![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
34 Cards in this Set
- Front
- Back
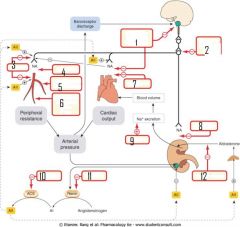
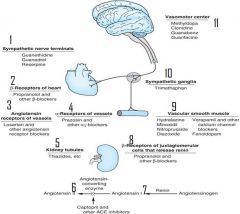
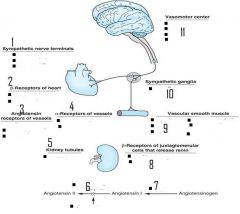
what drugs work at each site?
|
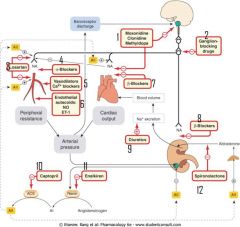
|
|
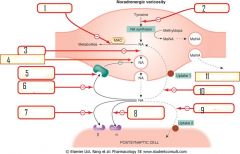
plug in the peripheral adrenergic drugs
|
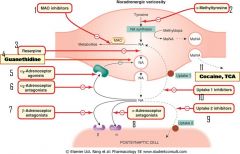
|
|
plug in the chemical and enzyme
|
|
|
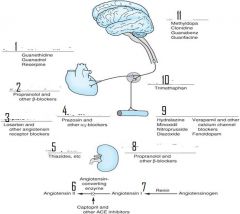
plug in site of action
|
|
|
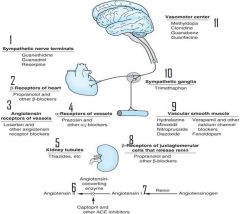
plug in drugs
|
|
|
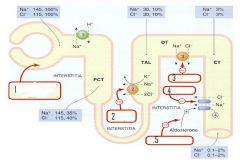
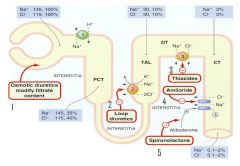
what diuretics work here?
|
|
|
|
what is normal, pre, stage 1, and stage 2 hypertension BP's?
|
normal-<120/<80
pre-120-139/80-89 stage1-140-159/80-89 stage2->160/>100 |
|
|
what is first line treatment for hypertension?
|
thiazide diuretics
|
|
|
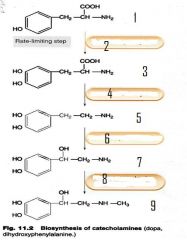
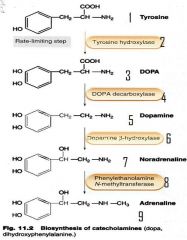
what is the rate limiting step in catecholamine synthesis?
|
tyrosine conversion to dopa by tyrosine hydroxylases
|
|
|
what 2 substances breakdown catecholamines?
|
MAO and COMT
|
|
|
what is the site of action of centrally acting sympatholytics?
|
a2 receptors of the vasomotor center
|
|
|
3 drugs acting on a2 receptors
|
clonidine, guanabenz, guanfacine
|
|
|
prodrug that acts on a2 receptor
|
a-methyldopa
|
|
|
active form of a-methyldopa
|
a-methylnorepinephrine
|
|
|
intracerebroventricular injection of a2 agonists cause BP to go higher or lower?
|
lower
|
|
|
sedation, vertigo, and lactation in men are side effects of what class of drugs?
|
centrally acting sympatholytics
|
|
|
what type of drug would block the effect of clonidine and guanethadine?
|
tricyclic antidepressants
|
|
|
what is the MOA of reserpine?
|
blocks repackaging of NE, dopamine, seratonin taken up into cell causing eventual depletion of NE, dopamine, seratonin stores
|
|
|
what is the MOA of guanethadine?
|
displaces NE from vesicle, prevents release by anesthetic-like effect, causes eventual depletion of NE stores
|
|
|
what does vesicular depletion of transmitter stores do to post synaptic receptors?
|
causes upregulation, supersensitivity of receptors
|
|
|
caution should be taken when using OTC cold medicines while taking guanethadine because...
|
sympathomimmetics in cold medicines can cause hypertensive crisis
|
|
|
guanethadine is used in pheocromocytoma pts but can cause what?
|
hypertensive crisis by release of lg stores of NE in tumor
|
|
|
what were the problems with the first a blockers?
|
blocked both a1 and a2 and caused tachycardia and tolerance to antihypertensive effects
|
|
|
what is the major difference between phentolamine and phenoxybenzamine?
|
phenoxybenzamine is irreversible
|
|
|
which 2 a1 blockers have significant first pass effect?
|
prazosin and terazosin
|
|
|
which 4 B blockers have ISA?
|
acebutolol, carteolol, pindolol, penbutolol
|
|
|
what is the most selective B1 antagonist also thought to have B2 agonist properties?
|
nebivolol
|
|
|
Longest acting B antagonist, doesn't pass BBB
|
nadolol
|
|
|
what effect does B1 blockade have on the kidney?
|
blocks renin release thus blocking RAAS response to drop in BP
|
|
|
What is nebivolol's effect in the kidney?
|
blocks renin release and decreases peripheral resistance, B2 agonist action causes renal vasodilation via NO formation
|
|
|
what is missing in ESRD pts that normally breaks down NE and E in the synapse?
|
renalase
|
|
|
What are the 2 benefits of using a B blocker with ISA?
|
less resting bradycardia but still blocks exercise induced increase in HR, less receptor upregulation after long term use/less supersensitivity
|
|
|
what conditions are contraindicated for use of B blockers?
|
AVB, CHF, asthma, SB
|
|
|
How does B blockers contribute to atherogenesis?
|
increasing triglycerides and LDL, decreasing HDL
|

