![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
132 Cards in this Set
- Front
- Back
|
What are the subdivisions of the respiratory system?
|
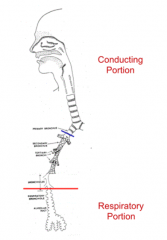
- Conducting portion
- Respiratory portion |
|
|
What is the function of the conducting portion of the respiratory system?
|
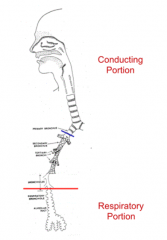
- Conditions air
- Transports air to more distal respiratory passages |
|
|
What is the characteristic structure in the respiratory portion of the respiratory system?
|
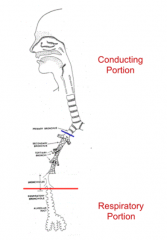
Alveoli - thin-walled structures where gas exchange occurs between inhaled air and blood
|
|
|
Clinically, how is the respiratory system divided? Why?
|
- Upper Respiratory Tract
- Lower Respiratory Tract - Based on infectious conditions |
|
|
What are the sites of upper respiratory infections?
|
- Nasal
- Oral - Middle ear cavities - Paranasal sinuses - Pharynx |
|
|
What are the sites of lower respiratory infections?
|
- Larynx
- Trachea - Lungs |
|
|
What are the primary functions of the respiratory system?
|
- Air conduction
- Gas exchange |
|
|
What happens during air conduction?
|
- Air conditioning: humidification and warming of air
- Removal of foreign substances |
|
|
What happens during gas exchange?
|
- Occurs in alveoli
- Exhaled air flows in reverse |
|
|
What are the secondary functions of the respiratory system?
|
- Modulation or production of chemical messengers (angiotensin I to angiotensin II)
- Speech sound production - Regulation of acid base balance (in cooperation w/ kidneys) |
|
|
What is the term for the conducting passages located externally to the lungs?
|
Extrapulmonary passages
|
|
|
What is the term for the conducting passages located within the lungs?
|
Intrapulmonary passages
|
|
|
What lines the air conducting passages? Why is this important?
|
- Mucosa - contains lymphatic tissue and other defense related cells
- Important because they communicate with the external environment |
|
|
What are the extrapulmonary passage structures?
|
Conducting passages external to the lung
- Nasal cavities - Paranasal sinuses - Nasopharynx - Oropharynx - Larynx - Trachea |
|
|
What happens in the nasal cavities?
|
- Air is warmed, moistened, and filtered
- Olfaction - detection of odorant molecules |
|
|
Through what does air enter the nasal cavities? What lines this structure?
|
Nasal Vestibules - lined w/ stratified squamous keratinized epithelium which contains stiff hairs called Vibrissae
|
|
|
What kind of epithelium lines the nasal vestibules?
|
Stratified squamous keratinized epithelium
|
|
|
What is the term for the stiff hairs in the nasal vestibule?
|
Vibrissae
|
|
|
What kind of epithelium lines the nasal cavities? What kind of cells are in here?
|
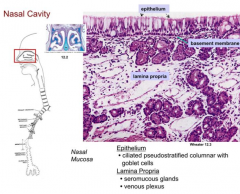
Pseudostratified ciliated columnar epithelium containing goblet cells = Respiratory Epithelium
|
|
|
What is the configuration of the Respiratory Epithelium?
|
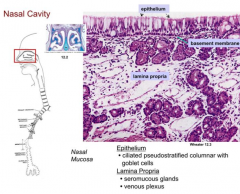
Pseudostratified ciliated columnar epithelium containing goblet cells
|
|
|
What covers the apical surface of the Respiratory Epithelium? Function?
|
- Bilayer of mucus (external) and serous fluid (internal)
- Traps particulates in the air in the external layer of mucus (smoking and other irritants can reduce the effectiveness of this function) |
|
|
What moves the mucus layer on the apical surface of the Respiratory Epithelium?
|
The underlying serous fluid transports the mucus
|
|
|
What moves the serous layer on the apical surface of the Respiratory Epithelium?
|
Moves by beating of cilia embedded within it
|
|
|
What ultimately happens to the mucus on the apical surface of the Respiratory Epithelium?
|
Either swallowed or expectorated (ejected by coughing) through the oral cavity
|
|
|
What is the term for the ciliary driven mucous cleaner?
|
Mucociliary Escalator
|
|
|
What is in the underlying lamina propria of the nasal vestibule?
|
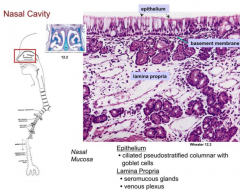
- Seromucous glands
- Extensive vascular plexus |
|
|
What is the function of the extensive vascular plexus within the underlying lamina propria?
|
Blood passing through warms the inspired air
|
|
|
What is responsible for warming the inspired air?
|
Blood passing through the extensive vascular plexus within the underlying lamina propria
|
|
|
What is the nasal cavity mucosa attached to?
|
Firmly attached to the underlying periosteum by collagen fibers within the lamina propria
|
|
|
What kind of mucosa is located in the superior portion of the nasal cavity? What kind of epithelium is it covered by?
|
Olfactory Mucosa - covered by Olfactory Epithelium
|
|
|
What kind of epithelium is the Olfactory Epithelium?
|
Pseudostratified columnar epithelium containing Olfactory Cells
|
|
|
What kind of cells are Olfactory Cells? Function?
|
- Bipolar neurons that have an axon at their base and a knob-like olfactory vesicle at apex containing primary cilia
- Detects odors |
|
|
What kind of cells are in the Olfactory Epithelium?
|
- Olfactory Cells
- Supporting, basal (stem) and brush cells |
|
|
What is in the lamina propria of the olfactory mucosa?
|
- Axon bundles
- Serous Olfactory Glands |
|
|
What is produced by the olfactory glands? Function?
|
- Fluid containing odorant binding protein
- Binds to odorants and together they bind to Odorant Receptors on cilia of olfactory cells |
|
|
What happens when an odorant binds to the odorant receptors?
|
- Binding activates gated Na+ channel
- Causes ion influx that generates an AP |
|
|
What color is the olfactory mucosa? Why?
|
- Yellow-brown
- Pigment contained in epithelium and glands |
|
|
What lines the paranasal sinuses?
|
Thinner version of respiratory mucosa (pseudostratified ciliated columnar epithelium)
|
|
|
What lines the nasopharynx?
|
- Respiratory mucosa (pseudostratified ciliated columnar epithelium)
- Stratified squamous non-keratinized |
|
|
Where is the lymphatic tissue in the nasopharynx?
|
- Abundant in lamina propria
- Accumulates superiorly as Pharyngeal Tonsil = Adenoids |
|
|
What are the Adenoids?
|
Pharyngeal Tonsils = lymphatic tissue that accumulates superiorly in nasopharynx
|
|
|
What does the mucosa of the nasopharynx adhere to?
|
Nasopharynx
|
|
|
When does the larynx close the airway?
|
During swallowing and while producing speech sounds
|
|
|
What supports the laryngeal passageway?
|
- Hyaline cartilage
- Elastic cartilage - Connected by ligaments - Moved by skeletal muscles |
|
|
What lines the larynx?
|
Respiratory mucosa (pseudostratified ciliated columnar epithelium)
|
|
|
What covers the epiglottis and the vocal fold?
|
Stratified squamous non-keratinized
|
|
|
What are the characteristics of the superficial layer of the vocal fold?
|
Lamina Propria is poorly vascularized, lacks lymphatic vessels, and has few elastic fibers
|
|
|
What is Reinke's Space?
|
Potential space between the vocal ligament and the overlying mucosa that can collect fluid
|
|
|
What is the function of Reinke's Space?
|
Facilitates vocal cord vibration
|
|
|
What happens if Reinke's Space collects fluid?
|
Hoarseness during chronic inflammation of vocal cords
|
|
|
What are the characteristics of the vocal fold core?
|
- Stiff
- Consists of remaining lamina propria - Vocal ligament and vocalis muscle |
|
|
What kind of cells are unusually abundant in the larynx lamina propria?
|
Mast cells
|
|
|
What happens in Croup?
|
Inflammation of the mucosa in the larynx (laryngitis), trachea, and bronchi
|
|
|
What are the layers in the wall of the trachea?
|
1. Mucosa
2. Submucosa 3. Cartilage 4. Adventitia |
|
|
What kind of epithelium covers the mucosa of the trachea?
|
Respiratory Epithelium (pseudostratified ciliated columnar epithelium)
|
|
|
What are the characteristics of the basement membrane in the trachea?
|
Appears thick d/t expanded reticular layer
|
|
|
What is in the submucosal layer of the trachea?
|
- Loose CT
- Separated from mucosa by elastic membrane - Contains seromucous glands - Contains abundant lymphatic tissue |
|
|
What is the location of the seromucous glands of the trachea?
|
Submucosal layer
|
|
|
Where is the lymphatic tissue in the trachea?
|
Abundant in the lamina propria and the submucosa
|
|
|
What supports the tracheal airway?
|
C-shaped hyaline cartilages
|
|
|
What bridges the free end of the C-shaped hyaline cartilages in the trachea?
|
Smooth muscle and fibroelastic tissue
|
|
|
What are the components of the intrapulmonary passages?
|
- Bronchi (except for initial segment)
- Bronchioles |
|
|
What happens as the passages of the bronchiole branches become smaller in diameter?
|
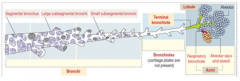
- Organization of wall becomes less complex
- At certain levels, some wall components (cartilage and glands) disappear - Height of epithelium is progressively reduced |
|
|
What are the layers of the wall of the bronchi?
|
- Mucosa
- Muscularis - Submucosa - Cartilage - Adventitia |
|
|
What kind of epithelium covers the bronchial mucosa?
|
Respiratory Epithelium (height is reduced as you get deeper)
|
|
|
What are the characteristics of the muscularis layer of the bronchi? Location?
|
- 2 discontinuous layers of spiraling smooth muscle
- Lies between the lamina propria and the submucosa |
|
|
Where are the seromucous glands of the bronchi?
|
Lamina propria and submucosa
|
|
|
What is unique about the extrapulmonary portion of the primary bronchi?
|
They have C-shaped cartilage rings
|
|
|
What is unique about the intrapulmonary portion of the primary bronchi?
|
There are irregular shaped cartilage plates
|
|
|
What is in the adventitia of the bronchi wall?
|
Moderately dense CT - continuous w/ surrounding lung parenchyma
|
|
|
What is the average diameter of the bronchioles?
|
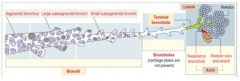
1 mm (5 mm - 0.3 mm)
|
|
|
What do the walls of the bronchioles lack?
|
- Cartilage plates
- Seromucous glands |
|
|
What kind of epithelium covers the mucosa of the bronchioles?
|
Ranges from ciliated simple columnar to simple cuboidal epithelium
|
|
|
What kind of cells can be present within the epithelium over the mucosa of the bronchioles?
|
- Goblet cells occasionally
- Clara cells - columnar cells w/ dome-shaped apex and short microvilli |
|
|
What kind of cells are characteristic of the bronchiole epithelium?
|
Clara cells - columnar cells w/ dome-shaped apex and short microvilli
|
|
|
What do the Clara Cells contain in the bronchioles? Function?
|
- Secretory granules and their product, Clara Cell Protein (CC16/CC10)
- Protects the bronchiolar epithelium via anti-inflammatory action - Also contain abundant smooth ER w/ cytochrome that degrades toxins - May also produce a surfactant-like molecule - Release Cl- via a cGMP regulated ion channel |
|
|
What is external to the lamina propria in the bronchioles?
|
Loose network of smooth muscle oriented in helical configuration
|
|
|
What kind of lymphatic tissue is in the the bronchi and bronchioles? Which layer?
|
BALT - found in mucosa
|
|
|
What are the most distal bronchiole branches called? Average diameter?
|
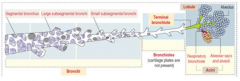
Terminal Bronchioles - 0.5 mm
|
|
|
What is the end of the conducting portion of the lung?
|
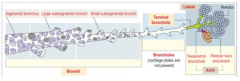
Terminal Bronchioles
|
|
|
What are the clinical conditions affecting intrapulmonary conducting airways?
|
- Chronic Bronchitis
- Asthma - Cystic Fibrosis - Bronchial Carcinoma |
|
|
What causes Chronic Bronchitis? Outcome?
|
- Caused by repeated damage to mucosa
- Hypertrophy and/or hyperplasia of mucous glands and smooth muscle leads to wall thickening |
|
|
What causes Asthma? Outcome?
|
- Hyperresponsiveness of airway triggered by repeated antigen exposure or abnormal autonomic regulation of airway function
- Leads to airway wall inflammation, hypersecretion of thick bronchial mucus, and vasodilation of bronchial microvasculature - Prolonged smooth muscle contraction leads to bronchoconstriction during exhalation |
|
|
What causes Cystic Fibrosis?
|
- Alteration of Cl- ion channel protein (CFTR) on submuocsal gland cell causes defective Cl- transport and increased Na+ absorption --> more viscous mucus that traps bacteria
- Production of a thick mucus by the epithelium causes the airways to be blocked - Thick mucus interferes w/ proper function of mucociliary escalator - Followed by bacterial infections |
|
|
What protein is mutated in Cystic Fibrosis? Location?
|
CFTR = Cystic Fibrosis Transmembrane Conductance Regulator (Cl- ion channel protein)
- Found in submucosal gland cells - Also found in pancrease excorine cells and sweat gland ducts |
|
|
What causes Bronchial Carcinoma?
|
Squamous metaplasia resulting from chronic irritation or from small granule (neuroendocrine) cells in epithelium
|
|
|
What are the components of the respiratory passages?
|
- Respiratory bronchioles
- Alveolar ducts - Alveolar sacs - Alveoli |
|
|
What does a terminal bronchiole branch into?
|
Several Respiratory Bronchioles
|
|
|
What kind of epithelium lines the respiratory bronchioles?
|
Simple cuboidal epithelium, eventually becomes non-ciliated
|
|
|
What kind of cells are found in the respiratory bronchiole epithelium?
|
Clara cells - predominate more in distal portions
|
|
|
What are the out-pouchings of the respiratory bronchiole wall?
|
Alveoli - sites of gas exchange
|
|
|
What structure is found between adjacent alveoli?
|
Small knob-like septum containing:
- Smooth muscle cells - Reticular fibers - Elastic tissue |
|
|
What does the opening to the alveoli contain?
|
Fibers of elastin and type III collagen, but LACK smooth muscle
|
|
|
What surrounds and interconnects the respiratory passages?
|
Network of fine elastic fibers
|
|
|
How many alveoli are there per lung?
|
150-300 million small, thin walled chambers called Alveoli
|
|
|
What kind of epithelium lines alveoli?
|
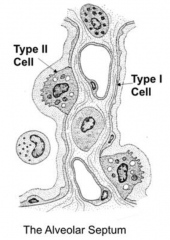
Alveolar Epithelium:
- Squamous type I alveolar cells or Pneumocytes (95% of surface area) - Cuboidal type II alveolar cells or Pneumocytes (5% of surface area) |
|
|
How are Type I Pneumocytes related? What kind of epithelium?
|
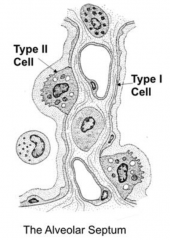
- Connected to adjacent cells by occluding junctions
- Squamous epithelium |
|
|
What is the function of type II Pneumocytes? What kind of epithelium?
|
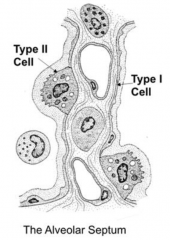
- Produce, reabsorb, and recycle components of pulmonary surfactant
- Cytoplasm contains apical secretory granules called Lamellar Bodies - Cuboidal epithelium |
|
|
What are Lamellar Bodies and where are they found?
|
- Secretory granules for pulmonary surfactant
- Found in cytoplasm on apical side of Type II (cuboidal) alveolar cells / pneumocytes |
|
|
How does the number of Type I (squamous) and Type II (cuboidal) pneumocytes compare? How much alveolar surface area do they take up?
|
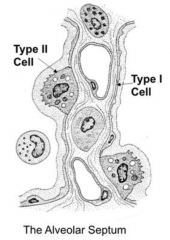
- Equal amounts of type I and II cells (if not more type II)
- Type I cells occupy 95% of alveolar surface area - Type II cells only occupy 5% of alveolar surface area |
|
|
Besides the Type I and II Pneumocytes, what other cells are found in the alveolar epithelium?
|
Brush cells
|
|
|
What does the alveolar septum contain?
|
- Plexus of continuous capillaries surrounded by fibers of elastin and type III collagen
- Macrophages, lymphocytes, mast cells, and fibroblasts |
|
|
What are the openings in the alveolar septum?
|
Alveolar Pores
|
|
|
What kind of cell becomes a "dust cell" in the alveoli? How?
|
- Some macrophages migrate between adjacent Type I cells and enter the alveolar lumen
- Become alveolar macrophages / dust cells |
|
|
What is the function of alveolar macrophages / dust cells?
|
- Phagocytize particulates and bacteria
- Aid type II cells in phagocytosis of surfactant |
|
|
What are the components of the blood-air barrier?
|
- Pulmonary surfactant
- Type I pneumocyte - Fused basement membranes - Capillary endothelial cells |
|
|
What are the components of pulmonary surfactant?
|
Phospholipids:
- Phosphotidylcholine - Phosphotidylglycerol Proteins: - Surfactant Proteins A, B, C, and D Antioxidants |
|
|
What is the organization of the lipids and proteins in pulmonary surfactant?
|
Lipids flot on layer of proteins
|
|
|
What happens following heart failure and pulmonary congestion?
|
- RBCs extravasate into alveoli
- Engulfed by macrophages that stain positively for iron content = Heart Failure Cells |
|
|
What are Heart Failure Cells?
|
- Macrophages that have engulfed the RBCs that have extravasated from the alveoli
- Causes macrophages to stain positively for iron content |
|
|
What are the clinical conditions that affect the respiratory passages?
|
- Emphysema
- Acute Respiratory Distress Syndrome - Interstitial Fibrosis - Infections - Lung Cancer |
|
|
What are the characteristics of Emphysema?
|
- Progressive destruction of alveolar septa
- Leads to enlarged air spaces - Decreased surface area available for gas exchange |
|
|
What happens to the amount of elastic tissue in Emphysema? Why?
|
Decreased elastic tissue d/t inhibition of α1-antitrypsin activity that protects elastic fibers from degradation by proteases
|
|
|
What is the function of α1-antitrypsin?
|
Protects elastic fibers from degradation by proteases in the lung (inhibited in Emphysema)
|
|
|
What parts of the respiratory system are involved in Emphysema?
|
- Just the respiratory bronchiole
- Or all parts of the pulmonary acinus (region of the lung supplied with air from one of the terminal bronchioles) |
|
|
What are the forms of Chronic Obstructive Pulmonary Disease?
|
- Asthma
- Chronic bronchitis - Emphysema |
|
|
What are the characteristics of COPD?
|
Decreased airflow in individuals w/ normal or increased total lung and forced vital capacity combined w/ decreased forced expiratory volume
|
|
|
What happens in Acute Respiratory Distress Syndrome?
|
- Air-blood barrier is compromised by toxins, infectious agents, or trauma
- Fluid leaks from capillaries causing pulmonary edema - Fibrin and cell debris accumulate in alveolar lumen inhibiting surfactant function |
|
|
What causes Acute Respiratory Distress Syndrome? What does this lead to?
|
- Toxins, infectious agents, or trauma compromise the air-blood barrier
- Leads to chronic fibrosis of distal airways |
|
|
What causes Interstitial Fibrosis?
|
Progressive condition involving increased collagen and elastin production by fibroblasts within inter-alveolar septum
|
|
|
What does Interstitial Fibrosis lead to?
|
Accumulation of fibrous CT within septum impededs gas exchange leading to hypoxia
|
|
|
What is Interstitial Fibrosis associated with?
|
Accumulation of inhaled particulates such as silica, coal dust, or asbestos within the septal macrophages
|
|
|
What causes Pneumonia?
|
- Toxins from bacterial and viral infections stimulate an inflammatory reaction in lung resulting in pneumonia
- Fluid accumulates in alveoli and reduces amount of lung parenchyma available for gas exchange |
|
|
What cells can lung cancer originate from?
|
Cells lining the conducting passageways or the distal airways
|
|
|
What is a "mucosa"?
|
Lining membrane of cavities that have a connection to the exterior of the body
|
|
|
What are the functions of a mucosa?
|
- Immunological and physical barrier
- Source of secretory products - Selective absorptive interface |
|
|
What are the components of a mucosa?
|
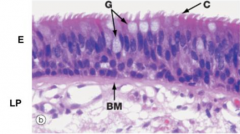
- Epithelium (at surface)
- Lamina Propria (a CT layer that supports the epithelium) |
|
|
In what disease are the cilia of the respiratory epithelium defective?
|
Primary Ciliary Diskinesias (e.g., congenital immotile cilia or Kartagener's syndrome)
|
|
|
What kind of cells are found in Respiratory Epithelium?
|
- Columnar cells
- Goblet cells - Basal cells - Small granule cels - Brush cells |
|
|
What kind of cells are found in Olfactory Epithelium?
|
- Olfactory cells
- Supporting cells - Basal cells - Brush cells |
|
|
What is a pulmonary lobule?
|
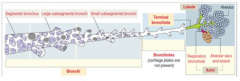
Terminal bronchiole and the lung tissue it supplies
|
|
|
What is a pulmonary acinus?
|
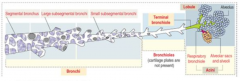
Portion of the lung supplied by a respiratory bronchiole
|

