![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
19 Cards in this Set
- Front
- Back
- 3rd side (hint)
|
Definition of SLE |
A multisystemic autoimmune inflammatory disorder in which autoantibodies to a variety of autoantigens result in the formation and deposition of immune complexes |
|
|
|
Classic presentation of SLE |
Woman of childbearing age presenting with a triad of fever, joint pain and rash |
3 |
|
|
Epidemiology of SLE |
- affects 0.2% of the population - 90% female - child-bearing age - more common in Afro-Carribeans & Asians |
4 |
|
|
Clinical features of SLE |
A relapsing-remitting picture with constitutional features, such as fatigue, weight loss, fever & myalgia A RASH POINts and MD - arthritis: involves peripheral joints, early morning stiffness - Raynaud's/renal: proteinuria, increased BP - ANA: positive in 95% - serositis: pleuritis, pericarditis - haematological: AIHA, decreased WCC & platelets - photosensitivity - oral ulcers - immune phenomenon - neurological: psychoses, seizures - malar rash - discoid rash |
12 |
|
|
Immune phenomenon in SLE |
- anti-double stranded DNA (anti-dsDNA): 60% specificity - anti-smooth muscle (anti-Sm) - anti-phospholipid - extractable nuclear antibodies: positive in 30%, includes anti-Sm, anti-Ro, anti-La & anti-ribonucleoprotein (RNP) |
4 |
|
|
Rashes in SLE |
- malar rash: facial erythema sparing the nasolabial folds - discoid rash: pigmented hyperkeratotic papules that become atrophic depressed lesions |
2 |
|
|
Diagnosis of SLE |
American Rheumatism Association criteria require four of the following: - malar rash - discoid rash - photosensitivity - oral ulcers - arthritis - serositis - renal disorder - neurological features - haematological disorder - immunological features - ANA disorder. |
10x |
|
|
Monitoring disease activity in SLE |
- anti-dsDNA titres - complement: decreased C3 & C4 - increased ESR |
|
|
|
Causes of drug-induced SLE - antibodies |
Will have anti-histone antibodies - procainimide - phenytoin - hydralazine - isoniazid |
4 |
|
|
Maintenance therapy in SLE |
Manage in specialist clinics - joints: NSAIDs, hydroxychloroquine (DMARD) - skin: sunblock, +/- low dose steroids |
3 |
|
|
Severe flares of SLE |
AIHA, lupus nephritis, pericarditis, CNS disease - high dose prednisolone - IV cyclophosphamide - ACE inhibitors: proteinuria from lupus nephritis |
3 |
|
|
Complications of treatment of SLE |
- haemorrhagic cystitis - pneumocystis pneumonia - steroid side effects |
3 |
|
|
Prognosis in SLE |
80% survival at 15yrs |
|
|
|
Antiphospholipid syndrome definition |
An acquired autoimmune disorder that manifests clinically as recurrent thrombosis |
|
|
|
Causes of antiphospholipid syndrome |
- primary: 70% - secondary to SLE: 30% |
2 |
|
|
Immune complexes in antiphospholipid syndrome |
Antiphospholipid antibodies - anti-cardiolipin - lupus anticoagulant |
2 |
|
|
Features of antiphospholipid syndrome |
CLOTs (DVT are venous, stroke is arterial) - coagulation defect: increased aPTT - livedo reticularis - obstetric complications: recurrent 1st trimester abortion - thrombocytopenia |
4 |
|
|
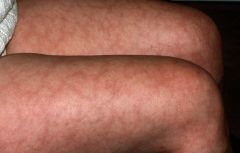
Livedo reticularis |
|
|
|
Treatment of antiphospholipid syndrome |
- low dose aspirin - warfarin: if recurrent thrombosis (INR: 3.5) |
2 |

