor sites on the surface of uterine smooth muscles• Increases the force and frequency of uterine contractions Indication:• Postpartum hemorrhage Contraindication:• Known hypersensitivity to the drug• Presence of a fetus with impending delivery• Not recommended for use with pediatric patients Side effects: Dose: Infusion: 10 to 20 U in 1,000 mL (1.0 L) of NS or LR• IM: 10 U Route: Infusion• IM |
|
|
|
phenylephrine nasal spray 0.5% ( Neo-synephrine) |
Classification: topical vasoconstrictor Action: stimulates alpha receptors to vasoconstrict blood vessels in the nasal mucosa. Reduces the risk of bleeding during insertion of a nasotracheal tube. Indication: administered prior to insertion of a nasotracheal tube Contraindication: hypersenitivity Side effects: none Dose: 1-2 sprays Route: IN |
|
|
|
pralidoxime (Protopam) |
Classification:Antidote Action:Regenerates cholinesterase activity that became inhibited by anorganophosphate pesticide Indication: organophosphate pesticide poisoning Contraindication: none in the prehospital setting. not recommended for use on peds Side effects: Dose: auto-jet 600mg may repeat after 15min Route: IM |
|
|
|
proparacaine ophthalmic (Alcaine) |
Classification: Topical anesthetic Action: Alleviates pain at the ophthalmic nerve cell membrane Indication:• Chemical exposure to the eyes requiring irrigation Contraindication: Known hypersensitivity to the drug Side effects: Dose:1 to 2 drops Route: Ocular |
|
|
|
rocuronium (Zumeron) |
Classification: Non-depolarizing neuromuscular blocker• Paralytic Action: Binds to nicotinic cholinergic receptor sites at the nerve fiber’s motor endplate• Antagonizes acetylcholine binding at the nerve fiber’s motor end plateresulting in neuromuscular blockade Indication: Induction of paralysis to facilitate rapid sequence intubation Contraindication: hypersensitivity Side effects: Dose: 0.6 to 1.2 mg/kg Route: IV IO |
|
|
|
Sodium bicarbonate 7.8-8.4 |
Class: Alkalizing agent Action:Buffers metabolic acidosis• Increases the pH of blood and urine Indication: • Pre-existing or known metabolic acidosis • Acidosis refractory to effective ventilation • Salicylate overdose • Tricyclic antidepressant overdose • Hyperkalemia • Prolonged cardiac arrest • Crush syndrome Contraindication: none Side effects: Dose: • 1.0 mEq/kg• May repeat the dosage 0.5 mEq/kg every 10 minutes Route: IV IO |
|
|
|
succinylcholine (Anectine) |
Class: Depolarizing neuromuscular, paralytic Action: Inhibits neuromuscular transmission resulting in temporary paralysis Indication: induction of paralysis to facilitate rapid sequence intubation Contraindication: hypersensitivity Side effects: respiratory depression, respiratory arrest, dysrhythmias Dose: 0.6 to 2.0 mg/kg may repeat once in 2-3min for adult 1.0 to 2.0 mg/kg for peds may repeat once in 2-3min Route: IV-IO |
|
|
|
tetracaine (Altacaine) |
CLASS• Topical anesthetic Action: Alleviates corneal pain Indication: Chemical exposure to the eyes requiring irrigation Contraindication:• Known hypersensitivity to the drug• Not recommended for use with pediatric patients Side effects: Dose:1 to 2 drops Route:Ocular |
|
|
|
thiamine (Betlan) |
Class: vitamin Action: Metabolizes carbohydrates Indication: Delirium tremens • Wernicke encephalopathy • Korsakoff syndrome • Unconsciousness of unknown etiology • Alcoholism • Malnutrition Contraindication: NONE Side effects: Dose: 100 mg Route: IV IO ET |
|
|
|
activated charcoal(Actidose ®• EZ-Char ®• Liqui-Char ®)
|
CLASS• Adsorbent MOA• Binds (adsorbs) and inactivates toxic substances in the gastrointestinal tract INDICATIONS• Oral poisonings• Oral overdoses CONTRAINDICATIONS• The patient cannot protect their airway• Ingestion of Caustics Hydrocarbons Acids Corrosives Cyanide Solvents Iron Lithium Lead Petroleum products Route: oral ADULT DOSAGES• 30 to 60 Gm (1.0 to 2.0 Gm/kg) PEDIATRIC • 0.5 to 1.0 Gm/kg |
|
|
|
vasopressin(Pitressin ®)
|
CLASS• Vasopressor MOA• Produces vasoconstriction INDICATIONS• Cardiac arrest: ventricular fibrillation pulseless ventricular tachycardia asystole pulseless electrical activity CONTRAINDICATION• Not recommended for use with pediatric patients ROUTE: IV IO ET ADULT DOSAGES• Cardiac arrest IV/IO: 40 U administered once• Cardiac arrest ET: 40 U diluted in 10 mL normal saline |
|
|
|
verapamil ( Isoptin, Calan) |
Class: Calcium channel blocker antidrysrhythmic MOA: slows extracellular calcium ion influx across myocardial cell membranes slows conduction through the SA node and the AV node slows the ventricular conduction rate in a fib and flutter INDICATIONS • Atrial fibrillation with rapid ventricular rate • Atrial flutter with rapid ventricular rate • Supraventricular tachycardia CONTRAINDICATIONS• Known hypersensitivity to the drug • Hypotension• Myocardial infarction • Cardiogenic shock• Ventricular tachycardia • Second-degree and third-degree heart block • Wolff-Parkinson-White (WPW) syndrome • Not recommended for use with pediatric patients ROUTE• IV• IO ONSET OF ACTION• 2 to 5 minutes ADULT DOSAGES• 2.5 mg over 2 minutes• May repeat the dosage 5.0 to 10 mg in 15 to 30 minutes• Maximum dosage 30 mg |
|
|
|
abciximab (Reopro ®) |
CLASSES• Antiplatelet agent • Platelet aggregation inhibitor M O A• Reversibly binds with Glycoprotein (GP) IIb/IIIa receptors on the surface ofplatelets inhibiting the final common pathway for platelet aggregation • GP Iib/IIIa receptor blockade interferes with the binding of fibrinogen, vonWillebrand factors, and other platelet aggregation modulators to the surface ofplatelets, thus preventing aggregation • Binding with GP Iib/IIIa receptors effectively prevents the formation ofintravascular thrombus and may contribute to the resolution of pre-existingthrombus INDICATIONS• Infusion monitoring during interfacility transport only• Adjunctive to or in preparation of percutaneous transluminal coronary arteryangioplasty (PTCA) for the prevention and treatment of acute coronarysyndrome and associated acute cardiac ischemic complications in patients atrisk for abrupt closure of the treated coronary vessel• Heparin should be concurrently administered and monitored |
|
|
|
albumin, normal serum 5% / 25%( Albuked 5®• Albuked 25®)
|
CLASSES• Blood derivative• Placental human plasma MECHANISM OF ACTION Exerts oncotic pressure which expands the volume of circulating blood andmaintains cardiac output INDICATIONS • Restores plasma volume in burns • Hyperbilirubinemia • Shock • Hypoproteinemia • Prevention of cerebral edema • Cardiopulmonary bypass procedures • ARDS |
|
|
|
bumetanide (Bumex®) |
CLASS:Loop diuretic MECHANISM OF ACTION Inhibits electrolyte reabsorption in the ascending loop of Henle leading to diuresis INDICATIONS • Pulmonary edema • Congestive heart failure |
|
|
|
chitosan (Chitin ®)
|
CLASS: Hemostatic MECHANISMS OF ACTION • This drug is a naturally occurring bio-compatible polysaccharide that becomesextremely adherent when in contact with blood • Seals the wound and controls bleeding • Red blood cells create a seal over the wound as they are drawn into thebandage INDICATION Life-threatening hemorrhage on external wounds as an adjunct with direct pressurewhen direct pressure is ineffective |
|
|
|
cimetidine (Tagamet®) |
CLASSES • Antiulcer • H2 blocker MECHANISM OF ACTION Competitively inhibits action of histamine at the H2 receptor sites of parietal cells,decreasing gastric acid secretions INDICATIONS • Infusion monitoring during interfacility transport • Short-term treatment of duodenal ulcer; maintenance therapy • Pathological hypersecretory conditions • Prevention of upper GI bleeding |
|
|
|
eptifibatide (Integrilin ®) |
CLASSES • Antiplatelet • Platelet aggregation inhibitor MECHANISMS OF ACTION • Reversibly binds with Glycoprotein (GP) IIb/IIIa receptors on the surface ofplatelets inhibiting the final common pathway for platelet aggregation• GP Iib/IIIa receptor blockade interferes with the binding of fibrinogen, vonWillebrand factors, and other platelet aggregation modulators to the surface ofplatelets, thus preventing aggregation INDICATIONS • Infusion monitoring during interfacility transport only • For the treatment of acute coronary syndrome • For patients to be managed medically or those undergoing percutaneoustransluminal coronary angioplasty (PTCA) or atherectomy • Heparin should be concurrently administered and monitored |
|
|
|
famotidine(Pepcid ®)
|
CLASSES • Antiulcer • H2 blocker MECHANISM OF ACTION Competitively inhibits action of histamine at the H2 receptor sites of parietal cells,decreasing gastric acid secretions INDICATIONS • Infusion monitoring during interfacility transport only • Hospitalized patients who cannot take the oral drug or who have intractableulceration or hypersecretory conditions |
|
|
|
insulin
|
CLASS Pancreatic hormone M O A • Promotes glucose transport which stimulates carbohydrate metabolism inskeletal and cardiac muscle and adipose tissue • Promotes phosphorylation of glucose in the liver where it is converted toglycogen • Directly affects fat and protein metabolism • Stimulates protein synthesis • Inhibits release of free fatty acids • Indirectly decreases phosphate and potassium INDICATIONS • Type 1 (insulin-dependent) diabetes mellitus • Type 2 (non-insulin-dependent) diabetes mellitus unresponsive to diet andoral hypoglycemics |
|
|
|
kaolin (Kaolin Clay – Power Pozz®)
|
CLASS Hemostatic M O A : This drug is an inert mineral and promotes clotting by 2 main modes of action: • Activation of Factor XII (FXII) in the presence of kallikrein and high molecularweight kininogen; activated FXII initiates the intrinsic clotting pathway via theactivate of Factor XI; activated FXI continues the coagulation pathway thatends with the formation of a fibrin clot• This drug promotes the activation of platelet-associated FXI and is a distinctand separate molecule from plasma FXI; activated platelet-associated FXIinitiates the intrinsic clotting pathway in normal and FXII deficient patients INDICATION Life-threatening hemorrhage on external wounds as an adjunct with direct pressurewhen direct pressure is ineffective |
|
|
|
nalmefene hydrochloride (Revex®)
|
CLASS: Narcotic (opioid) antagonist M O A• Competitive inhibition at narcotic receptor sites • Reverses respiratory depression secondary to narcotics INDICATIONS Antidote for• Opioid poisoning when naloxone (Narcan®) is not available • May differentiate opioid-induced coma from other causes |
|
|
|
norepinephrine (Levophed®)
|
CLASSES • Sympathomimetic • Alpha- and beta-adrenergic agonist • Inotropic cardiac stimulant • Vasopressor M O A Stimulates beta1 receptors in sympathetic nervous system causing vasoconstriction,increased blood pressure, enhanced contractility, and increased heart rate INDICATION Severe hypotension due to cardiogenic, septic, or neurogenic shock either refractoryto intravascular fluid boluses or in which intravascular fluid blousing iscontraindicated (e.g. pulmonary edema) |
|
|
|
propofol (Diprivan ®)
|
CLASS General anesthetic MOA Sedative-hypnotic agent that is suspected to produce effects by the passivemodulation of the inhibitory function of the neurotransmitter gamma aminobutyricacid (GABA) through the ligand-gated GABA receptors INDICATION Intensive care unit (ICU) sedation of intubated mechanically ventilated adult patients |
|
|
|
ranitidine (Zantac®)
|
CLASS Antiulcer M O A• Competitively inhibits action of histamine at the H2 receptor sites of parietalcells • Decreases gastric acid secretions INDICATIONS • Infusion monitoring during interfacility transport only • Short-term maintenance therapy for treatment of a duodenal ulcer • Pathological hypersecretory condition |
|
|
|
tirofiban (Aggrastat®)
|
CLASSES • Antiplatelet • Platelet aggregation inhibitor M O A• Reversibly binds with Glycoprotein (GP) IIb/IIIa receptors on the surface ofplatelets inhibiting the final common pathway for platelet aggregation • GP IIb/IIIa receptor blockade interferes with the binding of fibrinogen, vonWillebrand factors, and other platelet aggregation modulators to the surface ofplatelets, thus preventing aggregation INDICATIONS • Infusion monitoring during interfacility transport only • Adjunctive to or in preparation of percutaneous transluminal coronary arteryangioplasty (PTCA) for the prevention and treatment of acute coronarysyndrome and associated acute cardiac ischemic complications in patients atrisk for abrupt closure of the treated coronary vessel • Heparin should be concurrently administered and monitored |
|
|
|
total parenteral nutrition (TPN) Kabiven®• Procalamine®• Perikabiven®
|
CLASS Intravenous hyperalimentation M O A Parenteral nutrition is the feeding of specialist nutritional products to a patientintravenously, bypassing the usual process of eating and digestion. The patientreceives highly complex nutritional formulae that contain nutrients such as salts,glucose, amino acids, lipids and added vitamins and dietary minerals. INDICATIONS • Patients with long-term need for intravenous feeding who cannot receivenutrients adequate enough to meet physiologic needs through the GI system• Conditions include Hypercatabolic states (burns, trauma, sepsis, etc.) Various gastrointestinal diseases Renal failure Pancreatitis |
|

