![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
21 Cards in this Set
- Front
- Back
|
Define osteoarthritis |
OA is a progressive, degenerative disorder of the joints caused by gradual loss of cartilage, and resulting in the development of bony spurs and cysts at the margins of the joints. |
|
|
What parts of the body are affected by OA? (3) |
Weight-bearing components of joints: bone, articular cartilage and menisci |
|
|
Draw a diagram comparing a normal and osteoarthritic joint (7) |
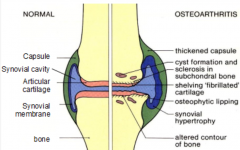
|
|
|
What is the main component of a synovial joint affected by RA? What are the main changes which may occur? |
- articular cartilage - increased swelling - change in colour - cartilage fibrillation - erosion down to subchondral bone |
|
|
What cell type synthesis cartilage? From what stem cells are they derived? What is the main collagen type? |
chondrocytes mesenchymal stem cells type II |
|
|
During OA, the balance of cartilage components is disrupted. Elaborate (4) |
Decrease in; –Water content –Proteoglycan synthesis –Collagen x-linking –Size of Aggrecan, GAG & Hyaluronic acid |
|
|
How prevalent is OA? Who is most affected? What joints are most affected? (4) |
- most common form or arthritis (8 million in UK) - more woman then men and >45 - most common at ends of fingers, thumbs, lower back, knees and hips |
|
|
Give 4 examples of secondary causes of OA |
- trauma - hip dysplasia - infection - DM |
|
|
Give 10 examples of risk factors for OA |
- increasing age - genetics - gender (females) - diet and nutrition (low vitamin C and D) - trauma - obesity - occupation - abnormal joint mechanics - knee extensor weakness - sports |
|
|
Describe the main symptoms of OA (4) |
•Pain, especially when doing load-bearing activities, such aswalking •Short-lived stiffness in the morning, which improves in 30 minutes or less when you start to move •Difficulty moving affected joints or doing certain activities |
|
|
What aspects of a patients clinical history might suggest OA (6) |
- pain - decreased walking distance - sleep disturbance - limp and Trendelenburg sign - stiffness |
|
|
What signs on an X ray might suggest OA? (4) |
- narrowing of joint space - osteophytes - subchondral sclerosis - cyst formation |
|
|
What are the aims of treatment for OA? (4) |
- slow progression - reduce pain - increase range of motion - increase muscle strength |
|
|
List 4 non-operative treatments for OA |
- medications - physiotherapy - walking aids - joint injections |
|
|
List 3 medications that might be administered |
paracetemol (pain) NSAIDs e.g. ibuprofen or diclofenac (pain) glucosamine and chondroitin sulfate |
|
|
List 4 approaches of physiotherapy for OA |
- range of motion exercises - muscle strengthening - aerobic conditioning - weight loss |
|
|
What are the main benefits of using walking aids? |
- transfers load to unaffected side - reduces load by ~40% |
|
|
What joint injections may be used in OA? (2) Describe the benefits of each |
- cortisone/corticosteroids: reduce inflammation and pain more rapidly than NSAIDs - viscous supplements: replace synovial fluid; increases viscosity and elasticity of fluid |
|
|
list potential surgical interventions (3) |
- arthroscopy - cartilage transplantation - joint replacement |
|
|
Describe what can be done by arthroscopy in OA (3) |
(- keyhole surgery) - repair damaged cartilage - remove fragments of loose bone or cartilage - drain away any excess fluid |
|
|
What are the aims of joint replacement? (2) |
- reduce pain - increase range of motion |

