![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
100 Cards in this Set
- Front
- Back
|
The bacterial enzymes that inactivate penicillins and cephalosporins are?
a) mef efflux proteins b) DNA gyrases c) erm methylases d) Beta lactamases e) Topoisomerases |

Beta-lactamases
|
|
|
Among the enzymes responsible for synthesizing bacterial cell walls are?
a) Transpeptidases and carboxypeptidases b) Ligases c) Phospholipases d) Esterases e) Methyl formylases |
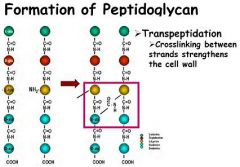
Transpeptidases and carboxypeptidases
|
|
|
Imipenen is a unique Beta-lactam because it?
a) has a very short half life b) serves to inactivate both penicillin binding proteins and beta-lactamases c) Acts on aminoglycoside transferases d) Interferes with DNA segregation e) Inhibits DNA gyrase, in addition to inhibiting beta-lactamase activity |
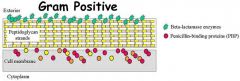
Serves to inactivate both penicillin binding proteins and beta-lactamases
|
|
|
A know side effect of tetracyclines is that they
a) Stain the enamel of teeth b) Causes nail discoloration c) Interferes with mental functions by inhibiting GABA transmission d) Causes heart arrhythmias e) Promote constipation |
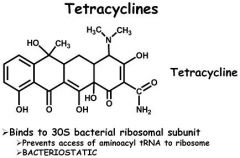
Stain the enamel of teeth
|
|
|
While in general quinolones are safe antibiotics, a recognized side effect is?
a) Prolongation of the QT interval in the heart b) tinnitus c) ataxia d) incontinence e) constipation |
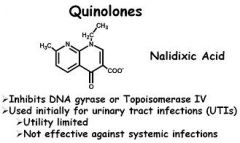
Prolonged QT interval of the heart
|
|
|
Pill dysphagia is seen with
a) tetracycline b) nitrofurantoin c) trimethoprim d) erythomycin e) sulfamethoxazole |
Tetracycline
|
|

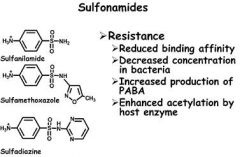
Interference with folate synthesis in seen with
a) clindamycin b) tetracycline c) chloramphenicol d) sulfamethoxazole |
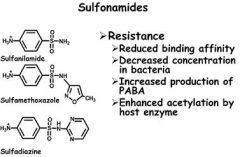
Sulfamethoxazole
|
|
|
Which of the following antibiotic classes interfere with bacterial protein synthesis?
a) Metronidazole b) Quinolones c) Penicillin d) Macrolides |
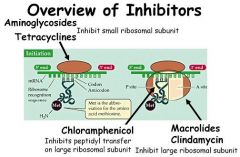
Macrolides
|
|
|
The most likely antibiotic to cause prolongation of the prothrombin time when patients are taking coumadin are
a) tetracycline b) chloramphenicol c) trimethoprim d) rifampin |

rifampin
|
|
|
Which of the following drugs is NOT used to treat Mycobacterium tuberculosis?
a) Isoniazid b) Rifampin c) Ethambutol d) Streptomycin e) Quinolones |

Quinolones
|
|
|
A known side effect of isoniazid is
a) tinnitus b) arthralgias c) hepatitis d) peripheral neuropathy e) Parkinson;s syndrome/disease |

Hepatits
|
|
|
Which of the following drugs should NOT be used to treat influenza in the first 36 hours?
a) Amantadine b) Rimantadine c) Erythromycin d) Zanamivir (Relenza) |
Erythromycin
|
|
|
All of the following are drugs used to treat HIV infections EXCEPT
a) AZT b) DDI c) 3TC d) Amantadine |
Amantadine
|
|
|
Which of the following drugs has NO antiinflammatory properties?
a) Aspirin b) Rofecoxib (Vioxx) c) Ibuprofen d) Acetaminophen e) Cortisol/Prednisone |
Acetaminophen
|
|
|
Prophylactic use of trimethoprim-sulfamethoxazole in HIV protects against
a) Pneumocystis carinii pneumonia b) Pneumococcal pneumonia c) influenza d) Respiratory syncytial virus pneumonia |
Pneumocystis carinii pneumonia
|
|
|
The mechanism of action of AZT is best described by which of the following?
A.Molecular rearrangements within DNA B.DNA translocation C.DNA inversion D.DNA chain termination |
DNA chain termination
|
|
|
Which of the following is the drug of first choice in treating trigeminal neuralgia?
A.Phenobarbital B.Buspirone C.Disulfiram D.Carbamazepine E.Naltrexone |
Carbamazepine
|
|
|
The following receptors are all ligand-gated ion channels EXCEPT
A.GABAA receptor. B.dopamine D2 receptor. C.nicotinic acetylcholine receptor. D.5HT3 receptor. E.NMDA (Glutamate receptor). |
Dopamine D2 receptor
|
|
|
Bacteria can rapidly evolve to develop resistance to antibiotics by all of the following mechanisms EXCEPT
A.inactivation of enzymes that metabolize antibiotics. B.altering the structure of the target of the antibiotic. C.expressing efflux pumps for the antibiotic. D.altering porin channels. E.secretion of antitoxins. |
Inactivation of enzymes that metabolize antibiotics
|
|
|
Which of the following drugs is contraindicated in women of child-bearing age?
A.Aspirin B.Prednisone C.Misoprostol D.Ibuprofen E.Acetaminophen |
Misoprostol
|
|
|
A patient who has been taking large quantities of aspirin might show increased postoperative bleeding because aspirin inhibits
A.synthesis of thromboxane and prevents platelet aggregation. B.synthesis of prostacyclin and prevents platelet disaggregation. C.synthesis of prostaglandin and prevents production of blood platelets. D.thrombin and prevents formation of the fibrin network. E.intestinal absorption of vitamin K and prevents synthesis of blood clotting factors. |
Synthesis of thromboxane and prevent platelet aggregation
|
|
|
Which of the following pharmacologic actions is NOT produced by prostaglandins?
A.Pyrexia B.Uterine contraction C.Decreased gastric acid secretion D.Increased renal vasoconstriction E.Decreased sensitivity to pain |
Increased renal vasoconstriction
(I think this might be wrong) |
|
|
All of the following agents useful for treatment of rheumatoid arthritis can be used simultaneously with anakinra EXCEPT
A.aspirin. B.celecoxib (Celebrex). C.infliximab (Etanercept). D.methotrexate. E.prednisone. |
Infliximab (Etanercept)
|
|
|
The most prominent acute toxic effect associated with acetaminophen use is
A.hemorrhage. B.renal nephropathy. C.hepatic necrosis. D.gastric ulceration. E.respiratory alkalosis. |
Hepatic Necrosis
|
|
|
Tetracycline antibiotics are considered “broad-spectrum” antibiotics because they are effective against all of the following EXCEPT
A.most Gram-positive bacteria growing aerobically B.most Gram-negative bacteria growing anaerobically C.mycobacteria D.fungal pathogens |
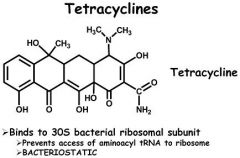
Fungal Pathogens
|
|
|
All of the following statements concerning cephalosporins are correct EXCEPT
A.they are effective inhibitors of cell wall synthesis. B.most oral anaerobic bacteria are insensitive to cephalosporins. C.they contain a modified beta-lactam ring. D.they are related to penicillins. |
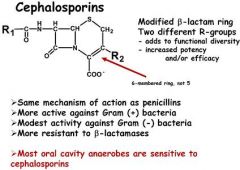
Most oral anaerbic bacteria are insensitive to cephalosporins
|
|
|
Which of the following classes of antibiotics can cause ototoxicity at high doses?
A.Tetracyclines B.Vancomycin C.Aminoglycosides D.Penicillins E.Erythromycin |

Aminoglycosides
|
|
|
All of the following statements concerning prostanoid synthesis via the COX-1 isoform of cyclooxygenase are correct EXCEPT
A.COX-1 expression is constitutive. B.arachidonic acid is the primary substrate of COX-1. C.COX-1 is expressed primarily in macrophages, monocytes and the vascular endothelium. D.the downstream prostanoid synthases are soluble cytosolic enzymes. E.aspirin and ibuprofen selectivity inhibit COX-1 versus COX-2. |
COX-1 is expressed primarily in macrophages, monocytes and the vascular endothelium
|
|
|
Compared to local anesthesia, general anesthesia has all of the following advantages EXCEPT
A.amnesia regarding the surgery/trauma. B.cardiovascular toxicity is more easily avoided. C.patient cooperation is not completely essential. D.the patient is unconscious. E.titration of the level of anesthesia is easier. |

Cardiovascular toxicity is more easily avoided
|
|
|
For volatile anesthetics, the rapidity of onset of anesthesia is determined primarily by
A.lipid solubility. B.metabolism by blood pseudocholinesterases. C.solubility in muscle. D.the blood:gas partition coefficient. E.the rate of liver metabolism |
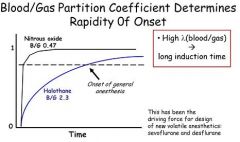
The blood:gas partition coefficient
|
|
|
All of the following are potential adverse effects of general anesthetics EXCEPT
A.coma. B.fulminant hepatic necrosis with halothane. C.malignant hyperthermia. D.peripheral pain sensitization with volatile anesthetics. E.pneumothorax with nitrous oxide. |

Peripheral paine sensitization with volatile anesthetics
|
|
|
Compared to most other parenteral anesthetics, midazolam has the desirable property of producing
A.a block of peripheral pain sensitization. B.amnesia. C.analgesia. D.decreased salivation. E.lack of hallucination upon recovery. |

Amnesia
|
|
|
Symptoms of hyperthyroidism include all of the following EXCEPT
A.muscle wasting. B.nervousness. C.poor cold resistance. D.tachycardia. E.tremor. |
Poor cold resistance
|
|
|
A certain pharmacology professor has a root canal performed by student dentists. To alleviate the extreme pain caused by the prolonged daylong procedure, he washes down 25 tablets of Tylenol™ with half a bottle of Johnny Walker Black Label. Which organ or tissue will most likely be adversely affected by the acetaminophen?
A.Brain B.Gums C.Kidney D.Liver E.Teeth |
Liver
|
|
|
Analgesic agents are primarily distinguished from anesthetic agents in that:
A.Analgesics are administered orally and anesthetics by intravenous injection. B.Analgesics are more selective for inhibition of the sensation of pain, relative to other sensory modalities. C.Analgesics have a lower therapeutic index than anesthetics. D.Analgesics primarily act directly at synapses in the spinal cord, whereas anesthetics act in the brain. E.Anesthetics are more selective for inhibition of Adelta and C fibers than analgesics. |
Analgesics are more selective for inhibition of the sensation of pain, relative to other sensory modalities
|
|
|
Which of the following drugs is directed against a target in fungal cell walls?
A. Amphotericin B B. Caspofungin C. Flucytosine D. Trimethoprim-sulfamethoxazole E. Voriconazole |

Caspofungin
|
|
|
Which of the following drugs should always be administered in addition to a second antifungal agent?
A. Amphotericin B B. Caspofungin C. Flucytosine D. Trimethoprim-sulfamethoxazole E. Voriconazole |

Flucytosine
|
|
|
Which of the following antifungal drugs at a therapeutic dose is most likely to cause abnormal vision, skin rashes and intrahepatic cholestasis?
A. Amphotericin B B. Caspofungin C. Fluconazole D. Itraconazole E. Voriconazole |

Voriconazole
|
|
|
Which of the following is most effective in treating infections with Pneumocystis carinii?
A. Amphotericin B B. Caspofungin C. Flucytosine D. Trimethoprim-sulfamethoxazole E. Voriconazole |
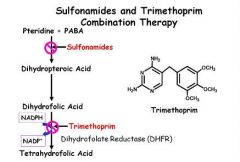
Trimethoprim-Sulfamethoxazole
|
|
|
Which of the following causes the most interactions with drugs metabolized by cytochromes P450 3A4?
A. Amphotericin B B. Caspofungin C. Itraconazole D. Trimethoprim-sulfamethoxazole E. Voriconazole |

Itraconazole
|
|
|
Antifungal triazoles work by
A. binding to ergosterol in fungal membranes. B. inhibiting a fungal cytochrome P450. C. inhibiting cytosolic ergosterol biosynthesis. D. inhibiting fungal cell wall biosynthesis. E. interfering with fungal DNA biosynthesis. |
Inhibiting fungal cytochrome P450
|
|
|
A known side effect of tetracyclines is that it
A. causes nail discoloration. B. causes prolongation of the QT interval. C. interferes with mental functions by inhibiting GABA transmission. D. stains the enamel of teeth. |
Stains the enamel of teeth
|
|
|
Which of the following agents is an opiod antitussive with minimal problems of dependence or addiction?
A. Codeine B. Dextromethorphan C. Guaifenesin D. Hydrocodone E. Oxycodone |
Dextromorphan
|
|
|
All of the following terms have a distinct medical meaning or definition EXCEPT
A. opioid. B. opiate. C. dependence. D. addiction. E. narcotic. |
Narcotic
|
|
|
All of the following effects can be produced by administration of an opioid EXCEPT
A.suppression of cough reflex. B.elevation of mood. C.constriction of pupils. D.inhibition of vomiting. E.stimulation of release of histamine from mast cells. |

Inhibition of vomiting
|
|
|
Which of the following agents is LEAST likely to produce either physical dependence or addiction?
A.Codeine B.Morphine C.Oxycodone D.Hydrocodone E.Tramadol |

Tramadol
|
|
|
Local anesthetics produce anesthesia primarily through phasic (or frequency-dependent) blockade of
A. Mg2+ channels. B. Na+ channels. C. K+ channels. D. Ca2+ channels. E. Cl- channels. |
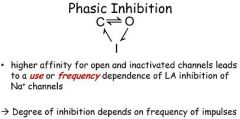
Na+ Channels
|
|
|
All of the following agents can bind to and inactivate Na+ channels EXCEPT
A.local anesthetics. B.general anesthetics. C.dihydropyridine class Ca2+ channel antagonists. D.frog toxins. E.beta-adrenergic antagonists. |
beta-adrenergic antagonists
|
|
|
All of the following agents or conditions can affect local anesthetic potency and/or efficacy EXCEPT
A. vasoconstrictors. B. alkalinization of blood or tissue. C. pregnancy. D. site of injection. E. protein binding. |

Protein Binding
|
|
|
All of the following are signs of CNS toxicity from local anesthetics EXCEPT
A. vertigo. B. flushing (of the skin). C. tinnitus. D. circum-oral numbness. E. garrulousness. |

Flushing of the Skin
|
|
|
Compared to local anesthesia, general anesthesia has all of the following advantages EXCEPT
A.patient cooperation is not completely essential. B.the patient is unconscious. C.amnesia regarding the surgery/trauma. D.titration of the level of anesthesia is easier. E.cardiovascular toxicity is more easily avoided. |

Cardiovascular toxicity is more easily avoided
|
|
|
For volatile anesthetics, the rapidity of onset of anesthesia is determined primarily by
A.lipid solubility. B.the rate of liver metabolism. C.the blood:gas partition coefficient. D.solubility in muscle. E.metabolism by blood pseudocholinesterases |
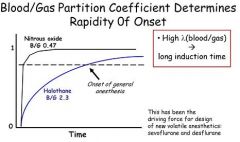
The blood:gas partition coefficient
|
|
|
All of the following are potential adverse effects of general anesthetics EXCEPT
A.pneumothorax with nitrous oxide. B.malignant hyperthermia. C.fulminant hepatic necrosis with halothane. D.coma. E.peripheral pain sensitization with volatile anesthetics. |

Peripheral pain sensitization with volatile anesthetics
|
|
|
Compared to most other parenteral anesthetics, midazolam has the desirable property of producing
A.loss of consciousness. B.analgesia. C.decreased salivation. D.amnesia. E.lack of hallucination upon recovery. |

Amnesia
|
|
|
Which of the following drugs is highly likely to cause skin rash and allergic reactions when applied topically?
A. Antibiotic ointments B. Benzocaine C. Lubriderm D. Selenium sulfide E. Hydrocortisone |

Benzocaine
|
|
|
Which of the following drugs or groups of drugs are responsible for the most accidental overdoses?
A. Heroin and similar “narcotics” B. Alcohol C. OTC drugs such as analgesics and antihistamines D. OTC vitamins |
OTC drugs such as analgesics and antihistamines
|
|
|
All of the following bind to opioid receptors EXCEPT
A. endorphins. B. enkephalins. C. naloxone. D. triptans. E. dynorphins. |

Triptans
|
|
|
If a patient takes 25 tablets of tylenol and washes it down with a bottle of johnny walker, which of the following should be administered as a antidote?
a) N-acetycysteine b) Naloxone c) Morphine d) Ethanol e) Pralidoxime |
N-acetycysteine
Actually I think this is Naloxone |
|
|
The bacterial enzymes that inactivate penicillins and cephalosporins are?
a) beta lactamases b) DNA gyrases c) erm methylases d) mef efflux proteins |
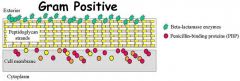
beta lactamases
|
|
|
Among the enzymes responsible for synthesizing bacterial cell walls are?
a) transpeptidases and carboxypeptidases b) ligases c) esterases d) methyl formylases |
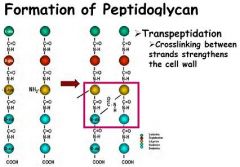
Transpeptidases and carboxypeptidases
|
|
|
Imipenem is a unique beta lactam because it?
a) has a very short half life b) serves to inactivated penicillins binding proteins and beta lactamases c) acts on aminoglycoside transferases d) interferes with DNA segregation |
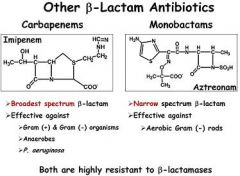
Serves to inactivate penicillins binding proteins and beta lactamases
|
|
|
A known side effect of tetracyclines is that it?
|
stains the enamel of teeth
(y'all better know this one by now!!) |
|
|
While in general quinolones are safe antibiotics, a recognized side effect is?
a) prolongation of the QT interval b) tinnitus c) ataxia d) incontinence |

Prolongation of the QT interval
|
|
|
Pill dysphagia is seen with
a) tetracycline b) nitrofurantoin c) trimethoprim d) sulfamethoxazole |
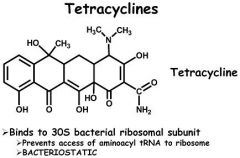
Tetracycline
|
|
|
Interferance with folate synthesis is seen with?
a) clindamycin b) tetracycline c) chloramphenicol d) sulfamethoxazole |

Sulfamethoxazole
|
|
|
Which of the following antibiotics interfere with bacterial protein synthesis?
a) metronidazole b) quinolones c) penicillin d) macrolides |

Macrolides
|
|
|
The most likely antibiotic to cause prolongation of the prothrombin time when patients are taking coumadin are?
a) tetracycline b) chloramphenicol c) trimethoprim d) rifampin |

Rifampin
|
|

Which of the following drugs is NOT used to treat Mycobacterium tuberculosis?
a) Isoniazid b) Rifampin c) Ethambutol d) Streptomycin e) Chloramphenicol |

Chloramphenicol
|
|
|
A known side effect of isoniazid is?
a) Tinnitus b) Arthralgias c) Hepatitis d) Peripheral Neuropathy |

Hepatitis
|
|
|
Which of the following drugs should NOT be used to treat influenza in the first 36 hours?
a) Amantadine b) Rimantadine c) Erythromycin d) Relenza |

Erythromycin
|
|
|
All of the following are drugs used to treat HIV infection EXCEPT
a) AZT b) DDI c) 3TC d) amantadine |
amantadine
|
|
|
The cell count of which cell type is an important predictor of opportunistic infections in patients with HIV?
|
CD4+ Lypmhocytes
|
|
|
Bacteria can rapidly evolve to develop resistance to antibiotics by all of the following mechanisms EXCEPT
a) Inactivation of enzymes that metabolize antibiotics b) Altering (mutating) the target of the antibiotic c) Expressing efflux pumps for the antibiotic d) Altering expression of porin channels e) Secretion of antitoxins |
Inactivation of enzymes that metabolize antibiotics
|
|
|
Which of the following drugs is directed against a target in fungal cell walls?
a) Amphotericin A b) Trimethoprim-sulfamethoxazole c) Flucytosine d) Caspofungin e) Voriconazole |

Caspofungin
|
|

Which of the following drugs should always be administered with another antifungal agent?
a) Amphotericin A b) Trmethoprim-sulfamethoxazole c) Flucytosine d) Caspofungin e) Voriconazole |

Caspofungin
(think that this is actually Flucytosine) |
|

All of the following antigungal agents have some efficacy against Aspergillus spp. EXCEPT
a) Amphotericin A b) Fluconazole c) Voriconazole d) Itraconazole e) Caspofungin |

Fluconazole
|
|
|
Antacids should NOT be given to patients taking which of the following antifungal drugs?
a) Amphotericin A b) Fluconazole c) Voriconazole d) Itraconazole e) Caspofungin |
Itraconazole
|
|
|
Tetracycline antibiotics are considered "broad-spectrum" antibiotics because they are effective against all of the following EXCEPT
a) Most gram positive bacteria growing aerobically b) Most gram negative bacteria growing anaerobically c) Mycobacteria d) Fungal pathogens |
Fungal pathogens
|
|
|
Cephalosporins exert their bacteriocidal effects at the
a) ribosome b) cell nucleus c) cell membrane d) cell wall |
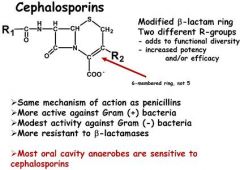
Cell wall
|
|
|
Which of the following classes of antibiotics can cause ototoxicity at high doses?
a) Tetracycline b) Vancomycin c) Aminoglycosides d) Penicillins e) Erythromycin |

Aminoglycosides
|
|

Which of the following statements concerning cephalosporins is incorrect?
a) They are effective inhibitors of cell wall synthesis b) Most oral anaerobic bacteria are insensitive to cephalosporins c) They contain a modified beta lactam rind d) they are related to penicillins |
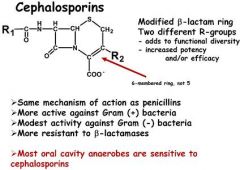
Most oral anaerobic bacteria are insensitive to cephalosporins
|
|
|
Fungi come in a variety of flavors. All of the following statements about fungi are correct EXCEPT
a) Yeasts are fungi that are usually round and smooth b) Molds are fungi that form hyphae as part of their life cycle c) Among the groups of fungi, dermatophytes belong the molds d) Dimorphic fungi are rounded when infecting tissues but form hyphae when in culture e) Candida spp are examples of molds |
Candida spp. are examples of molds
|
|
|
All of the following are correct statements about cells EXCEPT
a) bacteria have no nucleus b) you and I have 46 chromosomes (we hope) c) Bacteria cannot grow in the absence of oxygen d) Most but not all bacteria have a single chromosome e) Bacteria can grow in deep sea vents at temperatures of 90 deg C under >200 atmospheres of pressure |
Bacteria cannot grow in the absence of oxygen
|
|
|
Which of the following drugs are an effective antitussive?
a) Ibuprofen b) Dextromethorphan c) Guaifenesin d) Aspirin e) Acetaminophen |
Dextromethorphan
|
|

Receptors which mediate the primary effects of opioids are?
a) Presynaptic transporters of amines b) Membrane proteins activated by endogenous peptides c) Enzymes which convert arachidonic acid to prostaglandins d) NMDA and glutamate receptors e) Present in the brain but not the spinal cord |

Membrane proteins activated by endogenous peptides
|
|
|
All of the following bind to opioid receptors EXCEPT
a) Endorphins b) Enkephalins c) Naloxone d) Substance P e) dynorphins |

Substance P
|
|
|
All of the following effects are commonly produced by administration of an opioid EXCEPT
a) respiratory depression b) nausea c) constipation d) tolerance e) smooth muscle relaxation |

Smooth muscle relaxation
|
|
|
Which of the following agents sensitizes peripheral nerve endings to noxious and/or painful stimuli?
a) Bradykinin b) Serotonin c) Histamine (itching) d) H+ (acid) e) Prostaglandins |
Prostaglandins
|
|
|
All of the following effects can be produced by administration of an opioid EXCEPT
a) Suppresion of the cough reflex (antitussive) b) Elevation of mood c) Constriction of pupils d) Inhibition of vomiting (antiemetic) e) Stimulation of release of histamine from mast cells |
Inhibition of vomiting (antiemetic)
|
|
|
Which of the following agents is LEAST likely to produce either physical dependence or addiction?"
a) Codeine b) Morphine c) Oxycodone d) Hydrocodone e) Tramadol |
Tramadol
|
|

All of the following statements regarding local anesthetics are correct EXCEPT
a) Amide class local anesthetics are more stable in solution than those of the ester class b) Ester class local anesthetics have a high risk of allergic reactions especially when applied topically c) Both classes act by blocking Ca++ channels d) Ester class local anesthetics are metabolized predominately by pseudocholinesterases e) Amide class local anesthetics are metabolized by liver cytochrome P450 enzymes |

Both classes act by blocking Ca++ channels
|
|
|
Local anesthetics produce anesthesia primarily through phasic (or frequency-dependent) blockade of
a) Mg++ channels b) Na+ channels c) K+ channels d) Ca++ channels e) Chloride channels |
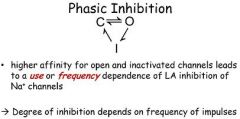
Na+ channels
|
|
|
All of the following agents can bind to and inactivate Na+ channels EXCEPT
a) Local anesthetics b) general anesthetics c) Dihydropyridine class Ca++ channel antagonists d) Frog toxins e) Beta adrenergic antagonists |
Dihydropyridine class Ca++ channel antagonists
|
|
|
All of the following agents or conditions can affect local anesthetic potency and/or efficacy EXCEPT
a) Vasoconstrictors b) Alkalinization of blood or tissue pregnancy c) Site of injection d) Pregnancy e) Protein binding |

Protein binding
|
|
|
All of the following are signs of CNS toxicity from local anesthetics EXCEPT
a) Vertigo b) Flushing (of the skin) c) Tinnitus d) Circum-oral numbness e) Garrulousness |

Flushing of the skin
|
|
|
Compared to local anesthesia, general anesthesia has all of the following advantages EXCEPT
a) Patient cooperation is not completely essential b) The patient is unconscious c) The patient has amnesia regarding the surgery/trauma d) Titration of the level of anesthesia e) Cardiovascular toxicity is more easily avoided |
Cardiovascular toxicity is more easily avoided
|
|
|
All of the following are potential adverse effects of general anesthetics EXCEPT
a) Pneumothorax with nitrous oxide b) Malignant hyperthermia c) Fulminant hepatic necrosis with halothane d) Coma e) Peripheral pain sensitization with volatile anesthetics |
Peripheral pain sensitization with volatile anesthetics
|
|

Compared to most other agents used parenterally, midazolam has the desirable property of producing
a) loss of consciousness b) analgesia c) decreased salivation d) amnesia e) lack of hallucination upon recovery |

Amnesia
|
|
|
Patient sprayed in the face with pesticide. In the ER, he exhibited tachycardia, lachrymation, increased salivation, and increased anxiety. Which of the following is most likely to be an effective antidote?
a) N-acetycysteine b) Naloxone c) Morphine d) Ethanol e) Pralidoxime |

Naloxone
|
|
|
Patient took 25 tablets of tylenol washed down with a half bottle of Whiskey. Which of the following agents should be administered as an antidote?
a) N-acetycysteine b) Naloxone c) Morphine d) Ethanol e) Pralidoxime |
N-acetycysteine
|

