![]()
![]()
![]()
Use LEFT and RIGHT arrow keys to navigate between flashcards;
Use UP and DOWN arrow keys to flip the card;
H to show hint;
A reads text to speech;
49 Cards in this Set
- Front
- Back
|
Present pathogenous strains of E. coli. Briefly discuss their virulence factors
|
- Enterotoxigenic E. coli (ETEC) VF: Fimbriae K99, K88 and F41 and enterotoxins like; LT, STa and STb. Enterocyte adherence via fimbriae, enterotoxins causes secretory diarrhea. - Enteropathogenic E. coli (EPEC) VF: Intimin, toxins uncertain. Adherence due to intimin, attachment and lesion results from bacterial attacment to enterocytes and bruch border microvilli. Diarrhea because malabsorption. - Enterohaemorrhagic E. coli (EHEC) VF: Stx1 and Stx2. Causes haemorrhages. - Enteroinvasive E. coli (EIEC) VF: - Necrotoxigenic E. coli (NTEC) VF: Invasins, fimbrial and afimbrial adhesins, toxins like CNF1- and 2. Intestinal colonization to enterocytes and to blood vessels --> edema. - Enteroaggregative E. coli (EAggEC) VF: |
|
|
Selective medias to enterobacteriaceae
|
McC - not very permissive Xylose Lysine Deoxychocolate agar - good for shigella and salmonella Hektoen agar - differential media between salmonella (black) and shigella (green) Brilliant green agar - highly selective for salmonella other than S. typhi. Salmonella Shigella agar - inhibits proteus spp. Used for isolation of salmonella and shigella. Selenite F broth - enrichment medium for salmonella or shigella. |
|
|
Shipping fever - describe causative agent and the disease.
|
Bovine pneumonic pasteurellosis Caused by M. haemolytica serotype A1. - Gram neg - Coccobacilli to rods - Non-motile - Bipolar staining - Microaerophilic with fermentative metabolism (ferment mannitol, but not D-mannose which diffenrentiate them from Pasturella) - Fastidious - Grow on McC - Phenotypic resemblance to bacteria that belong to Pasturella - Catalase + - Oxidase + Multifactoral, depends on environmental factors, concurrent infections and viruses and other bacterial agents. Also depends on the dose of M. haemolytica and host immune system status. Causes severe bronchopneumonia. Depression, fever, anorexia, nasal discharge soft moist cough. Apparent after 6-10 days after stressful episode. When extensive, dyspnea and open-mouth breathing. |
|
|
Isolation and testing of salmonella
|
Specimen collection: blood, urine, feces, vomit, bile, milk med mera. Inoculate in selenite F broth for enrichment and multiplied growth. Then inoculate on BA, McC and SS. Growth on all 3 = salmonella. - Biochemical tests: Lactose neg Indole neg Nitrate + Urease neg Oxidase neg Catalase + H2S neg Lysine decarboxylation + - Serotyping - most imp - Antibiotic susceptibility |
|
|
CAMP test
|
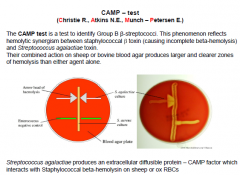
|
|
|
General features of actinobacillus
|
- Gram neg - Rods/coccobacilli - Fastidious bacteria - Anaerobic, CO2 required for growth. - Carbohydrates fermented without gas production. - Grow on media supplemented with blood and serum - Temperature 20-42*C - Most strains on McC but poorly - Cultures die witin a week - Oxidase + - Indole neg - Nitrate reducant Variably haemolytic on blood agar. |
|
|
How to identify virulent strains of staphylococci?
|
By tube test testing the presence of coagulase (present in all pathogenic strains) Isolated staphylococcal strains introduced to the tube with rabbit plasma. How fast the clot is formed depends on amount and phase of growth. Clotting occurs between 4-24 h. If negative, 4 h incubation 35*C (room temp) and then read again due to some strains capability of lysing the clot (= false negative result) |
|
|
Pathogenesis of stranglers. How is it transmitted?
|
Stranglers in horses. Caused by Streptococcus equi spp. equi, where the bacteria is commensal to the mucosa of the upper respiratory tract. Opportunistic pathogen. Pathogenesis: Attaches to tonsillar crypt cells and adjacent lymphoid nodules. Within hours translocated into local lymphatics. Fever, malaise, nasal dischargem cough, swelling at mandibular lymph node --> pressure on airway and respiratory difficulty. Metastatic abscessation --> spread via circulation or lymphatic route to lungs, abdomen, brain (fairly common). Clinical course short, often no complications but myocarditis and purpura haemorrhagica can follow (PH considered to be immune-mediated disease, occur 1-3 weeks after illness. Transmission through direct contact with nasal discharge or via drainage of abscesses. Often when horses are assembled in one place, like markets, races or competitions. May continue the shed of bacteria 4 weeks after development of clinical signs. |
|
|
Diagnostic methods for identification of mastitis
|
Clinical signs: inflammation of mammary tissue,and clots in the milk Mastitic milk: clotted, watery, may contain mucus, pus, even blood Milk samples should be collected carefullyto avoid contamination Specimens (milk) should be cultured on blood agar, Edwards medium and MacConkey agar and incubated aerobically at 37*C for 24-48h. Id by haemolysis, biochemical tests and Lancefield grouping. |
|
|
Explain phenomenon of clumping factor
|
It's when coagulase is bound to the bacterial wall, which differentiate from the free coagulase released from pathogenic staphylococcus strains. The clumping factor converts fibrinogen in plasma to fibrin which causes the bacterial cells to clump together. A slide test alike the agglutination test is done (but no antibodies are involved) but it's an auto-reaction.
|
|
|
Describe at least 2 selective medias for Salmonella and discuss the outcome of inoculation
|
Hektoen Enteric agar: Bile salts inhibit gram + Substrates: - Lactose - Salicin - Thiosulfate/ferric ammonium citrate - Bromothymol blue Differential medium. Blue/green = lactose non-fermented. Yellowish = lactose fermented. Salmonella black colonies (FAC). Shigella transluscent green colonies. Brilliant green agar: Brilliant green dye - inhibit gram + and most members of the enterobacteriaceae except Salmonella. Substrates: - Lactose - Sucrose - Phenol red if sugars not fermented = pink colonies. (= salmonella). If sugars are fermented = yellow/green colonies. |
|
|
Name causative agent in environmental mastitis
|
E. coli, Klebsiella ssp., S. dysgalactiae, M. bovis, C. bovis
|
|
|
Shipping fever laboratory diagnosis
|
Specimen: - Nasal swabs - Purulent nasal discharge Post-mortem: pneumonic lung Direct examination: rods or coccobacilli. Culture technique: McC. If heavily contaminated BA with neomycin, bacitrin and acitidone. Incubate for: 24-48 h aerobically at 37*C. Id: - Colonial morphology --> pinpoint red colonies on McC. No agar, indole negative and have beta-haemolytic colonies. - growth on McC - + oxidase test - + catalase test |
|
|
Characterize selective media for Enterobacteriaceae family
|
Hektoen Agar, Brilliant Green agar, Xyline Lysine deoxycholate agar, Salmonella Shigella agar, Selenite F broth.
|
|
|
Species of genus Actinobacillus
|
Species: - A. lignieresii - A. pleuropneumoniae - A. equuli (ssp. equuli, in Eq and Su, and ssp. haemolyticus onlu in horses) - A. suis - A. seminisA. actinomycetemcomitans (aggregatibacter actinomycetemcomitans) (do not grow on McC) |
|
|
Characterize genus Actionbacillus, name species of veterinary importance |
Gram negative Rods to cocci Anaerobic, require CO2 for growth Carbohydrates fermented without gas production Temp 20-42 Fastidious, need blood and serum Most strains grow on McC but poorly Oxidase + Indole - Nitrate reductant Variably haemolytic on BA
A. ligniersii A. pleuropneumoniae A equuli (spp. equuli and haemolytica) A. suis A. seminis A. actinomycetemcomitans |
|
|
Five examples of discriminatory features of Pasturella spp. and Mannheimiia haemolytica
|
Pasturella is: Non-haemolytic Indole positive Do not grow on McC Sweetish odor Shiny, grayish, moderate size, round colonies M. haemolytica: Haemolytic (beta-haemolytic) Do grow on McC Indole negative Pinpoint red colonies on McC No odor |
|
|
General characteristics of Enterobacteriaceae family
|
• Gram-negative * facultively anaerobic rods • Ferment glucose and other sugars • Reduce nitrate to nitrite • Oxidase negative • Catalase positive • Non-sporeforming • Tolerate bile salts in McC agar • Non-fastidious, grow on non-enriched media *Most motile by peritrichous flagella (= flagella projecting in all directions) |
|
|
Haemophilius species of vet. Importance and caused diseases
|
Main pathogens: - H. parasuis(pigs) - Glässer's disease, meningitis, myositis, pneumonia, septicaemia - H. paragallinarium(chickens) - Infectious coryza - H. influenzaemurium(rodents) - respiratory infection, ocular disease |
|
|
What cause cholera and what are the virulence factors
|
Vibrio cholerae. VF: Polysaccharide capsule - Enterotoxins - LT (activates adenylate cyclase which activates cAMP which lead to hypersecretion of fluids and electrolytes which results in watery diarrhea. - LPS (core nec to survive bile) - Siderophores - Pili - adherence |
|
|
Describe growth of Proteus spp on selective media
|
Swarming bacteria. A multicellular behaviour, a cyclical differentiation of short vegetative cells called swimmer cells and filamentous highly flagallated cells called swarmer cells. Result in a coordinated behaviour.
|
|
|
Compare and differentiate between Y. enterocolitica and Y. pseudotuberculosis
|
Y. pseudotuberculosis: - cause severe systemic disease - have 10 serotypes (I, II, III most pathogenic) cause; enteric yearsinosis in farmed deers - pseudotuberculosis in guinea pgs - septicaemic yearsiniosis in caged birds Y. enterocolitica: - less likely to become systemic disease - cause disease in humans mostly - 5 biotypes and 50 serotypes Both found in intestinal tract of wild mammals. Mechanically spread by birds. Both cause sporadic abortion in ewes. Same VF (adhesins, invasins, resistance to phagolysis, induce macrophage apoptosis, enterotoxins like YST (mostly in enterocolitica) and iron acquisation) |
|
|
Vibrio species of veterinary importance and disease they cause
|
V.metschinikovii - cholera like disease in poultry and young birds housed in zoological collections V. ordalii - Vibriosis in fish. Haemorrhagic septicaemia in eels, salmons and trouts. V. salmonicida- Cold-water vibriosis. Skin haemorrhages in cultured Atlantic salmon. |
|
|
Media for haemophilus. Explain phenomenon of “satellitism"
|
Chocolate agar contain the necessary X factors (hemin) and V factors (NAD). Satellitism is when you inoculate blood agar with Haemophilus and then streak S. aureus (feeder streak) across. The S. aureus provide the necessary V factors for haemophilus growth - the growth occur only near the feeder streak. Common in sputum cultures (where both bacterias can be present). |
|
|
Purpose and method of salmonella serotyping
|
The purpose of salmonella serotyping is to differentiate between the 2 400 diff. salmonella serotypes. Serotyping refers to the differences in microbial surface antigens between different Salmonella serovars. Members of a serogroup is called serovars. Method: Serovars id'd by 2 sets of antigens O - somatic antigens discovered by agglutination test. Gives the serogroup. H - flagellar antigens. Often biphasic, discovered by 2 rounds of agglutination tests. Vi - (in some serovars) superficial capsular K-antigens. |
|
|
What are the functions of E.coli in normal flora and how is it transmitted?
|
Fermentation of ingesta. Transmitted fecal-oral route.
|
|
|
Lab diagnosis of EHEC
|
Specimen: feces, urine, blood, milk, tissue samples Culture: SMAC (McC with sorbitol) Incubation 24 h 37*C Results: Growth on McC (lac +) colourless colonies in SMAC, difference between other E. coli that would result in pink colonies - which mean EHEC does not ferment sorbitol (like the other strains do). Esp. for E. coli O157 (EHEC) Further on biochemical tests, PCS (genes encoding pathogenicity), serotyping and antibiotic susceptibility |
|
|
Characterize Vibrioaneceae family
|
Gram neg rods (some curved) Halophilic (thrive in salty conditions) Non-fastidious but need NaCl complementation Habitat in salty to breckish waters. Facultative anaerobes catalase + oxidase + motile Opportunistic pathogen in fish and in chicken. V. metschnikovii V. ordalii V. salmonicida |
|
|
Isolation of Salmonella from fodder
|
Specimen: Suspected contaminated fodder or animal feed. Preincubation in buffered peptone water (enrichment broth which supplies bacteria with N compounds and maintain pH) Incubation for 16-24 h in 37*C Transfer to SF broth 18-24 h 37*C Inoculate on SS, BGA, Hektoen agar or XLD agar Incubate 18-24 h 37*C Biochemical differentiation and serotyping of result. |
|
|
Staphylococcus morphological features and characteristics of colonies on blood agar
|
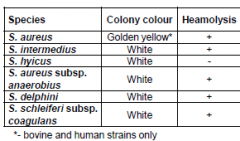
|
|
|
Toxins and enzymes produced by Staphylococci
|

Enzymes: Coagulase Lipase Nucleases Hyaluronidase |
|
|
Characteristic of Staphylococci and Streptococci growth on liquid and solid surfaces
|
Morphology Staphylococci: Medium sized White, creamy, yellowish, yellow, orange Haemolysis type beta: Complete - S.aureus Incomplete - S. pseudointermedius and S. intermedius No haemolysis - S. epidermidis OF test - aerobic growth Morphology Streptococci: Small transluscent colonies Type of haemolysis OF test - aerobic growth |
|
|
Virulence factors of Staphylococcus species
|
Coagulase (act thrombin - fibrinogen to fibrin) Protein A - binds to immunoglobulins (Fab and Fc - inhibit fagocytosis) Capsular polysaccharide (release of cytokines, interfere with host defense mechanism) Peptidoglycan and lipotheichoic acid (cytokine release) Adhesins - MSCRAMMs Hyaluronidase - spreading factor (so that pathogen can invade deeper tissues) Toxins TSST-1 = superantigen, stimulate T cells without antigen recognition. Staphylococcal enterotoxins (SEs) - vomiting activity Exfoliative toxins (ETs) - widespread blistering and loss of epidermis (S.pseudointermedius - canine pyoderma) Haemolysin - Alpha and beta Leukocidin - Panton-Valentine leukocidin (PVL) necrotizing factor. Poreforming, act on neutrophils. (S. aureus) |
|
|
Differentiation of Staphylococcus species
|
The complete, incomplete or absent haemolysis. Coagulase slide test - clearest + result in S.aureus. Variable result in S. pseudointermedius. S. aureus is golden yellow on blood agar. Others white PCR |
|
|
Test tube detection of coagulase
|
Check for + or neg result for the coagulase enzyme. The clumping factor, dvs. coagulase bound to the bacterial cell wall (not free coagulase). Used to identify pathogenic species. When bacteria is isolated, introduce into tube with rabbit plasma. Positive result gives clotting which occurs within 4-24 h (incubated 35*C). After should be held at room temperature and read again after 18-24 h, because some strains lysis the clot and will then give a false negative result at the 1st reading. |
|
|
Differentiation of G+ pyogenic cocci
|
Differences in colony morphology Catalase test (strepto neg, staphylo pos) OF test (micrococcus F-) Resistance to lysostaphin (enzyme that cleaves cross-bridges in cell wall). Staphylo susceptible, Micrococcus resistant |
|
|
What medium is used for isolation of Haemophilus and why
|
Chocolate agar Because it provides the necessary X factors (hemin) and V factors (NAD) necessary for haemophilus growth. |
|
|
Pyogenic Streptococcus species |
S. Agalactiae S. Dysgalactiae S. Uberis S. Equi ssp. Zooepidemicus |
|
|
Pathogenic Streptococcus species
|
S. pyogenes - man, scarlet fever S. agalactiae - cattle sheep goat, chronic mastitis S.dysgalactiae - cattle, acute mastitis S. equi ssp. equi - horses, Strangles S. equi ssp. zooepidemicus - horses, mastitis S. suis - pigs, septicaemia S. canis - carnivores, neonatal septicaemia S. uberis - cattle, mastitis S. pneumoniae - man primates ect, septicaemia |
|
|
Streptococcal species and pathogenicity
|
S. pyogenes - man, scarlet fever S. agalactiae - cattle sheep goat, chronic mastitisS.dysgalactiae - cattle, acute mastitis S. equi ssp. equi - horses, Strangles S. equi ssp. zooepidemicus - horses, mastitisS. suis - pigs, septicaemia S. canis - carnivores, neonatal septicaemia S. uberis - cattle, mastitis S. pneumoniae - man primates ect, septicaemia Pathogenicity: Beta-haemolytic more pathogenic than alpha-haemolytic. Virulence factors: • Exotoxins: - Streptolysins (haemolysins) Beta-haemolysin cytotoxic for eukaryotic cells by pore forming in target cell membrane. CAMP factor (ceramide-binding protein) of S. agalactiae --> haemolysis of staphylococcal sphingomyelinase (cytotoxic for mammary glands) Pyrogenic exotoxin A - superantigen --> stimulate cytokine production by T cells (streptococcal toxic chock syndrome) Streptolysin O (SLO) - produce streptococci of A, C and G. Cholesterol-binding toxin. Potent membrane-damaging effects. - Hyaluronidase - DNAse - Streptokinase - Protease - Polysaccharide capsule, antiphygocytic (S. pyogenes, S. pneumoniae and some strains of S. qui) - Cell wall M proteins --> antiphagocytic also • Enzymes Dissolve fibrin • Binding of plasma components - avoid IMS or phagocytic effect. |
|
|
Identification of Streptococcus responsible for mastitis
|
Streptococcus agalactiae. BA and McC. No growth on McC. Colonies mucoid transluscent, with beta-heamolysis. Incubation 37*C for 24-48 h |
|
|
Morphology and characteristics of Pasteurella
|
- Small - Non-motile - Gram neg - Rods/coccobacilli - Oxidase + - Facultative anaerobes - Most species catalase + - Fastidious - Bipolar staining - Most commensals of the upper respiratory tract mucosa, some respiratory pathogens. - Survival in environment relatively short. Vet importance: Pastuerella multocida Bibersteinia trehalosi Morph: Round, shiny, grayish, moderate sized colonies. Smell sweetish. |
|
|
Major pathogenic species of Pasteurella, as well as those of minor veterinary importance
|
Vet importance:Pastuerella multocida Bibersteinia trehalosi Minor: P. aerogenes P. anatis P. avium P. caballi P. canis P. dagmatis P. gallinarium P. limphangitis P. pneumotropica |
|
|
Pasteurella species and pathogenicity
|
Vet importance:Pastuerella multocida Bibersteinia trehalosi Minor:P. aerogenesP. anatisP. aviumP. caballiP. canisP. dagmatisP. gallinariumP. limphangitisP. pneumotropica Endogenous infections.Commensal in upper respiratory tract, invade tissues of immunosuppressed animals.Transmission --> exogenous by direct contact or through aerosol.Importance in disease development: - Adhesions - Avoidance of phagocytosis - Fimbriae, enhance mucosal attachment - Hyaluronic capsule, antiphagocytosis role DiseaseSepticaemic pasteurellosis --> severe endotoxaemia and disseminated intravascular coagulation which cause serious illness which can prove fatal. Endotoxin is pyrogenic. |
|
|
Vibrio pathogenicity
|
Virulence factors for V. cholerae - Capsular - adherence + protection - Polysaccharide - Toxins - similar to LT enterotoxin of E. coli. 2 component toxin; B subunit (mediates entry) and A subunit activate cellular adenylate cyclase, causing cAMP accumulation and result in hypersecretion of electrolytes and fluids. - LPS - core necessary to survive bile. - Siderophores - acquisation of iron - Pili - adherence |
|
|
What diseases are caused by Actinobacillus, which species causes each disease?
|
A. ligniersii- wood tongue in bovine A. pleuropneumoniae- pleuropneumonia in pigs A equuli (spp. equuli and haemolytica)- septicaemia and sleepy foal disease A. suis- septicaemia, pneumonia A. seminis- epididymitis A. actinomycetemcomitans- epididymitis |
|
|
Characteristics and pathogenicity of Aeromonas and Plesiomonas
|
Aeromonas: Invade host cell, disseminate to any organ. Death due to massive septicaemia and toxic etracellular products of the organism, which interefere with host blood supply and result in tissue necrosis.Virulence factors - Toxin - cytotoxin, similar to Shiga toxin - Surface proteins - Extracellular degradative enzymes. - Heamolysins - aerolysins, poreforming toxin that causes ion leakage --> cell lysis - Cytotoxic enterotoxin, heat-stable cytotoxic toxin and heat-labile enterotoxin --> enteropathogenicity. - Flagellae - swimming - Pili - adhesins - Capsule - Wide range of enzymes (serine protease, lipases, aminopeptidases, metalloproteases and phospholipases. - Siderophores Plesiomonas: - Cholera-like toxin - Haemolysin - role in iron acquisation - Heat-stable enterotoxin |
|
|
|
|
|
Lab diagnosis of A. lignieresii |
Wash pus or exudate with distilled water on a petri dish. Suspend the white granules in 10% KOH on a slide and cover with a glass slip. Observe under microscope the clubs and the area that surrounds the clubs that the granulomatous create (low magnitude). Can also be stained for better vision. |

